Abstract
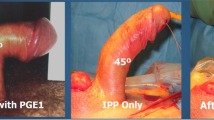
The aim of this study was to study the clinical effectiveness of a structured home modeling (HM) protocol in Peyronie’s disease (PD) patients who have residual curvature up to 45° after inflatable penile prosthesis (PP) placement. A total of 92 patients with PD and coexistent refractory erectile dysfunction received inflatable PP. If residual curvature after manual modeling (MM) was more than 45°, incision–grafting was performed. If curvature was <45° after MM, patients were instructed to perform HM daily for 6 months, after 4 weeks from PP implantation. The mean preoperative penile curvature was 39.4 ± 5.7° (30–60). Sixteen (17.4%) patients required incision–grafting and the remaining 76(82.6%) patients followed HM protocol. The mean postoperative residual curvature after MM was 29.7 ± 3.2° (5–50). Sixty-five (85.5%) patients who underwent HM had 10° or less residual curvature after 3 months and 72 (94.7%) patients had 10° or less residual curvature after 6 months. Seventy (92.1%) patients responded as satisfied or very satisfied on the questionnaire with the outcome after 6 months. HM of the penis over Inflatable PP may straighten the penis without the need for an additional surgical maneuver in vast majority of the PD patients having residual curvature of <45°.
Similar content being viewed by others
References
Hellstrom W. History, epidemiology, and clinical presentation of Peyronie’s disease. Int J Impot Res. 2003;15 Suppl 5:S91–2.
Sharma KL, Alom M, Trost L. The etiology of Peyronie’s disease: pathogenesis and genetic contributions. Sex Med Rev. 2020;8:314–23.
El-Khatib FM, Towe M, Yafi FA. Management of Peyronie’s disease with collagenase clostridium histolyticum in the acute phase. World J Urol. 2020;38:299–304.
Martínez-Salamanca JI, Egui A, Moncada I, Minaya J, Ballesteros CM, Del Portillo L. Acute phase peyronie’s disease management with traction device: a nonrandomized prospective controlled trial with ultrasound correlation. J Sex Med. 2014;11:506–15.
Anaissie J, Yafi FA. A review of surgical strategies for penile prosthesis implantation in patients with Peyronie’s disease. Transl Androl Urol. 2016;5:342–50.
Krishnappa P, Fernandez-Pascual E, Carballido J, Moncada I, Lledo-Garcia E, Martinez-Salamanca JI. Surgical management of Peyronie’s disease with co-existent erectile dysfunction. Sex Med. 2019;7:361e370.
Mulhall J, Ahmed A, Anderson M. Penile prosthetic surgery for Peyronie’s disease: defining the need for intraoperative adjuvant maneuvers. J Sex Med. 2004;1:318–21.
Wilson SK, Delk JR 2nd. A new treatment for Peyronie’s disease: modeling the penis over an inflatable penile prosthesis. J Urol. 1994;152:1121–3.
Levine LA, Burnett AL. Standard operating procedures for Peyronie’s disease. J Sex Med. 2013;10:230–44.
Hatzichristodoulou G, Tsambarlis P, Kübler H, Levine LA. Peyronie’s graft surgery-tips and tricks from the masters in andrologic surgery. Transl Androl Urol. 2017;6:645–56.
Chung E. Penile reconstructive surgery in Peyronie disease: challenges in restoring normal penis size, shape, and function. World J Mens Health. 2020;38:1–8.
Garaffa G, Minervini A, Christopher NA, Minhas S, Ralph DJ. The management of residual curvature after penile prosthesis implantation in men with Peyronie’s disease. BJU Int. 2011;108:1152–6.
Gelbard M, Goldstein I, Hellstrom WJ, McMahon CG, Smith T, Tursi J, et al. Clinical efficacy, safety and tolerability of collagenase clostridium histolyticum for the treatment of Peyronie disease in 2 large double-blind, randomized, placebo controlled phase 3 studies. J Urol. 2013;190:199–207.
Garaffa G, Kuehhas FE, De Luca F, Ralph DJ. Long-term results of reconstructive surgery for Peyronie’s disease. Sex Med Rev. 2015;3:113–21.
Hatzichristodoulou G, Osmonov D, Kübler H, Hellstrom WJG, Yafi FA. Contemporary review of grafting techniques for the surgical treatment of Peyronie’s disease. Sex Med Rev. 2017;5:544–52.
