Abstract
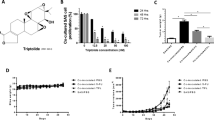
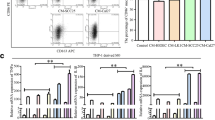
Fucoidan is a complex of polysaccharides showing antitumor and immunomodulation properties. Our previous studies found its regulation to myeloid immune cells, including macrophages. Aberrant infiltration and functions of macrophages are commonly found in oral squamous cell carcinoma (OSCC). In this study, we analyzed the effects of fucoidan on invasion of OSCC cells, and their regulation to macrophages, trying to evaluate its role as a potential therapy for OSCC. CAL27 and THP-1-derived macrophages were used as models for OSCC cells and tumor-infiltrated macrophages in the in vitro study, respectively. The effects of fucoidan on invasion of OSCC cells and their recruitment to macrophages were analyzed by transwell assay. KIF4A siRNA transfection was performed to investigate its role in fucoidan-modulated OSCC cells invasion. CCL3-neutralizing antibody was added into the conditioned medium of OSCC cells to evaluate its role in fucoidan-mediated macrophages recruitment and re-education. Fucoidan reduced the invasive potential of CAL27 cells with a decrease of MMP-2 and KIF4A transcription. KIF4A knockdown in CAL27 cells led to decreased invasion and MMP-2 expression. The conditioned medium of fucoidan-treated CAL27 cells promoted recruitment and inflammatory cytokines secretion on THP-1-derived macrophages. Further analysis found that fucoidan increased CCL3 production in CAL27 cells. Blocking CCL3 expression reversed the effects of fucoidan on macrophage recruitment and re-education. Our study found that fucoidan regulated the invasion of OSCC cells and also their recruiting and re-educating effects on macrophages, suggesting it could be a complementary approach in the treatment of OSCC.





Similar content being viewed by others
References
Argiris A, Karamouzis MV, Raben D, Ferris RL. Head Neck Cancer Lancet. 2008;371:1695–709. doi:10.1016/S0140-6736(08)60728-X.
Atashrazm F, Lowenthal RM, Woods GM, Holloway AF, Dickinson JL. Fucoidan and cancer: a multifunctional molecule with anti-tumor potential. Mar Drugs. 2015;13:2327–46. doi:10.3390/md13042327.
Bachmann A, Straube A. Kinesins in cell migration. Biochem Soc Trans. 2015;43:79–83. doi:10.1042/BST20140280.
Braun A, Dang K, Buslig F, Baird MA, Davidson MW, Waterman CM, Myers KA. Rac1 and Aurora A regulate MCAK to polarize microtubule growth in migrating endothelial cells. J Cell Biol. 2014;206:97–112. doi:10.1083/jcb.201401063.
Chinn SB, Myers JN. Oral cavity carcinoma: current management, controversies, and future directions. J Clin Oncol. 2015;33:3269–76. doi:10.1200/JCO.2015.61.2929.
Chizhov AO, et al. A study of fucoidan from the brown seaweed Chorda filum. Carbohydr Res. 1999;320:108–19.
Choi EM, Kim AJ, Kim YO, Hwang JK. Immunomodulating activity of arabinogalactan and fucoidan in vitro. J Med Food. 2005;8:446–53. doi:10.1089/jmf.2005.8.446.
Costa NL, Valadares MC, Souza PP, Mendonca EF, Oliveira JC, Silva TA, Batista AC. Tumor-associated macrophages and the profile of inflammatory cytokines in oral squamous cell carcinoma. Oral Oncol. 2013;49:216–23. doi:10.1016/j.oraloncology.2012.09.012.
Dong Z, et al. Leptin-mediated regulation of MT1-MMP localization is KIF1B dependent and enhances gastric cancer cell invasion. Carcinogenesis. 2013;34:974–83. doi:10.1093/carcin/bgt028.
