Abstract
Background
Little is known about the efficacy of single versus dual extraventricular drain (EVD) use in intraventricular hemorrhage (IVH), with and without thrombolytic therapy.
Methods
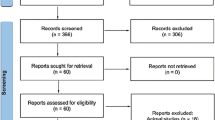
Post-hoc analysis of seven patients with dual bilateral EVDs from two multicenter trials involving 100 patients with IVH, and spontaneous intracerebral hemorrhage (ICH) volume <30 ml requiring emergency external ventricular drainage. Seven “control” patients with single catheters were matched by IVH volume and distribution and treatment assignment. Head CT scans were obtained daily during intraventricular injections for quantitative determination of IVH volume.
Results
Median [min–max] age of the 14 subjects was 56 [40–73] years. Median duration of EVD was 7.9 days (single catheter group) versus 12.2 days (dual catheter group) (P = 0.34). Baseline median IVH volume was not significantly different between groups (75.4 ml [22.4–105.1]—single EVD vs. 84.5 ml [42.0–132.0]—dual EVD; P = 0.28). Comparing the change in IVH volume on time-matched CT scans during dual EVD use, the median decrease in IVH volume in dual catheter patients was significantly larger (52.1 [31.7–81.1] ml) versus single catheter patients (34.5 [13.1–73.9] ml) (P = 0.004). There was a trend to greater decrease in IVH volume during dual EVD use in both rt-PA (P = 0.9) and placebo-treated (P = 0.11) subgroups.
Conclusion
The decision to place dual EVDs is generally reserved for large IVH (>40 ml) with casting and mass effect. The use of dual simultaneous catheters may increase clot resolution with or without adjunctive thrombolytic therapy.


Similar content being viewed by others
References
Vereecken KK, Van Havenbergh T, De Beuckelaar W, Parizel PM, Jorens PG. Treatment of intraventricular hemorrhage with intraventricular administration of recombinant tissue plasminogen activator. A clinical study of 18 cases. Clin Neurol Neurosurg. 2006;108(5):451–5.
Coplin WM, Vinas FC, Agris JM, et al. A cohort study of the safety and feasibility of intraventricular urokinase for nonaneurysmal spontaneous intraventricular hemorrhage. Stroke. 1998;29(8):1573–9.
Findlay JM, Grace MG, Weir BK. Treatment of intraventricular hemorrhage with tissue plasminogen activator. Neurosurgery. 1993;32(6):941–7. (discussion 947).
Andrews CO, Engelhard HH. Fibrinolytic therapy in intraventricular hemorrhage. Ann Pharmacother. 2001;35(11):1435–48.
Naff NJ, Carhuapoma JR, Williams MA, et al. Treatment of intraventricular hemorrhage with urokinase : effects on 30-Day survival. Stroke. 2000;31(4):841–7.
Staykov D, Huttner HB, Lunkenheimer J, et al. Single versus bilateral external ventricular drainage for intraventricular fibrinolysis in severe ventricular haemorrhage. J Neurol Neurosurg Psychiatry. 2010;81(1):105–8.
Kothari RU, Brott T, Broderick JP, et al. The ABCs of measuring intracerebral hemorrhage volumes. Stroke. 1996;27(8):1304–5.
Graeb DA, Robertson WD, Lapointe JS, Nugent RA, Harrison PB. Computed tomographic diagnosis of intraventricular hemorrhage. Etiology and prognosis. Radiology. 1982;143(1):91–6.
Pang D, Sclabassi RJ, Horton JA. Lysis of intraventricular blood clot with urokinase in a canine model: Part 1. Canine intraventricular blood cast model. Neurosurgery. 1986;19(4):540–6.
Mayfrank L, Kissler J, Raoofi R, et al. Ventricular dilatation in experimental intraventricular hemorrhage in pigs. Characterization of cerebrospinal fluid dynamics and the effects of fibrinolytic treatment. Stroke. 1997;28(1):141–8.
Acknowledgments
CLEAR IVH is sponsored by the FDA orphan drug program, assisted by a donation from Cathflo and a sponsored research agreement with Genentech. Use Patent holder: Johns Hopkins Medical Institutions. Drs. Hanley and Naff hold an Investigator IND for the use of intracerebral rt-PA.
Conflict of interest
Dr. Hinson, Mr. Melnychuk, and Mr. Muschelli have nothing to disclose. Dr. Hanley has received research support as PI of the CLEAR IVH trial, which is sponsored by the FDA Orphan Drug Program assisted by a donation from Cathflo and a sponsored research agreement from Genentech. Dr. Ziai has received personal compensation in an editorial capacity for Current Opinion in Neurology.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hinson, H.E., Melnychuk, E., Muschelli, J. et al. Drainage Efficiency with Dual Versus Single Catheters in Severe Intraventricular Hemorrhage. Neurocrit Care 16, 399–405 (2012). https://doi.org/10.1007/s12028-011-9569-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-011-9569-9