Abstract
Background
In this study considering the relationship between serum endocan and CHA2DS2-VASc score, we assumed that endocan level could be a new biomarker for stroke risk in patients with paroxysmal atrial fibrillation (PAF). It was examined that endocan could be an alternative to determine the risk of stroke and anticoagulation strategy in patients with PAF. The CHA2DS2-VASc scores were calculated for 192 patients with PAF, and their serum endocan levels were measured. The patients were divided into two groups as those with low to moderate (0-1) and those with high (≥ 2) CHA2DS2-VASc scores, and the endocan levels were compared between these two groups.
Results
The serum endocan level was significantly higher in the high CHA2DS2-VASc score group (p < 0.001). In the multivariate logistic regression analysis, endocan, C-reactive protein, and low-density lipoprotein were found to be independent determinants of the CHA2DS2-VASc score. The predictive value of endocan was analyzed using the ROC curve analysis, which revealed that endocan predicted a high stroke risk (CHA2DS2-VASc ≥ 2) at 82.5% sensitivity and 71.2% specificity at the cutoff value of 1.342.
Conclusion
This study indicates that endocan is significantly associated with CHA2DS2-VASc score. We demonstrated that endocan could be a new biomarker for the prediction of a high stroke risk among patients diagnosed with PAF.
Similar content being viewed by others
Background
Atrial fibrillation (AF) may cause various thromboembolic complications due to the effect of thrombogenic risk factors. It has an increasing incidence with age. It can manifest in various ways; thus, different classifications have been made. The American Heart Association and American College of Cardiology divided AF into four groups as intermittent paroxysmal AF (PAF) which may terminate spontaneously up to seven or with treatment, persistent AF that does not end after 7 days, long-lasting AF, lasting more than 12 months, and permanent AF in which rhythm control cannot be achieved but the treatment continues to control the heart [1]. AF causes serious mortality and morbidity with thromboembolic complications. The risk of stroke is five times greater in patients with AF, and the cause of a stroke in 20% of patients is AF [2]. Many studies have revealed no difference between PAF and persistent and permanent AF in terms of stroke [3, 4]. CHA2DS2-VASc is the most commonly used scoring system to determine the risk of stroke and anticoagulant therapy to prevent cerebrovascular events [5]. Anticoagulation is often recommended if the CHA2DS2-VASc score is ≥ 2. Although the guidelines lower recommendation anticoagulation for 0-1 points, this does not mean that the risk of stroke is very low [6]. Taking into account the bleeding status, there is no clear biochemical marker for the determination of the stroke risk and anticoagulation treatment decision other than scoring methods.
Endocan, formerly called endothelial cell-specific molecule-1 (ESM-1), is a proteoglycan molecule secreted from the heart, skin, kidneys, digestive system, lungs, liver, brain, lymph nodes, and the vascular endothelium of the thyroid gland [7].
Endocan has been accepted as an indicator of neovascularization, angiogenesis, and endothelial cell activation [8]. Endocan shows its effects by triggering the production of proinflammatory cytokines and regulating microvascular permeability and leukocyte adhesion [9]. The prognostic value of endocan has been demonstrated in inflammatory disorders, tumor progression, sepsis, transplant rejection, hypertension, and chronic kidney disease [10]. Similarly, a positive correlation has been identified between endocan and risk factors of cardiovascular events, such as hypertension, diabetes mellitus, and coronary artery disease [11, 12]. Many of these risk factors associated with endocan constitute the CHA2DS2-VASc score. In this regard, it is also possible to establish a close relationship between AF and endocan. When the literature is considered, this close relationship between CHA2DS2-VASc score and endocan level was not fully investigated. In this study, in order to determine the extent of this relationship, the serum endocan levels of patients with PAF were examined in relation to their CHA2DS2-VASc scores used to predict thromboembolic risk.
Methods
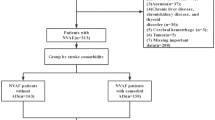
This study included a total of 192 patients presenting to our clinic with acute PAF, for whom rhythm control was achieved and a PAF attack was detected in the cardiac event recorder within 10 days but no electrophysiological procedure was performed. The CHA2DS2-VASc score was calculated for each patient as follows: + 1 point for congestive heart failure, + 1 point for hypertension, + 2 points for age ≥ 75 years, + 1 point for diabetes mellitus, + 2 points for a previous stroke/transient ischemic attack, + 1 point for vascular disease, + 1 point for age between 65 and 74 years, and + 1 point for female gender [5]. The patients with a CHA2DS2-VASc score of ≥ 2 were considered to have a high risk of stroke and evaluated in one group and those with a score of 0 and 1 were considered to have a low and moderate stroke risk, respectively, and evaluated in another group. Malignant diseases, history of acute myocardial infarction and cerebrovascular disease, renal disease, thyroid dysfunction, type 1 diabetes, pregnant women were excluded from the examination. High sensitivity C-reactive protein > 10 mg/dl and persistent or permanent AF subgroups were excluded as many comorbid conditions were accompanied by them.
