Abstract
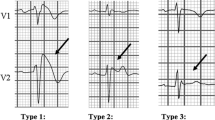
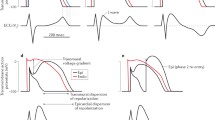
The Brugada syndrome (BS) is a hereditary disease characterized by typical electrocardiographic alterations (elevation of the ST segment in right precordial leads) that affects young individuals without structural heart disease, predisposing them to ventricular arrhythmias and sudden death (SD). Several genetic mutations of different subunits of the sodium, calcium and potassium channel have been involved. The majority of patients with BS remain asymptomatic; however, the most frequent symptoms are syncope and/or SD secondary to polymorphic ventricular tachycardia (PVT) or ventricular fibrillation (VF). Electrocardiographic manifestations of the BS are typically dynamic and occasionally only become apparent after the administration of a sodium channel blocker or with fever. Risk stratification is mainly based on symptoms and the surface electrocardiogram. However, in asymptomatic patients, risk evaluation is still controversial and requires further studies. This review provides an updated summary of the BS from the point of view of genetic, clinical manifestations, risk stratification and management.



Similar content being viewed by others
Abbreviations
- BS:
-
Brugada syndrome
- ECG:
-
Electrocardiogram
- EPS:
-
Electrophysiological study
- ICD:
-
Implantable cardioverter defibrillator
- PVT:
-
Polymorphic ventricular tachycardia
- SD:
-
Sudden death
- VF:
-
Ventricular fibrillation
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Brugada P, Brugada J. Right bundle branch block, persistent st segment elevation and sudden cardiac death: A distinct clinical and electrocardiographic syndrome: a multicenter report. J Am Coll Cardiol. 1992;20:1391–6.
Antzelevitch C, Brugada P, Borggrefe M, Brugada J, Brugada R, Corrado D, et al. Brugada syndrome: report of the second consensus conference: endorsed by the heart rhythm society and the european heart rhythm association. Circulation. 2005;111:659–70.
Schulze-Bahr E, Eckardt L, Breithardt G, Seidl K, Wichter T, Wolpert C, et al. Sodium channel gene (scn5a) mutations in 44 index patients with brugada syndrome: different incidences in familial and sporadic disease. Hum Mutat. 2003;21:651–2.
Chen Q, Kirsch GE, Zhang D, Brugada R, Brugada J, Brugada P, et al. Genetic basis and molecular mechanism for idiopathic ventricular fibrillation. Nature. 1998;392:293–6.
Priori SG, Napolitano C, Giordano U, Collisani G, Memmi M. Brugada syndrome and sudden cardiac death in children. Lancet. 2000;355:808–9.
Rook MB, Bezzina Alshinawi C, Groenewegen WA, van Gelder IC, van Ginneken ACG, Jongsma HJ, et al. Human scn5a gene mutations alter cardiac sodium channel kinetics and are associated with the brugada syndrome. Cardiovasc Res. 1999;44:507–17.
Cordeiro JM, Barajas-Martinez H, Hong K, Burashnikov E, Pfeiffer R, Orsino A-M, et al. Compound heterozygous mutations p336l and i1660v in the human cardiac sodium channel associated with the brugada syndrome. Circulation. 2006;114:2026–33.
Pfahnl AE, Viswanathan PC, Weiss R, Shang LL, Sanyal S, Shusterman V, et al. A sodium channel pore mutation causing brugada syndrome. Heart Rhythm. 2007;4:46–53.
Weiss R, Barmada MM, Nguyen T, Seibel JS, Cavlovich D, Kornblit CA, et al. Clinical and molecular heterogeneity in the brugada syndrome: a novel gene locus on chromosome 3. Circulation. 2002;105:707–13.
London B, Michalec M, Mehdi H, Zhu X, Kerchner L, Sanyal S, et al. Mutation in glycerol-3-phosphate dehydrogenase 1–like gene (gpd1-l) decreases cardiac na + current and causes inherited arrhythmias. Circulation. 2007;116:2260–8.
