Abstract
Endoscopic retrograde cholangiopancreatography (ERCP) in patients with surgically altered anatomy involves challenging procedures for ERCP endoscopists. In these patients, the anatomical structure of the intestine is substantially altered, and an endoscope needs to be inserted into the long afferent limb. Moreover, the papilla is observed in the opposite view from the normal anatomy. Recently, a balloon-assisted enteroscope (BAE) has been developed and made available for use in daily practice. The two types of BAE are single-balloon enteroscope (SBE), which is inserted with one balloon attached to the overtube using a balloon-assisted method, and double-balloon enteroscope (DBE), which is inserted with two balloons, one attached to the overtube and the other attached to the tip of the enteroscope. In addition, short-type DBE (short-DBE) and short-type SBE (short-SBE) with a working length of approximately 150 cm, which could be used with various ERCP accessories, are commercially available or under development. Notably, the success rate of ERCP through coordinated manipulation with a balloon was remarkably improved with the use of BAE, even in patients with surgically altered anatomy. Here, we report the current status and procedures of ERCP in patients with surgically altered anatomy.
Similar content being viewed by others
Introduction
Endoscopic retrograde cholangiopancreatography (ERCP) in patients with surgically altered anatomy involves challenging procedures for ERCP endoscopists. These procedures include identification and access to the afferent limb, reaching the papilla or anastomotic site of the pancreaticobiliary-enteric anastomosis, and cannulation to the bile and pancreatic ducts through the native papilla or anastomotic site without using an elevator function. In particular, an endoscope must be inserted beyond the long afferent limb in patients with Roux-en-Y (R-Y) reconstruction or hepaticojejunostomy. The papilla also appears in reverse of the usual appearance. Moreover, in patients with pancreatic or biliary anastomosis, the anastomotic site occasionally has stenosis due to duct-enteric anastomosis.
In patients with Billroth-II reconstruction, the use of a duodenoscope, an oblique-viewing endoscope, or a forward-viewing endoscope reportedly results in a high success rate of ERCP [1]. However, in patients with R-Y reconstruction, hepaticojejunostomy, or pancreaticoduodenectomy (PD), the target site is difficult to reach, and the outcomes have not been sufficiently satisfactory [2, 3].
Recently, a balloon-assisted enteroscope (BAE) has been developed and made available for use in daily practice [4–9]. With this BAE, the success rate of ERCP through coordinated manipulation with a balloon was remarkably improved even in patients with surgically altered anatomy. However, ERCP using BAE also involves difficult procedures, and some technical aspects must be thoroughly understood to successfully carry out such procedures. Here, we report the current status of and provide technical tips regarding ERCP using BAE performed in patients with surgically altered anatomy.
Anatomy after digestive reconstruction
Before performing ERCP in patients with surgically altered anatomy, it is important to confirm and thoroughly understand the anatomy of such patients, as well as the surgical reconstructions involved.
Billroth-II reconstruction connects the greater curvature of the stomach to the first part of the jejunum in a side-to-side manner. This often follows resection of the lower part of the stomach. When performing ERCP, the endoscope should be inserted into the afferent limb and the scope must be advanced to the papilla (Fig. 1a).
Schema of surgically altered anatomy. a B-II reconstruction. The greater curvature of the stomach connects to the first part of the jejunum in a side-to-side manner. b R-Y reconstruction. End-to-side anastomosis of the jejunum is created. To reach the papilla, this end-to-side anastomosis must be located, and the endoscope should be inserted into the appropriate limb. c Whipple reconstruction. Reconstruction consists of attaching the pancreas to the jejunum and then joining the hepatic duct to the jejunum as the sequence of bile duct, pancreas, and stomach. d Child reconstruction. The sequence is pancreas, bile duct, and stomach
R-Y reconstruction is a surgically created end-to-side anastomosis of the jejunum. Typically, this is between the small bowel and the small bowel that is distal from the cut end. To reach the papilla, this end-to-side anastomosis must be located and the endoscope should be inserted into the appropriate limb (Fig. 1b). R-Y is usually performed to treat bile duct obstruction that may arise due to a common bile duct or hepatic duct tumor, a bile duct injury, or bypass operation for unresectable pancreatic cancer. The anatomy of R-Y hepaticojejunostomy is similar to that of an R -Y gastrectomy. Although the stomach is not resected and still remains intact, endoscope manipulation is occasionally difficult because the scope easily bends in the stomach.
