Abstract
Background
Intravenous administration of vascular endothelial growth factor (VEGF)-inhibiting drugs is associated with adverse gastrointestinal (GI) events. Clinical trials of VEGF inhibitors used for the treatment of retinal diseases have suggested higher risks of adverse GI events among patients treated with bevacizumab. However, population-based studies have been lacking.
Objective
Our objective was to assess risks for GI adverse events associated with intravitreal injections of VEGF-inhibiting drugs.
Methods
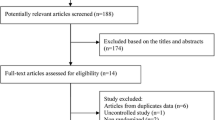
We conducted a population-based, nested case–control study of 114,427 older adults in Ontario, Canada, with retinal disease identified between 1 November 2005 and 30 April 2011. Of these, 3,582 cases were admitted to hospital or assessed in an emergency department for GI adverse events. Controls were matched to cases on the basis of age, sex, and outcome history.
Results
Patients experiencing adverse events were equally as likely as matched controls to have been exposed to bevacizumab or ranibizumab. Adjusted odds ratios for bevacizumab were 1.05 (95 % confidence interval [CI] 0.69–1.61) for upper GI ulceration, 1.29 (95 % CI 0.86–1.96) for diverticular disease, 1.49 (95 % CI 0.84–2.63) for pancreatitis, 0.82 (95 % CI 0.53–1.29) for cholelithiasis, and 1.45 (95 % CI 0.67–3.12) for cholecystitis. For ranibizumab they were 1.25 (95 % CI 0.88–1.77) for upper GI ulceration, 1.12 (95 % CI 0.83–1.52) for diverticular disease, 0.85 (95 % CI 0.51–1.40) for pancreatitis, 0.77 (95 % CI 0.53–1.11) for cholelithiasis, and 0.83 (95 % CI 0.44–1.56) for cholecystitis. Results were similar when the analysis was restricted to patients only exposed to a single type of VEGF inhibitor.
Conclusions
In this population-based study, intravitreal injections of bevacizumab and ranibizumab were not associated with increased risks of adverse GI events.


Similar content being viewed by others
References
Ip MS, Scott IU, Brown GC, Brown MM, Ho AC, Huang SS, et al. Anti-vascular endothelial growth factor pharmacotherapy for age-related macular degeneration—a report by the American Academy of Ophthalmology. Ophthalmology. 2008;115:1837–46.
Brown DM, Kaiser PK, Michels M, Soubrane G, Heier JS, Kim RY, et al. Ranibizumab versus verteporfin for neovascular age-related macular degeneration. N Engl J Med. 2006;355:1432–44.
Rosenfeld PJ, Brown DM, Heier JS, Boyer DS, Kaiser PK, Chung CY, et al. Ranibizumab for neovascular age-related macular degeneration. N Engl J Med. 2006;355:1419–31.
CATT Research Group, Martin D, Maguire M, Ying G, Grunwald J, Fine S, et al. Ranibizumab and bevacizumab for neovascular age-related macular degeneration. N Engl J Med. 2011;364:1897–908.
Campochiaro PA, Heier JS, Feiner L, Gray S, Saroj N, Rundle AC, et al. Ranibizumab for macular edema following branch retinal vein occlusion: six-month primary end point results of a phase III study. Ophthalmology. 2010;117:1102.e1–1112.e1.
Elman MJ, Bressler NM, Qin H, Beck RW, 3rd Ferris FL, Friedman SM, et al. Expanded 2-year follow-up of ranibizumab plus prompt or deferred laser or triamcinolone plus prompt laser for diabetic macular edema. Ophthalmology. 2011;118:609–14.
Kamba T, McDonald D. Mechanisms of adverse effects of anti-VEGF therapy for cancer. Br J Cancer. 2007;96:1788.
Tuñón J, Ruiz-Moreno JM, Martín-Ventura JL, Blanco-Colio LM, Lorenzo O, Egido J. Cardiovascular risk and antiangiogenic therapy for age-related macular degeneration. Surv Ophthalmol. 2009;54:339–48.
Snider KL, Maitland ML. Cardiovascular toxicities: clues to optimal administration of vascular endothelial growth factor signaling pathway inhibitors. Targeted Oncol. 2009;4:67–76.
Csaky K, Do DV. Safety implications of vascular endothelial growth factor blockade for subjects receiving intravitreal anti-vascular endothelial growth factor therapies. Am J Ophthalmol. 2009;148:647–56.
Scappaticci FA, Skillings JR, Holden SN, Gerber HP, Miller K, Kabbinavar F, et al. Arterial thromboembolic events in patients with metastatic carcinoma treated with chemotherapy and bevacizumab. J Natl Cancer Inst. 2007;99:1232–9.
Choueiri TK, Mayer EL, Je Y, Rosenberg JE, Nguyen PL, Azzi GR, et al. Congestive heart failure risk in patients with breast cancer treated with bevacizumab. J Clin Oncol. 2011;29:632–8.
