Abstract
Background
We conducted a retrospective cohort study to evaluate and compare the longitudinal effect of monotherapy with L-, L/T-, L/N-, and L/N/T-type calcium channel blockers (CCBs) on estimated glomerular filtration rate (eGFR), and to investigate the association of treatment duration with eGFR in diabetic patients with hypertension.
Methods
Using a clinical database, we identified new users of five CCBs, i.e. amlodipine (L-type, n = 693), nifedipine (L-type, n = 189), azelnidipine (L/T-type, n = 91), benidipine (L/N/T-type, n = 183), and cilnidipine (L/N-type, n = 61). We used a multivariable regression model to evaluate and compare the effects of these drugs on eGFR and serum creatinine, up to 12 months after initiation of study drug administration.
Results
There was no significant association between treatment duration and both eGFR and serum creatinine level with all CCB types. In addition, there was no significant difference in mean change in eGFR among the five CCBs, with any treatment duration.
Conclusions
Our findings suggest that monotherapy with an L-, L/T-, L/N/T-, or L/N-type CCB may have little influence on renal function parameters and may be safely used in hypertensive patients with diabetes.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
We compared the long-term effects on estimated glomerular filtration rate (eGFR) among five calcium channel blockers (CCBs), i.e. amlodipine, nifedipine, azelnidipine, benidipine, and cilnidipine, and investigated the association of treatment duration with eGFR and serum creatinine level in diabetic patients with hypertension. |
We found no significant association between treatment duration and both eGFR and serum creatinine level, and no significant difference in the change in eGFR and serum creatinine level, among the five CCBs. |
These five CCBs might be safely used in diabetic patients with hypertension. |
1 Introduction
Hypertension and diabetes mellitus (DM) are common diseases that are associated with progression of chronic kidney disease (CKD). Several CKD guidelines strongly recommend the control of blood pressure in patients with DM [1,2,3]; therefore, it is important to examine the longitudinal effect of antihypertensive drugs on renal parameters in patients with DM.
Calcium channel blockers (CCBs), which block voltage-dependent calcium channels (classified into L, N, T, P/Q, and R subtypes), are widely used as first-line antihypertensive drugs in Japan [3]. In the kidney, L-type calcium channels are expressed in afferent arterioles, but not in efferent arterioles. Therefore, L-type CCBs that target L-type calcium channels increase intraglomerular pressure by dilating afferent arterioles predominantly, and potentially subsequently reduce renal function and cause kidney damage, such as a decrease of glomerular filtration rate (GFR) and increase of urinary protein. In contrast, T-type calcium channels are prevalent in both the afferent and efferent arterioles, and N-type calcium channels are present at sympathetic nerve terminals distributed along afferent and efferent arterioles [4]. Therefore, L/T-type, L/N-type, and L/N/T-type CCBs, which target T- and/or N-type calcium channels, decrease intraglomerular pressure by dilating both afferent and efferent arterioles, and potentially result in renal protection, such as maintenance of GFR and decrease of urinary protein [5]. Several clinical studies have shown a reduction in albuminuria in hypertensive patients with CKD who are treated with L/T-, L/N-, or L/N/T-type CCBs [6,7,8,9]; however, it is unclear whether these CCBs affect renal function, e.g. maintain or reduce GFR.
Although some studies have reported the effect of L/T-, L/N-, or L/N/T-type CCBs on estimated GFR (eGFR), their results vary according to concomitant drugs, treatment duration, and medical history of the patients [6, 7, 10]. In addition, some CCBs are known to cause an increase in GFR, hyperfiltration, and edema in the acute phase of initiation of treatment in patients with CKD [11,12,13]. Agodoa et al. reported that eGFR increased during the first 3 months of treatment with amlodipine, an L-type CCB, but decreased after 36 months in patients without proteinuria [14]. Therefore, whether the effects of these CCBs on renal function are influenced by duration of treatment is especially of clinical interest.
In this study, we evaluated and compared the longitudinal effects of monotherapy with L-, L/T-, L/N-, and L/N/T-type CCBs on eGFR and serum creatinine level, and investigated the association between treatment duration and both eGFR and serum creatinine level in diabetic patients with hypertension.