Etienne-Manneville S. Microtubules in cell migration. Annu Rev Cell Dev Biol. 2013;29:471–99. doi:10.1146/annurev-cellbio-101011-155711.
Feinmesser M, et al. Histologic and immunohistochemical characterization of tumor and inflammatory infiltrates in oral squamous cell carcinomas treated with local multikine immunotherapy: the macrophage at the front line. Eur Arch Otorhinolaryngol. 2004;261:359–68. doi:10.1007/s00405-003-0615-x.
Hanahan D, Weinberg RA. Hallmarks of cancer: the next generation. Cell. 2011;144:646–74. doi:10.1016/j.cell.2011.02.013.
He KF, et al. CD163 + tumor-associated macrophages correlated with poor prognosis and cancer stem cells in oral squamous cell carcinoma. Biomed Res Int. 2014;2014:838632. doi:10.1155/2014/838632.
Heintz TG, Heller JP, Zhao R, Caceres A, Eva R, Fawcett JW. Kinesin KIF4A transports integrin beta1 in developing axons of cortical neurons. Mol Cell Neurosci. 2014;63:60–71. doi:10.1016/j.mcn.2014.09.003.
Jewett A, Head C, Cacalano NA. Emerging mechanisms of immunosuppression in oral cancers. J Dent Res. 2006;85:1061–73.
Lee KW, Jeong D, Na K. Doxorubicin loading fucoidan acetate nanoparticles for immune and chemotherapy in cancer treatment. Carbohydr Polym. 2013;94:850–6. doi:10.1016/j.carbpol.2013.02.018.
Liu X, Gong H, Huang K. Oncogenic role of kinesin proteins and targeting kinesin therapy. Cancer Sci. 2013;104:651–6. doi:10.1111/cas.12138.
Lu W, Fox P, Lakonishok M, Davidson MW, Gelfand VI. Initial neurite outgrowth in Drosophila neurons is driven by kinesin-powered microtubule sliding. Curr Biol. 2013;23:1018–23. doi:10.1016/j.cub.2013.04.050.
Maurer M, von Stebut E. Macrophage inflammatory protein-1. Int J Biochem Cell Biol. 2004;36:1882–6. doi:10.1016/j.biocel.2003.10.019.
Miki H, Okada Y, Hirokawa N. Analysis of the kinesin superfamily: insights into structure and function. Trends Cell Biol. 2005;15:467–76. doi:10.1016/j.tcb.2005.07.006.
Minakawa Y, et al. Kinesin family member 4A: a potential predictor for progression of human oral cancer. PLoS ONE. 2013;8:e85951. doi:10.1371/journal.pone.0085951.
Morris EJ, Nader GP, Ramalingam N, Bartolini F, Gundersen GG. Kif4 interacts with EB1 and stabilizes microtubules downstream of Rho-mDia in migrating fibroblasts. PLoS ONE. 2014;9:e91568. doi:10.1371/journal.pone.0091568.
Murdoch C, Muthana M, Coffelt SB, Lewis CE. The role of myeloid cells in the promotion of tumour angiogenesis. Nat Rev Cancer. 2008;8:618–31. doi:10.1038/nrc2444.
Nakashima E, et al. A candidate for cancer gene therapy: MIP-1 alpha gene transfer to an adenocarcinoma cell line reduced tumorigenicity and induced protective immunity in immunocompetent mice. Pharm Res. 1996;13:1896–901.
Nath A, Chattopadhya S, Chattopadhyay U, Sharma NK. Macrophage inflammatory protein (MIP)1alpha and MIP 1beta differentially regulate release of inflammatory cytokines and generation of tumoricidal monocytes in malignancy. Cancer Immunol Immunother. 2006;55:1534–41. doi:10.1007/s00262-006-0149-3.
Noy R, Pollard JW. Tumor-associated macrophages: from mechanisms to therapy. Immunity. 2014;41:49–61. doi:10.1016/j.immuni.2014.06.010.
