Abstract
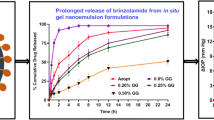
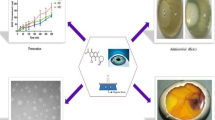
Dilutable nanoemulsions are potent drug delivery vehicles for ophthalmic use due to their numerous advantages as sustained effect and high ability of drug penetration into the deeper layers of the ocular structure and the aqueous humor. The aim of this article was to formulate the antiglaucoma drug dorzolamide hydrochloride as ocular nanoemulsion of high therapeutic efficacy and prolonged effect. Thirty-six systems consisting of different oils, surfactants, and cosurfactants were prepared and their pseudoternary-phase diagrams were constructed by water titration method. Seventeen dorzolamide hydrochloride nanoemulsions were prepared and evaluated for their physicochemical and drug release properties. These nanoemulsions showed acceptable physicochemical properties and exhibited slow drug release. Draize rabbit eye irritation test and histological examination were carried out for those preparations exhibiting superior properties and revealed that they were nonirritant. Biological evaluation of dorzolamide hydrochloride nanoemulsions on normotensive albino rabbits indicated that these products had higher therapeutic efficacy, faster onset of action, and prolonged effect relative to either drug solution or the market product. Formulation of dorzolamide hydrochloride in a nanoemulsion form offers, thus, a more intensive treatment of glaucoma, a decrease in the number of applications per day, and a better patient compliance compared to conventional eye drops.




Similar content being viewed by others
References
Hughes PM, Mitra AK. Overview of ocular drug delivery and iatrogenic ocular cytopathologies. In: Mitra AK, editor. Ophthalmic drug delivery systems. New York: Marcel Dekker; 1993. p. 1–27.
Patton TF, Robinson JR. Quantitative precorneal disposition of topically applied pilocarpine nitrate in rabbit eyes. J Pharm Sci. 1976;65:1295–301.
Sieg JW, Robinson JR. Vehicle effects on ocular drug bioavailability II: evaluation of pilocarpine. J Pharm Sci. 1977;66:1222–8.
Chein YW, Cabana BE, Mares SE. Ocular controlled release drug administration. In: Chein YW, editor. Novel drug delivery systems; fundamentals, development concepts, biomedical assessments (drugs and the pharmaceutical sciences), vol. 14. New York: Marcel Dekker; 1982. p. 13–55.
Middleton DL, Leung SS, Robinson JR. Ocular bioadhesive delivery systems. In: Lenaerts V, Gurny R, editors. Bioadhesive drug delivery systems. Boca Raton: CRC; 1990. p. 179–202.
Desai SD, Blanchard J. Ocular drug formulation and delivery. In: Swarbick J, Boylan JC, editors. Encyclopedia of pharmaceutical technology, vol. 11. New York: Marcel Dekker; 1994. p. 43–75.
Felt O, Furrer P, Mayer JM, Plazonnet B, Buri P, Gurny R. Topical use of chitosan in ophthalmology: tolerance, assessment and evaluation of precorneal retention. Int J Pharm. 1999;180:185–93.
Munier A, Gunning T, Kenny D, O’Keefe M. Causes of blindness in the adult population of the Republic of Ireland. Br J Ophthalmol. 1998;82:630–3.
Blomdahl S, Calissendorff BM, Tengrowth B, Wallin O. Blindness in glaucoma patients. Acta Ophthalmol (Copenh). 1997;75:589–91.
Kaur IP, Smitha R, Aggarwal D, Kapil M. Acetazolamide: future perspective in topical glaucoma therapeutics. Int J Pharm. 2002;248:1–14.
Hoyng PF, van Beek LM. Pharmacological therapy for glaucoma: a review. Drugs. 2000;59:411–34.
Maren TH. The development of topical carbonic anhydrase inhibitors. Glaucoma. 1995;4:49–62.
Sugrue MF. The preclinical pharmacology of dorzolamide hydrochloride, a topical carbonic anhydrase inhibitor. J Ocul Pharmacol Ther. 1996;12:363–76.
Sugrue MF. Pharmacological and ocular hypotensive properties of topical carbonic anhydrase inhibitors. Prog Retin Eye Res. 2000;19:87–112.
Sigurdsson HH, Stefansson E, Gudmundsdottir E, Eysteinsson T, Thorsteinsdottir M, Loftsson T. Cyclodextrin formulation of dorzolamide and its distribution in the eye after topical administration. J Control Release. 2005;102:255–62.