2 Methods
2.1 Data Source
This was a retrospective cohort study using data from the Nihon University School of Medicine (NUSM) Clinical Data Warehouse (CDW), which includes an order entry database and a laboratory results database from the hospital information systems at three hospitals affiliated with the NUSM—Nihon University Itabashi Hospital, Nerima Hikarigaoka Hospital, and Nihon University Hospital. The prescribing data of over 0.7 million patients are linked longitudinally to detailed clinical information, such as patient demographics, diagnosis, and laboratory data. To protect patient privacy, patient identifiers are replaced with anonymous identifiers in all databases of the CDW. Several epidemiological studies examining the effects of drugs on laboratory parameters using the NUSM CDW have been published [15,16,17].
2.2 Study Population
We examined Japanese diabetic patients with mild to moderate hypertension aged over 20 years who had been newly treated with an L-type CCB (amlodipine or nifedipine), L/T-type CCB (azelnidipine), L/N/T-type CCB (benidipine), or L/N-type CCB (cilnidipine) for at least 3 months between 1 December 2004 and 31 May 2012. We identified 19,268 diabetic hypertensive patients treated with amlodipine, 11,134 treated with nifedipine, 3580 treated with azelnidipine, 5173 treated with benidipine, and 2816 treated with cilnidipine. Patients with severe renal failure (eGFR <30), patients who were pregnant, and patients who had been treated with other antihypertensive agents during the study period were excluded. The study population consisted of 693 patients in the amlodipine group, 189 in the nifedipine group, 91 in the azelnidipine group, 183 in the benidipine group, and 61 in the cilnidipine group. The mean dosage was 4.3, 25.3, 12.7, 4.8 and 8.9 mg/day for amlodipine, nifedipine, azelnidipine, benidipine, and cilnidipine, respectively. The experimental protocol was approved by the Ethics Committee of the NUSM, and the study was conducted in compliance with the Ethical Guidelines for Medical and Health Research Involving Human Subjects of the Ministry of Education, Culture, Sports, Science and Technology, and the Ministry of Health, Labour and Welfare, Japan [18].
2.3 Exposure and Measurements
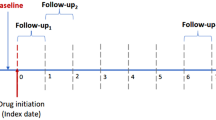
The baseline measurement period (non-exposure period) was defined as within 3 months before the start of treatment with each CCB, while the exposure period (treatment duration) was defined as the number of days since the start of treatment, as follows: 0–3 months (>0 to ≤3 months), 3–6 months (>3 to ≤6 months), 6–9 months (>6 to ≤9 months), and 9–12 months (>9 to ≤12 months). Laboratory data for serum creatinine level for each subject were collected at the date nearest to the start of study drug administration in the baseline period, and at dates within 0–3, 3–6, 6–9, and 9–12 months after the start of treatment in the exposure period. Serum creatinine was determined by the enzymatic method used for routine laboratory testing at the NUSM hospital, and was assayed at a central laboratory (Central Laboratory, SRL Co., Tokyo, Japan) with an enzymatic creatinine assay method using a Japanese electron creatinine auto-analyzer (JCA-BM8060; JEOL Ltd, Tokyo, Japan) and enzyme solution (Preauto-S CRE-L; Sekisui Medical Co., Ltd, Tokyo, Japan). eGFR was calculated according to the Japanese formula specified by the Japanese Society of Nephrology (JSN): eGFR (JSN equation for Japan) (mL/min/1.73 m2) = 194*SCr−1.094*Age−0.287 (*0.739 if female) (this formula is modified) [19]. The percentage change in eGFR was calculated as (eGFR in exposure period − eGFR in baseline period)/(eGFR in baseline period)*100 [20, 21].
2.4 Data Elements
For each patient, we collected information on patient demographics (age and sex), medical history, and use of medications that are clinically important or have the possibility of affecting the outcome as baseline covariates for adjustment. Medical history included urinary protein, cerebrovascular disease (International Classification of Diseases, Tenth Revision [ICD-10] code I60–69), ischemic heart disease (I20–I25), other heart disease (I30–I52), rheumatoid arthritis (M05–M06), liver disease (K70–K77), kidney disease (N00–N19), and hyperlipidemia (E78.0–E78.5) during the 365 days preceding the first date of administration of each CCB. Drugs used during the 90 days before the start of treatment with each CCB included oral hypoglycemics, antithrombotics, corticosteroids, non-steroidal anti-inflammatory drugs (NSAIDs), and statins.
