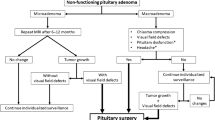
Key Points
-
Many patients previously treated for pituitary tumours have chronic, multisystem morbidity in addition to hypopituitarism
-
Many patients previously treated for pituitary tumours with visual-field defects have hypothalamic dysfunction that is associated with morbidity and mortality
-
Many patients appropriately treated for acromegaly have chronic morbidity owing to irreversible effects of previous excess of growth hormone and insulin-like growth factor 1
-
Many patients adequately treated for Cushing disease have morbidity and an increased risk of death owing to irreversible effects of previous cortisol excess
Abstract
Ultimately, almost all patients who are appropriately treated for pituitary tumours enter a chronic phase with control or cure of hormonal excess, adequate treatment of pituitary insufficiency and relief of mass effects. This phase is associated with improvement of initial signs and symptoms, but also with the persistent consequences of the initial disease and associated treatments. Pituitary insufficiency is a common denominator in many of these patients, and is associated with a reduction in quality of life, despite adequate endocrine substitution. Hypothalamic dysfunction can be present in patients previously treated for visual impairments caused by large suprasellar adenomas, or craniopharyngiomas. In addition to hypopituitarism, these patients can have multisystem morbidities caused by altered hypothalamic function, including weight gain and disturbed regulation of sleep–wake cycles. Mortality can also be affected. Patients cured of Cushing disease or acromegaly have chronic multisystem morbidities (in the case of Cushing disease, also affecting mortality) caused by irreversible effects of the previous excesses of cortisol in Cushing disease and growth hormone and insulin-like growth factor 1 in acromegaly. In addition to early diagnosis and treatment of pituitary tumours, research should focus on the amenability of these chronic post-treatment syndromes to therapeutic intervention, to improve quality of life and clinical outcomes.

Similar content being viewed by others
References
Sudhakar, N., Ray, A. & Vafidis, J. A. Complications after trans-sphenoidal surgery: our experience and a review of the literature. Br. J. Neurosurg. 18, 507–512 (2004).
Loeffler, J. S. & Shih, H. A. Radiation therapy in the management of pituitary adenomas. J. Clin. Endocrinol. Metab. 96, 1992–2003 (2011).
van der Klaauw, A. A. et al. Disease-specific impairments in quality of life during long-term follow-up of patients with different pituitary adenomas. Clin. Endocrinol. (Oxf.) 69, 775–784 (2008).
Romijn, J. A., Smit, J. W. & Lamberts, S. W. Intrinsic imperfections of endocrine replacement therapy. Eur. J. Endocrinol. 149, 91–97 (2003).
Filipsson, H., Monson, J. P., Koltowska-Häggström, M., Mattsson, A. & Johannsson, G. The impact of glucocorticoid replacement regimens on metabolic outcome and comorbidity in hypopituitary patients. J. Clin. Endocrinol. Metab. 91, 3954–3961 (2006).
Zueger, T. et al. Glucocorticoid replacement and mortality in patients with nonfunctioning pituitary adenoma. J. Clin. Endocrinol. Metab. 97, E1938–E1942 (2012).
Carvalho, P., Lau, E. & Carvalho, D. Surgery induced hypopituitarism in acromegalic patients: a systematic review and meta-analysis of the results. Pituitary 18, 844–860 (2015).
Heald, A. H. et al. Long-term negative impact on quality of life in patients with successfully treated Cushing's disease. Clin. Endocrinol. (Oxf.) 61, 458–465 (2004).
Minniti, G. et al. The long-term efficacy of conventional radiotherapy in patients with GH-secreting pituitary adenomas. Clin. Endocrinol. (Oxf.) 62, 210–216 (2005).
Minniti, G. et al. Fractionated stereotactic radiotherapy for large and invasive non-functioning pituitary adenomas: long-term clinical outcomes and volumetric MRI assessment of tumor response. Eur. J. Endocrinol. 172, 433–441 (2015).
