Abstract
Objective
We sought to compare the outcomes of Carpentier-Edwards PERIMOUNT (CEP), Magna and Magna Ease valves in Japanese elderly patients with severe aortic valve stenosis (AS).
Methods
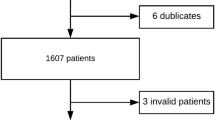
We retrospectively identified 136 patients (mean age 76.61 ± 5.5 years old) who had undergone isolated surgical aortic valve replacement (SAVR) using CEP, Magna, and Magna Ease valves at a single institution, from January 2001 to December 2013. We compared the valves according to their survival rates, freedom from major adverse cardiovascular and cerebrovascular events (MACCE), and durability and hemodynamic performance by echocardiographic data.
Results
The thirty-day mortality after isolated SAVR in all the valve groups was “zero”. The differences among the three groups in terms of survival rates, freedom from MACCE at 2 years, durability and hemodynamic performance of the valves by echocardiographic data was not statistically significant.
Conclusion
All CEP, Magna and Magna Ease valves seemed to be similarly useful in Japanese elderly patients with severe AS. Our data did not clearly support the superiority of one valve over another. A longer follow-up period might be necessary to compare the durability and hemodynamic performance of these valves with more certainty.



Similar content being viewed by others
References
Committee for Scientific Affairs, The Japanese Association for Thoracic Surgery, Masuda M, Kuwano H, Okumura M, Arai H, et al. Thoracic and cardiovascular surgery in Japan during 2013 annual report by The Japanese Association for Thoracic Surgery. Gen Thorac Cardiovasc Surg. 2015;12:670–701.
Minakata K, Tanaka S, Okawa Y, Shimamoto M, Kaneko T, Takahara Y, et al. Long-term outcome of the Carpentier-Edwards pericardial valve in the aortic position in Japanese patients. Circ J. 2014;78:882–9.
Bourguignon T, Bouquiaux-Stablo AL, Candolfi P, Mirza A, Loardi C, May MA, et al. Very long-term outcomes of the Carpentier-Edwards Perimount valve in aortic position. Ann Thorac Surg. 2015;99:831–7.
McClure RS, Narayanasamy N, Wiegerinck E, Lipsitz S, Maloney A, Byrne JG, et al. Late outcomes for aortic valve replacement with the Carpentier-Edwards pericardial bioprosthesis: up to 17-year follow-up in 1000 patients. Ann Thorac Surg. 2010;89:1410–6.
Forcillo J, Pellerin M, Perrault LP, Cartier R, Bouchard D, Demers P, et al. Carpentier-Edwards pericardial valve in the aortic position: 25-years experience. Ann Thorac Surg. 2013;96:486–93.
Ruggieri VG, Flecher E, Anselmi A, Lelong B, Corbineau H, Verhoye JP, et al. Long-term results of the Carpentier-Edwards supraannular aortic valve prosthesis. Ann Thorac Surg. 2012;94:1191–7.
Banbury MK, Cosgrove DM 3rd, Thomas JD, Blackstone EH, Rajeswaran J, Okies JE, et al. Hemodynamic stability during 17 years of the Carpentier-Edwards aortic pericardial bioprosthesis. Ann Thorac Surg. 2002;73:1460–5.
Dalmau MJ, Maríagonzález-Santos J, López-Rodríguez J, Bueno M, Arribas A. The Carpentier-Edwards Perimount Magna aortic xenograft: a new design with an improved hemodynamic performance. Interact CardioVasc Thorac Surg. 2006;5:263–7.
Edmunds LH Jr, Clark RE, Cohn LH, Grunkemeier GL, Miller DC, Weisel RD. Guidelines for reporting morbidity and mortality after cardiac valvular operations. Ad Hoc Liaison Committee for standardizing definitions of prosthetic heart valve morbidity of The American Association for Thoracic Surgery and The Society of Thoracic Surgeons. J Thorac Cardiovasc Surg. 1996;112:708–11.
Murashita T, Greason KL, Suri RM, Nkomo VT, Holmes DR, Rihal CS, Mathew V. Aortic valve replacement for severe aortic valve stenosis in the nonagenarian patient. Ann Thorac Surg. 2014;98:1593–7.