2.5 Statistical Analysis
We used a general linear model for continuous variables and the Chi squared test for categorical data to compare differences in baseline characteristics among the five CCB groups. This study was a retrospective observational study with repeated measures data, and, as the non-randomized subjects had inherent issues of selection bias and confounding factors, we used an unadjusted and a covariate-adjusted linear mixed model with a compound symmetry covariance structure (MIXED procedure in SAS software) to assess the relationship between treatment duration and laboratory parameters, including eGFR and serum creatinine level in each CCB group. The model was adjusted for age, sex, and duration of DM. In addition, we used an unadjusted and covariate-adjusted linear mixed model (covariance structure: Compound Symmetry) to compare the mean change of eGFR and serum creatinine level during the exposure period from baseline among the CCB groups. The model in this analysis was adjusted for age, sex, duration of DM, medical history (including urinary protein, cerebrovascular disease, other heart disease, liver disease, kidney disease, and hyperlipidemia), and medications (including antithrombotic drugs, liver disease therapeutics, corticosteroids, NSAIDs, and statins, which showed a significant difference in baseline parameters among the five CCB groups (Table 1). A multiple comparison test (Turkey’s post hoc analysis) was used to analyze the difference in least square means among the five CCB groups. All reported p values <0.05 were considered to indicate statistical significance. All statistical analyses were performed using SAS software, version 9.3 (SAS Institute Inc., Cary, NC, USA).
3 Results
Table 1 shows the baseline characteristics of patients who had been treated with each CCB. The mean age of amlodipine, nifedipine, azelnidipine, benidipine, and cilnidipine users was 66.3, 66.4, 63.8, 64.7, and 62.5 years, respectively; the female percentage was 46.3, 39.1, 44.0, 37.2, and 31.2%, respectively; and the duration of DM was 2.2, 1.9, 3.2, 2.5, and 2.7 years, respectively. Statistically significant differences were observed in the following baseline characteristics among the five CCBs: mean age, percentage of women, medical history (including urinary protein, cerebrovascular disease, ischemic heart disease, other heart disease, kidney disease, and hyperlipidemia), and medication (including the use of antithrombotic drugs, liver disease therapeutics, corticosteroids, NSAIDs, and statins).
Table 2 shows the relationship between treatment duration and laboratory parameters, including eGFR and serum creatinine level, in the groups receiving the five CCBs. No significant association was observed between treatment duration and both eGFR and serum creatinine level in the five CCB groups before and after adjustment.
Table 3 shows the unadjusted and adjusted mean change in eGFR and serum creatinine level in the five CCB groups during each exposure period. There was no significant difference in the change of eGFR and serum creatinine level among the five CCB groups, with any treatment duration.
Figure 1 shows the adjusted mean percentage change of eGFR in each of the five CCB groups, suggesting that the shape of the curve may depend on the type (L-type, L/T-type, L/N/T-type, and L/N-type) of calcium channel; however, no significant difference was seen among treatment durations in the five CCB groups (data not shown).
Adjusted mean percentage change of eGFR (error bar indicates standard error) during each exposure period for five calcium channel blockers (L-type: amlodipine and nifedipine, L/T-type: azelnidipine, L/N/T-type: benidipine, L/N-type: cilnidipine). Data were adjusted for covariates of age, sex, and duration of diabetes mellitus. eGFR estimated glomerular filtration rate
4 Discussion
In this study, we evaluated and compared the longitudinal effect of monotherapy among five CCBs, i.e. amlodipine (L-type), nifedipine (L-type), azelnidipine (L/T-type), benidipine (L/N/T-type), and cilnidipine (L/N-type), on eGFR and serum creatinine level in hypertensive patients with DM, up to 12 months of treatment. Our study showed no significant association between treatment duration and both mean eGFR and serum creatinine level in the five CCB groups. In addition, the difference in the change of eGFR and serum creatinine level was not significant among the five CCB groups, with any treatment duration.