González, B. et al. Health-related quality of life in patients with nonfunctioning pituitary adenomas undergoing postoperative radiation therapy: a case–control study. Endocr. Pract. 22, 540–545 (2016).
van Beek, A. P. et al. Radiotherapy is not associated with reduced quality of life and cognitive function in patients treated for nonfunctioning pituitary adenoma. Int. J. Radiat. Oncol. Biol. Phys. 68, 986–991 (2007).
van der Klaauw, A. A., Biermasz, N. R., Hoftijzer, H. C., Pereira, A. M. & Romijn, J. A. Previous radiotherapy negatively influences quality of life during 4 years of follow-up in patients cured from acromegaly. Clin. Endocrinol. (Oxf.) 69, 123–128 (2008).
Olsson, D. S., Andersson, E., Bryngelsson, I. L., Nilsson, A. G. & Johannsson, G. Excess mortality and morbidity in patients with craniopharyngioma, especially in patients with childhood onset: a population-based study in Sweden. J. Clin. Endocrinol. Metab. 100, 467–474 (2015).
Olsson, D. S. et al. Excess mortality in women and young adults with nonfunctioning pituitary adenoma: a Swedish nationwide study. J. Clin. Endocrinol. Metab. 100, 2651–2658 (2015).
Dekkers, O. M., Pereira, A. M. & Romijn, J. A. Treatment and follow-up of clinically nonfunctioning pituitary macroadenomas. J. Clin. Endocrinol. Metab. 93, 3717–3726 (2008).
Dekkers, O. M. et al. Quality of life is decreased after treatment for nonfunctioning pituitary macroadenoma. J. Clin. Endocrinol. Metab. 91, 3364–3369 (2006).
Saper, C. B., Scammell, T. E. & Lu, J. Hypothalamic regulation of sleep and circadian rhythms. Nature 437, 1257–1263 (2005).
van der Klaauw, A. A. et al. Patients cured from craniopharyngioma or nonfunctioning pituitary macroadenoma (NFMA) suffer similarly from increased daytime somnolence despite normal sleep patterns compared to healthy controls. Clin. Endocrinol. (Oxf.) 69, 769–774 (2008).
Biermasz, N. R. et al. Patients previously treated for nonfunctioning pituitary macroadenomas have disturbed sleep characteristics, circadian movement rhythm, and subjective sleep quality. J. Clin. Endocrinol. Metab. 96, 1524–1532 (2011).
Joustra, S. D., Kruijssen, E., Verstegen, M. J., Pereira, A. M. & Biermasz, N. R. Determinants of altered sleep-wake rhythmicity in patients treated for nonfunctioning pituitary macroadenomas. J. Clin. Endocrinol. Metab. 99, 4497–4505 (2014).
Edgar, D. M., Dement, W. C. & Fuller, C. A. Effect of SCN lesions on sleep in squirrel monkeys: evidence for opponent processes in sleep-wake regulation. J. Neurosci. 13, 1065–1079 (1993).
Romeijn, N. et al. Medical history of optic chiasm compression in patients with pituitary insufficiency affects skin temperature and its relation to sleep. Chronobiol. Int. 29, 1098–1108 (2012).
Borgers, A. J. et al. Arginine vasopressin immunoreactivity is decreased in the hypothalamic suprachiasmatic nucleus of subjects with suprasellar tumors. Brain Pathol. 23, 440–444 (2013).
Joustra, S. D. et al. Alterations in diurnal rhythmicity in patients treated for nonfunctioning pituitary macroadenoma: a controlled study and literature review. Eur. J. Endocrinol. 171, 217–228 (2014).
Joustra, S. D. et al. High prevalence of metabolic syndrome features in patients previously treated for nonfunctioning pituitary macroadenoma. PLoS ONE 9, e90602 (2014).
Tomlinson, J. W. et al. Association between premature mortality and hypopituitarism. Lancet 357, 425–431 (2001).
Müller, H. L. Craniopharyngioma. Endocr. Rev. 35, 513–543 (2014).
Pereira, A. M. et al. High prevalence of long-term cardiovascular, neurological and psychosocial morbidity after treatment for craniopharyngioma. Clin. Endocrinol. (Oxf.) 62, 197–204 (2005).
Karavitaki, N. et al. Craniopharyngiomas in children and adults: systematic analysis of 121 cases with long-term follow-up. Clin. Endocrinol. (Oxf.) 62, 397–409 (2005).
