Abstract
Objective
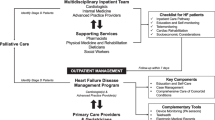
To evaluate the impact of comprehensive, multidisciplinary management programs on the process of care, resource utilization, health care costs, and clinical outcomes in patients with congestive heart failure.
Measurements and main results
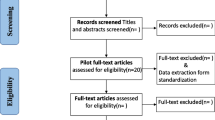
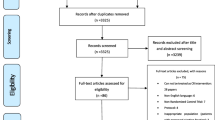
A MEDLINE search identified seven english-language reports that compared the process of care, clinical outcomes, or economic variables related to implementation of a multidisciplinary congestive heart failure management program of at least 3 month’s duration to a control or reference group. The primary intent of the programs was to emphasize compliance with recommended therapeutic principles, enhance patient education, and provide careful patient surveillance. Five of the studies reported improved functional status, aerobic capacity, or patient satisfaction. Six of the studies reported a 50% to 85% reduction in the risk of hospital admission. Three studies reported economic analyses with suggestive but not compelling evidence of financial benefit.
Conclusions
Comprehensive, multidisciplinary management programs for congestive heart failure can improve functional status and reduce the risk of hsspital admission, and they may lower medical costs.
Similar content being viewed by others
References
Captopril Multicenter Research Group. A placebo-controlled trial of refractory chronic congestive heart failure. J Am Coll Cardiol. 1983;2:755–63.
Packer M, Lee WH, Yushak M, Medina N. Comparison of captopril and enalapril in patients with severe chronic heart failure. N Engl J Med. 1986;315:847–53.
Kjekshus J, Swedberg K. Tolerability of enalapril in congestive heart failure. Am J Cardiol. 1988;62:A67–72.
The CONSENSUS Trial Study Group. Effects of enalapril on mortality in severe congestive heart failure: results of the Cooperative North Scandinavian Enalapril Survival Study. N Engl J Med. 1987;316:1429–35.
The SOLVD Investigators. Effect of enalapril on survival in patients with reduced left ventricular ejection fractions and congestive heart failure. N Engl J Med. 1991;325:293–302.
Rogers WJ, Johnstone DE, Yusuf S, et al. Quality of life among 5,025 patients with left ventricular dysfunction randomized between placebo and enalapril: the Studies of Left Ventricular Dysfunction. J Am Coll Cardiol. 1994;23:393–400.
Cohn JN, Johnson G, Zieshe S, et al. A comparison of enalapril with hydralazine-isosorbide in the treatment of chronic congestive heart failure. N Engl J Med. 1991;325:303–10.
Pfeffer MA, Braunwald E, Moye LA. et al. Effect of captopril on mortality and morbidity in patients with left ventricular dysfunction after myocardial infarction. N Engl J Med. 1992;327:669–77.
Philbin EF, Rocco TA. The utility of angiotensin-converting enzyme inhibitors in heart failure with preserved systolic function. Am Heart J. 1997;134:188–95.
Paul SD, Kuntz KM, Eagle KA, Weinstein NC. Costs and effectiveness of angiotensin converting enzyme inhibition in patients with congestive heart failure. Arch Intern Med. 1994;154:1143–9.
Konstam MA, Dracup K, Bottoroff MB. et al. Quick Reference Guide For Clinicians, No. 11: Heart Failure: Management of Patients with Left Ventricular Systolic Dysfunction. Rockville, Md: Agency for Health Care Policy and Research, Public Health Service, United States Department of Health and Human Services: 1994. AHCPR publication 94-0613.
Johnstone DE, Abdulla A, Arnold JMO. et al. Diagnosis and management of heart failure. Can J Cardiol. 1994;10:613–31.
The Digitalis Investigation Group. The effect of digoxin on mortality and morbidity in patients with heart failure. N Engl J Med. 1997;336:525–33.
Philbin EF, Rocco TA, Cotto M, Jenkins PL. Association between attenuated diuretic response and death in acute heart failure. Am J Cardiol. 1997;80:519–22.
Packer M, Bristow MR, Cohn JN. et al. The effect of carvedilol on morbidity and mortality in patients with chronic heart failure. N Engl J Med. 1996;334:1349–55.
Doval HC, Nul DR, Vancelli HO, Elizari M. Randomized trial of low-dose amiodarone in severe congestive heart failure. Lancet. 1994;344:493–8.
Costanzo MR, Augustine S, Bourge R. et al. Selection and treatment of candidates for heart transplantation: a statement for health professionals from the Committee on Heart Failure and Cardiac Transplantation of the Council on Clinical Cardiology. American Heart Association. Circulation. 1995;92:3593–612.
Killip T, Passamani E, Davis K. Coronary Artery Surgery Study (CASS): a randomized trial of coronary bypass surgery: eight years follow-up and survival in patients with reduced ejection fraction. Circulation. 1985;72(suppl V):V-102–9.
Smith W, McAnulty JH, Rahimtoola SH. Severe aortic stenosis with impaired left ventricular function and clinical heart failure: results of valve replacement. Circulation. 1978;58:258–64.