L/N-, L/T-, and L/N/T-type CCBs are well known to improve proteinuria in patients with CKD through dilation of the efferent renal arteriole and protection of the glomerulus from hyperfiltration injury; however, it is unclear whether these CCBs affect renal function and/or maintain GFR. In patients with hypertensive CKD treated with the maximum dose of angiotensin II receptor blockers, 6 months of additional treatment with benidipine did not significantly change eGFR [6]. Supporting these previous reports, our study showed that eGFR and serum creatinine level in benidipine users were not significantly associated with treatment duration. The percentage change of eGFR in benidipine users was also unchanged during the exposure period. Some studies have shown that treatment with azelnidipine (L/T-type CCB) decreases GFR in patients with type 2 diabetes or CKD. In hypertensive patients with type 2 diabetes, eGFR was significantly decreased after 24 and 48 weeks of treatment with azelnidipine, compared with baseline [22], and in patients with type 2 diabetes treated with an ARB, 32 weeks of additional treatment with azelnidipine decreased eGFR [8]. Uchida et al. reported that eGFR was significantly decreased after 3 months of treatment with cilnidipine, after switching from amlodipine treatment, in hypertensive patients with CKD [10]. Abe et al. reported there was no significant difference in serum creatinine level, which predicts the decline of eGFR, between 16 weeks of treatment with azelnidipine and cilnidipine in hypertensive patients with type 2 diabetes [23]. Supporting these previous reports, our study showed no significant difference in mean changes of eGFR and serum creatinine level between azelnidipine and cilnidipine users, and the treatment duration in azelnidipine and cilnidipine users was not significantly associated with both eGFR and serum creatinine level. These findings support the experience in clinical practice that regular checks of eGFR should be performed prior to and at least up to 12 months after L/T-, L/N- and L/N/T-type CCB initiation.
L-type CCBs such as amlodipine and nifedipine are known to dilate the afferent renal arteriole predominantly, thereby inducing glomerular hyperfiltration and having no renoprotective effect. Some studies have reported that L-type CCBs increase GFR in the acute phase of treatment. In patients with mild to moderate hypertension, 8 weeks of treatment with amlodipine significantly increased GFR [24], and in renal transplant patients, 6 weeks of treatment with amlodipine also significantly increased GFR [25]. These increases in eGFR a few months after initiation of L-type CCBs, observed in both this study and previous studies, may be mediated, in part, by hyperfiltration caused by renal hemodynamic change, such as afferent arteriolar vasodilation. In addition, Agodoa et al. reported that GFR was increased at 3 months after initiation of amlodipine treatment in patients with hypertension, and stated that this instability of GFR may be caused by afferent arteriolar vasodilation and loss of renal autoregulation [14]. Furthermore, Agodoa et al. reported that GFR changed to a decline at 36 months after initiation of amlodipine treatment in patients without proteinuria [14]. In our study, there was no significant association of treatment duration with both mean eGFR and serum creatinine level in amlodipine users and nifedipine users; however, the percentage change of eGFR in amlodipine and nifedipine users showed the similar shape of the curve during the exposure period in our study. These findings suggest the possibility that some mechanism, including the antihypertensive action leading to a decrease in intraglomerular pressure, may exist to compensate an increase in GFR several months after initiation of L-type CCB treatment. Further studies are needed to elucidate the mechanism maintaining GFR in patients with L-type CCB treatment as this study could not address this issue. However, there was no significant difference in mean change in eGFR among the five CCB groups with any treatment duration. Monotherapy with an L-, L/T-, L/N/T-, or L/N-type CCB may have little influence on glomerular function and may be safely used in hypertensive patients with diabetes, at least up to 12 months.
Our study has several limitations. First, this was a retrospective, non-randomized study with potential for selection bias and confounding factors. We used rigorous statistical methods to control for potential confounding variables among the five CCB groups, including a multivariable regression model; however, their ability to control for differences was limited to variables that were available or measurable. Second, we did not fix the daily dose of the five CCBs because achievement of the blood pressure goal requires various doses of an agent across different individuals, or even in the same individual, in clinical practice. This study was not designed to assess the effects of each CCB at each dose because it is difficult to determine whether or not pharmacodynamics are dose-dependent in clinical settings. Third, we could not analyze micro- and macroalbuminuria because many data were missing. When sufficient data including albuminuria are accumulated, further studies will be needed to determine the detailed effect of the five CCBs on renal function. Fourth, CCBs are frequently used with other antihypertensive agents, including angiotensin II receptor blockers, angiotensin-converting enzyme inhibitors, and antihypertensive diuretics. In this study, we focused on patients with diabetes who had been treated with CCB monotherapy. Consequently, many patients were excluded from the study population, according to the exclusion and inclusion criteria. This study may have systematically excluded patients with uncontrolled hypertension despite the use of CCB monotherapy, potentially limiting the ability to generalize the findings. In this study, there was no significant difference in mean changes of renal parameters among the five CCBs. One reason for this might be reduction of the statistical power by the decrease in sample size. It would be of interest to examine and compare the effects of combination therapy and monotherapy with CCBs on renal function because information obtained in clinical settings may be more informative for clinicians. We will evaluate this theme in our next study when our database is large enough to carry out appropriate analysis. However, the findings of our comparative effectiveness study, using a sophisticated statistical method in a real-world setting, are reliable and relevant to clinical practice.