Nalluri SR, Chu D, Keresztes R, Zhu X, Wu S. Risk of venous thromboembolism with the angiogenesis inhibitor bevacizumab in cancer patients: a meta-analysis. JAMA. 2008;300:2277.
Hapani S, Sher A, Chu D, Wu S. Increased risk of serious hemorrhage with bevacizumab in cancer patients: a meta-analysis. Oncology. 2010;79:27–38.
Taugourdeau-Raymond S, Rouby F, Default A, Jean-Pastor MJ, French Network of Pharmacovigilance C. Bevacizumab-induced serious side-effects: a review of the french pharmacovigilance database. Eur J Clin Pharmacol. 2012;68:1103–7.
Fuloria J. Safety profiles of current antiangiogenic therapies for metastatic colorectal cancer. Onco Targets Ther. 2012;5:133–42.
Hurwitz H, Fehrenbacher L, Novotny W, Cartwright T, Hainsworth J, Heim W, et al. Bevacizumab plus irinotecan, fluorouracil, and leucovorin for metastatic colorectal cancer. N Engl J Med. 2004;350:2335–42.
CATT Research Group, Martin DF, Maguire MG, Fine SL, Ying G, Jaffe GJ, et al. Ranibizumab and bevacizumab for treatment of neovascular age-related macular degeneration: two-year results. Ophthalmology. 2012;119:1388–98.
IVAN Study Investigators, Chakravarthy U, Harding SP, Rogers CA, Downes SM, Lotery AJ, et al. Ranibizumab versus bevacizumab to treat neovascular age-related macular degeneration: one-year findings from the IVAN randomized trial. Ophthalmology. 2012;119:1399–411.
Cohen D. Roche and Novartis colluded over wet AMD drugs, says Italian regulator. BMJ. 2014;348:g2006.
Liew G, Mitchell P. Ranibizumab for neovascular age-related macular degeneration. N Engl J Med. 2007;356:747–8.
Vandenbroucke JP, Psaty BM. Benefits and risks of drug treatments. JAMA. 2008;300:2417–9.
Curtis LH, Hammill BG, Schulman KA, Cousins SW. Risks of mortality, myocardial infarction, bleeding, and stroke associated with therapies for age-related macular degeneration. Arch Ophthalmol. 2010;128:1273–9.
Campbell RJ, Bell CM, Paterson JM, Bronskill SE, Moineddin R, Whitehead M, et al. Stroke rates after introduction of vascular endothelial growth factor inhibitors for macular degeneration: a time series analysis. Ophthalmology. 2012;119:1604–8.
Campbell RJ, Gill SS, Bronskill SE, Paterson JM, Whitehead M, Bell CM. Adverse events with intravitreal injection of vascular endothelial growth factor inhibitors: nested case-control study. BMJ. 2012;345:e4203.
French DD, Margo CE. Age-related macular degeneration, anti-vascular endothelial growth factor agents, and short-term mortality: a postmarketing medication safety and surveillance study. Retina. 2011;31:1036–42.
Campbell RJ, Bell CM, Campbell Ed, Gill SS. Systemic effects of intravitreal vascular endothelial growth factor inhibitors. Curr Opin Ophthalmol. 2013;24:197–204.
von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP, et al. Strengthening the reporting of observational studies in epidemiology (STROBE) statement: guidelines for reporting observational studies. BMJ. 2007;335:806–8.
Williams JI, Young W. A summary of studies on the quality of health care administration databases in Canada. In: Goel V, Williams JI, Anderson GM, Blackstien-Hirsch P, Fooks C, Naylor CD, eds. Patterns of Health Care in Ontario. The ICES Practice Atlas. 2nd ed. Ottawa: Canadian Medical Association; 1996. pp. 339–345. http://www.ices.on.ca/~/media/Files/Atlases-Reports/1996/Patterns-of-health-care-in-Ontario-2nd-edition/Full%20report.ashx. Accessed 8 May 2014.
Juurlink DN, Preyra C, Croxford R, Chong A, Austin P, Tu J, et al. Canadian Institute for Health Information Discharge Abstract Database: a validation study. ICES Investigative Report. Toronto: Institute for Clinical Evaluative Sciences; 2006. http://www.ices.on.ca/~/media/Files/Atlases-Reports/2006/CIHI-DAD-a-validation-study/Full%20report.ashx. Accessed 8 May 2014.
Gruneir A, Bell CM, Bronskill SE, Schull M, Anderson GM, Rochon PA. Frequency and pattern of emergency department visits by long-term care residents—a population-based study. J Am Geriatr Soc. 2010;58:510–7.
Gill SS, Anderson GM, Fischer HD, Bell CM, Li P, Normand SLT, et al. Syncope and its consequences in patients with dementia receiving cholinesterase inhibitors: a population-based cohort study. Arch Intern Med. 2009;169:867.