Blood glucose, creatinine, complete blood count, serum lipid, total cholesterol, low-density lipoprotein cholesterol, high-density lipoprotein cholesterol (HDL-C), and triglyceride levels were measured from the blood samples taken from the antecubital vein after 12 h of fasting. For endocan, the blood samples taken from the same region were centrifuged at 2000 rpm for 15 min in a refrigerated centrifuge with a 30-min collection time. The separated serums were kept in a freezer at −80 °C. Twelve hours prior to laboratory analysis, the samples were allowed to defrost at + 4 °C. The samples were measured by enzyme-linked immunosorbent assay (ELISA) according to the manufacturer’s protocol (Shanghai Crystal Day Biotech Co Ltd., Shanghai, China), which has high sensitivity and specificity for detecting human endocan levels. The serum CRP levels (normal range 0-0.5) were measured by a nephelometric method (UniCel DxC 800 System, Beckman Coulter, Fullerton, CA, USA).
Statistical analyses were performed using the Statistical Package for the Social Sciences, version 20.0 (SPSS, Inc., Chicago, IL). The t test or the Mann-Whitney U test was used for continuous variables, and the data were expressed as mean ± standard deviation. Categorical variables were expressed as percentages and compared between the groups using the chi-square or Fisher’s exact test. The variables other than the components of the CHA2DS2-VASc score, which were found to be significant factors in the univariate analysis, were included in a multiple logistic regression analysis to determine the independent determinants of a high CHA2DS2-VAS score. A p value of < 0.05 was considered statistically significant. For the correlation analysis, Pearson’s and Spearman’s rank tests were conducted. Receiver operating characteristic (ROC) analyses were also undertaken to compare the performance power of endocan in determining the group with a high CHA2DS2-VASc score.
Results
As a result of this study conducted with a total of 192 patients with PAF (mean age, 60.43 ± 3.22 years, 51% men), the mean CHA2DS2-VASc scores were calculated as 4.92 ± 2.77 for the group with a high stroke risk (CHA2DS2-VASc ≥ 2) and 0.19 ± 0.08 for the group with a low to moderate stroke risk. The baseline characteristics of all the patients are shown in Table 1. As expected, in addition to the CHA2DS2-VASc score components, the LDL, CRP, and endocan levels were higher for the patients at high risk of stroke while their white blood cell was statistically significantly lower.
Using the univariate analysis, the variables showing with a high stroke risk positive or negative correlation were determined as white blood cell (r = −256, p = 0.002), LDL-C (r = 346, p < 0.001), CRP (r = 382, p < 0.001), and endocan (r = 301, p < 0.001). By excluding the CHA2DS2-VASc score components, the multivariate logistic regression analysis was conducted to identify the independent determinants of this score. LDL, CRP, and endocan (odds ratio, 1.862; 95% confidence interval, 1.358-4.064; p < 0.001) were found to be associated with a high CHA2DS2-VASc score after the potential confounding factors were adjusted (Table 2).
ROC curves were used to determine the ability of endocan to predict high CHA2DS2-VASc scores. The area under the curve for endocan was 0.793 (95% CI 0.694-0.892; p < 0.001). Using a cutoff value of 1.342 ng/mL, endocan predicted high CHA2DS2-VASc scores at a sensitivity of 82.5% and specificity of 71.2% (Fig. 1). The risk of stroke was significantly lower in patients with endocan values lower than 1.342 ng/mL compared to the study population.
Discussion
To the best of our knowledge, this is the first study to determine the close relationship between the serum endocan level and CHA2DS2-VASc score. Many studies have been conducted recently to investigate the relationship between cardiovascular diseases and endocan. It has been reported that in patients with acute myocardial infarction, an elevated level of endocan at the time of presentation to the hospital is an independent predictor of adverse cardiovascular outcomes, and it has also been independently associated with the severity of hypertensive coronary artery disease [13, 14]. Studies particularly focusing on the effects of cardiovascular diseases on the endothelium suggest that endocan may be a useful predictor of these diseases [15].
