Abstract
Background
Spontaneous intracranial hypotension has become a well-recognized cause of headaches and a wide variety of other manifestations have been reported. Recently, several patients with asymptomatic spontaneous intracranial hypotension were reported. I now report two patients with spontaneous intracranial hypotension who developed multiple arterial strokes associated with death in one patient, illustrating the spectrum of disease severity in spontaneous intracranial hypotension.
Methods
Medical records and radiologic imaging of the two patients were reviewed.
Results
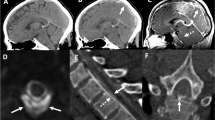
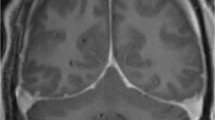
Case 1. A 45-year-old man presented with an orthostatic headache. Neurologic examination was normal. MRI showed bilateral subdural fluid collections, brain sagging, and pachymeningeal enhancement. At lumbar puncture, the opening pressure was too low to record. He underwent two epidural blood patches with transient improvement of symptoms. His headaches progressed and a CT-myelogram showed a lower cervical CSF leak. Subsequently, periodic lethargy and confusion was noted and he then rapidly deteriorated. Examination showed coma (GCS: 4 [E1, M2, V1]), a fixed and dilated right pupil, and decerebrate posturing. Bilateral craniotomies were performed for the evacuation of chronic subdural hematomas. Immediate postoperative CT showed bilateral posterior cerebral artery infarcts and a recurrent right subdural hematoma, requiring re-evacuation. Postoperative examination was consistent with brain death and support was withdrawn. Case 2. A 42-year-old man presented with a non-positional headache. Neurologic examination was normal. CT showed bilateral acute on chronic subdural hematomas and effacement of the basilar cisterns. MRI showed brain sagging, bilateral subdural hematomas, and pachymeningeal enhancement. Bilateral craniotomies were performed and subdural hematomas were evacuated. Postoperatively, the patient became progressively lethargic (GCS: 8 [E2, M4, V2]) and variable degrees of pupillary asymmetry and quadriparesis were noted. MRI now also showed multiple areas of restricted diffusion in the pons and midbrain, consistent with multiple infarcts. CT showed worsening subdural fluid collections with midline shift and increased effacement of the basilar cisterns. Repeat bilateral craniotomies were performed for evacuation of the subdural fluid collections. Neurologic examination was then noted to be fluctuating but clearly improved when lying flat (GCS: 10T [E4, M6, VT]). CT-myelography demonstrated an extensive cervico-thoracic CSF leak. An epidural blood patch was performed. The patient made a good, but incomplete, recovery with residual quadriparesis and dysphagia.
Conclusions
Arterial cerebral infarcts are rare, but potentially life-threatening complications of spontaneous intracranial hypotension. The strokes are due to downward displacement of the brain and can be precipitated by craniotomy for evacuation of associated subdural hematomas.

Similar content being viewed by others
References
Schievink WI. Spontaneous spinal cerebrospinal fluid leaks and intracranial hypotension. JAMA. 2006;295:2286–96.
Schwedt TJ, Dodick DW. Spontaneous intracranial hypotension. Curr Pain Headache Rep. 2007;11:56–61.
Schievink WI, Mamelak AN, Maya MM. Spontaneous intracranial hypotension as an incidental finding on MRI. Neurology. 2012;79:1298–9.
Billings JJ, Gilford EJ, Henderson JK. The low intracranial pressure syndrome. Proc Aust Assoc Neurol. 1975;12:31–4.
Fishman RA, Dillon WP. Dural enhancement and cerebral displacement secondary to intracranial hypotension. Neurology. 1993;43:609–11.
Schievink WI, Maya MM, Tourje J, Moser FG. Pseudo-subarachnoid hemorrhage: a CT-finding in spontaneous intracranial hypotension. Neurology. 2005;65:135–7.
Kelley GR, Johnson PL. Sinking brain syndrome: craniotomy can precipitate brainstem herniation in CSF hypovolemia. Neurology. 2004;62:157.
Schievink WI, Palestrant D, Maya MM, Rappard G. Spontaneous spinal cerebrospinal fluid leak as a cause of a coma after craniotomy for clipping of an unruptured intracranial aneurysm. J Neurosurg. 2009;110:521–4.
Lai TH, Fuh JL, Lirng JF, Tsai PH, Wang SJ. Subdural haematoma in patients with spontaneous intracranial hypotension. Cephalalgia. 2007;27:133–8.
Chi NF, Wang SJ, Lirng JF, Fuh JL. Transtentorial herniation with cerebral infarction and duret haemorrhage in a patient with spontaneous intracranial hypotension. Cephalalgia. 2007;27:279–82.
Whiteley W, Al-Shahi R, Myles L, Lueck CJ. Spontaneous intracranial hypotension causing confusion and coma: a headache for the neurologist and the neurosurgeon. Br J Neurosurg. 2003;17:456–8.
Han SR, Kim YJ, Kim YI, Lee KS, Kim BS, Choo SW. A case report of unexpected clinical course of spontaneous intracranial hypotension. J Korean Neurol Assoc. 1995;13:129–33.
Acknowledgments
I acknowledge the assistance of the attending neurosurgeons who cared for these patients and gave permission to publish this report.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Schievink, W.I. Stroke and Death Due to Spontaneous Intracranial Hypotension. Neurocrit Care 18, 248–251 (2013). https://doi.org/10.1007/s12028-012-9800-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-012-9800-3