Abstract
Purpose of Review
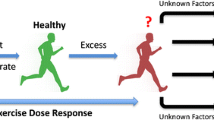
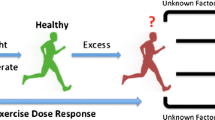
This review summarizes several issues at the forefront of recent controversies involving the appropriate exercise dose including epidemiologic data describing mortality trends in those who engage in high levels of physical activity and recent observational data suggesting adverse cardiovascular outcomes among long-term endurance athletes.
Recent Findings
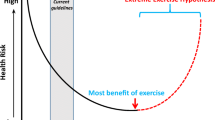
The benefits of habitual and moderate levels of exercise on cardiovascular disease outcomes in the general population have been well established. However, recent data have questioned whether higher doses of physical and athletic activity are associated with adverse cardiovascular outcomes.
Summary
Specifically in regard to adverse cardiovascular outcomes, the evidence and limitations of the available data associating veteran endurance athletes with an increased risk of atrial fibrillation, exercise-induced arrhythmogenic cardiac remodeling, and accelerated coronary atherosclerosis will be discussed. This review will also provide a conceptual framework in the context of the clinical management of athletic patients and will highlight key areas of future research that may resolve many of these controversial issues.

Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Wen CP, Wai JP, Tsai MK, Yang YC, Cheng TY, Lee MC, et al. Minimum amount of physical activity for reduced mortality and extended life expectancy: a prospective cohort study. Lancet. 2011;378:1244–53.
Paffenbarger Jr RS, Hyde RT, Wing AL, Lee IM, Jung DL, Kampert JB. The association of changes in physical-activity level and other lifestyle characteristics with mortality among men. N Engl J Med. 1993;328:538–45.
Sofi F, Capalbo A, Cesari F, Abbate R, Gensini GF. Physical activity during leisure time and primary prevention of coronary heart disease: an updated meta-analysis of cohort studies. Eur J Cardiovasc Prev Rehabil. 2008;15:247–57.
Sattelmair J, Pertman J, Ding EL, Kohl 3rd HW, Haskell W, Lee IM. Dose response between physical activity and risk of coronary heart disease: a meta-analysis. Circulation. 2011;124:789–95.
Andersen K, Farahmand B, Ahlbom A, Held C, Ljunghall S, Michaelsson K, et al. Risk of arrhythmias in 52 755 long-distance cross-country skiers: a cohort study. Eur Heart J. 2013;34:3624–31. This study is the largest cohort study of high-level endurance athletes demonstrating an association between endurance exercise and atrial fibrillation. Importantly, those athletes who competed in the most number of cross-country skiing events and who were the fastest were most at risk.
La Gerche A, Burns AT, Mooney DJ, Inder WJ, Taylor AJ, Bogaert J, et al. Exercise-induced right ventricular dysfunction and structural remodelling in endurance athletes. Eur Heart J. 2012;33:998–1006. In this study of 40 elite endurance athletes, an association was observed between reduced right ventricular systolic function and increased cardiac biomarkers immediately after completion of an ultra-endurance exercise event. In addition, in a small number of athletes studied at baseline, fibrosis was noted in the right ventricle by cardiac MRI of unclear significance.
Mohlenkamp S, Lehmann N, Breuckmann F, Brocker-Preuss M, Nassenstein K, Halle M, et al. Running: the risk of coronary events : prevalence and prognostic relevance of coronary atherosclerosis in marathon runners. Eur Heart J. 2008;29:1903–10. This study found increased coronary artery calcium scores in veteran marathon runners compared to relatively matched non-marathon running controls. In addition, four marathon runners had coronary events within 2 years of follow-up.
Schnohr P, O’Keefe JH, Marott JL, Lange P, Jensen GB. Dose of jogging and long-term mortality: the Copenhagen City Heart Study. J Am Coll Cardiol. 2015;65:411–9. In this epidemiologic study of 1100 joggers, a U-shaped association was found between dose of jogging and all-cause mortality. However, for the strenuous joggers, subject numbers were extremely limited.
