Abstract
Background
Backside damage of the polyethylene in TKA is a potential source of debris. The location of the tibial post in posterior-stabilized implants may influence micromotion, and thus affect backside damage, as may surface roughness.
Questions
We used implant retrieval analysis to (1) examine if there were differences in backside damage among three modern posterior-stabilized implants attributable to variable surface roughness; (2) determine if the location of damage on the tibial post affected the pattern of backside damage; and (3) determine if demographics influenced backside damage.
Methods
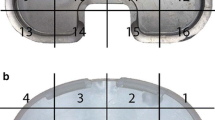
We identified 403 posterior-stabilized tibial retrieved inserts (147 NexGen®, 152 Optetrak®, 104 Genesis® II). The damage on the surfaces of the tibial posts was previously graded. The backside of the inserts (divided into quadrants) were scored for evidence of damage. The total quadrant damage was compared for each implant group, the relationship between post face damage and location of damage on the backside was determined for each implant group, and total backside damage was compared among the three implant groups.
Results
No correlation was found between the location of damage on the post and location of damage on the backside of the implant for any of the three groups. The Genesis® II polyethylene implants, which articulate with a highly polished tibial tray, showed a significantly lower total backside damage score (p < 0.01) when compared with the other two implant groups. The Genesis® II and Optetrak® showed significantly more damage in the posterior quadrants of the implants (p < 0.01) when compared with the anterior quadrants. A linear regression analysis revealed that lower tibial tray surface roughness was correlated with decreased damage.
Conclusions
An implant design with a highly polished tibial tray was associated with decreased backside damage. However, tibial post design and location did not influence the location of backside damage.
Clinical Relevance
Our study showed that a highly polished tibial tray was associated with decreased damage to the backside of polyethylene inserts independent of post design and location. These findings should be taken into consideration when new generations of implants are designed.


Similar content being viewed by others
References
Barrack RL. Modularity of Prosthetic Implants. J Am Acad Orthop Surg. 1994;2:16–25.
Bartel DL, Burstein AH, Santavicca EA, Insall JN. Performance of the tibial component in total knee replacement. J Bone Joint Surg Am. 1982;64:1026–1033.
Berry DJ, Currier JH, Mayor MB, Collier JP. Knee wear measured in retrievals: a polished tray reduces insert wear. Clin Orthop Relat Res. 2012;470:1860–1868.
Billi F, Sangiorgio SN, Aust S, Ebramzadeh E. Material and surface factors influencing backside fretting wear in total knee replacement tibial components. J Biomech. 2010;43:1310–1315.
Conditt MA, Ismaily SK, Alexander JW, Noble PC. Backside wear of modular ultra-high molecular weight polyethylene tibial inserts. J Bone Joint Surg Am. 2004;86:1031–1037.
Conditt MA, Thompson MT, Usrey MM, Ismaily SK, Noble PC. Backside wear of polyethylene tibial inserts: mechanism and magnitude of material loss. J Bone Joint Surg Am. 2005;87:326–331.
Cuckler JM, Lemons J, Tamarapalli JR, Beck P. Polyethylene damage on the nonarticular surface of modular total knee prostheses. Clin Orthop Relat Res. 2003;410:248–253.
Dolan MM, Kelly NH, Nguyen JT, Wright TM, Haas SB. Implant design influences tibial post wear damage in posterior-stabilized knees. Clin Orthop Relat Res. 2011;469:160–167.
Furman BD, Lipman J, Kligman M, Wright TM, Haas SB. Tibial post wear in posterior-stabilized knee replacements is design-dependent. Clin Orthop Relat Res. 2008;466:2650–2655.
Galvin A, Jennings LM, McEwen HM, Fisher J. The influence of tibial tray design on the wear of fixed-bearing total knee replacements. Proc Inst Mech Eng H. 2008;222:1289–1293.
Gupta SK, Chu A, Ranawat AS, Slamin J, Ranawat CS. Osteolysis after total knee arthroplasty. J Arthroplasty. 2007;22:787–799.
Harman MK, Banks SA, Hodge WA. Backside damage corresponding to articular damage in retrieved tibial polyethylene inserts. Clin Orthop Relat Res. 2007;458:137–144.
Hood RW, Wright TM, Burstein AH. Retrieval analysis of total knee prostheses: a method and its application to 48 total condylar prostheses. J Biomed Mater Res. 1983;17:829–842.
Jayabalan P, Furman BD, Cottrell JM, Wright TM. Backside wear in modern total knee designs. HSS J. 2007;3:30–34.
Li S, Scuderi G, Furman BD, Bhattacharyya S, Schmieg JJ, Insall JN. Assessment of backside wear from the analysis of 55 retrieved tibial inserts. Clin Orthop Relat Res. 2002;404:75–82.
Lombardi AV Jr, Ellison BS, Berend KR. Polyethylene wear is influenced by manufacturing technique in modular TKA. Clin Orthop Relat Res. 2008;466:2798–2805.
McKellop H, Shen FW, Lu B, Campbell P, Salovey R. Effect of sterilization method and other modifications on the wear resistance of acetabular cups made of ultra-high molecular weight polyethylene: a hip-simulator study. J Bone Joint Surg Am. 2000;82:1708–1725.
Parks NL, Engh GA, Topoleski LD, Emperado J. The Coventry Award: Modular tibial insert micromotion. A concern with contemporary knee implants. Clin Orthop Relat Res. 1998;356:10–15.
Rao AR, Engh GA, Collier MB, Lounici S. Tibial interface wear in retrieved total knee components and correlations with modular insert motion. J Bone Joint Surg Am. 2002;84:1849–1855.
Small SR, Berend ME, Ritter MA, Buckley CA. A comparison in proximal tibial strain between metal-backed and all-polyethylene anatomic graduated component total knee arthroplasty tibial components. J Arthroplasty. 2010;25:820–825.
Taki N, Goldberg VM, Kraay MJ, Rimnac CM. Backside wear of Miller-Galante I and Insall-Burstein II tibial inserts. Clin Orthop Relat Res. 2004;428:198–206.
Wasielewski RC. The causes of insert backside wear in total knee arthroplasty. Clin Orthop Relat Res. 2002;404:232–246.
Wasielewski RC, Parks N, Williams I, Surprenant H, Collier JP, Engh G. Tibial insert undersurface as a contributing source of polyethylene wear debris. Clin Orthop Relat Res. 1997;345:53–59.
Author information
Authors and Affiliations
Corresponding author
Additional information
One author certifies that he (SBH), or a member of his immediate family, has or may receive payments or benefits, during the study period, an amount in excess of USD 1,000,000 from Smith & Nephew, Inc (Memphis, TN, USA).
All ICMJE Conflict of Interest Forms for authors and Clinical Orthopaedics and Related Research editors and board members are on file with the publication and can be viewed on request.
Clinical Orthopaedics and Related Research neither advocates nor endorses the use of any treatment, drug, or device. Readers are encouraged to always seek additional information, including FDA-approval status, of any drug or device prior to clinical use.
Each author certifies that his or her institution approved the human protocol for this investigation and that all investigations were conducted in conformity with ethical principles of research.
This work was performed at the Hospital for Special Surgery, New York, NY, USA.
About this article
Cite this article
Abdel, M.P., Gesell, M.W., Hoedt, C.W. et al. Polished Trays Reduce Backside Wear Independent of Post Location in Posterior-stabilized TKAs. Clin Orthop Relat Res 472, 2477–2482 (2014). https://doi.org/10.1007/s11999-014-3621-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11999-014-3621-y