Abstract
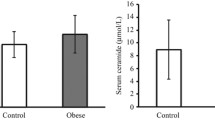
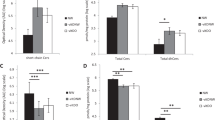
The purpose of this study was to determine low-grade inflammation associated with obesity that is mediated partially by TNF-α, an adipocytokine which stimulates sphingomyelinase activity in adipocytes. Circulating ceramide (Cer) and sphingosine 1-phosphate (S1P) are elevated in genetically obese (ob/ob) mice. We aimed to determine whether serum sphingolipid concentrations correlate with measures of obesity, insulin resistance, and lipid profiles in overweight versus lean adolescents. This cross-sectional study recruited 30 healthy overweight (body mass index, BMI ≥ 85%) and 15 lean (BMI 10–84%) adolescents. Anthropometric measurements and fasting blood samples were collected at one clinic visit. Serum glucose, insulin, and fasting lipid profiles were measured. Serum adipocytokine concentrations were measured by ELISA or colorimetric assay and sphingolipids were measured by HPLC–mass spectrometry. Between group differences in serum sphingolipid concentrations were assessed. Correlations between sphingolipid concentrations and (i) body mass index, (ii) calculated homeostasis model assessment of insulin resistance (HOMA-IR), (iii) adipocytokines, and (iv) lipoproteins were determined. The results showed that significant differences in HOMA-IR (4.5 ± 3.2 vs. 1.2 ± 0.7), free fatty acids (0.8 ± 0.3 mmol/l vs. 0.4 ± 0.3 mmol/l), and adiponectin (6.4 ± 3.8 vs. 12.6 ± 9.9 μg/ml) were seen between groups (overweight vs. lean). There were significant correlations between Cer and TNF-α (r = 0.429), S1P and TNF-α (r = 0.288), Cer and adiponectin (r = 0.321), Cer:S1P and adiponectin (r = 0.324), Cer and HOMA-IR (r = 0.307), and Cer:S1P and LDL cholesterol (r = 0.453); these associations persisted after adjustment for BMI Z-score, sex, and Tanner stage. We concluded that elevated sphingolipid concentrations correlate with TNF-α, adiponectin, lipoprotein profiles, and HOMA-IR. Ceramide is associated with atherogenic lipid profiles and the development of insulin resistance in obese adolescents, similar to adults.

Similar content being viewed by others
References
C. Ogden, M. Carroll, NCHS health e-stat: prevalence of obesity among children and adolescents: United States, trends 1963–1965 through 2007–2008. http://www.cdc.gov/nchs/data/hestat/obesity_child_07_08/obesity_child_07_08.htm (2010). Accessed 12 December 2011
R. Sinha, G. Fisch, B. Teague, W.V. Tamborlane, B. Banyas, K. Allen, M. Savoye, V. Rieger, S. Taksali, G. Barbetta, R.S. Sherwin, S. Caprio, Prevalence of impaired glucose tolerance among children and adolescents with marked obesity. N. Engl. J. Med. 346(11), 802–810 (2002)
Y. Aggoun, Obesity, metabolic syndrome, and cardiovascular disease. Pediatr. Res. 61(6), 653–659 (2007)
P.W. Wilson, R.B. D’Agostino, H. Parise, L. Sullivan, J.B. Meigs, Metabolic syndrome as a precursor of cardiovascular disease and type 2 diabetes mellitus. Circulation 112(20), 3066–3072 (2005)
J.C. Pickup, Inflammation and activated innate immunity in the pathogenesis of type 2 diabetes. Diabetes Care 27(3), 813–823 (2004)
C. Herder, S. Schneitler, W. Rathmann, B. Haastert, H. Schneitler, H. Winkler, R. Bredahl, E. Hahnloser, S. Martin, Low-grade inflammation, obesity, and insulin resistance in adolescents. J. Clin. Endocrinol. Metab. 92(12), 4569–4574 (2007)