Honegger, J., Buchfelder, M. & Fahlbusch, R. Surgical treatment of craniopharyngiomas: endocrinological results. J. Neurosurg. 90, 251–257 (1999).
Verhelst, J. et al. Baseline characteristics and response to 2 years of growth hormone (GH) replacement of hypopituitary patients with GH deficiency due to adult-onset craniopharyngioma in comparison with patients with nonfunctioning pituitary adenoma: data from KIMS (Pfizer International Metabolic Database). J. Clin. Endocrinol. Metab. 90, 4636–4643 (2005).
Yuen, K. C. et al. Primary treatment regimen and diabetes insipidus as predictors of health outcomes in adults with childhood-onset craniopharyngioma. J. Clin. Endocrinol. Metab. 99, 1227–1235 (2014).
Dekkers, O. M. et al. Quality of life in treated adult craniopharyngioma patients. Eur. J. Endocrinol. 154, 483–489 (2006).
Sterkenburg, A. S. et al. Survival, hypothalamic obesity, and neuropsychological/psychosocial status after childhood-onset craniopharyngioma: newly reported long-term outcomes. Neuro Oncol. 17, 1029–1038 (2015).
Poretti, A., Grotzer, M. A., Ribi, K., Schönle, E. & Boltshauser, E. Outcome of craniopharyngioma in children: long-term complications and quality of life. Dev. Med. Child. Neurol. 46, 220–229 (2004).
Gautier, A. et al. Markers of recurrence and long-term morbidity in craniopharyngioma: a systematic analysis of 171 patients. J. Clin. Endocrinol. Metab. 97, 1258–1267 (2012).
Pickering, L. et al. Sleep–wake and melatonin pattern in craniopharyngioma patients. Eur. J. Endocrinol. 170, 873–884 (2014).
Müller, H. L. et al. Melatonin treatment in obese patients with childhood craniopharyngioma and increased daytime sleepiness. Cancer Causes Control 17, 583–589 (2006).
Roth, C. L. et al. Semiquantitative analysis of hypothalamic damage on MRI predicts risk for hypothalamic obesity. Obesity (Silver Spring) 23, 1226–1233 (2015).
Kim, R. J. et al. Energy expenditure in obesity associated with craniopharyngioma. Childs Nerv. Syst. 26, 913–917 (2010).
Harz, K. J., Müller, H. L., Waldeck, E., Pudel, V. & Roth, C. Obesity in patients with craniopharyngioma: assessment of food intake and movement counts indicating physical activity. J. Clin. Endocrinol. Metab. 88, 5227–5231 (2003).
Shaikh, M. G., Grundy, R. G. & Kirk, J. M. Reductions in basal metabolic rate and physical activity contribute to hypothalamic obesity. J. Clin. Endocrinol. Metab. 93, 2588–2593 (2008).
Holmer, H. et al. Reduced energy expenditure and impaired feeding-related signals but not high energy intake reinforces hypothalamic obesity in adults with childhood onset craniopharyngioma. J. Clin. Endocrinol. Metab. 95, 5395–5402 (2010).
Hoffmann, A. et al. Nonalcoholic fatty liver disease and fatigue in long-term survivors of childhood-onset craniopharyngioma. Eur. J. Endocrinol. 173, 389–397 (2015).
Daubenbüchel, A. M. et al. Hydrocephalus and hypothalamic involvement in pediatric patients with craniopharyngioma or cysts of Rathke's pouch: impact on long-term prognosis. Eur. J. Endocrinol. 172, 561–569 (2015).
Sherlock, M. et al. Mortality in patients with pituitary disease. Endocr. Rev. 31, 301–342 (2010).
Holdaway, I. M., Bolland, M. J. & Gamble, G. D. A meta-analysis of the effect of lowering serum levels of GH and IGF-I on mortality in acromegaly. Eur. J. Endocrinol. 159, 89–95 (2008).
Jallad, R. S., Musolino, N. R., Salgado, L. R. & Bronstein, M. D. Treatment of acromegaly with octreotide-LAR: extensive experience in a Brazilian institution. Clin. Endocrinol. (Oxf.) 63, 168–175 (2005).