Hux JE, Ivis F, Flintoft V, Bica A. Diabetes in Ontario: determination of prevalence and incidence using a validated administrative data algorithm. Diabetes Care. 2002;25:512–6.
Cattaruzzi C, Troncon MG, Agostinis L, Garcia Rodriguez LA. Positive predictive value of ICD-9th codes for upper gastrointestinal bleeding and perforation in the Sistema Informativo Sanitario Regionale Database. J Clin Epidemiol. 1999;52:499–502.
Raiford DS, Perez Gutthann S, Garcia Rodriguez LA. Positive predictive value of ICD-9 codes in the identification of cases of complicated peptic ulcer disease in the Saskatchewan Hospital Automated Database. Epidemiology. 1996;7:101–4.
Moores K, Gilchrist B, Carnahan R, Abrams T. A systematic review of validated methods for identifying pancreatitis using administrative data. Pharmacoepidemiol Drug Saf. 2012;21:194–202.
Urbach DR, Stukel TA. Rate of elective cholecystectomy and the incidence of severe gallstone disease. CMAJ. 2005;172:1015–9.
Schneeweiss S, Seeger JD, Maclure M, Wang PS, Avorn J, Glynn RJ. Performance of comorbidity scores to control for confounding in epidemiologic studies using claims data. Am J Epidemiol. 2001;154:854–64.
Bell CM, Hatch WV, Fischer HD, Cernat G, Paterson JM, Gruneir A, et al. Association between tamsulosin and serious ophthalmic adverse events in older men following cataract surgery. JAMA. 2009;301:1991.
Breslow N, Day N. Fitting models to continuous data. 82nd ed. France: IARC Scientific Publications; 1987. p. 178–229.
Suissa S. Novel approaches to pharmacoepidemiology study design and statistical analysis. England: Wiley; 2005. p. 811–29.
Breslow N, Lubin J, Marek P, Langholz B. Multiplicative models and cohort analysis. J Am Stat Assoc. 1983;78:1–12.
Essebag V, Platt RW, Abrahamowicz M, Pilote L. Comparison of nested case-control and survival analysis methodologies for analysis of time-dependent exposure. BMC Med Res Methodol. 2005;5:5.
Liddell F, McDonald J, Thomas D. Methods of cohort analysis: appraisal by application to asbestos mining. J R Stat Soc Ser A. 1977;140:469–91.
Austin PC. Balance diagnostics for comparing the distribution of baseline covariates between treatment groups in propensity-score matched samples. Stat Med. 2009;28:3083–107.
Drazen JM, Curfman GD, Baden LR, Morrissey S. Compounding errors. N Engl J Med. 2012;367:2436–7.
Contributors
All authors were involved in the design and conduct of the study; collection, management, analysis, and interpretation of the data; and preparation, review, or approval of the manuscript. RJC drafted the manuscript and approved the final version to be published. SSG, SEB, JMP, MW, EdeLPC, and CMB critically revised the manuscript for important intellectual content. RJC, MW, SEB, SSG, and CMB conducted the statistical analysis. RJC and SSG obtained funding. RJC supervised the study and is the guarantor.
Funding
This study was funded by the Canadian Institutes of Health Research (CIHR) and the Ontario Ministry of Health and Long-Term Care (MOHLTC). The work was also supported by the Institute for Clinical Evaluative Sciences (ICES), a non-profit research institute funded by the Ontario MOHLTC. RJC is supported by a Clinician Scientist Award from the Southeastern Ontario Academic Medical Organization, which receives funding from the MOHLTC, and holds research grants from the CIHR and the MOHLTC for related work. SSG and SEB are supported by CIHR New Investigator Awards from the Institute of Aging. CMB is supported by a CIHR and Canadian Patient Safety Institute chair in Patient Safety and Continuity of Care.
Data Access and Responsibility
Dr. RJ Campbell had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis.
Conflicts of Interest
RJ Campbell, CM Bell, SE Bronskill, JM Paterson, M Whitehead, EdeL Campbell, and SS Gill have no conflicts of interest.
Role of the Sponsors
The sponsors of this study had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; or the decision to submit for publication. The opinions, results, and conclusions reported in this paper are those of the authors and are independent from the funding sources. No endorsement by ICES or the Ontario MOHLTC is intended or should be inferred.
Ethical Approval
The study protocol was approved by the Research Ethics Board at Queen’s University, Kingston, Ontario, Canada (file No. 6004374).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Campbell, R.J., Bell, C.M., Bronskill, S.E. et al. Adverse Gastrointestinal Events with Intravitreal Injection of Vascular Endothelial Growth Factor Inhibitors: Nested Case–Control Study. Drug Saf 37, 723–733 (2014). https://doi.org/10.1007/s40264-014-0211-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40264-014-0211-6