I. Aeberli, L. Molinari, G. Spinas, R. Lehmann, D. l’Allemand, M.B. Zimmermann, Dietary intakes of fat and antioxidant vitamins are predictors of subclinical inflammation in overweight Swiss children. Am. J. Clin. Nutr. 84(4), 748–755 (2006)
Y.S. Moon, D.H. Kim, D.K. Song, Serum tumor necrosis factor-alpha levels and components of the metabolic syndrome in obese adolescents. Metabolism 53(7), 863–867 (2004)
P. Peraldi, G.S. Hotamisligil, W.A. Buurman, M.F. White, B.M. Spiegelman, Tumor necrosis factor (TNF)-alpha inhibits insulin signaling through stimulation of the p55 TNF receptor and activation of sphingomyelinase. J. Biol. Chem. 271(22), 13018–13022 (1996)
Y.A. Hannun, The sphingomyelin cycle and the second messenger function of ceramide. J. Biol. Chem. 269(5), 3125–3128 (1994)
S. Spiegel, O. Cuvillier, L.C. Edsall, T. Kohama, R. Menzeleev, Z. Olah, A. Olivera, G. Pirianov, D.M. Thomas, Z. Tu, J.R. Van Brocklyn, F. Wang, Sphingosine-1-phosphate in cell growth and cell death. Ann. N. Y. Acad. Sci. 845, 11–18 (1998)
J.M. Haus, S.R. Kashyap, T. Kasumov, R. Zhang, K.R. Kelly, R.A. DeFronzo, J.P. Kirwan, Plasma ceramides are elevated in obese subjects with type 2 diabetes and correlate with the severity of insulin resistance. Diabetes 58(2), 337–343 (2009)
H. Huang, T. Kasumov, P. Gatmaitan, H.M. Heneghan, S.R. Kashyap, P.R. Schauer, S.A. Brethauer, J.P. Kirwan, Gastric bypass surgery reduces plasma ceramide subspecies and improves insulin sensitivity in severely obese patients. Obesity 19, 2235–2240 (2011)
L. Wang, X.P. Xing, A. Holmes, C. Wadham, J.R. Gamble, M.A. Vadas, P. Xia, Activation of the sphingosine kinase-signaling pathway by high glucose mediates the proinflammatory phenotype of endothelial cells. Circ. Res. 97(9), 891–899 (2005)
D. English, Z. Welch, A.T. Kovala, K. Harvey, O.V. Volpert, D.N. Brindley, J.G. Garcia, Sphingosine 1-phosphate released from platelets during clotting accounts for the potent endothelial cell chemotactic activity of blood serum and provides a novel link between hemostasis and angiogenesis. FASEB J. 14(14), 2255–2265 (2000)
N. Murata, K. Sato, J. Kon, H. Tomura, M. Yanagita, A. Kuwabara, M. Ui, F. Okajima, Interaction of sphingosine 1-phosphate with plasma components, including lipoproteins, regulates the lipid receptor-mediated actions. Biochem. J. 352(Pt 3), 809–815 (2000)
P. Hanel, P. Andreani, M.H. Graler, Erythrocytes store and release sphingosine 1-phosphate in blood. FASEB J. 21(4), 1202–1209 (2007)
O. Cuvillier, G. Pirianov, B. Kleuser, P.G. Vanek, O.A. Coso, S. Gutkind, S. Spiegel, Suppression of ceramide-mediated programmed cell death by sphingosine-1-phosphate. Nature 381(6585), 800–803 (1996)
F. Samad, K.D. Hester, G. Yang, Y.A. Hannun, J. Bielawski, Altered adipose and plasma sphingolipid metabolism in obesity: a potential mechanism for cardiovascular and metabolic risk. Diabetes 55(9), 2579–2587 (2006)
R.J. Kuczmarski, C.L. Ogden, S.S. Guo, L.M. Grummer-Strawn, K.M. Flegal, Z. Mei, R. Wei, L.R. Curtin, A.F. Roche, C.L. Johnson, 2000 CDC growth charts for the United States: methods and development. Vital Health Stat. 11(246), 1–190 (2002)