Sesmilo, G. et al. Escape and lipodystrophy in acromegaly during pegvisomant therapy, a retrospective multicentre Spanish study. Clin. Endocrinol. (Oxf.) 81, 883–890 (2014).
Ronchi, C. L. et al. Prevalence of GH deficiency in cured acromegalic patients: impact of different previous treatments. Eur. J. Endocrinol. 161, 37–42 (2009).
van der Klaauw, A. A. et al. Limited effects of growth hormone replacement in patients with GH deficiency during long-term cure of acromegaly. Pituitary 12, 339–346 (2009).
Giavoli, C. et al. GH replacement improves quality of life and metabolic parameters in cured acromegalic patients with growth hormone deficiency. J. Clin. Endocrinol. Metab. 97, 3983–3988 (2012).
Imran, S. A. et al. Morphometric changes correlate with poor psychological outcomes in patients with acromegaly. Eur. J. Endocrinol. 174, 41–50 (2016).
Biermasz, N. R., Pereira, A. M., Smit, J. W., Romijn, J. A. & Roelfsema, F. Morbidity after long-term remission for acromegaly: persisting joint-related complaints cause reduced quality of life. J. Clin. Endocrinol. Metab. 90, 2731–2739 (2005).
Sievers, C. et al. Prevalence of mental disorders in acromegaly: a cross-sectional study in 81 acromegalic patients. Clin. Endocrinol. (Oxf.) 71, 691–701 (2009).
Fatti, L. M., Scacchi, M., Pincelli, A. I., Lavezzi, E. & Cavagnini, F. Prevalence and pathogenesis of sleep apnea and lung disease in acromegaly. Pituitary 4, 259–262 (2001).
Herrmann, B. L. et al. Effects of octreotide on sleep apnoea and tongue volume (magnetic resonance imaging) in patients with acromegaly. Eur. J. Endocrinol. 151, 309–315 (2004).
Davi', M. V. et al. Sleep apnoea syndrome is highly prevalent in acromegaly and only partially reversible after biochemical control of the disease. Eur. J. Endocrinol. 159, 533–540 (2008).
Castellani, C. et al. Morphological study of upper airways and long-term follow-up of obstructive sleep apnea syndrome in acromegalic patients. Endocrine 51, 308–316 (2016).
Morgenstern, M. et al. Obstructive sleep apnea: an unexpected cause of insulin resistance and diabetes. Endocrinol. Metab. Clin. North. Am. 43, 187–204 (2014).
Zamarrón, C., Valdés Cuadrado, L. & Alvarez-Sala, R. Pathophysiologic mechanisms of cardiovascular disease in obstructive sleep apnea syndrome. Pulm. Med. 2013, 521087 (2013).
Lombardi, G., Galdiero, M., Auriemma, R. S., Pivonello, R. & Colao, A. Acromegaly and the cardiovascular system. Neuroendocrinology 83, 211–217 (2006).
Colao, A. et al. Reversal of acromegalic cardiomyopathy in young but not in middle-aged patients after 12 months of treatment with the depot long-acting somatostatin analogue octreotide. Clin. Endocrinol. (Oxf.) 58, 169–176 (2003).
Colao, A. et al. High prevalence of cardiac valve disease in acromegaly: an observational, analytical, case–control study. J. Clin. Endocrinol. Metab. 88, 3196–3201 (2003).
Pereira, A. M. et al. Increased prevalence of regurgitant valvular heart disease in acromegaly. J. Clin. Endocrinol. Metab. 89, 71–75 (2004).
van der Klaauw, A. A. et al. Increased aortic root diameters in patients with acromegaly. Eur. J. Endocrinol. 159, 97–103 (2008).
Casini, A. F. et al. Aortic root ectasia in patients with acromegaly: experience at a single center. Clin. Endocrinol. (Oxf.) 75, 495–500 (2011).
Fieffe, S. et al. Diabetes in acromegaly, prevalence, risk factors, and evolution: data from the French Acromegaly Registry. Eur. J. Endocrinol. 164, 877–884 (2011).
Colao, A. et al. GH and IGF-I excess control contributes to blood pressure control: results of an observational, retrospective, multicentre study in 105 hypertensive acromegalic patients on hypertensive treatment. Clin. Endocrinol. (Oxf.) 69, 613–620 (2008).