Quint MP, Grove J, Thomas SM. Dorzolamide hydrochloride. In: Brittain HG, editor. Analytical profiles of drug substances and excipients, vol. 26. New York: Academic; 1999. p. 283–316.
Rusk C, Sharpe E, Laurence J, Polis A, Adamsons I. Comparison of the efficacy and safety of 2% dorzolamide and 0.5% betaxolol in the treatment of elevated intraocular pressure. Dorzolamide comparison study group. Clin Ther. 1998;20:454–66.
Silver LH. Ocular comfort of brinzolamide 1.0% ophthalmic suspension compared with dorzolamide 2.0% ophthalmic solution: results from two multicenter comfort studies. Brinzolamide Comfort Study Group. Surv Ophthalmol. 2000;44(Suppl 2):S141–45.
Salminen L. Review: systemic absorption of topically applied ocular drugs in humans. J Ocul Pharmacol Ther. 1990;6:243–9.
Baudouin C. Side effects of antiglaucomatous drugs on the ocular surface. Curr Opin Ophthalmol. 1996;7:80–6.
Arici MK, Arici DS, Topalkara A, Guler C. Adverse effects of topical antiglaucoma drugs on the ocular surface. Clin Experiment Ophthalmol. 2000;28:113–7.
Konowal A, Morrison JC, Brown SV, Cooke DL, Maguire LJ, Verdier DV, et al. Irreversible corneal decompensation in patients treated with topical dorzolamide. Am J Ophthalmol. 1999;127:403–6.
Silva-Cunha A, Fialho SL, Carneiro LB, Oréfice F. Microemulsões como veículos de drogas para administração ocular tópica. Arq Bras Oftalmol. 2003;66:385–91.
Alany RG, Rades T, Nicoll J, Tucker IG, Davies NM. W/O microemulsions for ocular delivery: evaluation of ocular irritation and precorneal retention. J Control Release. 2006;111:145–52.
Vandamme TF. Microemulsions as ocular drug delivery systems: recent developments and future challenges. Prog Retin Eye Res. 2002;21:15–34.
Garti N, Aserin A, Tiunova I, Fanun MA. DSC study of water behavior in water-in-oil microemulsions stabilized by sucrose esters and butanol. Colloids Surf A Physicochem Eng Asp. 2000;170:1–18.
Moreno MA, Ballesteros MP, Frutos P. Lecithin-based oil-in-water microemulsions for parenteral use: pseudoternary phase diagrams, characterization and toxicity studies. J Pharm Sci. 2003;92:1428–37.
Shafiq S, Shakeel F, Talegaonkar S, Ahmad FJ, Khar RK, Ali M. Development and bioavailability assessment of ramipril nanoemulsion formulation. Eur J Pharm Biopharm. 2007;66:227–43.
Miyazaki S, Suzuki S, Kawasaki N, Endo K, Takahashi A, Attwood D. In situ gelling xyloglucan formulations for sustained release ocular delivery of pilocarpine hydrochloride. Int J Pharm. 2001;229:29–36.
Wu C, Qi H, Chen W, Huang C, Su C, Li W, et al. Preparation and evaluation of a carbopol/HPMC-based in situ gelling ophthalmic system for puerarin. Yakugaku Zasshi. 2007;127:183–91.
Khan KA, Rhodes CT. Effect of compaction pressure on the dissolution efficiency of some direct compression systems. Pharm Acta Helv. 1972;47:594–607.
Draize JH, Woodard G, Calvey HO. Methods for the study of irritation and toxicity of substances applied topically to the skin and mucous membranes. J Pharmacol Exp Ther. 1944;82:377–90.
Hughes WFJ. The tolerance of rabbit cornea for various chemical substances. Bull Johns Hopkins Hosp. 1948;82:338–49.
Laillier J, Plazonnet B, Le Douarec JC. Evaluation of an objective method of studying eye irritation. Proc Eur Soc Toxicol. 1976;17:336–50.
Conquet P, Durand G, Laillier J, Plazonnet B. Evaluation of ocular eye irritation in the rabbit: objective versus subjective assessment. Tox App Pharmacol. 1977;39:129–39.
Yamaguchi M, Yasueda S, Isowaki A, Yamamoto M, Kimura M, Inada K, et al. Formulation of an ophthalmic lipid emulsion containing an anti-inflammatory steroidal drug, difluprednate. Int J Pharm. 2005;301:121–8.