Antzelevitch C, Pollevick GD, Cordeiro JM, Casis O, Sanguinetti MC, Aizawa Y, et al. Loss-of-function mutations in the cardiac calcium channel underlie a new clinical entity characterized by st-segment elevation, short qt intervals, and sudden cardiac death. Circulation. 2007;115:442–9.
Delpón E, Cordeiro JM, Núñez L, Thomsen PEB, Guerchicoff A, Pollevick GD, et al. Functional effects of kcne3 mutation and its role in the development of brugada syndrome. Circ Arrhythmia Electrophysiol. 2008;1:209–18.
Schulze-Bahr E, Semsarian C, Towbin JA, Watkins H, Wilde A, Wolpert C, et al. Hrs/ehra expert consensus statement on the state of genetic testing for the channelopathies and cardiomyopathies: this document was developed as a partnership between the heart rhythm society (hrs) and the european heart rhythm association (ehra). Europace. 2011;13:1077–109. This article summarizes the state of the art of genetic testing for the channelopathies and cardiomyopathies and the opinion of the international writing group members with respect to the use and role of genetic testing for these hereditary diseases.
Brugada J, Brugada R, Brugada P. Right bundle-branch block and st-segment elevation in leads v1 through v3: a marker for sudden death in patients without demonstrable structural heart disease. Circulation. 1998;97:457–60.
Brugada P, Brugada R, Brugada J. Sudden death in patients and relatives with the syndrome of right bundle branch block, st segment elevation in the precordial leads v(1)to v(3)and sudden death. Eur Heart J. 2000;21:321–6.
Donohue D, Tehrani F, Jamehdor R, Lam C, Movahed MR. The prevalence of brugada ecg in adult patients in a large university hospital in the western united states. Am Heart Hosp J. 2008;6:48–50.
Sinner MF, Pfeufer A, Perz S, Schulze-Bahr E, Mönnig G, Eckardt L, et al. Spontaneous brugada electrocardiogram patterns are rare in the german general population: results from the kora study. Europace. 2009;11:1338–44.
Miyasaka Y, Tsuji H, Yamada K, Tokunaga S, Saito D, Imuro Y, et al. Prevalence and mortality of the brugada-type electrocardiogram in one city in japan. J Am Coll Cardiol. 2001;38:771–4.
Matsuo K, Akahoshi M, Nakashima E, Suyama A, Seto S, Hayano M, et al. The prevalence, incidence and prognostic value of the brugada-type electrocardiogram: a population-based study of four decades. J Am Coll Cardiol. 2001;38:765–70.
Bezzina CR, Shimizu W, Yang P, Koopmann TT, Tanck MWT, Miyamoto Y, et al. Common sodium channel promoter haplotype in asian subjects underlies variability in cardiac conduction. Circulation. 2006;113:338–44.
Nademanee K. Sudden unexplained death syndrome in southeast asia. Am J Cardiol. 1997;79:10–1.
Catalano O, Antonaci S, Moro G, Mussida M, Frascaroli M, Baldi M, et al. Magnetic resonance investigations in brugada syndrome reveal unexpectedly high rate of structural abnormalities. Eur Heart J. 2009;30:2241–8.
van Hoorn F, Campian ME, Spijkerboer A, Blom MT, Planken RN, van Rossum AC, et al. Scn5a mutations in brugada syndrome are associated with increased cardiac dimensions and reduced contractility. PLoS One. 2012;7:e42037.
Kamakura S, Ohe T, Nakazawa K, Aizawa Y, Shimizu A, Horie M, et al. Japan ftBSIi. Long-term prognosis of probands with brugada-pattern st-elevation in leads v1–v3. Circ Arrhythmia Electrophysiol. 2009;2:495–503.
Probst V, Veltmann C, Eckardt L, Meregalli PG, Gaita F, Tan HL, et al. Long-term prognosis of patients diagnosed with brugada syndrome: results from the finger brugada syndrome registry. Circulation. 2010;121:635–43. The FINGER study evaluates the prognosis and risk factors of sudden death in Brugada syndrome in a international multicentric prospective registry of 1029 consecutive individuals.