Oshino, S. et al. Prevalence of cerebral aneurysm in patients with acromegaly. Pituitary 16, 195–201 (2013).
Manara, R. et al. Increased rate of intracranial saccular aneurysms in acromegaly: an MR angiography study and review of the literature. J. Clin. Endocrinol. Metab. 96, 1292–1300 (2011).
Celik, O., Akhan, S. E., Hatipoglu, E. & Kadioglu, P. Increased incidence of pelvic organ prolapse in women with acromegaly. Eur. J. Obstet. Gynecol. Reprod. Biol. 183, 44–47 (2014).
Renehan, A. G. et al. Determination of large bowel length and loop complexity in patients with acromegaly undergoing screening colonoscopy. Clin. Endocrinol. (Oxf.) 62, 323–330 (2005).
Wassenaar, M. J. et al. Acromegaly is associated with an increased prevalence of colonic diverticula: a case–control study. J. Clin. Endocrinol. Metab. 95, 2073–2079 (2010).
Dworakowska, D. et al. Repeated colonoscopic screening of patients with acromegaly: 15-year experience identifies those at risk of new colonic neoplasia and allows for effective screening guidelines. Eur. J. Endocrinol. 163, 21–28 (2010).
Lois, K. et al. The role of colonoscopic screening in acromegaly revisited: review of current literature and practice guidelines. Pituitary 18, 568–574 (2015).
Wassenaar, M. J. et al. Arthropathy in long-term cured acromegaly is characterised by osteophytes without joint space narrowing: a comparison with generalised osteoarthritis. Ann. Rheum. Dis. 70, 320–325 (2011).
Karkucak, M. et al. Ultrasonographic measurement of femoral cartilage thickness in acromegalic patients. Clin. Rheumatol. 34, 157–161 (2015).
Biermasz, N. R. et al. Automated image analysis of hand radiographs reveals widened joint spaces in patients with long-term control of acromegaly: relation to disease activity and symptoms. Eur. J. Endocrinol. 166, 407–413 (2012).
Claessen, K. M. et al. Two phenotypes of arthropathy in long-term controlled acromegaly? A comparison between patients with and without joint space narrowing (JSN). Growth Horm. IGF Res. 23, 159–164 (2013).
Mazziotti, G. et al. Bone turnover, bone mineral density, and fracture risk in acromegaly: a meta-analysis. J. Clin. Endocrinol. Metab. 100, 384–394 (2015).
Claessen, K. M. et al. Progression of vertebral fractures despite long-term biochemical control of acromegaly: a prospective follow-up study. J. Clin. Endocrinol. Metab. 98, 4808–4815 (2013).
Mazziotti, G. et al. Vertebral fractures in patients with acromegaly: a 3-year prospective study. J. Clin. Endocrinol. Metab. 98, 3402–3410 (2013).
Claessen, K. M., Mazziotti, G., Biermasz, N. R. & Giustina, A. Bone and joint disorders in acromegaly. Neuroendocrinology 103, 86–95 (2016).
Rees, D. A. et al. Long-term follow-up results of transsphenoidal surgery for Cushing's disease in a single centre using strict criteria for remission. Clin. Endocrinol. (Oxf.) 56, 541–551 (2002).
van Aken, M. O. et al. Quality of life in patients after long-term biochemical cure of Cushing's disease. J. Clin. Endocrinol. Metab. 90, 3279–3286 (2005).
Guerin, C. et al. Bilateral adrenalectomy in the 21st century: when to use it for hypercortisolism? Endocr. Relat. Cancer 23, R131–R142 (2016).
Pereira, A. M., Tiemensma, J. & Romijn, J. A. Neuropsychiatric disorders in Cushing's syndrome. Neuroendocrinology 92 (Suppl. 1), 65–70 (2010).
Tiemensma, J. et al. Subtle cognitive impairments in patients with long-term cure of Cushing's disease. J. Clin. Endocrinol. Metab. 95, 2699–2714 (2010).