Pollard TD, Borisy GG. Cellular motility driven by assembly and disassembly of actin filaments. Cell. 2003;112:453–65.
Qian BZ, Pollard JW. Macrophage diversity enhances tumor progression and metastasis. Cell. 2010;141:39–51. doi:10.1016/j.cell.2010.03.014.
Quan J, Johnson NW, Zhou G, Parsons PG, Boyle GM, Gao J. Potential molecular targets for inhibiting bone invasion by oral squamous cell carcinoma: a review of mechanisms. Cancer Metastasis Rev. 2012;31:209–19. doi:10.1007/s10555-011-9335-7.
Sun J, et al. Fucoidan increases TNF-alpha-induced MMP-9 secretion in monocytic cell line U937. Inflamm Res. 2010;59:271–6. doi:10.1007/s00011-009-0095-6.
Torre LA, Bray F, Siegel RL, Ferlay J, Lortet-Tieulent J, Jemal A. Global cancer statistics, 2012. CA Cancer J Clin. 2015;65:87–108. doi:10.3322/caac.21262.
Vandenbroucke RE, Libert C. Is there new hope for therapeutic matrix metalloproteinase inhibition? Nat Rev Drug Discovery. 2014;13:904–27. doi:10.1038/nrd4390.
Wang CQ, et al. Overexpression of Kif2a promotes the progression and metastasis of squamous cell carcinoma of the oral tongue. Oral Oncol. 2010;46:65–9. doi:10.1016/j.oraloncology.2009.11.003.
Wang H, et al. Leptin-promoted human extravillous trophoblast invasion is MMP14 dependent and requires the cross talk between Notch1 and PI3K/Akt signaling. Biol Reprod. 2014;90:78. doi:10.1095/biolreprod.113.114876.
Weber M, et al. Small oral squamous cell carcinomas with nodal lymphogenic metastasis show increased infiltration of M2 polarized macrophages—an immunohistochemical analysis. J Craniomaxillofac Surg. 2014;42:1087–94. doi:10.1016/j.jcms.2014.01.035.
Wehrhan F, et al. Increased malignancy of oral squamous cell carcinomas (oscc) is associated with macrophage polarization in regional lymph nodes—an immunohistochemical study. BMC Cancer. 2014;14:522. doi:10.1186/1471-2407-14-522.
Wiesner C, Faix J, Himmel M, Bentzien F, Linder S. KIF5B and KIF3A/KIF3B kinesins drive MT1-MMP surface exposure, CD44 shedding, and extracellular matrix degradation in primary macrophages. Blood. 2010;116:1559–69. doi:10.1182/blood-2009-12-257089.
Wu Y, Li YY, Matsushima K, Baba T, Mukaida N. CCL3-CCR5 axis regulates intratumoral accumulation of leukocytes and fibroblasts and promotes angiogenesis in murine lung metastasis process. J Immunol. 2008;181:6384–93.
Yang M, et al. Fucoidan stimulation induces a functional maturation of human monocyte-derived dendritic cells. Int Immunopharmacol. 2008;8:1754–60. doi:10.1016/j.intimp.2008.08.007.
Zhao P, et al. Response gene to complement 32 (RGC-32) expression on M2-polarized and tumor-associated macrophages is M-CSF-dependent and enhanced by tumor-derived IL-4. Cell Mol Immunol. 2015;12:692–9. doi:10.1038/cmi.2014.108.
Acknowledgements
This work was supported by the National Natural Science Foundation of China (Grant Numbers 81271105, 31470885 and 31270971).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
All the authors declare no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Junda Lin and Ketao Wang have contributed equally to this work.
Rights and permissions
About this article
Cite this article
Lin, J., Wang, K., Wang, H. et al. Fucoidan reduced the invasion of oral squamous cell carcinoma cells and modified their effects to macrophages. Med Oncol 34, 9 (2017). https://doi.org/10.1007/s12032-016-0858-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12032-016-0858-1