Abstract
Purpose
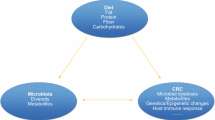
Adenoma is the most common benign neoplasm with potential to progress into colorectal cancer (CRC), a disease responsible for high rates of mortality. However, it is not possible yet to establish which lesions will evolve into CRC. We aimed to investigate the intrinsic factors, diet profile, and microenvironment as factors involved in adenoma-CRC progression.
Methods
We evaluated nutritional profile and microscopic features. Adenomas and CRC lesions were stained with Mallory’s trichrome to reveal fibrosis and Alcian blue to identify mast cells.
Results
A total of 143 patients was selected, 66 % diagnosed with normal mucosa, 28.4 % with benign lesion, and 5.6 % with CRC. A higher frequency of lesions was associated with patients older than 50 years (26.57 %) and women (18.18 %), but men were more likely to develop CRC. Regarding microscopic aspects, epithelium-connective tissue interface with disorganization feature was significantly higher in CRC when compared to adenoma (P = 0.0007). A greater fibrosis around vessels was also observed in CRC (P = 0.01). The statistical analysis indicated a significant correlation between mast cell population and patients older than 50 years (P < 0.01), male (P < 0.01), with right colon lesion (P < 0.05) and CRC. Low consumption of leafy greens (P < 0.001) and carotenoids (P < 0.01) and elevated consumption of red meat (P < 0.001) were associated with a high density of mast cells.
Conclusions
An association between clinical, diet profile, and microscopic features in colorectal lesions was observed, with a progressive change in the microenvironment during adenoma-CRC sequence.



Similar content being viewed by others
Abbreviations
- CRC:
-
colorectal cancer
- ECM:
-
extracellular matrix
- DNA:
-
deoxyribonucleic acid
- TNFα:
-
tumor necrosis factor alpha
References
Jemal A, Bray F, Center MM, Ferlay J, Ward E, Forman D. Global cancer statistics. CA Cancer J Clin. 2011;61:69–90. doi:10.3322/caac.20107.
Mansouri D, McMillan DC, Grant Y, Crighton EM, Horgan PG. The impact of age, sex and socioeconomic deprivation on outcomes in a colorectal cancer screening programme. PLoS One. 2013;8(6):e66063. doi:10.1371/journal.pone.0066063.
Hjartåker A, Aagnes B, Robsahm TE, Langseth H, Bray F, Larsen IK. Subsite-specific dietary risk factors for colorectal cancer: a review of cohort studies. J Oncol. 2013;2013:1–14. doi:10.1155/2013/703854.
Haas SL, Ye W, Löhr JM. Alcohol consumption and digestive tract cancer. Curr Opin Clin Nutr Metab Care. 2012;15(5):457–67. doi:10.1097/MCO.0b013e3283566699.
Koh WP, Nelson HH, Yuan JM, Van den Berg D, Jin A, Wang R, et al. Glutathione S-transferase (GST) gene polymorphisms, cigarette smoking and colorectal cancer risk among Chinese in Singapore. Carcinogenesis. 2011;32(10):1507–11. doi:10.1093/carcin/bgr175.
Murphy N, Norat T, Ferrari P, Jenab M, Bueno-de-Mesquita B, Skeie G, et al. Dietary fiber intake and risks of cancers of the colon and rectum in the European prospective investigation into cancer and nutrition (EPIC). PLoS One. 2012;7(6):e39361. doi:10.1371/journal.pone.0039361.
Aune D, Lau R, Chan DS, Vieira R, Greenwood DC, Kampman E, et al. Dairy products and colorectal cancer risk: a systematic review and meta-analysis of cohort studies. Ann Oncol. 2012;23(1):37–45. doi:10.1093/annonc/mdr269.
Burton AM, Hovick SR, Peterson SK. Health behaviors in patients and families with hereditary colorectal cancer. Clin Colon Rectal Surg. 2012;25(2):111–7. doi:10.1055/s-0032-1313782.
Levental KR, Yu H, Kass L, Lakins JN, Egeblad M, Erler JT, et al. Matrix cross linking forces tumor progression by enhancing integrin signaling. Cell. 2009;139(5):891–906. doi:10.1016/j.cell.2009.10.027.
Wyckoff JB, Wang Y, Lin EY, Li JF, Goswami S, Stanley ER, et al. Direct visualization of macrophage-assisted tumor cell intravasation in mammary tumors. Cancer Res. 2007;67(6):2649–56.
Zhao LW, Li C, Zhang RL, Xue HG, Zhang FX, Zhang F, et al. B7-H1 and B7-H4 expression in colorectal carcinoma: correlation with tumor FOXP3+ regulatory T-cell infiltration. Acta Histochem. 2014;116(7):1163–8. doi:10.1016/j.acthis.2014.06.003.
Ribatti D. Mast cells as therapeutic target in cancer. Eur J Pharmacol. 2015;S0014–2999(15):00356–8. doi:10.1016/j.ejphar.2015.02.056.
Midulla F, Tromba V, Lo Russo L, Mileto F, Sabatino G, Sgarrella M, et al. Cytokines in the nasal washes of children with respiratory syncytial virus bronchiolitis. Int J Immunopathol Pharmacol. 2006;19(1):231–5.
Theoharides TC, Conti P. Mast cells: the Jekyll and Hyde of tumor growth. Trends Immunol. 2004;25(5):235–41.
Fisher ER, Sass R, Watkins G, Johal J, Fisher B. Tissue mast cells in breast cancer. Breast Cancer Res Treat. 1985;5(3):285–91.
