Abstract
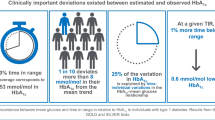
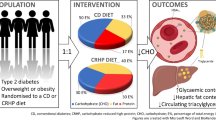
Hormonal change in carbohydrate metabolism through the circadian rhythm is well known. An impaired nocturnal insulin secretion and lower level melatonin coexist in diabetics at the end of the night period. Administration of melatonin may improve impaired insulin secretion and control hyperglycemia. In a randomized, double-blind study, 64 type 2 tics were treated for 12 weeks (period 1) with placebo, and then for another 12 weeks (period 2) with 6 mg of melatonin. Fasting blood glucose (FBG), total triglyceride (TG), total cholesterol (CHOL), high-density (HDL), and low-density lipoprotein (LDL) cholesterol and glycosylated hemoglobin levels (HbA1c) were measured at baseline, 12 and 24 weeks. Following 3 months of melatonin treatment, mean HbA1c (±standard error) was significantly lower than at baseline (7.65 % ± 0.086 % versus 7.1 % ± 0.111 %, respectively, P = 0.0001). The mean FBG level was significantly decreased at the end of the study (164 ± 5.4 versus 157 ± 5.5, respectively, P < 0.001). The HDL cholesterol level increased at the end of the study (42 ± 1.3 versus 45 ± 1.39, respectively, P < 0.05) but no significant changes in TG, CHOL, and LDL were observed. Results showed that bed time melatonin administration in patients with type 2 diabetes, improved control of diabetes. Trial registration: IRCT2012062610115N1, http://en.search.irct.ir/search?query=melatonin+and+rezvanfar

Similar content being viewed by others
References
Cajochen C, Krauchi K, Wirz-Justice A. Role of melatonin in the regulation of human circadian rhythms and sleep. J Neuroendocrinol. 2003;15(4):432–7.
Mulder H, Nagorny CL, Lyssenko V, et al. Melatonin receptors in pancreatic islets: good morning to a novel type 2 diabetes gene. Diabetologia. 2009;52:1240–9.
Radziuk J, Pye S. Diurnal rhythm in endogenous glucose production is a major contributor to fasting hyperglycaemia in type 2 diabetes. Suprachiasmatic deficit or limit cycle behaviour? Diabetologia. 2006;49:1619–28.
Lima FB, Machado UF, Bartol I, et al. Pinealectomy causes lucose intolerance and decreases adipose cell responsiveness to insulin in rats. Am J Phys. 1998;275:934–41.
Rasmussen DD, Boldt BM, Wilkinson CW, et al. Daily melatonin administration at middle age suppresses male rat visceral fat, plasma leptin, and plasma insulin to youthful levels. Endocrinology. 1999;140:1009–12.
Sartori C, Dessen P, Mathieu C, et al. Melatonin improves glucose homeostasis and endothelial vascular function in high-fat diet-fed insulin resistant mice. Endocrinology. 2009;150(12):5311–7.
Cagnacci A, Arangino S, Renzi A, et al. Influence of melatonin administration on glucose tolerance and insulin sensitivity of post-menopausal women. Clin Endocrinol. 2001;54(3):339–46.
Javier E, José A, Pariente A, et al. Role of melatonin on diabetes-related metabolic disorders. World J Diabetes. 2011;2(6):82–91.
Peschke E. Melatonin, endocrine pancreas and diabetes. J Pineal Res. 2008;44(1):26–40.
Robeva R, Kirilov G, Tomova A, et al. Melatonin-insulin interactions in patients with metabolic syndrome. J Pineal Res. 2008;44(1):52–6.
Agil A, Rosado I, Ruiz R, et al. Melatonin improves glucose homeostasis in young Zucker diabetic fatty rats. J Pineal Res. 2012;52(2):203–10.
American Diabetes Association. Diagnosis and classification of diabetes mellitus. Diabetes Care. 2014;37(Suppl. 1):S81–90.