H. Yokoyama, M. Emoto, S. Fujiwara, K. Motoyama, T. Morioka, M. Komatsu, H. Tahara, T. Shoji, Y. Okuno, Y. Nishizawa, Quantitative insulin sensitivity check index and the reciprocal index of homeostasis model assessment in normal range weight and moderately obese type 2 diabetic patients. Diabetes Care 26(8), 2426–2432 (2003)
B. Rosner, R.J. Prineas, J.M. Loggie, S.R. Daniels, Blood pressure nomograms for children and adolescents, by height, sex, and age, in the United States. J. Pediatr. 123(6), 871–886 (1993)
C. Li, E.S. Ford, A.H. Mokdad, S. Cook, Recent trends in waist circumference and waist-height ratio among US children and adolescents. Pediatrics 118(5), e1390–e1398 (2006)
S. Cook, P. Auinger, C. Li, E.S. Ford, Metabolic syndrome rates in United States adolescents, from the National Health and Nutrition Examination Survey, 1999–2002. J. Pediatr. 152(2), 165–170 (2008)
J.M. Lee, M.J. Okumura, M.M. Davis, W.H. Herman, J.G. Gurney, Prevalence and determinants of insulin resistance among US adolescents. Diabetes Care 29(11), 2427–2432 (2006)
A. Gupta, S. Ten, H. Anhalt, Serum levels of soluble tumor necrosis factor-alpha receptor 2 are linked to insulin resistance and glucose intolerance in children. J. Pediatr. Endocrinol. Metab. 18(1), 75–82 (2005)
R. Weiss, J. Dziura, T.S. Burgert, W.V. Tamborlane, S.E. Taksali, C.W. Yeckel, K. Allen, M. Lopes, M. Savoye, J. Morrison, R.S. Sherwin, S. Caprio, Obesity and the metabolic syndrome in children and adolescents. N. Engl. J. Med. 350(23), 2362–2374 (2004)
M. Nikolova-Karakashian, E.T. Morgan, C. Alexander, D.C. Liotta, A.H. Merrill Jr., Bimodal regulation of ceramidase by interleukin-1beta. Implications for the regulation of cytochrome p450 2C11. J. Biol. Chem. 272(30), 18718–18724 (1997)
L.D. Mastrandrea, S.M. Sessanna, S.G. Laychock, Sphingosine kinase activity and sphingosine-1 phosphate production in rat pancreatic islets and INS-1 cells: response to cytokines. Diabetes 54(5), 1429–1436 (2005)
A.U. Blachnio-Zabielska, M. Pulka, M. Baranowski, A. Nikolajuk, P. Zabielski, M. Górska, J. Górski, Ceramide metabolism is affected by obesity and diabetes in human adipose tissue. J. Cell Physiol. 227, 550–557 (2012)
S.M. Hammad, J.S. Pierce, F. Soodavar, K.J. Smith, M.M. Al Gadban, B. Rembiesa, R.L. Klein, Y.A. Hannun, J. Bielawski, A. Bielawska, Blood sphingolipidomics in healthy humans: impact of sample collection methodology. J. Lipid Res. 51(10), 3074–3087 (2010)
G. Delogu, G. Famularo, F. Amati, L. Signore, A. Antonucci, V. Trinchieri, L. Di Marzio, M.G. Cifone, Ceramide concentrations in septic patients: a possible marker of multiple organ dysfunction syndrome. Crit. Care Med. 27(11), 2413–2417 (1999)
Acknowledgments
The authors would like to thank Kathleen Bethin, MD, PhD, Suzanne Laychock, PhD, and Joan Dorn, PhD for their thoughtful review and helpful comments concerning this manuscript. The authors would also like to thank Lisa B. Rafalson, PhD and Chang-Xing Ma, PhD for their assistance with statistical analysis.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Majumdar, I., Mastrandrea, L.D. Serum sphingolipids and inflammatory mediators in adolescents at risk for metabolic syndrome. Endocrine 41, 442–449 (2012). https://doi.org/10.1007/s12020-011-9589-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-011-9589-4