Arem H, Moore SC, Patel A, Hartge P, de Gonzalez BA, Visvanathan K, et al. Leisure time physical activity and mortality: a detailed pooled analysis of the dose-response relationship. JAMA Intern Med. 2015;175:959–67.
O’Keefe JH, Lavie CJ. Run for your life … at a comfortable speed and not too far. Heart. 2013;99:516–9.
Levine BD. Can intensive exercise harm the heart? The benefits of competitive endurance training for cardiovascular structure and function. Circulation. 2014;130:987–91.
Reynolds G. Can too much exercise harm the heart? New York Times. December 30, 2015. (http://well.blogs.nytimes.com/2015/12/30/can-too-much-exercise-harm-the-heart/?_r = 0).
Rosenbaum L. Extreme exercise and the heart. The New Yorker. July 15, 2014. (http://www.newyorker.com/tech/elements/extreme-exercise-and-the-heart).
Wasfy MM, Baggish AL. Exercise dose in clinical practice. Circulation. 2016;133:2297–313.
Lee DC, Pate RR, Lavie CJ, Sui X, Church TS, Blair SN. Leisure-time running reduces all-cause and cardiovascular mortality risk. J Am Coll Cardiol. 2014;64:472–81. In this epidemiologic analysis, the authors found that low-dose running significantly reduced all-cause and cardiovascular mortality. In addition, metrics of running dose were startified into quintiles and there were minimal differences in mortaliy benefit across quintiles.
Armstrong ME, Green J, Reeves GK, Beral V, Cairns BJ. Million women study C. Response to letter regarding article, “Frequent physical activity may not reduce vascular disease risk as much as moderate activity: large prospective study of women in the United Kingdom”. Circulation. 2015;132:e225.
Sarna S, Sahi T, Koskenvuo M, Kaprio J. Increased life expectancy of world class male athletes. Med Sci Sports Exerc. 1993;25:237–44.
Chakravarty EF, Hubert HB, Lingala VB, Fries JF. Reduced disability and mortality among aging runners: a 21-year longitudinal study. Arch Intern Med. 2008;168:1638–46.
Farahmand BY, Ahlbom A, Ekblom O, Ekblom B, Hallmarker U, Aronson D, et al. Mortality amongst participants in Vasaloppet: a classical long-distance ski race in Sweden. J Intern Med. 2003;253:276–83.
Clarke PM, Walter SJ, Hayen A, Mallon WJ, Heijmans J, Studdert DM. Survival of the fittest: retrospective cohort study of the longevity of Olympic medallists in the modern era. BMJ. 2012;345, e8308.
Marijon E, Tafflet M, Antero-Jacquemin J, El Helou N, Berthelot G, Celermajer DS, et al. Mortality of French participants in the Tour de France (1947-2012). Eur Heart J. 2013;34:3145–50.
Iwasaki YK, Nishida K, Kato T, Nattel S. Atrial fibrillation pathophysiology: implications for management. Circulation. 2011;124:2264–74.
Colilla S, Crow A, Petkun W, Singer DE, Simon T, Liu X. Estimates of current and future incidence and prevalence of atrial fibrillation in the U.S. adult population. Am J Cardiol. 2013;112:1142–7.
Karjalainen J, Kujala UM, Kaprio J, Sarna S, Viitasalo M. Lone atrial fibrillation in vigorously exercising middle aged men: case-control study. BMJ. 1998;316:1784–5.
Molina L, Mont L, Marrugat J, Berruezo A, Brugada J, Bruguera J, et al. Long-term endurance sport practice increases the incidence of lone atrial fibrillation in men: a follow-up study. Europace. 2008;10:618–23.
Elosua R, Arquer A, Mont L, Sambola A, Molina L, Garcia-Moran E, et al. Sport practice and the risk of lone atrial fibrillation: a case-control study. Int J Cardiol. 2006;108:332–7.
Heidbuchel H, Anne W, Willems R, Adriaenssens B, Van de Werf F, Ector H. Endurance sports is a risk factor for atrial fibrillation after ablation for atrial flutter. Int J Cardiol. 2006;107:67–72.
Abdulla J, Nielsen JR. Is the risk of atrial fibrillation higher in athletes than in the general population? A systematic review and meta-analysis. Europace. 2009;11:1156–9.