Brugada J, Brugada R, Antzelevitch C, Towbin J, Nademanee K, Brugada P. Long-term follow-up of individuals with the electrocardiographic pattern of right bundle-branch block and st-segment elevation in precordial leads v1 to v3. Circulation. 2002;105:73–8.
Priori SG, Napolitano C, Gasparini M, Pappone C, Bella PD, Giordano U, et al. Natural history of brugada syndrome: insights for risk stratification and management. Circulation. 2002;105:1342–7.
Brugada J, Brugada R, Brugada P. Determinants of sudden cardiac death in individuals with the electrocardiographic pattern of brugada syndrome and no previous cardiac arrest. Circulation. 2003;108:3092–6.
Eckardt L, Probst V, Smits JPP, Bahr ES, Wolpert C, Schimpf R, et al. Long-term prognosis of individuals with right precordial st-segment–elevation brugada syndrome. Circulation. 2005;111:257–63.
Kusano KF, Taniyama M, Nakamura K, Miura D, Banba K, Nagase S, et al. Atrial fibrillation in patients with brugada syndrome: relationships of gene mutation, electrophysiology, and clinical backgrounds. J Am Coll Cardiol. 2008;51:1169–75.
Schimpf R, Giustetto C, Eckardt L, Veltmann C, Wolpert C, Gaita F, et al. Prevalence of supraventricular tachyarrhythmias in a cohort of 115 patients with brugada syndrome. Ann Noninvasive Electrocardiol. 2008;13:266–9.
Eckardt L, Kirchhof P, Johna R, Haverkamp W, Breithardt G, Borggrefe M. Wolff-parkinson-white syndrome associated with brugada syndrome. Pacing Clin Electrophysiol. 2001;24:1423–4.
Morita H, Fukushima-Kusano K, Nagase S, Miyaji K, Hiramatsu S, Banba K, et al. Sinus node function in patients with brugada-type ecg. Circ J. 2004;68:473–6.
Letsas KP, Korantzopoulos P, Efremidis M, Weber R, Lioni L, Bakosis G, et al. Sinus node disease in subjects with type 1 ecg pattern of brugada syndrome. J Cardiol. 2013;61:227–31.
Benito B, Brugada J. Recurrent syncope: an unusual presentation of brugada syndrome. Nat Clin Pract Cardiovasc Med. 2006;3:573–7. quiz following 577.
Makita N, Sumitomo N, Watanabe I, Tsutsui H. Novel scn5a mutation (q55x) associated with age-dependent expression of brugada syndrome presenting as neurally mediated syncope. Heart Rhythm. 2007;4:516–9.
Matsuo K, Kurita T, Inagaki M, Kakishita M, Aihara N, Shimizu W, et al. The circadian pattern of the development of ventricular fibrillation in patients with brugada syndrome. Eur Heart J. 1999;20:465–70.
Mizumaki K, Fujiki A, Tsuneda T, Sakabe M, Nishida K, Sugao M, et al. Vagal activity modulates spontaneous augmentation of st elevation in the daily life of patients with brugada syndrome. J Cardiovasc Electrophysiol. 2004;15:667–73.
Takigawa M, Noda T, Shimizu W, Miyamoto K, Okamura H, Satomi K, et al. Seasonal and circadian distributions of ventricular fibrillation in patients with brugada syndrome. Heart Rhythm. 2008;5:1523–7.
Chockalingam P, Rammeloo LA, Postema PG, Hruda J, Clur S-AB, Blom NA, et al. Fever-induced life-threatening arrhythmias in children harboring an scn5a mutation. Pediatrics. 2011;127:e239–44.
Litovsky SH, Antzelevitch C. Differences in the electrophysiological response of canine ventricular subendocardium and subepicardium to acetylcholine and isoproterenol. A direct effect of acetylcholine in ventricular myocardium. Circ Res. 1990;67:615–27.
Wichter T, Matheja P, Eckardt L, Kies P, Schäfers K, Schulze-Bahr E, et al. Cardiac autonomic dysfunction in brugada syndrome. Circulation. 2002;105:702–6.
Kies P, Wichter T, Schäfers M, Paul M, Schäfers KP, Eckardt L, et al. Abnormal myocardial presynaptic norepinephrine recycling in patients with brugada syndrome. Circulation. 2004;110:3017–22.