Hussain SA, Khadim HM, Khalaf BH, et al. Effects of melatonin and zinc on glycemic control in type 2 diabetic patients poorly controlled with metformin. Saudi Med J. 2006;27(10):1483–8.
Nishida S, Segawa T, Murai I, et al. Long-term melatonin administration reduces hyperinsulinemia and improves the altered fatty-acid compositions in type 2 diabetic rats via the restoration of delta-5 desaturase activity. J Pineal Res. 2002;32(1):26–33.
Wolden-Hanson T, Mitton DR, McCants RL, et al. Daily melatonin administration to middle-aged male rats suppresses body weight, Intraabdominal adiposity, and plasma leptin and insulin independent of food intake and Total body Fat1. Endocrinology. 2000;141(2):487–97.
Nogueira TC, Lellis-Santos C, Jesus DS, et al. Absence of melatonin induces night-time hepatic insulin resistance and increased gluconeogenesis due to stimulation of nocturnal unfolded protein response. Endocrinology. 2011;152(4):1253–63.
Bazwinsky-Wutschke I, Bieseke L, et al. Influence of melatonin receptor signalling on parameters involved in blood glucose regulation. J Pineal Res. 2014;56(1):82–96.
Sinha N, Mishra T, Singh T, et al. Effect of iron deficiency anemia on hemoglobin A1c level. Ann Lab Med 2012; 32: 17–22. [PMC free article]
Tamura H, Nakamura Y, Narimatsu A, et al. Melatonin treatment in peri- and postmenopausal women elevates serum high-density lipoprotein cholesterol levels without influencing total cholesterol levels. J Pineal Res. 2008;45(1):101–5.
Wade AG, Ford I, Crawford G, et al. Nightly treatment of primary insomnia with prolonged release melatonin for 6 months: a randomized placebo controlled trial on age and endogenous melatonin as predictors of efficacy and safety. BMC Med. 2010;8:51.
Tang Y, Meng L, Li D, et al. Interaction of sleep quality and sleep duration on glycemic control in patients with type 2 diabetes mellitus. Chin Med J. 2014;127(20):3543–7.
Tsai YW, Kann NH, Tung TH, et al. Impact of subjective sleep quality on glycemic control in type 2 diabetes mellitus. Fam Pract. 2012;29(1):30–5. doi:10.1093/fampra/cmr041.
Yoda K, Inaba M, Hamamoto K, et al. Association between poor glycemic control, impaired sleep quality, and increased arterial thickening in type 2 diabetic patients. PLoS ONE. 2015;10(4):e0122521. doi:10.1371/journal.pone.0122521.
Wade AG, Crawford G, Ford I, et al. Prolonged release melatonin in the treatment of primary insomnia: evaluation of the age cut-off for short- and long-term response. Curr Med Res Opin. 2011;27(1):87–98.
Zisapel N. Sleep and sleep disturbances: biological basis and clinical implications. Cell Mol Life Sci. 2007;64(10):1174–86.
Peschke E, Bähr I, Mühlbauer E. Experimental and clinical aspects of melatonin and clock genes in diabetes. J Pineal Res. 2015;59(1):1–23. doi:10.1111/jpi.12240.
Shweta Sharma, Hemant Sing, Nabeel Ahmad, et al. The role of melatonin in diabetes: therapeutic implications. Arch. Endocrinol. Metab. 59(5):391–9, 2015
Lenters-Westra E, Slingerland RJ. Hemoglobin A1c point-of-care assays; a new world with a lot of consequences! J Diabetes Sci Technol. 2009;3(3):418–23.
Stratton IM, Adler AI, Neil HA, et al. Association of glycaemia with macrovascular and microvascular complications of type 2 diabetes (UKPDS 35): prospective observational study. BMJ. 2000;321(7258):405–12.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Rezvanfar, M.R., Heshmati, G., Chehrei, A. et al. Effect of bedtime melatonin consumption on diabetes control and lipid profile. Int J Diabetes Dev Ctries 37, 74–77 (2017). https://doi.org/10.1007/s13410-016-0497-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13410-016-0497-2