Alany RG, Tucker IG, Davies NM, Rades T. Characterizing colloidal structures of pseudoternary phase diagrams formed by oil/water/amphiphile systems. Drug Dev Ind Pharm. 2001;27:31–8.
Chemicals BF. Cremophor® EL. Technical leaflet, ME 074 e. Ludwigshafen: BASF Fine Chemicals; 1997.
Kommuru TR, Gurley B, Khan MA, Reddy IK. Self-emulsifying drug delivery systems (SEDDS) of coenzyme Q10: formulation development and bioavailability assessment. Int J Pharm. 2001;212:233–46.
Grant WM, Schuman JS. Toxicology of the eye. 4th ed. Springfield: Charles C. Thomas; 1993.
Bietti GB, Virno M, Pecori-Giraldi J. Propylene glycol: a new osmotic agent for ophthalmic uses. Doc Ophthalmol. 1973;34:77–92.
Tamilvanan S, Benita S. The potential of lipid emulsion for ocular delivery of lipophilic drugs. Eur J Pharm Biopharm. 2004;58:357–68.
Aboofazeli R, Lawrence MJ. Investigations into the formation and characterization of phospholipid microemulsions. II. Pseudo-ternary phase diagrams of systems containing water–lecithin–isopropyl myristate and alcohol: influence of purity of lecithin. Int J Pharm. 1994;106:51–61.
Trotta M, Gallarate M, Pattarino F, Carlotti ME. Investigation of the phase behaviour of systems containing lecithin and 2-acyl lysolecithin derivatives. Int J Pharm. 1999;190:83–9.
Warisnoicharoen W, Lansley AB, Lawrence MJ. Nonionic oil-in-water microemulsions: the effect of oil type on phase behaviour. Int J Pharm. 2000;198:7–27.
Huibers PD, Shah D. Evidence for synergism in non-ionic surfactant mixtures: enhancement of solubilization in water-in-oil microemulsions. Langmuir. 1997;13:5762–5.
Engels T, Forster T, Rybinsko WV. The influence of coemulsifier type on the stability of oil-in-water emulsions. Colloids Surf A Physicochem Eng Aspects. 1995;99:141–9.
Weingarten C, Magalhaes NSS, Baszkin A, Benita S, Seiller M. Interaction of a nonionic ABA copolymer surfactant with phospholipid monolayers: possible relevance to emulsion stabilization. Int J Pharm. 1991;75:171–9.
Ninham BW, Chen SJ, Evans DF. Role of oils and other factors in microemulsion design. J Phys Chem. 1984;88:5855–7.
Taha MO, Abdel-Halim H, Al-Ghazawi M, Khalil E. QSPR modeling of pseudoternary microemulsions formulated employing lecithin surfactants: application of data mining, molecular and statistical modeling. Int J Pharm. 2005;295:135–55.
Kawakami K, Yoshikawa T, Hayashi T, Nishihara Y, Masuda K. Microemulsion formulation for enhanced absorption of poorly soluble drugs. II. In vivo study. J Control Release. 2002;81:75–82.
HaBe A, Keipert S. Development and characterization of microemulsions for ocular application. Eur J Pharm Biopharm. 1997;43:179–83.
Chen H, Chang X, Weng T, Zhao X, Gao Z, Yang Y, et al. A study of microemulsion systems for transdermal delivery of triptolide. J Control Release. 2004;98:427–36.
Tenjarla S. Microemulsions: an overview and pharmaceutical applications. Crit Rev Ther Drug Carrier Syst. 1999;16:461–521.
Zignani M, Tabatabay C, Gurny R. Topical semi-solid drug delivery: kinetics and tolerance of ophthalmic hydrogels. Adv Drug Deliv Rev. 1995;16:51–61.
Radomska-Soukharev A, Wojciechowska J. Microemulsions as potential ocular drug delivery systems: phase diagrams and physical properties depending on ingredients. Acta Pol Pharm. 2005;62:465–71.
Fialho SL, da Silva-Cunha A. New vehicle based on a microemulsion for topical ocular administration of dexamethasone. Clin Experiment Ophthalmol. 2004;32:626–32.
Ciba-Geigy. Wissenschaftliche Tabellen Geigy. 8th ed. Basel: Ciba-Geigy; 1997. Through Fialho SL, da Silva-Cunha A. New vehicle based on microemulsion for topical ocular administration of dexamethasone. Clin Experiment Ophthalmol. 2004;32:626-32.