PD is a major surgical operation involving the pancreas, duodenum, and other organs. This operation is mainly performed to treat cancerous tumors on the head of the pancreas, and malignant tumors involving the common bile duct, duodenal papilla, or duodenum near the pancreas. Reconstruction consists of attaching the pancreas to the jejunum (pancreaticojejunostomy) and then joining the hepatic duct to the jejunum (hepaticojejunostomy) to allow digestive juices and bile, respectively, to flow into the gastrointestinal tract, and thereafter attaching the stomach to the jejunum (gastrojejunostomy) to allow food passage. Whipple originally used the sequence bile duct, pancreas, and stomach (Fig. 1c), whereas presently the common reconstruction method involves the sequence of pancreas, bile duct, and stomach, which is known as Child’s operation (Fig. 1d). Basically, the anatomical reconstruction is similar to the Billroth-II reconstruction. However, as the native papilla is resected, we should cannulate through the anastomotic site.
Balloon-assisted enteroscope
For the BAE, the two types of enteroscope used are the single-balloon enteroscope (SBE) and the double-balloon enteroscope (DBE). The SBE is inserted with one balloon attached to the overtube using a balloon-assisted method (Fig. 2a). The DBE is inserted with two balloons, one attached to the overtube and the other attached to the enteroscope tip (Fig. 2b). As conventional enteroscopes have recently been designed to have a working length of approximately 200 cm, various accessories for the ERCP procedure that can be used in combination have become limited. At present, short-type DBE (short-DBE) [10] and short-type SBE (short-SBE) [11] with a working length of approximately 150 cm are commercially available or under development. One possible advantage of a short-type enteroscope is its usefulness because it provides a larger working channel, and it can be used with various accessories. As a long-type enteroscope can deploy only limited devices, interventional procedures become limited because of the long working channel. However, the target site cannot be reached in some cases because of the shorter scope length. Moreover, in some difficult cases, a change from a short-type enteroscope to a long-type enteroscope is required because of the insufficient length of the short-type enteroscope.
Balloon-assisted ERCP procedures
Scope insertion
The scope is inserted using coordinated manipulation with the balloon and overtube. Following the insertion of a BAE into the intestine while forming a loop, the intestine can be fixed with the balloon and shortened or straightened. Furthermore, by simultaneously using an overtube to transmit force to the enteroscope tip, the enteroscope can be inserted into the target site. The use of carbon dioxide was recognized as a technical improvement issue for endoscope insertion. In inserting an enteroscope, one of the most difficult procedures may be identifying the jejunojejunostomy site (Fig. 3) in cases of R-Y anatomy. One of the technical improvements to overcome this difficulty is that a transparent hood should be attached to the enteroscope to locate the jejunojejunostomy site. Moreover, the approximate site should be confirmed under X-ray fluoroscopic guidance while the intestine is dilated with carbon dioxide. After the enteroscope is inserted into the afferent limb, bile juice is usually recognized in many cases. The previously reported indigo carmine dye method [12] is also useful for identifying the appropriate afferent limb. To correctly identify the right limb at the anastomotic site of the intestine, local injection of India ink with an endoscope is helpful. When an enteroscope is inserted beyond the long limb, the intestine needs to be shortened (Fig. 4a, b). However, in some patients who have undergone R-Y hepaticojejunostomy without gastrectomy, it may be difficult to insert an endoscope because no force is transmitted to the endoscope at the bend of the stomach. In fact, manual compression is necessary in such patients.
Cannulation technique
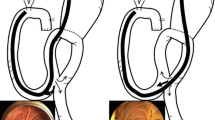
Biliary cannulation through the papilla in cases with surgically altered anatomy is difficult compared to cases with normal anatomy. This is because of the following: (1) the papilla appears in reverse of the usual appearance in normal anatomy, (2) the anastomotic site is occasionally difficult to recognize because of an anastomotic stricture in cases of Whipple resection, and (3) the BAE has no elevator to change the direction of the catheter. Thus, the scope should be manipulated to adjust the direction. Scope position is very important because the direction of the catheter is fixed according to the scope type. The direction of the catheter position in the endoscopic view is 8 O’clock using the SBE (Fig. 5) and 7 O’clock using the DBE. The papilla should be adjusted in these positions according to the scope type. For failed cases of cannulation after conventional methods, using an angle-changeable catheter and performing a precut sphincterotomy are alternative options.
Some problems encountered when cannulating the bile duct and pancreatic duct through the anastomotic site after PD include difficulties in detecting the anastomotic site, cannulation, and intubation of the catheter due to stenosis. A transparent cap placed at the end of the endoscope is useful for searching behind or between the folds [14].
If the anastomotic site could not be identified during the procedure, a rendezvous technique is an option [14–16]. Endoscopic ultrasound-guided puncture of the bile duct and pancreatic duct and subsequent guidewire insertion are effective for carrying out the rendezvous technique (Fig. 6a–c). However, there is no specialized equipment for this procedure. Moreover, this kind of procedure is not yet established, particularly in pancreatic intervention. There are still a number of alternative procedures, and thus, further investigation is needed.