Veen T, Stormark K, Nedrebø BS, Berg M, Søreide JA, Kørner H, et al. Long-term follow-up and survivorship after completing systematic surveillance in stage I–III colorectal cancer: who is still at risk? J Gastrointest Cancer. 2015;46(3):259–66. doi:10.1007/s12029-015-9723-2.
Winawer SJ, Fletcher RH, Miller L, Godlee F, Stolar MH, Mulrow CD, et al. Colorectal cancer screening: clinical guidelines and rationale. Gastroenterology. 1997;112(2):594–642.
Meguid RA, Slidell MB, Wolfgang CL, Chang DC, Ahuja N. Is there a difference in survival between right- versus left-sided colon cancers? Ann Surg Oncol. 2008;15(9):2388–94. doi:10.1245/s10434-008-0015-y.
Paszek MJ, Weaver VM. The tension mounts: mechanics meets morphogenesis and malignancy. J Mammary Gland Biol Neoplasia. 2004;9(4):325–42.
Paszek MJ, Zahir N, Johnson KR, Lakins JN, Rozenberg GI, Gefen A, et al. Tensional homeostasis and the malignant phenotype. Cancer Cell. 2005;8(3):241–54.
Higashi N, Ishii H, Fujiwara T, Morimoto-Tomita M, Irimura T. Redistribution of fibroblasts and macrophages as micrometastases develop into established liver metastases. Clin Exp Metastasis. 2002;19(7):631–8.
Ch’ng S, Wallis RA, Yuan L, Davis PF, Tan ST. Mast cells and cutaneous malignancies. Mod Pathol. 2006;19(1):149–59.
Yang Z, Zhang B, Li D, Lv M, Huang C, Shen GX, et al. Mast cells mobilize myeloid-derived suppressor cells and Treg cells in tumor microenvironment via IL-17 pathway in murine hepatocarcinoma model. PLoS One. 2010;5(1):e8922. doi:10.1371/journal.pone.0008922.
Malfettone A, Silvestris N, Saponaro C, Ranieri G, Russo A, Caruso S, et al. High density of tryptase-positive mast cells in human colorectal cancer: a poor prognostic factor related to protease-activated receptor 2 expression. J Cell Mol Med. 2013;17(8):1025–37. doi:10.1111/jcmm.12073.
Coussens LM, Raymond WW, Bergers G, Laig-Webster M, Behrendtsen O, Werb Z, et al. Inflammatory mast cells up-regulate angiogenesis during squamous epithelial carcinogenesis. Genes Dev. 1999;13(11):1382–97.
Kim MS, Chae HJ, Shin TY, Kim HM, Kim HR. Estrogen regulates cytokine release in human mast cells. Immunopharmacol Immunotoxicol. 2001;23(4):495–504.
Mahay S, Pariente JA, Lajas AI, Adeghate E, Rolph CE, Singh J. Effects of ageing on morphology, amylase release, cytosolic Ca2+ signals and acyl lipids in isolated rat parotid gland tissue. Mol Cell Biochem. 2004;266(1-2):199–208.
Ishikawa S, Tamaki S, Ohata M, Arihara K, Itoh M. Heme induces DNA damage and hyperproliferation of colonic epithelial cells via hydrogen peroxide produced by hemeoxygenase: a possible mechanism of heme-induced colon cancer. Mol Nutr Food Res. 2010;54(8):1182–91. doi:10.1002/mnfr.200900348.
Vergara-Castañeda HA, Guevara-González RG, Ramos-Gómez M, Reynoso-Camacho R, Guzmán-Maldonado H, Feregrino-Pérez AA, et al. Non-digestible fraction of cooked bean (Phaseolusvul- garis L.) cultivar Bayo Madero suppresses colonic aberrant crypt foci in azoxymethane-induced rats. Food Funct. 2010;1(3):294–300. doi:10.1039/c0fo00130a.
Campos-Vega R, Reynoso-Camacho R, Pedraza-Aboytes G, Acosta-Gallegos JA, Guzman-Maldonado SH, Paredes-Lopez O, et al. Chemical composition and in vitro polysaccharide fermentation of different beans (Phaseolus vulgaris L.). J Food Sci. 2009;74(7):T59–65. doi:10.1111/j.1750-3841.2009.01292.x.
Acknowledgments
This work was supported by grants from Brazilian National Council for Scientific and Technological Development (CNPq) process number: 479694 2013-3 and the State of Espírito Santo Research Foundation (FAPES) process number: 67659870 006/2014. The funding sources did not participate in any part of this study.
The authors gratefully acknowledge Rossini Cipriano Gama, Vitória ApartHospital, Service of Coloproctology, which provided valuable help during the medical procuderes.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no conflict of interest.
Authors’ Contributions
ISSA participated in all phases of this study. PHPC performed the questionnaire applied and histological analysis to identify mast cells. GJZL and LPNG were responsible to medical procedures. FR was responsible to histopathological diagnosis. WGB, KLAC, and MSP contributed to the data analysis and interpretation. LNGS designed the study and participated in all phases. All authors contributed to the manuscript writing, revision, and final approval of this paper.
Rights and permissions
About this article
Cite this article
Alves, I.S.S., Coser, P.H.P., Loureiro, G.J.Z. et al. Fibrosis and Mast Cells in Colorectal Lesions: Significance in Adenoma-Colorectal Cancer Sequence and Association with Diet. J Gastrointest Canc 47, 278–286 (2016). https://doi.org/10.1007/s12029-016-9829-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12029-016-9829-1