Abstract
Background
To improve physical function, physical activity (PA) guidelines for older adults recommend completing PA in bouts of 10 min or more. Spontaneous PA (< 10 min) can also benefit older adults. However, a paucity of research exists examining if shorter bouts of PA are associated with greater physical function.
Aim
To determine the association between various patterns of PA and the likelihood of greater physical function in older adults.
Methods
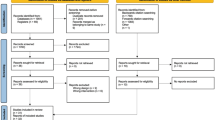
Older adults from the 2003–2004 and 2005–2006 cycles of the National Health and Nutrition Examination Survey were included for analysis. PA lasting 1, 5, 10, 30, and 60 min was quantified using accelerometers. Physical function was assessed using a Likert scale reflecting the self-reported capability to complete 11 tasks. A single function score was then computed using factor analysis. Logistic regression analyses calculated the association between PA bout length and the likelihood of above average function.
Results
PA performed in 1-min (odds ratio [OR] 1.02; 95% confidence interval [CI] 1.01–1.03), 5-min (OR 1.02; CI 1.01–1.03), or 10-min bouts (OR 1.02; CI 1.01–1.03) was associated with greater physical function following adjustment for confounders. When scaled to represent an accumulation of 10 min of MVPA, likelihoods increased for both 1-min ([OR] 1.25; 95% [CI] 1.11–1.39) and 5-min (OR 1.22; 95% CI 1.08–1.37) bouts.
Discussion/conclusions
Our findings suggest bouts of PA lasting 10 min or shorter in duration are associated with greater physical function in older adults.

Similar content being viewed by others
References
Martinez-Gomez D, Bandinelli S, Del-Panta V et al (2017) Three-year changes in physical activity and decline in physical performance over 9 years of follow-up in older adults: The Invecchiare in Chianti Study. J Am Geriatr Soc 65:1176–1182. https://doi.org/10.1111/jgs.14788
Visser M, Simonsick EM, Colbert LH et al (2005) Type and intensity of activity and risk of mobility limitation: the mediating role of muscle parameters. J Am Geriatr Soc 53:762–770. https://doi.org/10.1111/j.1532-5415.2005.53257.x
Miller ME, Rejeski WJ, Reboussin BA et al (2015) Physical activity, functional limitations, and disability in older adults. J Am Geriatr Soc 48:1264–1272. https://doi.org/10.1111/j.1532-5415.2000.tb02600.x
Guralnik JM, Alecxih L, Branch LG et al (2002) Medical and long-term care costs when older persons become more dependent. Am J Public Health 92:1244–1245
Santos DA, Silva AM, Baptista F et al (2012) Sedentary behavior and physical activity are independently related to functional fitness in older adults. Exp Gerontol 47:908–912. https://doi.org/10.1016/j.exger.2012.07.011
World Health Organization (2010) Global recommendations on physical activity for health. WHO Press
Tremblay MS, Warburton DER, Janssen I et al (2011) New canadian physical activity guidelines. Appl Physiol Nutr Metab 36:36–46. https://doi.org/10.1139/H11-009
Colley RC, Garriguet D, Janssen I et al (2011) Physical activity of Canadian adults: accelerometer results from the 2007 to 2009 Canadian Health Measures Survey. Health Rep 22:7–14
Watson KB (2016) Physical inactivity among adults aged 50 years and older—United States, 2014. MMWR. https://doi.org/10.15585/mmwr.mm6536a3
Chau J, Chey T, Burks-Young S et al (2017) Trends in prevalence of leisure time physical activity and inactivity: results from Australian National Health Surveys 1989–2011. Aust N Z J Public Health 41:617–624. https://doi.org/10.1111/1753-6405.12699
Piercy KL, Troiano RP, Ballard RM et al (2018) The physical activity guidelines for Americans. JAMA 320:2020–2028. https://doi.org/10.1001/jama.2018.14854
Kehler DS, Clara I, Hiebert B et al (2018) The association between bouts of moderate to vigorous physical activity and patterns of sedentary behavior with frailty. Exp Gerontol 104:28–34. https://doi.org/10.1016/j.exger.2018.01.014
Jefferis BJ, Parsons TJ, Sartini C et al (2018) Objectively measured physical activity, sedentary behaviour and all-cause mortality in older men: does volume of activity matter more than pattern of accumulation. Br J Sports Med. https://doi.org/10.1136/bjsports-2017-098733
Matthews CE, Chen KY, Freedson PS et al (2008) Amount of time spent in sedentary behaviors in the United States, 2003–2004. Am J Epidemiol 167:875–881. https://doi.org/10.1093/aje/kwm390
Sardinha LB, Santos DA, Silva AM et al (2015) Breaking-up sedentary time is associated with physical function in older adults. J Gerontol Ser A 70:119–124. https://doi.org/10.1093/gerona/glu193