Moss AJ, Hall WJ, Cannom DS. et al. Improved survival with an implanted defibrillator in patients with coronary disease at high risk for ventricular arrhythmia. N Engl J Med. 1996;335:1933–40.
Domanski MJ, Garg R, Yusuf S. Prognosis in congestive heart failure. In: Hosenpud JD, Greenberg BH, eds. Congestive Heart Failure: Pathophysiology, Diagnosis and Comprehensive Approach to Management. New York, NY: Springer-Verlag; 1994:622–7.
Parmley W. Pathophysiology and current treatment of congestive heart failure. J Am Coll Cardiol. 1989;13:771–85.
Cardiology Preeminence Roundtable. Beyond Four Walls. Cost-Effective Management of Chronic Congestive Heart Failure. Washington, DC: The Advisory Board Company: 1994:39–47.
Krumholz HM, Parent EM, Tu N. et al. Readmission after hospitalization for congestive heart failure among Medicare beneficaries. Arch Intern Med. 1997;157:99–104.
Philbin EF, DiSalvo TG. Managed care for congestive heart failure: influence of payer status on process of care, resource utilization and clinical outcomes. Am Heart J. 1998;136:553–61.
Philbin EF, Lynch LJ, Rocco TA. et al. Does quality improvement work? The Management to Improve Survival in Congestive Heart Failure (MISCHF) Study. Jt Comm J Qual Improv. 1996;22: 721–33.
O’Connell JB, Bristow MR. Economic impact of heart failure in the United States: time for a different approach. J Heart Lung Transplant. 1994;13:S107–12.
Philbin EF, Andreou C, Rocco TA, Lynch LJ, Baker SL. Patterns of angiotensin-converting enzyme inhibitor use in congestive heart failure in two community hospitals. Am J Cardiol. 1996;77:832–8.
Philbin EF. Factors determining angiotensin-converting enzyme inhibitor use in heart failure in the community setting. Clin Cardiol. 1998;21:103–8.
Ashton CM, Kuykendall DH, Johnson ML, Wray NP, Wu L. The association between the quality of inpatient care and early readmission. Ann Intern Med. 1995;122:415–21.
Philbin EF, Rocco TA, Lynch LJ, Rogers VA, Jenkins P. Predictors and determinants of hospital length of stay in congestive heart failure in ten community hospitals. J Heart Lung Transplant. 1997;16:548–55.
Weingarten S, Riedinger M, Conner L, Johnson B. Reducing lengths of stay in the coronary care unit with a practice guideline for patients with congestive heart failure: insights from a controlled clinical trial. Med Care. 1994;32:1232–43.
Fonarow GC, Stevenson LW, Walden JA. et al. Impact of a comprehensive heart failure management program on hospital readmission and functional status of patients with advanced heart failure. J Am Coll Cardiol. 1997;30:725–32.
Kornowski R, Zeeli D, Averbuch M. et al. Intensive home-care surveillance prevents hospitalization and improves morbidity among elderly patients with severe congestive heart failure. Am Heart J. 1995;129:762–6.
Rich MW, Beckman V, Wittenberg C, Leven CL, Freedland KE Carney RM. A multidisciplinary intervention to prevent the readmission of elderly patients with congestive heart failure. N Engl J Med. 1995;333:1190–5.
Shah NB, Der E, Ruggerio C, Heidenreich PA, Massie BM. Prevention of hospitalizations for heart failure with an interactive home monitoring program. Am Heart J. 1998;135:373–8.
Tilney CK, Whiting SB, Horrar JL, Perkins BD, Vance RP, Reeves JD. Improved clinical and financial outcomes associated with a comprehensive congestive heart failure program. Dis Manage. 1998; 1:175–83.
Weinberger M, Oddone EZ, Henderson WG. Does increased access to primary care reduce hospital readmissions? N Engl J Med. 1996;334:1441–7.
West JA, Miller NH, Parker KM. et al. A comprehensive management system for heart failure improves clinical outcomes and reduces medical resource utilization. Am J Cardiol. 1997;79:58–63.
Edep ME, Shah NB, Tateo IM, Massie BM. Differences between primary care physicians and cardiologists in management of congestive heart failure: relation to practice guidelines. J Am Coll Cardiol. 1997;30:518–26.
Reis SE, Holubkov R, Edmundowicz D. et al. Treatment of patients admitted to the hospital with congestive heart failure: specialty-related disparities in practice patterns and outcomes. J Am Coll Cardiol. 1997;30:733–8.
Philbin EF, Weil HF, Erb T. Outcomes in heart failure based on specialty care. Circulation. 1996;94[8 suppl 1]: 1–50. Abstract.
Shah N, Edep M, Massie BM. Differences between cardiologists and heart failure specialists in the management of congestive heart failure. Circulation. 1995;92[suppl 1]: 1–666. Abstract.
Retchin SM, Brown B. Elderly patients with congestive heart failure under prepaid care. Am J Med. 1991;90:236–42.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Philbin, E.F. Comprehensive multidisciplinary programs for the management of patients with congestive heart failure. J Gen Intern Med 14, 130–135 (1999). https://doi.org/10.1046/j.1525-1497.1999.00291.x
Issue Date:
DOI: https://doi.org/10.1046/j.1525-1497.1999.00291.x