Risk factors, such as advancing age, hypertension, coronary heart disease, diabetes mellitus, valvular heart disease, heart failure, and hyperthyroidism cause structural changes in the heart resulting in the development of AF [16]. In fact, many conditions that cause vascular changes lead to the formation of AF, and several of these situations constitute the CHA2DS2-VASc score. On the other hand, many studies have shown that AF leads to endothelial dysfunction for many reasons, including increased shear stress, decreased nitric oxide bioavailability, increased oxidative stress, inflammation, and abnormalities of the renin-angiotensin system [17, 18]. As shown in a recently published meta-analysis, endocan released from endothelial cells increases in serum in disease that are components of the CHA2DS2-VASc score such as hypertension, diabetes, and coronary artery disease [19]. Similarly, we substantiated positive correlation between serum endocan level and CHA2DS2-VASc score in PAF patients.
Endothelial dysfunction mechanisms are closely related to the development of atrial cardiopathy [20]. It has been concluded that endothelial dysfunction, which is considered to develop as a result of AF, improves following the achievement of normal sinus rhythm [21, 22].
In addition, the detection of inflammatory infiltrates in the atrial and ventricular biopsies of patients with AF suggests that inflammation plays a role in AF [23]. Cox et al. reported that endocan played a significant role in endothelial dysfunction, since it regulated cell adhesion in inflammatory disorders [24]. Endothelial dysfunction and inflammatory damage mechanism caused by the components of the CHA2DS2-VASc score will lead to endocan release. Endothelial dysfunction, inflammatory damage seen in AF physiopathology, and indirect increased serum endocan level from components of the CHA2DS2-VASc score make it possible to observe a very close relationship between the CHA2DS2-VASc score and the endocan. In this study, a positive correlation was determined between endocan and the CHA2DS2-VASc score (≥ 2), an indicator of a high stroke risk, which includes a significant part of risk factors.
Chua et al. referred to the necessity of using biomarkers in AF and emphasized that markers, such as BNP and FGF-23 could be associated with AF [25]. There is not yet a biomarker predictive of thromboembolic complications. We determined a close relationship between CHA2DS2-VASc scores and endocan, which is an endothelium-specific marker. In addition, endocan was detected as an independent determinant of high CHA2DS2-VASc scores, which is an indicator of increased stroke risk in PAF in which many cardiovascular diseases may play a causative role.
The limitations of this study include the relatively small number of patients, observation nature of the study, and its lack of prospective validation. Also, the study is monocentric and does not comprise a large sample size.
Conclusion
The results of our study clearly demonstrate that increased serum endocan in patients with PAF is a parameter that predicts a high risk of stroke. The use of endocan as a biomarker in patients with PAF will provide more objective evidence for a high stroke risk.
Availability of data and materials
All data and materials of the study are available.
Abbreviations
- PAF:
-
Paroxysmal atrial fibrillation
- AF:
-
Atrial fibrillation
- ESM-1:
-
Endothelial cell-specific molecule-1
- HDL-C:
-
High-density lipoprotein cholesterol
References
January CT, Wann LS, Alpert JS et al (2014) ACC/AHA task force members. 2014 AHA/ACC/HRS guideline for the management of patients with atrial fibrillation: executive summary: a report of the American College of Cardiology/American Heart Association task force on practice guidelines and the Heart Rhythm Society. Circulation. 130(23):2071–2104
Kim TH, Yang PS, Kim D et al (2017) CHA2DS2-VASc score for identifying truly low-risk atrial fibrillation for stroke: a Korean Nationwide cohort study. Stroke. 48:2984–2990
Takabayashi K, Hamatani Y, Yamashita Y et al (2015) Incidence of stroke or systemic embolism in paroxysmal versus sustained atrial fibrillation: the Fushimi atrial fibrillation registry. Stroke. 46:3354–3361
Banerjee A, Taillandier S, Olesen JB et al (2013) Pattern of atrial fibrillation and risk of outcomes: the Loire Valley atrial fibrillation project. Int J Cardiol 167:2682–2687
Lip GY, Nieuwlaat R, Pisters R et al (2010) Refining clinical risk stratification for predicting stroke and thromboembolism in atrial fibrillation using a novel risk factor-based approach: the euro heart survey on atrial fibrillation. Chest 137:263–272