Keipert S, Siebenbrodt I, Lüders F, Bornschein M. Mikroemulsionen und ihre. potenzielle pharmazeutische Nutzung. Pharmazie. 1989;44:433–44.
Miller D. Measurement of the surface tension of tears. Arch Ophthalmol. 1969;82:368–71.
Lin SP, Brenner H. Marangoni convection in a tear film. J Colloid Interface Sci. 1982;85:59–65.
Ciba-Geigy. Wissenschaftliche Tabellen Geigy. 8th ed. Basel: Ciba-Geigy; 1977.
Hasse A, Keipert S. Development and characterization of microemulsions for ocular application. Eur J Pharm Biopharm. 1997;43:179–83.
Mathis GA. Clinical ophthalmic pharmacology and therapeutics: ocular drug delivery. In: Gelatt KN, editor. Veterinary ophthalmology. Orlando: Lippincott Williams & Wilkins; 1999. p. 291–7.
Van Ooteghem MM. Formulations of ophthalmic solutions and suspensions. Problems and advantages. In: Edman P, editor. Biopharmaceutics of ocular drug delivery. Boca Raton: CRC; 1993. p. 31–2.
Polish Pharmaceutical Society. Polish Pharmacopoeia V, vol. 3. Warsaw: Polish Pharmaceutical Society; 1993. p. 39.
Terry JE, Hill RM. Human tear osmotic pressure, diurnal variation and closed eye. Arch Ophthalmol. 1978;96:120–2.
Rhee YS, Choi JG, Park ES, Chi SC. Transdermal delivery of ketoprofen using microemulsions. Int J Pharm. 2001;228:161–70.
Walters KA, Brain KR, Green DM, James VG, Watkinson AC, Sands RH. Comparison of the transdermal delivery of estradiol from two gel formulations. Maturitas. 1998;29:189–95.
Lee PJ, Langer R, Shastri VP. Novel microemulsion enhancer formulation for simultaneous transdermal delivery of hydrophilic and hydrophobic drugs. Pharm Res. 2003;20:264–9.
Roggeband R, York M, Pericoi M, Braun W. Eye irritation responses in rabbit and man after single applications of equal volumes of undiluted model liquid detergent products. Food Chem Toxicol. 2000;38:727–34.
Muchtar S, Abdulrazik M, Frucht-Pery J, Benita S. Ex vivo permeation study of indomethacin from a submicron emulsion through albino rabbit cornea. J Control Release. 1997;44:55–64.
Mainardes RM, Urban MC, Cinto PO, Khalil NM, Chaud MV, Evangelista RC, et al. Colloidal carriers for ophthalmic drug delivery. Curr Drug Targets. 2005;6:363–71.
van der Bijl P, van Eyk AD, Meyer D. Effects of three penetration enhancers on transcorneal permeation of cyclosporine. Cornea. 2001;20:505–8.
Liu Z, Li J, Nie S, Guo H, Pan W. Effects of Transcutol P on the corneal permeability of drugs and evaluation of its ocular irritation of rabbit eyes. J Pharm Pharmacol. 2006;58:45–50.
Lawrence MJ, Rees GD. Microemulsion-based media as novel drug delivery systems. Adv Drug Deliv Rev. 2000;45:89–121.
Kaur IP, Smitha R. Penetration enhancers and ocular bioadhesives: two new avenues for ophthalmic drug delivery. Drug Dev Ind Pharm. 2002;28:353–69.
Yu W, Tabosa do Egito ES, Barratt G, Fessi H, Devissaguet JP, Puisieux F. A novel approach to the preparation of injectable emulsions by a spontaneous emulsification process. Int J Pharm. 1993;89:139–46.
Acknowledgements
We gratefully appreciate the generous supply of dorzolamide hydrochloride by Jamjoom Pharma, Jeddah, KSA and the kind help for assessment of the ocular irritation test by Dr. Maali A. Halim, Faculty of Medicine, Cairo University. We also acknowledge the financial support provided by the National Research Center, Egypt.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ammar, H.O., Salama, H.A., Ghorab, M. et al. Nanoemulsion as a Potential Ophthalmic Delivery System for Dorzolamide Hydrochloride. AAPS PharmSciTech 10, 808–819 (2009). https://doi.org/10.1208/s12249-009-9268-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1208/s12249-009-9268-4