Nishida T, Sonoda H, Oishi Y, Tatewaki H, Tanoue Y, Shiokawa Y, Tominaga R. Long-term results of aortic valve replacement with mechanical prosthesis or Carpentier-Edwards Perimount bioprosthesis in Japanese patients according to age. Circ J. 2014;78:2688–95.
Nishioka N, Morimoto N, Nakagiri K, Matsushima S, Yoshida M, Mukohara N, et al. A case of left main trunk (LMT) obstruction after aortic valve replacement (AVR) using Carpentier-Edwards Perimount Magna. Jpn J Cardiovasc Surg. 2012;41:49–52.
Botzenhardt F, Eichinger WB, Guenzinger R, Bleiziffer S, Wagner I, Bauernschmitt R, et al. Hemodynamic performance and incidence of patient-prosthesis mismatch of the complete supraannular Perimount Magna bioprosthesis in the aortic position. Thorac Cardiov Surg. 2005;53:226–30.
Wagner IM, Eichinger WB, Bleiziffer S, Botzenhardt F, Gebauer I, Guenzinger R, et al. Influence of completely supra-annular placement of bioprostheses on exercise hemodynamics in patients with a small aortic annulas. J Thorac Cardiovasc Surg. 2007;133:1234–41.
Wyss TR, Bigler M, Stalder M, Englberger L, Aymard T, Kadner A, et al. Absence of prosthesis-patient mismatch with the new generation of Edwards stented aortic bioprosthesis. Interact Cardiovasc Thorac Surg. 2010;10:884–8.
Wendt D, Thielmann M, Plicht B, Aβmann J, Price V, Neuhauser M, et al. The new St Jude Trifecta versus Carpentier-Edwards Perimount Magna and Magna ease aortic bioprosthesis: is there a hemodynamic superiority? J Thorac Cardiovasc Surg. 2014;147:1553–60.
Thalji NM, Suri RM, Michelena HI, Greason KL, Dearani JA, et al. Do differences in early hemodynamic performance of current generation biologic aortic valves predict outcomes 1 year following surgery? J Thorac Cardiovasc Surg. 2015;149:163–73.
Jamieson WR, Lewis CT, Sakwa MP, Cooley DA, Kshettry VR, Jones KW, et al. St Jude Medical Epic porcine bioprosthesis: results of the regulatory evaluation. J Thorac Cardiovasc Surg. 2011;141:1449–54.
Ono K, Kuroda H. Pannus formation two years after bioprosthetic aortic valve implantation; report of a case. Kyobu Geka. 2015;68:785–7.
Hirota M, Isomura T, Yoshida M, Katsumata C, Ito F, Watanabe M. Subvalvular Pannus overgrowth after mosaic bioprosthesis implantation in the aortic position. Ann Thorac Cardiovasc Surg. 2016;22:108–11.
Sawa Y. Transcatheter aortic valve implantation. Surg Today. 2015;45:527–36.
Reinöhl J, Kaier K, Reinecke H, Schmoor C, Frankenstein L, Vach W, et al. Effect of availability of transcatheter aortic-valve replacement on clinical practice. N Engl J Med. 2015;373:2438–47.
Alizadeh-Ghavidel A, Azarfarin R, Alizadehasl A, Sadeghpour-Tabaei A, Totonchi Z. Moderate patient-prosthesis mismatch has no negative effect on patients’ functional status after aortic valve replacement with carbomedics prosthesis. Res Cardiovasc Med. 2016;5:e29038.
Saxena P, Greason KL, Schaff HV. Early structural valve deterioration of the Trifecta aortic valve biological prosthesis: a word of caution. J Thorac Cardiovasc Surg. 2014;147:e10–1.
Fouquet O, Flecher E, Nzomvuama A, Remadi JP, Bière L, Donal E, et al. Haemodynamic performance of the small supra-annular Trifecta bioprosthesis: results from a French multicentre study. Interact CardioVasc Thorac Surg. 2016;22:439–44.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All of the authors declare that they had no competing interests related to this study.
Rights and permissions
About this article
Cite this article
Nishioka, N., Yamada, A., Ujihira, K. et al. Outcomes of surgical aortic valve replacement using Carpentier-Edwards PERIMOUNT bioprosthesis series in elderly patients with severe aortic valve stenosis: a retrospective cohort study. Gen Thorac Cardiovasc Surg 64, 728–734 (2016). https://doi.org/10.1007/s11748-016-0698-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11748-016-0698-0