Endoscopic ultrasonography (EUS)-guided rendezvous technique in patients with Whipple resection. a The main pancreatic duct was punctured under EUS-guidance. b The guidewire was advanced to the jejunum through the stenotic anastomotic site. c The endoscope was exchanged for BAE. Endoscopic pancreatic stenting was performed using the rendezvous technique
Procedures for the papilla
After cannulation to the bile duct, some procedures for the papilla are necessary before performing various interventions. Endoscopic sphincterotomy (EST) is the most common and standard procedure for endoscopic transpapillary intervention. In the enteroscope procedures, the reversed view of the papilla can be seen, making sphincterotomy difficult. One of the methods of performing EST is using a needle knife with a biliary stent, in which the roof of the papilla is cut along the plastic stent (Fig. 7). Another technique is balloon dilation. Endoscopic papillary balloon dilation is an effective and simple procedure for the removal of common bile duct stones. Recently, endoscopic large balloon papillary dilation has been shown to be useful for the removal of large bile duct stones. A larger opening of the papilla orifice may allow the retrieval of large stones without performing lithotripsy, and this is effective for a large number of stones. These balloon dilation methods were shown to be effective for ERCP in patients with surgically altered anatomy.
Complications
The most severe complication we observed in enteroscopic ERCP was perforation. Although many of these cases improved with conservative management, some required surgical operation. Five types of perforation may occur during enteroscopic ERCP: (1) digestive tract perforation by the scope tip, (2) digestive tract perforation by the scope body, (3) digestive tract perforation resulting from the very tight tension brought about by scope manipulation, (4) digestive tract perforation near the papilla by device insertion, and (5) bile duct perforation by the balloon dilation procedure. Type (1) perforation could be avoided by careful scope manipulation, but this was difficult to achieve in perforation types (2) and (3). These perforations were observed on X-ray during or after the procedure.
Summary of BAE usage in ERCP for patients with surgically altered anatomy
There are some series already reported about ERCP using BAE. The use of BAE has demonstrated an enteroscopy success rate of 71–97 %, an ERCP success rate of 64.1–98 %, and a complication rate of 1.6–12.9 % [10, 11, 17–21] (Table 1). There are currently no data indicating which type of enteroscope (i.e., SBE or DBE) is superior for scope insertion. A previous multicenter survey report in Japan [13] revealed that the overall success rate of reaching the target site was not significantly different between SBE and DBE. On the other hand, the overall success rate of reaching the target site in patients with R-Y reconstruction was higher for DBE (94.7 %) than for SBE (85.1 %). The present results were obtained from a multicenter, cooperative, but non-randomized retrospective study. Additional studies of SBE and DBE as well as conventional and short-type BAE are highly anticipated.
Conclusion
We have described the current status and procedural techniques of ERCP in patients with surgically altered anatomy using BAE. Although the success rate of ERCP in patients with surgically altered anatomy has been improving, the procedures involved remain challenging. Sustained efforts to develop special devices for balloon-assisted ERCP should be exerted to achieve an easier and safer procedure.
Abbreviations
- ERCP:
-
Endoscopic retrograde cholangiopancreatography
- R-Y:
-
Roux-en-Y reconstruction
- PD:
-
Pancreaticoduodenectomy
- BAE:
-
Balloon-assisted enteroscope
- SBE:
-
Single-balloon enteroscope
- DBE:
-
Double-balloon enteroscope
- EST:
-
Endoscopic sphincterotomy
References
Park CH, Lee WS, Joo YE, et al. Cap-assisted ERCP in patients with a Billroth II gastrectomy. Gastrointest Endosc. 2007;66:612–5.
Elton E, Hanson BL, Qaseem T, et al. Diagnostic and therapeutic ERCP using an enteroscope and pediatric colonoscope in long-limb surgical bypass patients. Gastrointest Endosc. 1998;47:62–7.
Wright BE, Cass OW, Freeman ML. ERCP in patients with long-limb Roux-en-Y gastrojejunostomy and intact papilla. Gastrointest Endosc. 2002;56:225–32.
Dellon ES, Kohn GP, Morgan DR, et al. Endoscopic retrograde cholangiopancreatography with single-balloon enteroscopy is feasible in patients with a prior Roux-en-Y anastomosis. Dig Dis Sci. 2009;54:1798–803.
Emmett DS, Mallat DB. Double-balloon ERCP in patients who have undergone Roux-en-Y surgery: a case series. Gastrointest Endosc. 2007;66:1038–41.
