Abstract
Background
Physicians frequently rely on the systemic inflammatory response syndrome (SIRS) criteria to detect bloodstream infections (BSIs). We evaluated the diagnostic performance of procalcitonin (PCT) in detecting BSI in patients with and without SIRS.
Methods
We tested the association between BSI, serum PCT levels, contemporaneous SIRS scores and serum lactate using logistic regression in a dataset of 4279 patients. The diagnostic performance of these variables was assessed.
Results
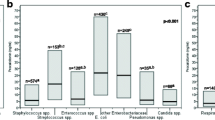
In multivariate regression analysis, only log(PCT) was independently associated with BSI (p < 0.05). The mean area under the curve (AUC) of PCT in detecting BSI (0.683; 95% CI 0.65–0.71) was significantly higher than serum lactate (0.615; 95% CI 0.58–0.64) and the SIRS score (0.562; 95% CI 0.53–0.58). The AUC of PCT did not differ significantly by SIRS status. PCT of less than 0.1 ng/mL had a negative predictive value (NPV) of 97.4 and NPV of 96.2% for BSI in the SIRS-negative and SIRS-positive patients, respectively. A PCT of greater than 10 ng/mL had a LR of 6.22 for BSI in SIRS-negative patients. The probability of BSI increased exponentially with rising PCT levels regardless of SIRS status.
Conclusion
The performance of PCT for the diagnosis of BSI was not affected by SIRS status. Only PCT was independently associated with BSI, while the SIRS criterion and serum lactate were not. A low PCT value may be used to identify patients at a low risk for having BSI in both settings. An elevated PCT value even in a SIRS negative patient should prompt a careful search for BSI.


Similar content being viewed by others
Abbreviations
- PCT:
-
Serum procalcitonin
- SIRS:
-
Systemic inflammatory response syndrome
- BSI:
-
Bloodstream infection
- SD:
-
Standard deviation
- OR:
-
Odds ratio
- CI:
-
Confidence interval
- NPV:
-
Negative predictive value
- EMR:
-
Electronic medical record
- HR:
-
Heart rate
- RR:
-
Respiratory rate
- WBC:
-
White blood cells
- ROC:
-
Receiver operating characteristic
- AUC:
-
Area under the curve
- ICU:
-
Intensive care unit
- LR:
-
Likelihood ratio
- qSOFA:
-
Quick Sequential Organ Failure Assessment
References
Leibovici L, Greenshtain S, Cohen O, Mor F, Wysenbeek AJ. Bacteremia in febrile patients. A clinical model for diagnosis. Arch Intern Med. 1991;151:1801–6. doi:10.1001/archinte.1991.00400090089016.
Goto M, Al-Hasan MN. Overall burden of bloodstream infection and nosocomial bloodstream infection in North America and Europe. Clin Microbiol Infect. 2013;19:501–9.
Weinstein MP, Towns ML, Quartey SM, Mirrett S, Reimer LG, Parmigiani G, et al. The clinical significance of positive blood cultures in the 1990s: a prospective comprehensive evaluation of the microbiology, epidemiology, and outcome of bacteremia and fungemia in adults. Clin Infect Dis. 1997;24:584–602.
American College of Chest Physicians/Society of Critical Care Medicine Consensus Conference. Definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. Crit Care Med. 1992;20:864–74.
Jaimes F, Garces J, Cuervo J, Ramirez F, Ramirez J, Vargas A, et al. The systemic inflammatory response syndrome (SIRS) to identify infected patients in the emergency room. Intensive Care Med. 2003;29:1368–71. doi:10.1007/s00134-003-1874-0.
Lai NA, Kruger P. The predictive ability of a weighted systemic inflammatory response syndrome score for microbiologically confirmed infection in hospitalised patients with suspected sepsis. Crit Care Resusc. 2012;14:146–50.
Bossink AWJ, Groeneveld ABJ, Hack CE, Thijs LG. The clinical host response to microbial infection in medical patients with fever. Chest. 1999;116:380–90. doi:10.1378/chest.116.2.380.
Liaudat S, Dayer E, Praz G, Bille J, Troillet N. Usefulness of procalcitonin serum level for the diagnosis of bacteremia. Eur J Clin Microbiol Infect Dis. 2001;20:524–7. doi:10.1007/s100960100548.
Kaukonen K-M, Bailey M, Pilcher D, Cooper DJ, Bellomo R. Systemic inflammatory response syndrome criteria in defining severe sepsis. N Engl J Med. 2015;372:1629–38. doi:10.1056/NEJMoa1415236.
Shankar-Hari M, Phillips GS, Levy ML, Seymour CW, Liu VX, Deutschman CS, et al. Developing a new definition and assessing new clinical criteria for septic shock: for the third international consensus definitions for sepsis and septic shock (Sepsis-3). JAMA. 2016;315:775–87. doi:10.1001/jama.2016.0289.