Di Diego JM, Cordeiro JM, Goodrow RJ, Fish JM, Zygmunt AC, Pérez GJ, et al. Ionic and cellular basis for the predominance of the brugada syndrome phenotype in males. Circulation. 2002;106:2004–11.
Matsuo K, Akahoshi M, Seto S, Yano K. Disappearance of the brugada-type electrocardiogram after surgical castration. Pacing Clin Electrophysiol. 2003;26:1551–3.
Shimizu W, Matsuo K, Kokubo Y, Satomi K, Kurita T, Noda T, et al. Sex hormone and gender difference—role of testosterone on male predominance in brugada syndrome. J Cardiovasc Electrophysiol. 2007;18:415–21.
Benito B, Sarkozy A, Mont L, Henkens S, Berruezo A, Tamborero D, et al. Gender differences in clinical manifestations of brugada syndrome. J Am Coll Cardiol. 2008;52:1567–73.
Probst V, Denjoy I, Meregalli PG, Amirault J-C, Sacher F, Mansourati J, et al. Clinical aspects and prognosis of brugada syndrome in children. Circulation. 2007;115:2042–8.
Wilde AAM, Antzelevitch C, Borggrefe M, Brugada J, Brugada R, Brugada P, et al. Proposed diagnostic criteria for the brugada syndrome: Consensus report. Circulation. 2002;106:2514–9.
Bayés de Luna A, Brugada J, Baranchuk A, Borggrefe M, Breithardt G, Goldwasser D, et al. Current electrocardiographic criteria for diagnosis of brugada pattern: A consensus report. J Electrocardiol. 2012;45:433–42. This new consensus report establishes a set of new ECG criteria for the diagnosis of Brugada syndrome and describes the key points of differential diagnosis with different conditions that lead to Brugada-like pattern in the right precordial leads.
Sangwatanaroj S, Prechawat S, Sunsaneewitayakul B, Sitthisook S, Tosukhowong P, Tungsanga K. New electrocardiographic leads and the procainamide test for the detection of the brugada sign in sudden unexplained death syndrome survivors and their relatives. Eur Heart J. 2001;22:2290–6.
Miyamoto K, Yokokawa M, Tanaka K, Nagai T, Okamura H, Noda T, et al. Diagnostic and prognostic value of a type 1 brugada electrocardiogram at higher (third or second) v1 to v2 recording in men with brugada syndrome. Am J Cardiol. 2007;99:53–7.
Miyazaki T, Mitamura H, Miyoshi S, Soejima K, Aizawa Y, Ogawa S. Autonomic and antiarrhythmic drug modulation of st segment elevation in patients with brugada syndrome. J Am Coll Cardiol. 1996;27:1061–70.
Antzelevitch C, Brugada R. Fever and brugada syndrome. Pacing Clin Electrophysiol. 2002;25:1537–9.
Pitzalis MV, Anaclerio M, Iacoviello M, Forleo C, Guida P, Troccoli R, et al. Qt-interval prolongation inright precordial leads: an additional electrocardiographic hallmark of brugada syndrome. J Am Coll Cardiol. 2003;42:1632–7.
Smits JPP, Eckardt L, Probst V, Bezzina CR, Schott JJ, Remme CA, et al. Genotype-phenotype relationship in brugada syndrome: electrocardiographic features differentiate scn5a-related patients from non–scn5a-related patients. J Am Coll Cardiol. 2002;40:350–6.
Maury P, Rollin A, Sacher F, Gourraud J-B, Raczka F, Pasquié J-L, et al. Prevalence and prognostic role of various conduction disturbances in patients with the brugada syndrome. Am J Cardiol. 2013;112:1384–9.
Hong K, Brugada J, Oliva A, Berruezo-Sanchez A, Potenza D, Pollevick GD, et al. Value of electrocardiographic parameters and ajmaline test in the diagnosis of brugada syndrome caused by scn5a mutations. Circulation. 2004;110:3023–7.