Aabakken L, Bretthauer M, Line PD. Double-balloon enteroscopy for endoscopic retrograde cholangiography in patients with a Roux-en-Y anastomosis. Endoscopy. 2007;39:1068–71.
Maaser C, Lenze F, Bokemeyer M, et al. Double balloon enteroscopy: a useful tool for diagnostic and therapeutic procedures in the pancreaticobiliary system. Am J Gastroenterol. 2008;103:894–900.
Saleem A, Baron TH, Gostout CJ, et al. Endoscopic retrograde cholangiopancreatography using a single-balloon enteroscope in patients with altered Roux-en-Y anatomy. Endoscopy. 2010;42:656–60.
Obana T, Fujita N, Ito K, et al. Therapeutic endoscopic retrograde cholangiography using a single-balloon enteroscope in patients with Roux-en-Y anastomosis. Dig Endosc. 2013;25(6):601–7.
Siddiqui AA, Chaaya A, Shelton C, et al. Utility of the short double-balloon enteroscope to perform pancreaticobiliary interventions in patients with surgically altered anatomy in a US multicenter study. Dig Dis Sci. 2013;58(3):858–64.
Yamauchi H, Kida M, Okuwaki K, et al. Short-type single balloon enteroscope for endoscopic retrograde cholangiopancreatography with altered gastrointestinal anatomy. World J Gastroenterol. 2013;19(11):1728–35.
Yano T, Hatanaka H, Yamamoto H, et al. Intraluminal injection of indigo carmine facilitates identification of the afferent limb during double-balloon ERCP. Endoscopy. 2012;44(Suppl 2):UCTN: E340–1.
Yane K, Katanuma A, Osanai M, et al. Successful removal of a pancreatic duct stone in a patient with Whipple resection, using a short single-balloon enteroscope with a transparent hood. Endoscopy. 2014;46:E86–7.
Kikuyama M, Itoi T, Ota Y, et al. Therapeutic endoscopy for stenotic pancreatodigestive tract anastomosis after pancreatoduodenectomy (with videos). Gastrointest Endosc. 2011;73:376–82.
Mallery S, Matlock J, Freeman ML. EUS-guided rendezvous drainage of obstructed biliary and pancreatic ducts: report of 6 cases. Gastrointest Endosc. 2004;59:100–7.
Kinney TP, Li R, Gupta K, et al. Therapeutic pancreatic endoscopy after Whipple resection requires rendezvous access. Endoscopy. 2009;41:898–901.
Shimatani M, Matsushita M, Takaoka M, et al. Effective “short” double-balloon enteroscope for diagnostic and therapeutic ERCP in patients with altered gastrointestinal anatomy: a large case series. Endoscopy. 2009;41:849–54.
Shah RJ, Smolkin M, Yen R, et al. A multicenter US experience of single-balloon, double-balloon, and rotational overtube-assisted enteroscopy ERCP in patients with surgically altered pancreaticobiliary anatomy (with video). Gastrointest Endosc. 2013;77(4):593–600.
Kawamura T, Mandai K, Uno K et al. Does single-balloon enteroscopy contribute to successful endoscopic retrograde cholangiopancreatography in patients with surgically altered gastrointestinal anatomy? ISRN Gastroenterology 2013; 214958. doi:10.1155/2013/214958.
Katanuma A, Isayama H. Current status of endoscopic retrograde cholangiopancreatography in patients with surgically altered anatomy in Japan: questionnaire survey and important discussion points at Endoscopic Forum Japan 2013. Dig Endosc. 2014;26:S109–15.
Itokawa F, Itoi T, Ishii K, et al. Single- and double-balloon enteroscopy-assisted endoscopic retrograde cholangiopancreatography in patients with Roux-en-Y plus hepaticojejunostomy anastomosis and Whipple resection. Dig Endosc. 2014;26:S136–43.
Acknowledgments
The authors are indebted to Associate Professor Edward F. Barroga (D.V.M., Ph.D.), Senior Medical Editor of the Department of International Medical Communications of Tokyo Medical University, for the editorial review of the English manuscript.
Disclosures
Conflict of Interest: Akio Katanuma, Kei Yane, Manabu Osanai, and Hiroyuki Maguchi declare that they have no conflict of interest.
Human/Animal Rights: All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2008 (5).
Informed Consent: Informed consent was obtained from all patients included in the study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Katanuma, A., Yane, K., Osanai, M. et al. Endoscopic retrograde cholangiopancreatography in patients with surgically altered anatomy using balloon-assisted enteroscope. Clin J Gastroenterol 7, 283–289 (2014). https://doi.org/10.1007/s12328-014-0505-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12328-014-0505-3