Levy MM, Fink MP, Marshall JC, Abraham E, Angus D, Cook D, et al. 2001 SCCM/ESICM/ACCP/ATS/SIS international sepsis definitions conference. Crit Care Med. 2003;31:1250–6.
Simpson SQ. New sepsis criteria: a change we should not make. Chest. 2016;149:1117–8. doi:10.1016/j.chest.2016.02.653.
Vincent J-L, Martin GS, Levy MM, Singer M, Deutschman C, Seymour C, et al. qSOFA does not replace SIRS in the definition of sepsis. Crit Care. 2016;20:210. doi:10.1186/s13054-016-1389-z.
Wacker C, Prkno A, Brunkhorst FM, Schlattmann P. Procalcitonin as a diagnostic marker for sepsis: a systematic review and meta-analysis. Lancet Infect Dis. 2013;13:426–35. doi:10.1016/S1473-3099(12)70323-7.
Riedel S, Carroll KC. Laboratory detection of sepsis: biomarkers and molecular approaches. Clin Lab Med. 2013;33:413–37.
Müller F, Christ-Crain M, Bregenzer T, Krause M, Zimmerli W, Mueller B, et al. Procalcitonin levels predict bacteremia in patients with community-acquired pneumonia: a prospective cohort trial. Chest. 2010;138:121–9. doi:10.1378/chest.09-2920.
van Nieuwkoop C, Bonten TN, van’t Wout JW, Kuijper EJ, Groeneveld GH, Becker MJ, et al. Procalcitonin reflects bacteremia and bacterial load in urosepsis syndrome: a prospective observational study. Crit Care. 2010;14:R206. doi:10.1186/cc9328.
Ratzinger F, Schuardt M, Eichbichler K, Tsirkinidou I, Bauer M, Haslacher H, et al. Utility of sepsis biomarkers and the infection probability score to discriminate sepsis and systemic inflammatory response syndrome in standard care patients. PLoS One. 2013;8:e82946. doi:10.1371/journal.pone.0082946.
Chirouze C, Schuhmacher H, Rabaud C, Gil H, Khayat N, Estavoyer J-M, et al. Low serum procalcitonin level accurately predicts the absence of bacteremia in adult patients with acute fever. Clin Infect Dis. 2002;35:156–61. doi:10.1086/341023.
Schuetz P, Chiappa V, Briel M, Greenwald JL. Procalcitonin algorithms for antibiotic therapy decisions: a systematic review of randomized controlled trials and recommendations for clinical algorithms. Arch Intern Med. 2011;171:1322–31. doi:10.1001/archinternmed.2011.318.
Hall KK, Lyman JA. Updated review of blood culture contamination. Clin Microbiol Rev. 2006;19:788–802. doi:10.1128/CMR.00062-05.
Harbarth S, Holeckova K, Froidevaux C, Pittet D, Ricou B, Grau GE, et al. Predictive value of procalcitonin and interleukin 6 in critically ill patients with suspected sepsis. Am J Respir Crit Care Med. 2002;164:396–402.
Brunkhorst FM, Wegscheider K, Forycki ZF, Brunkhorst R. Procalcitonin for early diagnosis and differentiation of SIRS, sepsis, severe sepsis, and septic shock. Intensive Care Med. 2000;26:S148–52. doi:10.1186/cc469.
Kim MH, Lim G, Kang SY, Lee WI, Suh JT, Lee HJ. Utility of procalcitonin as an early diagnostic marker of bacteremia in patients with acute fever. Yonsei Med J. 2011;52:276–81. doi:10.3349/ymj.2011.52.2.276.
Sprung CL, Sakr Y, Vincent J-L, Le Gall J-R, Reinhart K, Ranieri VM, et al. An evaluation of systemic inflammatory response syndrome signs in the sepsis occurrence in acutely ill patients (SOAP) study. Intensive Care Med. 2006;32:421–7.
Klein Klouwenberg PMC, Ong DSY, Bonten MJM, Cremer OL. Classification of sepsis, severe sepsis and septic shock: the impact of minor variations in data capture and definition of SIRS criteria. Intensive Care Med. 2012;38:811–9.
Cortegiani A, Russotto V, Montalto F, Foresta G, Accurso G, Palmeri C, et al. Procalcitonin as a marker of Candida species detection by blood culture and polymerase chain reaction in septic patients. BMC Anesthesiol. 2014;14:9. doi:10.1186/1471-2253-14-9.
Acknowledgements
We would like to thank Dr. John Song, Dr. Anne-Marie Weber, Dr. Jonathon Kirsch and Dr. Robert Foley for critically reviewing the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Arora, R., Campbell, J.P., Simon, G. et al. Does serum procalcitonin aid in the diagnosis of bloodstream infection regardless of whether patients exhibit the systemic inflammatory response syndrome?. Infection 45, 291–298 (2017). https://doi.org/10.1007/s15010-016-0965-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s15010-016-0965-0