Wilhelm M, Roten L, Tanner H, Wilhelm I, Schmid JP, Saner H. Atrial remodeling, autonomic tone, and lifetime training hours in nonelite athletes. Am J Cardiol. 2011;108:580–5.
Mozaffarian D, Furberg CD, Psaty BM, Siscovick D. Physical activity and incidence of atrial fibrillation in older adults: the cardiovascular health study. Circulation. 2008;118:800–7.
Marcus FI, McKenna WJ, Sherrill D, Basso C, Bauce B, Bluemke DA, et al. Diagnosis of arrhythmogenic right ventricular cardiomyopathy/dysplasia: proposed modification of the task force criteria. Circulation. 2010;121:1533–41.
James CA, Bhonsale A, Tichnell C, Murray B, Russell SD, Tandri H, et al. Exercise increases age-related penetrance and arrhythmic risk in arrhythmogenic right ventricular dysplasia/cardiomyopathy-associated desmosomal mutation carriers. J Am Coll Cardiol. 2013;62:1290–7.
Sharma S, Zaidi A. Exercise-induced arrhythmogenic right ventricular cardiomyopathy: fact or fallacy? Eur Heart J. 2012;33:938–40.
Benito B, Gay-Jordi G, Serrano-Mollar A, Guasch E, Shi Y, Tardif JC, et al. Cardiac arrhythmogenic remodeling in a rat model of long-term intensive exercise training. Circulation. 2011;123:13–22.
Ector J, Ganame J, van der Merwe N, Adriaenssens B, Pison L, Willems R, et al. Reduced right ventricular ejection fraction in endurance athletes presenting with ventricular arrhythmias: a quantitative angiographic assessment. Eur Heart J. 2007;28:345–53. In this small observational study of athletes with ventricular arrhythmias (RV origin) compared to those without ventricular arrhythmias, the authors found that the athletes with ventricular arrhythmias had reduced RV systolic function by invasive angiography.
Neilan TG, Januzzi JL, Lee-Lewandrowski E, Ton-Nu TT, Yoerger DM, Jassal DS, et al. Myocardial injury and ventricular dysfunction related to training levels among nonelite participants in the Boston marathon. Circulation. 2006;114:2325–33.
Whyte GP, George K, Sharma S, Lumley S, Gates P, Prasad K, et al. Cardiac fatigue following prolonged endurance exercise of differing distances. Med Sci Sports Exerc. 2000;32:1067–72.
Douglas PS, O’Toole ML, Hiller WD, Hackney K, Reichek N. Cardiac fatigue after prolonged exercise. Circulation. 1987;76:1206–13.
Scharhag J, George K, Shave R, Urhausen A, Kindermann W. Exercise-associated increases in cardiac biomarkers. Med Sci Sports Exerc. 2008;40:1408–15.
Wilson M, O’Hanlon R, Prasad S, Deighan A, Macmillan P, Oxborough D, et al. Diverse patterns of myocardial fibrosis in lifelong, veteran endurance athletes. J Appl Physiol (1985). 2011;110:1622–6.
Bohm P, Schneider G, Linneweber L, Rentzsch A, Kramer N, Abdul-Khaliq H, et al. Right and left ventricular function and mass in male elite master athletes: a controlled contrast-enhanced cardiovascular magnetic resonance study. Circulation. 2016;133:1927–35.
Baggish AL, Yared K, Wang F, Weiner RB, Hutter Jr AM, Picard MH, et al. The impact of endurance exercise training on left ventricular systolic mechanics. Am J Physiol Heart Circ Physiol. 2008;295:H1109–H16.
Gaziano TA, Bitton A, Anand S, Abrahams-Gessel S, Murphy A. Growing epidemic of coronary heart disease in low- and middle-income countries. Curr Probl Cardiol. 2010;35:72–115.
Ross R. The pathogenesis of atherosclerosis: a perspective for the 1990s. Nature. 1993;362:801–9.
Weber C, Noels H. Atherosclerosis: current pathogenesis and therapeutic options. Nat Med. 2011;17:1410–22.
