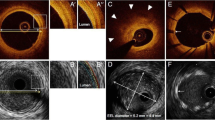
Abstract
The most common cause of acute coronary syndrome (ACS) is vulnerable plaque rupture. Other less common causes are attenuated plaques, erosions, and calcific nodules. We review the current intracoronary imaging techniques—grayscale intravascular ultrasound (IVUS), virtual histology (VH)-IVUS, optical coherence tomography (OCT), and near-infrared spectroscopy (NIRS)—and their ability to identify the causes of ACS and, potentially, improve the outcomes in ACS patients. Grayscale IVUS gives information about vessel and lesion morphology, but it is limited in terms of plaque composition and near-field resolution. VH-IVUS improves on the ability of grayscale IVUS to assess plaque composition, but it does not improve on resolution. OCT provides structural details with high resolution and can assess plaque composition, but is limited by a low penetration into tissue and the interference of light by blood. NIRS detects lipid core plaques, but does not give structural information. Each of these techniques offers important, but incomplete information when used individually. There are early, but real attempts to combine these technologies in a single catheter and system.

Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Fujii K, Kobayashi Y, Mintz GS, et al. Intravascular ultrasound assessment of ulcerated ruptured plaques: a comparison of culprit and nonculprit lesions of patients with acute coronary syndromes and lesions in patients without acute coronary syndromes. Circulation. 2003;108:2473–8.
Hirayama A, Ueda Y, Kodama K. Acute coronary syndrome diagnosed by the intravascular imaging. Nippon Rinsho. 2006;64:686–90.
• Lee SY, Mintz GS, Kim SY, et al. Attenuated plaque detected by intravascular ultrasound: clinical, angiographic, and morphologic features and post-percutaneous coronary intervention complications in patients with acute coronary syndromes. JACC Cardiovasc Interv 2009;2:65–72. Although uncommon, attenuated plaques in ACS are more associated with STEMI, higher C-reactive protein level, complex lesion, and low to no reflow before and after PCI.
• Maehara A, Mintz GS, Weissman NJ. Advances in intravascular imaging. Circ Cardiovasc Interv. 2009;2:482-90. Summarizes most of the coronary imaging techniques with their advantages and drawbacks.
Schaar JA, Mastik F, Regar E, et al. Current diagnostic modalities for vulnerable plaque detection. Curr Pharm Des. 2007;13:995–1001.
Tahara S, Bezerra HG, Sirbu V, et al. Angiographic, IVUS and OCT evaluation of the long-term impact of coronary disease severity at the site of overlapping drug-eluting and bare metal stents: a substudy of the ODESSA trial. Heart. 2010;96:1574–8.
Garcia-Garcia HM, Costa MA, Serruys PW. Imaging of coronary atherosclerosis: intravascular ultrasound. Eur Heart J. 2010;31:2456–69.
• Kawasaki M, Hattori A, Ishihara Y, et al. Tissue Characterization of Coronary Plaques and Assessment of Thickness of Fibrous Cap Using Integrated Backscatter Intravascular Ultrasound. Circ J. 2010. The thickness of the fibrous cap measured with a new IB-IVUS with high resolution correlates with OCT measurements.
Ko YG, Son JW, Park SM, et al. Effect of vessel size on lipid content of coronary plaques assessed by integrated backscatter intravascular ultrasound. Circ J. 2010;74:754–9.
• Coletta J, Suzuki N, Nascimento BR, et al. Use of optical coherence tomography for accurate characterization of atherosclerosis. Arq Bras Cardiol. 2010;94:250–4, 68–72, 4–9. The major of OCT in daily interventional practice because of its high resolution. The correlation of OCT with histology in the measurement of fibrous cap thickness.
Cilingiroglu M, Ozer K. Optical coherence tomography and its use in detection of vulnerable plaque. Curr Atheroscler Rep. 2006;8:140–3.
Mintz GS. Remodeling and restenosis: observations from serial intravascular ultrasound studies. Curr Interv Cardiol Rep. 2000;2:316–25.
Waxman S. Near-infrared spectroscopy for plaque characterization. J Interv Cardiol. 2008;21:452–8.
Caplan JD, Waxman S, Nesto RW, Muller JE. Near-infrared spectroscopy for the detection of vulnerable coronary artery plaques. J Am Coll Cardiol. 2006;47:C92–6.
Komatsu S, Hirayama A, Ueda Y, Kodama K. Evaluation of atherosclerosis of coronary artery by intravascular ultrasound and coronary angioscopy. Nippon Rinsho. 2006;64 Suppl 9:526–9.
Mintz G. Intracoronary Ultrasound. 2005:75–114.
• Kashiwagi M, Tanaka A, Kitabata H, et al. Relationship between coronary arterial remodeling, fibrous cap thickness and high-sensitivity C-reactive protein levels in patients with acute coronary syndrome. Circ J. 2009;73:1291–5. This article highlights the close association between positive remodeling, fibrous cap thickness, high-sensitivity C-reactive protein, and ACS. The detection of these parameters helps in identifying vulnerable plaques.
Hong YJ, Jeong MH, Choi YH, et al. Positive remodeling is associated with more plaque vulnerability and higher frequency of plaque prolapse accompanied with post-procedural cardiac enzyme elevation compared with intermediate/negative remodeling in patients with acute myocardial infarction. J Cardiol. 2009;53:278–87.
von Birgelen C, Klinkhart W, Mintz GS, et al. Size of emptied plaque cavity following spontaneous rupture is related to coronary dimensions, not to the degree of lumen narrowing. A study with intravascular ultrasound in vivo. Heart. 2000;84:483–8.
Hong MK, Mintz GS, Lee CW, et al. Plaque ruptures in stable angina pectoris compared with acute coronary syndrome. Int J Cardiol. 2007;114:78–82.