Meregalli PG, Ruijter JM, Hofman N, Bezzina CR, Wilde AAM, Tan HL. Diagnostic value of flecainide testing in unmasking scn5a-related brugada syndrome. J Cardiovasc Electrophysiol. 2006;17:857–64.
Priori SG, Wilde AA, Horie M, Cho Y, Behr ER, Berul C, et al. Executive summary: hrs/ehra/aphrs expert consensus statement on the diagnosis and management of patients with inherited primary arrhythmia syndromes. Europace. 2013;15:1389–406. This consensus document provides clinical guidance for diagnosis, risk stratification and management of patients affected by inherited primary arrhythmia syndromes.
Dumaine R, Towbin JA, Brugada P, Vatta M, Nesterenko DV, Nesterenko VV, et al. Ionic mechanisms responsible for the electrocardiographic phenotype of the brugada syndrome are temperature dependent. Circ Res. 1999;85:803–9.
Porres JM, Brugada J, Urbistondo V, Garcia F, Reviejo K, Marco P. Fever unmasking the brugada syndrome. Pacing Clin Electrophysiol. 2002;25:1646–8.
Ortega-Carnicer J, Benezet J, Ceres F. Fever-induced st-segment elevation and t-wave alternans in a patient with brugada syndrome. Resuscitation. 2003;57:315–7.
Kok L-C, Mitchell MA, Haines DE, Mounsey JP, DiMarco JP. Transient st elevation after transthoracic cardioversion in patients with hemodynamically unstable ventricular tachyarrhythmia. Am J Cardiol. 2000;85:878–81.
Gurevitz O, Lipchenca I, Yaacoby E, Segal E, Perel A, Eldar M, et al. St-segment deviation following implantable cardioverter defibrillator shocks: Incidence, timing, and clinical significance. Pacing Clin Electrophysiol. 2002;25:1429–32.
Brugada P, Brugada R, Brugada J. Patients with an asymptomatic brugada electrocardiogram should undergo pharmacological and electrophysiological testing. Circulation. 2005;112:279–92.
Priori SG, Gasparini M, Napolitano C, Della Bella P, Ottonelli AG, Sassone B, et al. Risk stratification in brugada syndrome: Results of the prelude (programmed electrical stimulation predictive value) registry. J Am Coll Cardiol. 2012;59:37–45. The PRELUDE study is a multicentric prospective registry of 308 consecutive patients desgined to evaluate the predictive accuracy of ventricular arrhythmia inducibility and to identify additional predictors of arrhythmic events in Brugada syndrome.
Giustetto C, Drago S, Demarchi PG, Dalmasso P, Bianchi F, Masi AS, et al. Risk stratification of the patients with brugada type electrocardiogram: a community-based prospective study. Europace. 2009;11:507–13.
Sarkozy A, Sorgente A, Boussy T, Casado R, Paparella G, Capulzini L, et al. The value of a family history of sudden death in patients with diagnostic type i brugada ecg pattern. Eur Heart J. 2011;32:2153–60. This single-centre prospective registry analyzed the value of a family history of sudden death in Brugada syndrome failing to show a relationship with arrhythmic events during follow-up.
Viswanathan PC, Benson DW, Balser JR. A common scn5a polymorphism modulates the biophysical effects of an scn5a mutation. J Clin Investig. 2003;111:341–6.
Poelzing S, Forleo C, Samodell M, Dudash L, Sorrentino S, Anaclerio M, et al. Scn5a polymorphism restores trafficking of a brugada syndrome mutation on a separate gene. Circulation. 2006;114:368–76.
Meregalli PG, Tan HL, Probst V, Koopmann TT, Tanck MW, Bhuiyan ZA, et al. Type of scn5a mutation determines clinical severity and degree of conduction slowing in loss-of-function sodium channelopathies. Heart Rhythm. 2009;6:341–8.
Sommariva E, Pappone C, Martinelli Boneschi F, Di Resta C, Rosaria Carbone M, Salvi E, Vergara P, Sala S, Cusi D, Ferrari M, Benedetti S. Genetics can contribute to the prognosis of brugada syndrome: A pilot model for risk stratification. Eur J Hum Genet. 2013
Brugada J, Brugada R, Brugada P. Electrophysiologic testing predicts events in brugada syndrome patients. Heart Rhythm. 2011;8:1595–7. References 74 and 75 represent a controversy between experts about the role of the electrophysiological study as a risk marker in patients diagnosed of Brugada syndrome.