Rice PG, Somani BK, Rees RW. Twenty years of plaque incision and grafting for Peyronie’s disease: a review of literature. Sex Med. 2019;7:115–28.
Garcia-Gomez B, Ralph D, Levine L, Moncada-Iribarren I, Djinovic R, Albersen M, et al. Grafts for Peyronie’s disease: a comprehensive review. Andrology. 2018;6:117–26.
Terrier JE, Tal R, Nelson CJ, Mulhall JP. Penile sensory changes after plaque incision and grafting surgery for Peyronie’s disease. J Sex Med. 2018;15:1491–7.
Nehra A, Alterowitz R, Culkin DJ, Faraday MM, Hakim LS, Heidelbaugh JJ, et al. Peyronie’s disease: AUA guideline. J Urol. 2015;194:745–53.
Wilson SK, Delk JR, Mulcahy JJ, Cleves M, Salem EA. Upsizing of inflatable penile implant cylinders in patients with corporal fibrosis. J Sex Med. 2006;3:736–42.
Henry GD, Carrion R, Jennermann C, Wang R. Prospective evaluation of postoperative penile rehabilitation: penile length/girth maintenance 1 year following Coloplast Titan inflatable penile prosthesis. J Sex Med. 2015;12:1298–304.
Chung PH, Siegel JA, Tausch TJ, Klein AK, Scott JM, Morey AF. Inflatable penile prosthesis as tissue expander: what is the evidence? Int Braz J Urol. 2017;43:911–6.
Valenzuela R, Ziegelmann M, Tokar S, Hillelsohn J. The use of penile traction therapy in the management of Peyronie’s disease: current evidence and future prospects. Ther Adv Urol. 2019;11:1756287219838139. https://doi.org/10.1177/1756287219838139.
Moncada I, Krishnappa P, Romero J, Torremade J, Fraile A, Martinez-Salamanca JI, et al. Penile traction therapy with the new device ‘Penimaster PRO’ is effective and safe in the stable phase of Peyronie’s disease: a controlled multicentre study. BJU Int. 2019;123:694–702.
Hatzimouratidis K, Giuliano F, Moncada I, Muneer A, Salonia A, Verze P. EAU guidelines: male sexual dysfunction [Internet]. Uroweb. http://uroweb.org/guideline/male-sexual-dysfunction/. Accessed 1 Oct 2019.
Alenghat FJ, Ingber DE. Mechanotransduction: all signals point to cytoskeleton, matrix, and integrins. Sci STKE. 2002;2002:pe6.
Ilizarov GA, Soĭbel’man LM. Clinical and experimental data on bloodless lengthening of lower extremities. Eksp Khir Anesteziol. 1969;14:27–32.
Alman BA, Greel DA, Ruby LK, Goldberg MJ, Wolfe HJ. Regulation of proliferation and platelet-derived growth factor expression in palmar fibromatosis (Dupuytren contracture) by mechanical strain. J Orthop Res. 1996;14:722–8.
Chung E, De Young L, Brock GB. Penile traction and Peyronie’s disease: in-vitro analysis of the efficacy of traction on cellular changes in Peyronie’s plaque in a strain culture system. J Sex Med. 2012;9(Suppl 2):130.
Ziegelmann MJ, Viers BR, McAlvany KL, Bailey GC, Savage JB, Trost LW. Restoration of penile function and patient satisfaction with intralesional collagenase clostridium histolyticum injection for Peyronie’s disease. J Urol. 2016;195:1051–6.
Author information
Authors and Affiliations
Contributions
All authors have: conceived and/or designed the work that led to the submission, acquired data, and/or played an important role in interpreting the results; drafted or revised the paper; approved the final version; agreed to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Moncada, I., Krishnappa, P., Ascencios, J. et al. Home modeling after penile prosthesis implantation in the management of residual curvature in Peyronie’s disease. Int J Impot Res 33, 616–619 (2021). https://doi.org/10.1038/s41443-020-0325-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41443-020-0325-6
- Springer Nature Limited
This article is cited by
-
Residual penile curvature correction by modeling during penile prosthesis implantation in Peyronie’s disease patients
International Journal of Impotence Research (2023)