Kirchhof P, Benussi S, Kotecha D et al (2016) 2016 ESC guidelines for the management of atrial fibrillation developed in collaboration with EACTS. EurHeart J 37(38):2893–2962
Zhang SM, Zuo L, Zhou Q et al (2012) Expression and distribution of endocan in human tissues. Biotech Histochem 87:172–178
Kali A, Shetty KSR (2014) Endocan: a novel circulating proteoglycan. Indian J Pharm 46:579–583
Lee W, Ku S-K, Kim S-W et al (2014) Endocan elicits severe vascular inflammatory responses in vitro and in vivo. J Cell Physiol 229:620–630
Yilmaz MI, Siriopol D, Saglam M et al (2014) Plasma endocan levels associate with inflammation, vascular abnormalities, cardiovascular events, and survival in chronic kidney disease. Kidney Int 86:1213–1220
Wang XS, Yang W, Luo T et al (2015) Serum endocan levels are correlated with the presence and severity of coronary artery disease in patients with hypertension. Genet Test Mol Biomarkers 19(3):124–127
Balamir I, Ates I, Topcuoglu C et al (2018) Association of endocan, ischemia-modified albumin, and hsCRP levels with endothelial dysfunction in type 2 diabetes mellitus. Angiology. 69(7):609–616
Kundi H, Balun A, Cicekoglu H et al (2016) Admission endocan level may be a useful predictor for in-hospital mortality and coronary severity index in patients with ST segment elevation myocardial infarction. Angiology. 68:46–51
Xiong C, Zhao ZW, Chen ZY et al (2015) Elevated human endothelial cell-specific molecule-1 level and its association with coronary artery disease in patients with hypertension. J Invest Med 63:867–870
Balta S, Mikhailidis DP, Demirkol S et al (2015) Endocan: a novel inflammatory indicator in cardiovascular disease? Atherosclerosis. 243:339–343
Kirchhof P, Lip GY, Van Gelder IC et al (2012) Comprehensive risk reduction in patients with atrial fibrillation: emerging diagnostic and therapeutic options—a report from the 3rd atrial fibrillation competence NETwork/European heart rhythm association consensus conference. Europace 14:8–27
Cai H, Li Z, Goette A et al (2002) Downregulation of endocardial nitric oxide synthase expression and nitric oxide production in atrial fibrillation: potential mechanisms for atrial thrombosis and stroke. Circulation. 106:2854–2858
Guazzi M, Arena R (2009) Endothelial dysfunction and pathophysiological correlates in atrial fibrillation. Heart. 95:102–106
Zhao T, Kecheng Y, Zhao X et al (2018) The higher serum endocan levels may be a risk factor for the onset of cardiovascular disease: a meta-analysis. Medicine (Baltimore) 97:e13407
Wijesurendra RS (2015) Casadei B atrial fibrillation: effects beyond the atrium? Cardiovasc Res 105(3):238–247
Takahashi N, Ishibashi Y, Shimada T et al (2002) Impaired exercise-induced vasodilatation in chronic atrial fibrillation: role of endothelium-derived nitric oxide. Circ J 66:583–588
Skalidis EI, Zacharis EA, Tsetis DK et al (2007) Endothelial cell function during atrial fibrillation and after restoration of sinus rhythm. Am J Cardiol 99(9):1258–1262
Frustaci A, Chimenti C, Bellocci F et al (1997) Histological substrate of atrial biopsies in patients with lone atrial fibrillation. Circulation. 96(4):1180–1184
Cox LA, van Eijk LT, Ramakers BP et al (2015) Inflammation induced increases in plasma endocan levels are associated with endothelial dysfunction in humans in vivo. Shock. 43(4):322–326
Chua W, Purmah Y, Cardoso RV et al (2019) Data-driven discovery and validation of circulating blood-based biomarkers associated with prevalent atrial fibrillation. Eur Heart J 40(16):1268–1276
Acknowledgements
Not applicable in the manuscript.
Funding
There is no funding source to declare.
Author information
Authors and Affiliations
Contributions
Gökhan Ceyhun: Conceptualization, data curation, methodology, visualization, original draft, review and editing, supervision, original draft, resources, formal analysis. The author read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Erzurum Regional Education and Research Ethics Committee approved the study, and all the participants provided their written informed consent (Decision number: KAEK 2019/10-110).
Consent for publication
Not applicable in the manuscript.
Competing interests
The author declares no conflicts of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Ceyhun, G. The relationship of the serum endocan level with the CHA2DS2-VASc score in patients with paroxysmal atrial fibrillation. Egypt Heart J 73, 9 (2021). https://doi.org/10.1186/s43044-021-00132-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s43044-021-00132-1