Wilde AAM, Viskin S. Ep testing does not predict cardiac events in brugada syndrome. Heart Rhythm. 2011;8:1598–600. References 74 and 75 represent a controversy between experts about the role of the electrophysiological study as a risk marker in patients diagnosed of Brugada syndrome.
Paul M, Gerss J, Schulze-Bahr E, Wichter T, Vahlhaus C, Wilde AAM, et al. Role of programmed ventricular stimulation in patients with brugada syndrome: A meta-analysis of worldwide published data. Eur Heart J. 2007;28:2126–33.
Fauchier L, Isorni MA, Clementy N, Pierre B, Simeon E, Babuty D. Prognostic value of programmed ventricular stimulation in brugada syndrome according to clinical presentation: an updated meta-analysis of worldwide published data. Int J Cardiol. 2013. doi:10.1016/j.ijcard.2013.04.146.
Morita H, Kusano KF, Miura D, Nagase S, Nakamura K, Morita ST, et al. Fragmented qrs as a marker of conduction abnormality and a predictor of prognosis of brugada syndrome. Circulation. 2008;118:1697–704.
Makimoto H, Kamakura S, Aihara N, Noda T, Nakajima I, Yokoyama T, et al. Clinical impact of the number of extrastimuli in programmed electrical stimulation in patients with brugada type 1 electrocardiogram. Heart Rhythm. 2012;9:242–8.
Makimoto H, Nakagawa E, Takaki H, Yamada Y, Okamura H, Noda T, et al. Augmented st-segment elevation during recovery from exercise predicts cardiac events in patients with brugada syndrome. J Am Coll Cardiol. 2010;56:1576–84.
Morita H, Kusano-Fukushima K, Nagase S, Fujimoto Y, Hisamatsu K, Fujio H, et al. Atrial fibrillation and atrial vulnerability in patients with brugada syndrome. J Am Coll Cardiol. 2002;40:1437–44.
Kawata H, Morita H, Yamada Y, Noda T, Satomi K, Aiba T, et al. Prognostic significance of early repolarization in inferolateral leads in brugada patients with documented ventricular fibrillation: a novel risk factor for brugada syndrome with ventricular fibrillation. Heart Rhythm. 2013;10:1161–8.
Takagi M, Aonuma K, Sekiguchi Y, Yokoyama Y, Aihara N, Hiraoka M. The prognostic value of early repolarization (j wave) and st-segment morphology after j wave in brugada syndrome: multicenter study in japan. Heart Rhythm. 2013;10:533–9.
Rollin A, Sacher F, Gourraud JB, Pasquié JL, Raczka F, Duparc A, et al. Prevalence, characteristics, and prognosis role of type 1 st elevation in the peripheral ecg leads in patients with brugada syndrome. Heart Rhythm. 2013;10:1012–8.
Castro Hevia J, Antzelevitch C, Tornés Bárzaga F, Dorantes Sánchez M, Dorticós Balea F, Zayas Molina R, et al. Tpeak-tend and tpeak-tend dispersion as risk factors for ventricular tachycardia/ventricular fibrillation in patients with the brugada syndrome. J Am Coll Cardiol. 2006;47:1828–34.
Babai Bigi MA, Aslani A, Shahrzad S. Avr sign as a risk factor for life-threatening arrhythmic events in patients with brugada syndrome. Heart Rhythm. 2007;4:1009–12.
Fish JM, Antzelevitch C. Cellular mechanism and arrhythmogenic potential of t-wave alternans in the brugada syndrome. J Cardiovasc Electrophysiol. 2008;19:301–8.
Sarkozy A, Chierchia G-B, Paparella G, Boussy T, De Asmundis C, Roos M, et al. Inferior and lateral electrocardiographic repolarization abnormalities in brugada syndrome. Circ Arrhythmia Electrophysiol. 2009;2:154–61.
