Abstract
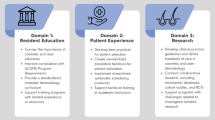
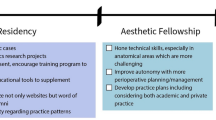
Dermatologic surgery is a major component of dermatology practice in the USA. The skill set required to perform surgical procedures is developed during the residency period and augmented through surgery-specific fellowships. In recent years, the breadth and scope of surgical procedures provided by dermatologists has increased exponentially. A commensurate expansion in the training requirements of residents and fellows has occurred to meet these demands. Concurrently, evaluation systems to assess competency have been broadened to ensure adequate training and safe delivery of care. However, the provision of surgical training to residents and fellows continues to be met with a number of challenges which are discussed herein.
Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Roenigk RK. Dermatologists perform more skin surgery than any other specialist: implications for health care policy, graduate and continuing medical education. Dermatol Surg. 2008;34(3):293–300.
Ahn CS, Davis S a, Dabade TS, Williford PM, Feldman SR. Noncosmetic skin-related procedures performed in the United States: an analysis of national ambulatory medical care survey data from 1995 to 2010. Dermatol Surg. 2013;39(12):1912–21.
Kimball AB, Resneck JS. The US dermatology workforce: a specialty remains in shortage. J Am Acad Dermatol. 2008;59(5):741–5.
Review Committee for Dermatology: ACGME., ACGME program requirements for graduate medical education in dermatology. [Online]. Available: https://www.acgme.org/acgmeweb/Portals/0/PFAssets/ProgramRequirements/080_dermatology_07012014_u06152014.pdf. [Accessed: 20-Mar-2015].
Lee EH, Nehal KS, Dusza SW, Hale EK, Levine VJ. Procedural dermatology training during dermatology residency: a survey of third-year dermatology residents. J Am Acad Dermatol. 2011;64(3):475–83. A survey study of the expectations and experience of graduating dermatology residents in the areas of surgical and cosmetic procedures.
S. M. R. and F. M. Services, Statistics—micrographic surgery & dermatologic oncology fellowship match. [Online]. Available: https://www.sfmatch.org/SpecialtyInsideAll.aspx?id=10&typ=1&name=Micrographic Surgery and Dermatologic Oncology#.
Hanke CW, Moy RL, Roenigk RK, Roenigk HH, Spencer JM, Tierney EP, et al. Current status of surgery in dermatology. J Am Acad Dermatol. 2013;69(6):972–1001.
The Accreditation Council for Graduate Medical Education, ACGME program requirements for graduate medical education in micrographic surgery and dermatologic oncology. [Online]. Available: https://www.acgme.org/acgmeweb/Portals/0/PFAssets/ProgramRequirements/081_MSDO_07012015_1-YR.pdf. [Accessed: 20-Mar-2015].
Nicholas L, Toren K, Bingham J, Marquart J. Simulation in dermatologic surgery: a new paradigm in training. Dermatol Surg. 2013;39(1 Pt 1):76–81. A survey of dermatology residents and surgical instructors opinions after hands-on surgery training with synthetic skin bust model simulator. Nearly all participants felt that simulators should be incorporated into dermatologic surgery training.
Adams CC, Marquart JD, Nicholas LL, Sperling LC, Meyerle JH. Survey of medical student preference for simulation models for basic dermatologic surgery skills: simulation platforms in medical education. Dermatol Surg. 2014;40(4):427–35.
Våpenstad C, Buzink SN. Procedural virtual reality simulation in minimally invasive surgery. Surg Endosc. 2013;27(2):364–77.
Bauer B, Williams E, Stratman EJ. Cosmetic dermatologic surgical training in US dermatology residency programs: identifying and overcoming barriers. JAMA Dermatol. 2014;150(2):125–9. A survey of cosmetic procedure training provided and program director attitudes toward cosmetic dermatology training during residency. Nearly all dermatology residents in the US receive cosmetic training while nearly one-third of PDs do not feel that cosmetic procedures should be taught during residency.
J. L. Reichel, R. P. Peirson, and D. Berg, Teaching and evaluation of surgical skills in dermatology: results of a survey. Arch. Dermatol., 2004.
T. A. C. for G. M. E. and T. A. B. of Dermatology, The Dermatology Milestone Project, 2014. [Online]. Available: http://acgme.org/acgmeweb/Portals/0/PDFs/Milestones/DermatologyMilestones.pdf.
The Accreditation Council for Graduate Medical Education and The American Board of Dermatology, The Procedural Dermatology Milestone Project, 2014. [Online]. Available: https://www.acgme.org/acgmeweb/Portals/0/PDFs/Milestones/ProceduralDermatologyMilestones.pdf.
Coleman WP, Hanke CW, Orentreich N, Kurtin SB, Brody H, Bennett R. A history of dermatologic surgery in the United States. Dermatol Surg. 2000;26(1):5–11.
Ibrahimi OA, Bangash H, Green L, Alam M, Armstrong AW, Eisen DB. Perceptions of expertise in cutaneous surgery and cosmetic procedures: what primary care physicians think. Dermatol Surg. 2012;38(10):1645–51.
Suneja T, Smith ED, Chen GJ, Zipperstein KJ, Fleischer AB, Feldman SR. Waiting times to see a dermatologist are perceived as too long by dermatologists: implications for the dermatology workforce. Arch Dermatol. 2001;137(10):1303–7.
Compliance with Ethics Guidelines
Conflict of Interest
Mark E. Burnett and Erica H. Lee declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is part of the Topical Collection on Medical Surgery
Rights and permissions
About this article
Cite this article
Burnett, M.E., Lee, E.H. Key Issues in Surgical Training of Residents and Fellows. Curr Derm Rep 4, 134–139 (2015). https://doi.org/10.1007/s13671-015-0109-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13671-015-0109-2