5 Conclusion
Our study showed no significant change in mean eGFR between baseline and any exposure period in each of the five CCB groups. Furthermore, there was no significant difference in mean change in eGFR and serum creatinine level between the five CCB groups with any treatment duration. These findings support the clinical evidence that monotherapy with an L-, L/T-, L/N/T-, or L/N-type CCB may have little influence on renal function and may be safely used in hypertensive patients with diabetes, at least up to 12 months.
References
Kidney Disease Outcomes Quality Initiative (K, DOQI). K/DOQI clinical practice guidelines on hypertension and antihypertensive agents in chronic kidney disease. Am J Kidney Dis. 2004;43(5 Suppl 1):S1–290.
Kidney Disease: Improving Global Outcomes (KDIGO) Management of Blood Pressure Work Group. KDIGO clinical practice guideline for the management of blood pressure in chronic kidney disease. Kidney Int. 2012;2(5):337–414.
Shimamoto K, Ando K, Fujita T, Hasebe N, Higaki J, Horiuchi M, et al. The Japanese Society of Hypertension Guidelines for the Management of Hypertension (JSH2014). Hypertens Res. 2014;37(4):253–390.
Hayashi K, Wakino S, Sugano N, Ozawa Y, Homma K, Saruta T. Ca2+ channel subtypes and pharmacology in the kidney. Circ Res. 2007;100(3):342–53.
Hayashi K, Homma K, Wakino S, Tokuyama H, Sugano N, Saruta T, et al. T-type Ca channel blockade as a determinant of kidney protection. Keio J Med. 2010;59(3):84–95.
Abe M, Okada K, Suzuki H, Yoshida Y, Soma M. T/L-type calcium channel blocker reduces the composite ranking of relative risk according to new KDIGO guidelines in patients with chronic kidney disease. BMC Nephrol. 2013;14:135.
Abe M, Okada K, Maruyama N, Matsumoto S, Maruyama T, Fujita T, et al. Benidipine reduces albuminuria and plasma aldosterone in mild-to-moderate stage chronic kidney disease with albuminuria. Hypertens Res. 2011;34:268–73.
Tawaramoto K, Kaneto H, Hashiramoto M, Kawasaki F, Tatsumi F, Shimoda M, et al. Azelnidipine, but not amlodipine, reduces urinary albumin excretion and carotid atherosclerosis in subjects with type 2 diabetes: blood pressure control with olmesartan and azelnidipine in type 2 diabetes (BOAT2 study). Diabetol Metab Syndr. 2015;7:80.
Takenaka T, Seto T, Okayama M, Kojima E, Nodaira Y, Sueyoshi K, et al. Long-term effects of calcium antagonists on augmentation index in hypertensive patients with chronic kidney disease: a randomized controlled study. Am J Nephrol. 2012;35(5):416–23.
Uchida S, Takahashi M, Sugawara M, Saito T, Nakai K, Fujita M, et al. Effects of the N/L-type calcium channel blocker cilnidipine on nephropathy and uric acid metabolism in hypertensive patients with chronic kidney disease (J-CIRCLE study). J Clin Hypertens (Greenwich). 2014;16(10):746–53.
Morrone LF, Ramunni A, Fassianos E, Saracino A, Coratelli P, Passavanti G. Nitrendipine and amlodipine mimic the acute effects of enalapril on renal haemodynamics and reduce glomerular hyperfiltration in patients with chronic kidney disease. J Hum Hypertens. 2003;17(7):487–93.
Volpe M, Tocci G. Rationale for triple fixed-dose combination therapy with an angiotensin II receptor blocker, a calcium channel blocker, and a thiazide diuretic. Vasc Health Risk Manag. 2012;8:371–80.
Rubio-Guerra AF, Castro-Serna D, Barrera CI, Ramos-Brizuela LM. Current concepts in combination therapy for the treatment of hypertension: combined calcium channel blockers and RAAS inhibitors. Integr Blood Press Control. 2009;2:55–62.