Naghavi M, Libby P, Falk E, et al. From vulnerable plaque to vulnerable patient: a call for new definitions and risk assessment strategies: Part II. Circulation. 2003;108:1772–8.
Nakamura T, Kubo N, Funayama H, Sugawara Y, Ako J, Momomura S. Plaque characteristics of the coronary segment proximal to the culprit lesion in stable and unstable patients. Clin Cardiol. 2009;32:E9–E12.
• Endo M, Hibi K, Shimizu T, et al. Impact of ultrasound attenuation and plaque rupture as detected by intravascular ultrasound on the incidence of no-reflow phenomenon after percutaneous coronary intervention in ST-segment elevation myocardial infarction. JACC Cardiovasc Interv. 2010;3:540–9. This article discusses the importance to identify ultrasound-attenuated plaque during PCI of STEMI and the consequence of no reflow phenomenon from distal embolism.
Choi SY, Mintz GS. What have we learned about plaque rupture in acute coronary syndromes? Curr Cardiol Rep. 2010;12:338–43.
Virmani R, Burke AP, Farb A, Kolodgie FD. Pathology of the unstable plaque. Prog Cardiovasc Dis. 2002;44:349–56.
Virmani R, Burke AP, Kolodgie FD, Farb A. Vulnerable plaque: the pathology of unstable coronary lesions. J Interv Cardiol. 2002;15:439–46.
Kim SH, Hong MK, Park DW, et al. Impact of plaque characteristics analyzed by intravascular ultrasound on long-term clinical outcomes. Am J Cardiol. 2009;103:1221–6.
• Stone GW, Maehara A, Lansky AJ, PROSPECT Investigators, et al. A prospective natural-history study of coronary atherosclerosis. N Engl J Med. 2011;364:226–35. PROSEPCT. Identification of patients at high risk for cardiac events by combining risk factors such as large plaque burden, small lumen area, and VH-TCFA.
investigators CLDtwCt. What should we do about Lipid Core Plaque? The InfraRedx Lipiscan IVUS and the Canary Trial. Cath Lab Digest 2010;18.
• Kubo T, Maehara A, Mintz GS, et al. The dynamic nature of coronary artery lesion morphology assessed by serial virtual histology intravascular ultrasound tissue characterization. J Am Coll Cardiol. 2010;55:1590–7. A limited number of studies have been performed concerning the natural course of coronary artery lesion. Although limited to 12 months, this study reveals that most VH-TCFA heals after this period, but new ones also develop.
Maehara A, Mintz GS, Bui AB, et al. Morphologic and angiographic features of coronary plaque rupture detected by intravascular ultrasound. J Am Coll Cardiol. 2002;40:904–10.
Burke AP, Kolodgie FD, Farb A, et al. Healed plaque ruptures and sudden coronary death: evidence that subclinical rupture has a role in plaque progression. Circulation. 2001;103:934–40.
Hong MK, Mintz GS, Lee CW, et al. Serial intravascular ultrasound evidence of both plaque stabilization and lesion progression in patients with ruptured coronary plaques: effects of statin therapy on ruptured coronary plaque. Atherosclerosis. 2007;191:107–14.
Rioufol G, Gilard M, Finet G, Ginon I, Boschat J, Andre-Fouet X. Evolution of spontaneous atherosclerotic plaque rupture with medical therapy: long-term follow-up with intravascular ultrasound. Circulation. 2004;110:2875–80.
Hong MK, Mintz GS, Lee CW, et al. Comparison of coronary plaque rupture between stable angina and acute myocardial infarction: a three-vessel intravascular ultrasound study in 235 patients. Circulation. 2004;110:928–33.
Rioufol G, Finet G, Ginon I, et al. Multiple atherosclerotic plaque rupture in acute coronary syndrome: a three-vessel intravascular ultrasound study. Circulation. 2002;106:804–8.
Farb A, Burke AP, Tang AL, et al. Coronary plaque erosion without rupture into a lipid core. A frequent cause of coronary thrombosis in sudden coronary death. Circulation. 1996;93:1354–63.
• Wu X, Maehara A, Mintz GS, et al. Virtual histology intravascular ultrasound analysis of non-culprit attenuated plaques detected by grayscale intravascular ultrasound in patients with acute coronary syndromes. Am J Cardiol. 2010;105:48–53. Attenuated plaques contain a large amount of necrotic core and a high prevalence of VH-TCFA.
van Soest G, Goderie T, Regar E, et al. Atherosclerotic tissue characterization in vivo by optical coherence tomography attenuation imaging. J Biomed Opt. 2010;15:011105.
Jaross W, Neumeister V, Lattke P, Schuh D. Determination of cholesterol in atherosclerotic plaques using near infrared diffuse reflection spectroscopy. Atherosclerosis. 1999;147:327–37.
Tanaka A, Imanishi T, Kitabata H, et al. Lipid-rich plaque and myocardial perfusion after successful stenting in patients with non-ST-segment elevation acute coronary syndrome: an optical coherence tomography study. Eur Heart J. 2009;30:1348–55.
Gardner CM, Tan H, Hull EL, et al. Detection of lipid core coronary plaques in autopsy specimens with a novel catheter-based near-infrared spectroscopy system. JACC Cardiovasc Imaging. 2008;1:638–48.
Disclosure
K. Fall: none; A. Maehara: payment for lecture from Volcano Corporation; G. S. Mintz: consultant to Volcano Corporation, Boston Scientific, and Light Lab.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Fall, K., Maehara, A. & Mintz, G.S. Intravascular Imaging in Patients with Acute Coronary Syndromes and Unstable Coronary Plaques. Curr Cardiovasc Imaging Rep 4, 269–275 (2011). https://doi.org/10.1007/s12410-011-9089-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12410-011-9089-1