Junttila MJ, Brugada P, Hong K, Lizotte E, DEZ M, Sarkozy A, et al. Differences in 12-lead electrocardiogram between symptomatic and asymptomatic brugada syndrome patients. J Cardiovasc Electrophysiol. 2008;19:380–3.
Postema PG, Wolpert C, Amin AS, Probst V, Borggrefe M, Roden DM, et al. Drugs and brugada syndrome patients: review of the literature, recommendations, and an up-to-date website (www.Brugadadrugs.Org). Heart Rhythm. 2009;6:1335–41.
Sacher F, Probst V, Iesaka Y, Jacon P, Laborderie J, Mizon-Gérard F, et al. Outcome after implantation of a cardioverter-defibrillator in patients with brugada syndrome: a multicenter study. Circulation. 2006;114:2317–24.
Sarkozy A, Boussy T, Kourgiannides G, Chierchia G-B, Richter S, De Potter T, et al. Long-term follow-up of primary prophylactic implantable cardioverter-defibrillator therapy in brugada syndrome. Eur Heart J. 2007;28:334–44.
Miyazaki S, Uchiyama T, Komatsu Y, Taniguchi H, Kusa S, Nakamura H, et al. Long-term complications of implantable defibrillator therapy in brugada syndrome. Am J Cardiol. 2013;111:1448–51. This study evaluates the prevalence of device-related complications and the clinical outcome in 41 consecutive patients during a a median follow-up of 76 months showing that adverse effects related to ICD implantation are not uncommon.
Belhassen B, Glick A, Viskin S. Efficacy of quinidine in high-risk patients with brugada syndrome. Circulation. 2004;110:1731–7.
Schweizer P, Becker R, Katus H, Thomas D. Successful acute and long-term management of electrical storm in brugada syndrome using orciprenaline and quinine/quinidine. Clin Res Cardiol. 2010;99:467–70.
Hermida J-S, Denjoy I, Clerc J, Extramiana F, Jarry G, Milliez P, et al. Hydroquinidine therapy in brugada syndrome. J Am Coll Cardiol. 2004;43:1853–60.
Márquez MF, Bonny A, Hernández-Castillo E, De Sisti A, Gómez-Flores J, Nava S, et al. Long-term efficacy of low doses of quinidine on malignant arrhythmias in brugada syndrome with an implantable cardioverter-defibrillator: a case series and literature review. Heart Rhythm. 2012;9:1995–2000. This study shows in 6 patients that low doses of quinidine are well tolerated and effective to prevent the ocurrence of ventricular arrhythmia, in subjects with Brugada syndrome with an implantable cardioverter-defibrillator.
Ohgo T, Okamura H, Noda T, Satomi K, Suyama K, Kurita T, et al. Acute and chronic management in patients with brugada syndrome associated with electrical storm of ventricular fibrillation. Heart Rhythm Off J Heart Rhythm Soc. 2007;4:695–700.
Haissaguerre M, Extramiana F, Hocini M, Cauchemez B, Jais P, Cabrera JA, et al. Mapping and ablation of ventricular fibrillation associated with long-qt and brugada syndromes. Circulation. 2003;108:925–8.
Nademanee K, Veerakul G, Chandanamattha P, Chaothawee L, Ariyachaipanich A, Jirasirirojanakorn K, et al. Prevention of ventricular fibrillation episodes in brugada syndrome by catheter ablation over the anterior right ventricular outflow tract epicardium. Circulation. 2011;123:1270–9. This article describes the findings of endocardial and epicardial mapping in nine patients with Brugada syndrome and the effects of epicardial catheter ablation over pathological areas.
Compliance with Ethics Guidelines
Conflict of Interest
Elena Arbelo and Josep Brugada declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is part of the Topical Collection on Invasive Electrophysiology and Pacing
Rights and permissions
About this article
Cite this article
Arbelo, E., Brugada, J. Risk Stratification and Treatment of Brugada Syndrome. Curr Cardiol Rep 16, 508 (2014). https://doi.org/10.1007/s11886-014-0508-1
Published:
DOI: https://doi.org/10.1007/s11886-014-0508-1