Agodoa LY, Appel L, Bakris GL, Beck G, Bourgoignie J, Briggs JP, et al.; African American Study of Kidney Disease and Hypertension (AASK) Study Group. Effect of ramipril vs amlodipine on renal outcomes in hypertensive nephrosclerosis: a randomized controlled trial. JAMA. 2001; 285(21):2719–28.
Susa N, Nishida Y, Yada Y, Nakayama T, Asai S, Takahashi Y. Comparative effect of fixed-dose combination tablets of candesartan cilexetil/amlodipine versus olmesartan medoxomil/azelnidipine on laboratory parameters in patients with hypertension: a retrospective cohort study. Clin Exp Hypertens. 2016;38(2):173–9.
Takahashi Y, Nishida Y, Nakayama T, Asai S. Adverse effect profile of trichlormethiazide: a retrospective observational study. Cardiovasc Diabetol. 2011;10:45.
Nishida Y, Takahashi Y, Susa N, Kanou N, Nakayama T, Asai S. Comparative effect of angiotensin II type I receptor blockers on serum uric acid in hypertensive patients with type 2 diabetes mellitus: a retrospective observational study. Cardiovasc Diabetol. 2013;12:159.
Ministry of Education, Culture, Sports, Science and Technology and Ministry of Health, Labour and Welfare. Ethical guidelines for medical and health research involving human subjects. http://www.mhlw.go.jp/file/06-Seisakujouhou-10600000-Daijinkanboukouseikagakuka/0000080278.pdf. Accessed 12 Aug 2016.
Matsuo S, Imai E, Horio M, Yasuda Y, Tomita K, Nitta K, et al. Revised equations for estimated GFR from serum creatinine in Japan. Am J Kidney Dis. 2009;53:982–92.
Coresh J, Turin TC, Matsushita K, Sang Y, Ballew SH, Appel LJ, et al.; CKD Prognosis Consortium. Decline in estimated glomerular filtration rate and subsequent risk of end-stage renal disease and mortality. JAMA. 2014;311(24):2518–31.
Wright JT Jr, Bakris G, Greene T, Agodoa LY, Appel LJ, Charleston J, et al.; African American Study of Kidney Disease and Hypertension Study Group. Effect of blood pressure lowering and antihypertensive drug class on progression of hypertensive kidney disease: results from the AASK trial. JAMA. 2002;288(19):2421–31.
Takihata M, Nakamura A, Kondo Y, Kawasaki S, Kimura M, Terauchi Y. Comparison of azelnidipine and trichlormethiazide in Japanese type 2 diabetic patients with hypertension: the COAT randomized controlled trial. PLoS One. 2015;10(5):e0125519.
Abe H, Mita T, Yamamoto R, Komiya K, Kawaguchi M, Sakurai Y, et al. Comparison of effects of cilnidipine and azelnidipine on blood pressure, heart rate and albuminuria in type 2 diabetics with hypertension: a pilot study. J Diabetes Investig. 2013;4(2):202–5.
Delles C, Klingbeil AU, Schneider MP, Handrock R, Weidinger G, Schmieder RE. Direct comparison of the effects of valsartan and amlodipine on renal hemodynamics in human essential hypertension. Am J Hypertens. 2003;16(12):1030–5.
Inigo P, Campistol JM, Lario S, Piera C, Campos B, Bescós M, et al. Effects of losartan and amlodipine on intrarenal hemodynamics and TGF-beta(1) plasma levels in a crossover trial in renal transplant recipients. J Am Soc Nephrol. 2001;12(4):822–7.
Acknowledgements
This work was supported by the Health Sciences Research Institute, Inc., Yokohama, Japan, and Convergence CT Japan K.K., Tokyo, Japan.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
Yayoi Nishida, Yasuo Takahashi, Kotoe Tezuka, Satoshi Takeuchi, Tomohiro Nakayama, and Satoshi Asai have no conflicts of interest to declare.
Ethical approval
Statement of Human Rights For this type of study, formal consent is not required.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Nishida, Y., Takahashi, Y., Tezuka, K. et al. Comparative Effect of Calcium Channel Blockers on Glomerular Function in Hypertensive Patients with Diabetes Mellitus. Drugs R D 17, 403–412 (2017). https://doi.org/10.1007/s40268-017-0191-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40268-017-0191-y