Bas-Hoogendam, J. M. et al. Altered neural processing of emotional faces in remitted Cushing's disease. Psychoneuroendocrinology 59, 134–146 (2015).
van der Werff, S. J. et al. Resting-state functional connectivity in patients with long-term remission of Cushing's disease. Neuropsychopharmacology 40, 1888–1898 (2015).
van der Werff, S. J. et al. Widespread reductions of white matter integrity in patients with long-term remission of Cushing's disease. Neuroimage Clin. 4, 659–667 (2014).
Crespo, I. et al. Impaired decision-making and selective cortical frontal thinning in Cushing's syndrome. Clin. Endocrinol. (Oxf.) 81, 826–833 (2014).
Andela, C. D. et al. Mechanisms in endocrinology: Cushing's syndrome causes irreversible effects on the human brain: a systematic review of structural and functional magnetic resonance imaging studies. Eur. J. Endocrinol. 173, R1–R14 (2015).
Sapolsky, R. M. Glucocorticoids and hippocampal atrophy in neuropsychiatric disorders. Arch. Gen. Psychiatry. 57, 925–935 (2000).
Nieman, L. K. et al. Treatment of Cushing's syndrome: an endocrine society clinical practice guideline. J. Clin. Endocrinol. Metab. 100, 2807–2831 (2015).
Tiemensma, J. et al. Drawings reflect a new dimension of the psychological impact of long-term remission of Cushing's syndrome. J. Clin. Endocrinol. Metab. 97, 3123–3131 (2012).
Barahona, M. J. et al. Persistent body fat mass and inflammatory marker increases after long-term cure of Cushing's syndrome. J. Clin. Endocrinol. Metab. 94, 3365–3371 (2009).
Wagenmakers, M. et al. Persistent centripetal fat distribution and metabolic abnormalities in patients in long-term remission of Cushing's syndrome. Clin. Endocrinol. (Oxf.) 82, 180–187 (2015).
Pereira, A. M. et al. Cardiac dysfunction is reversed upon successful treatment of Cushing's syndrome. Eur. J. Endocrinol. 162, 331–340 (2010).
Kamenický, P. et al. Cardiac structure and function in Cushing's syndrome: a cardiac magnetic resonance imaging study. J. Clin. Endocrinol. Metab. 99, E2144–E2153 (2014).
Neary, N. M. et al. Hypercortisolism is associated with increased coronary arterial atherosclerosis: analysis of noninvasive coronary angiography using multidetector computerized tomography. J. Clin. Endocrinol. Metab. 98, 2045–2052 (2013).
Santos, A. et al. Cardiovascular risk and white matter lesions after endocrine control of Cushing's syndrome. Eur. J. Endocrinol. 173, 765–775 (2015).
Colao, A. et al. Persistence of increased cardiovascular risk in patients with Cushing's disease after five years of successful cure. J. Clin. Endocrinol. Metab. 84, 2664–2672 (1999).
Dekkers, O. M. et al. Multisystem morbidity and mortality in Cushing's syndrome: a cohort study. J. Clin. Endocrinol. Metab. 98, 2277–2284 (2013).
Verdelho, A. et al. Differential impact of cerebral white matter changes, diabetes, hypertension and stroke on cognitive performance among non-disabled elderly. The LADIS study. J. Neurol. Neurosurg. Psychiatry 78, 1325–1330 (2007).
van Haalen, F. M., Broersen, L. H., Jorgensen, J. O., Pereira, A. M. & Dekkers, O. M. Management of endocrine disease: mortality remains increased in Cushing's disease despite biochemical remission: a systematic review and meta-analysis. Eur. J. Endocrinol. 172, R143–R149 (2015).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The author declares no competing financial interests.
PowerPoint slides
Rights and permissions
About this article
Cite this article
Romijn, J. The chronic syndromes after previous treatment of pituitary tumours. Nat Rev Endocrinol 12, 547–556 (2016). https://doi.org/10.1038/nrendo.2016.84
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrendo.2016.84
- Springer Nature Limited
This article is cited by
-
Hypothalamic syndrome
Nature Reviews Disease Primers (2022)
-
Metabolic syndrome and its components in adult hypopituitary patients
Pituitary (2020)
-
Cardiovascular autonomic dysfunction in patients with idiopathic diabetes insipidus
Pituitary (2018)