Copeland JL, Ashe MC, Biddle SJ et al (2017) Sedentary time in older adults: a critical review of measurement, associations with health, and interventions. Br J Sports Med 51:1539. https://doi.org/10.1136/bjsports-2016-097210
Troiano RP, Berrigan D, Dodd KW et al (2008) Physical activity in the united states measured by accelerometer. Med Sci Sports Exerc 40:181. https://doi.org/10.1249/mss.0b013e31815a51b3
Department of health, physical activity, health improvement and protection (2011) Start active, stay active: a report on physical activity from the four home countries’Chief Medical Officers. Crown, London
Chastin SFM, Buck C, Freiberger E et al (2015) Systematic literature review of determinants of sedentary behaviour in older adults: a DEDIPAC study. Int J Behav Nutr Phys Act 12:127. https://doi.org/10.1186/s12966-015-0292-3
Crombie IK, Irvine L, Williams B et al (2004) Why older people do not participate in leisure time physical activity: a survey of activity levels, beliefs and deterrents. Age Ageing 33:287–292. https://doi.org/10.1093/ageing/afh089
Mathews AE, Laditka SB, Laditka JN et al (2010) Older adults’ perceived physical activity enablers and barriers: a multicultural perspective. J Aging Phys Act 18:119–140. https://doi.org/10.1123/japa.18.2.119
Loprinzi PD, Cardinal BJ (2013) Association between biologic outcomes and objectively measured physical activity accumulated in ≥ 10-minute bouts and < 10-minute bouts. Am J Health Promot 27:143–151. https://doi.org/10.4278/ajhp.110916-QUAN-348
Glazer NL, Lyass A, Esliger DW et al (2013) Sustained and shorter bouts of physical activity are related to cardiovascular health. Med Sci Sports Exerc 45:109–115. https://doi.org/10.1249/MSS.0b013e31826beae5
Burton LC, Shapiro S, German PS (1999) Determinants of physical activity initiation and maintenance among community-dwelling older persons. Prev Med 29:422–430. https://doi.org/10.1006/pmed.1999.0561
Kosteli M-C, Williams SE, Cumming J (2016) Investigating the psychosocial determinants of physical activity in older adults: a qualitative approach. Psychol Health 31:730–749. https://doi.org/10.1080/08870446.2016.1143943
Michael YL, Perdue LA, Orwoll ES et al (2010) Physical activity resources and changes in walking in a cohort of older men. Am J Public Health 100:654–660. https://doi.org/10.2105/AJPH.2009.172031
Li F, Fisher J, Brownson RC (2005) A multilevel analysis of change in neighborhood walking activity in older adults. J Aging Phys Act 13:145–159
Gennuso KP, Thraen-Borowski KM, Gangnon RE et al (2016) Patterns of sedentary behavior and physical function in older adults. Aging Clin Exp Res 28:943–950. https://doi.org/10.1007/s40520-015-0386-4
Cooper AJM, Simmons RK, Kuh D et al (2015) Physical activity, sedentary time and physical capability in early old age: British birth cohort study. PLoS One. https://doi.org/10.1371/journal.pone.0126465
Ortlieb S, Dias A, Gorzelniak L et al (2014) Exploring patterns of accelerometry-assessed physical activity in elderly people. Int J Behav Nutr Phys Act 11:28. https://doi.org/10.1186/1479-5868-11-28
Shrestha N, Grgic J, Wiesner G et al (2018) Effectiveness of interventions for reducing non-occupational sedentary behaviour in adults and older adults: a systematic review and meta-analysis. Br J Sports Med. https://doi.org/10.1136/bjsports-2017-098270
Funding
The authors have no funding to report.
Author information
Authors and Affiliations
Contributions
Hrubeniuk T.J.: statistical analysis and interpretation of data, study concept, wrote manuscript. Sénéchal M.: analysis and interpretation of data, preparation of manuscript. Mayo A.: statistical analysis and interpretation of data, review of manuscript. Bouchard D.R.: study concept and design, analysis and interpretation of data, preparation of manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval and compliance
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. The NHANES data collection was ethically approved by the Institutional Review Board of the Centers for Disease Control and Prevention.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hrubeniuk, T.J., Sénéchal, M., Mayo, A. et al. Association between physical function and various patterns of physical activity in older adults: a cross-sectional analysis. Aging Clin Exp Res 32, 1017–1024 (2020). https://doi.org/10.1007/s40520-019-01288-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40520-019-01288-2