Aikawa E, Nahrendorf M, Figueiredo JL, Swirski FK, Shtatland T, Kohler RH, et al. Osteogenesis associates with inflammation in early-stage atherosclerosis evaluated by molecular imaging in vivo. Circulation. 2007;116:2841–50.
Budoff MJ, Shaw LJ, Liu ST, Weinstein SR, Mosler TP, Tseng PH, et al. Long-term prognosis associated with coronary calcification: observations from a registry of 25,253 patients. J Am Coll Cardiol. 2007;49:1860–70.
Delaney JA, Jensky NE, Criqui MH, Whitt-Glover MC, Lima JA, Allison MA. The association between physical activity and both incident coronary artery calcification and ankle brachial index progression: the multi-ethnic study of atherosclerosis. Atherosclerosis. 2013;230:278–83.
Schwartz RSKS, Schwartz JG, Wickstrom KK, Peichel G, Garberich RF, et al. Increased coronary artery plaque volume among male marathon runners. Mo Med. 2014;111:85–94.
Hagstrom E, Michaelsson K, Melhus H, Hansen T, Ahlstrom H, Johansson L, et al. Plasma-parathyroid hormone is associated with subclinical and clinical atherosclerotic disease in 2 community-based cohorts. Arterioscler Thromb Vasc Biol. 2014;34:1567–73.
Scott JP, Sale C, Greeves JP, Casey A, Dutton J, Fraser WD. The effect of training status on the metabolic response of bone to an acute bout of exhaustive treadmill running. J Clin Endocrinol Metab. 2010;95:3918–25.
Zerath E, Holy X, Douce P, Guezennec CY, Chatard JC. Effect of endurance training on postexercise parathyroid hormone levels in elderly men. Med Sci Sports Exerc. 1997;29:1139–45.
Criqui MH, Denenberg JO, Ix JH, McClelland RL, Wassel CL, Rifkin DE, et al. Calcium density of coronary artery plaque and risk of incident cardiovascular events. JAMA. 2014;311:271–8.
Kim JH, Malhotra R, Chiampas G, d’Hemecourt P, Troyanos C, Cianca J, et al. Cardiac arrest during long-distance running races. N Engl J Med. 2012;366:130–40.
Lamppa R. 2015 state of the sport-U.S. race trends. Running USA, 2015. (http://www.runningusa.org/annual-reports).
Schaaf M, Andre P, Altman M, Maucort-Boulch D, Placide J, Chevalier P, et al. Left atrial remodelling assessed by 2D and 3D echocardiography identifies paroxysmal atrial fibrillation. Eur Heart J Cardiovasc Imaging. 2016.
Baggish AL, Hale A, Weiner RB, Lewis GD, Systrom D, Wang F, et al. Dynamic regulation of circulating microRNA during acute exhaustive exercise and sustained aerobic exercise training. J Physiol. 2011;589:3983–94.
Baggish AL, Park J, Min PK, Isaacs S, Parker BA, Thompson PD, et al. Rapid upregulation and clearance of distinct circulating microRNAs after prolonged aerobic exercise. J Appl Physiol (1985). 2014;116:522–31.
Lewis GD, Farrell L, Wood MJ, Martinovic M, Arany Z, Rowe GC, et al. Metabolic signatures of exercise in human plasma. Sci Transl Med. 2010;2:33ra7.
Kim JHBS, Awad M, Yadalam A, Sher S, Tran V, et al. Training-related metabolic adaptations in American-style football participants. Ann Sports Med Res. 2015;2:1048.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Jonathan H. Kim is supported by the National Institutes of Health (K23 HL128795).
Aaron L. Baggish is supported by the National Institutes of Health (RO1 DA029141, RO1 HL117037, RO1 HL125869). The authors declare no conflicts of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Coronary Heart Disease
Rights and permissions
About this article
Cite this article
Kim, J.H., Baggish, A.L. Strenuous Exercise and Cardiovascular Disease Outcomes. Curr Atheroscler Rep 19, 1 (2017). https://doi.org/10.1007/s11883-017-0636-3
Published:
DOI: https://doi.org/10.1007/s11883-017-0636-3