Abstract
Background
Laparoscopic sleeve gastrectomy (LSG) is a favorable bariatric procedure. This study evaluated the status of LSG in China.
Methods
During the 4th International Forum of Bariatric and Metabolic Surgery in May 2016, Nanjing China, an on-the-spot questionnaire was filled out by 105 attending surgeons with experience of LSG. The feedback data was collected and analyzed.
Results
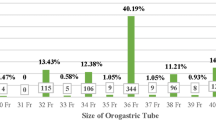
For preoperative preparations, surgeons preferred blood glucose control with insulin (61.0%), bowel cleaning (33.3%), and fasting and water deprivation (75.2%). For surgical techniques, surgeons preferred 36/38F bougie (86.7%), greater curvature mobilization with ultrasonic energy device (89.5%), direct transection of short gastric vessels (80%), antrum resection within 2–6 cm to the pylorus (84.8%) with 4.8 mm height stapler (72.4%), and 3.5 mm for corpus (94.3%). Whole stapler-line reinforcement, gastric sleeve fixation, leaking test, and abdominal drainage were preferred by 48.6, 62.9, 39, and 47.6% surgeons. For postoperative managements, surgeons preferred nasogastric tube insertion (33.3%), early liquid diet (69.6%), 4 weeks of liquid diet (55.2%), 2000 ml daily water intake before discharge (79%), 4 weeks of PPI (69.5%), and multi-vitamin supplementation 1 week after operation (77.1%). For postoperative complications, preferences were tachycardia as the onset of leak (81.0%) and oral contrast radiography for leak diagnosis (72.4%). Leak managements include US-guided percutaneous drainage (68.6%), nasogastric tube (87.6%), and parenteral nutrition (61%). For prolonged leak, enteral nutrition (87.6%) and Roux-en-Y bypass (84.8%) as the salvage procedure were preferred. 95.2% preferred endoscopic dilation for stricture.
Conclusions
LSG is gaining its wide application in China, but standardization of LSG is urgently needed.
Similar content being viewed by others
References
Ren CJ, Patterson E, Gagner M. Early results of laparoscopic biliopancreatic diversion with duodenal switch: a case series of 40 consecutive patients. Obes Surg. 2000;10(6):514–523; discussion 24. doi:10.1381/096089200321593715.
Regan JP, Inabnet WB, Gagner M, et al. Early experience with two-stage laparoscopic Roux-en-Y gastric bypass as an alternative in the super-super obese patient. Obes Surg. 2003;13(6):861–4. doi:10.1381/096089203322618669.
Kehagias I, Karamanakos SN, Argentou M, et al. Randomized clinical trial of laparoscopic Roux-en-Y gastric bypass versus laparoscopic sleeve gastrectomy for the management of patients with BMI < 50 kg/m2. Obes Surg. 2011;21(11):1650–6. doi:10.1007/s11695-011-0479-x.
Karamanakos SN, Vagenas K, Kalfarentzos F, et al. Weight loss, appetite suppression, and changes in fasting and postprandial ghrelin and peptide-YY levels after Roux-en-Y gastric bypass and sleeve gastrectomy: a prospective, double blind study. Ann Surg. 2008;247(3):401–7. doi:10.1097/SLA.0b013e318156f012.
Lee WJ, Chong K, Ser KH, et al. Gastric bypass vs sleeve gastrectomy for type 2 diabetes mellitus: a randomized controlled trial. Arch Surg. 2011;146(2):143–8. doi:10.1001/archsurg.2010.326.
Updated position statement on sleeve gastrectomy as a bariatric procedure. Surgery for obesity and related diseases: official journal of the American Society for Bariatric Surgery. 2012;8(3):e21–6. doi:10.1016/j.soard.2012.02.001.
Du X, Dai R, Zhou HX, et al. Bariatric surgery in China: how is this new concept going? Obes Surg. 2016; doi:10.1007/s11695-016-2204-2.
Reynolds K, Gu D, Whelton PK, et al. Prevalence and risk factors of overweight and obesity in China. Obesity (Silver Spring). 2007;15(1):10–8. doi:10.1038/oby.2007.527.
Xi B, Liang Y, He T, et al. Secular trends in the prevalence of general and abdominal obesity among Chinese adults, 1993–2009. Obesity reviews: an official journal of the International Association for the Study of Obesity. 2012;13(3):287–96. doi:10.1111/j.1467-789X.2011.00944.x.
Gloy VL, Briel M, Bhatt DL, et al. Bariatric surgery versus non-surgical treatment for obesity: a systematic review and meta-analysis of randomised controlled trials. BMJ. 2013;347:f5934. doi:10.1136/bmj.f5934.
Yanovski SZ, Yanovski JA. Long-term drug treatment for obesity: a systematic and clinical review. JAMA. 2014;311(1):74–86. doi:10.1001/jama.2013.281361.
Dombrowski SU, Knittle K, Avenell A, et al. Long term maintenance of weight loss with non-surgical interventions in obese adults: systematic review and meta-analyses of randomised controlled trials. BMJ. 2014;348:g2646. doi:10.1136/bmj.g2646.
Sakran N, Raziel A, Goitein O, et al. Laparoscopic sleeve gastrectomy for morbid obesity in 3003 patients: results at a high-volume bariatric center. Obes Surg. 2016; doi:10.1007/s11695-016-2063-x.
Osland E, Yunus RM, Khan S, et al. Postoperative early major and minor complications in laparoscopic vertical sleeve gastrectomy (LVSG) versus laparoscopic Roux-en-Y gastric bypass (LRYGB) procedures: a meta-analysis and systematic review. Obes Surg. 2016; doi:10.1007/s11695-016-2101-8.
Mechanick JI, Youdim A, Jones DB, et al. Clinical practice guidelines for the perioperative nutritional, metabolic, and nonsurgical support of the bariatric surgery patient—2013 update: cosponsored by American Association of Clinical Endocrinologists, The Obesity Society, and American Society for Metabolic & Bariatric Surgery. Obesity (Silver Spring). 2013;21(Suppl 1):S1–27. doi:10.1002/oby.20461.
Awad S, Carter S, Purkayastha S, et al. Enhanced recovery after bariatric surgery (ERABS): clinical outcomes from a tertiary referral bariatric centre. Obes Surg. 2014;24(5):753–8. doi:10.1007/s11695-013-1151-4.
Barreca M, Renzi C, Tankel J, et al. Is there a role for enhanced recovery after laparoscopic bariatric surgery? Preliminary results from a specialist obesity treatment center. Surgery for obesity and related diseases: official journal of the American Society for Bariatric Surgery. 2016;12(1):119–26. doi:10.1016/j.soard.2015.03.008.
Thorell A, MacCormick AD, Awad S, et al. Guidelines for perioperative care in bariatric surgery: Enhanced Recovery After Surgery (ERAS) society recommendations. World J Surg. 2016;40(9):2065–83. doi:10.1007/s00268-016-3492-3.
Lemanu DP, Singh PP, Berridge K, et al. Randomized clinical trial of enhanced recovery versus standard care after laparoscopic sleeve gastrectomy. The British journal of surgery. 2013;100(4):482–9. doi:10.1002/bjs.9026.
Obeidat F, Shanti H, Mismar A, et al. The magnitude of antral resection in laparoscopic sleeve gastrectomy and its relationship to excess weight loss. Obes Surg. 2015;25(10):1928–32. doi:10.1007/s11695-015-1642-6.
Rosenthal RJ, Diaz AA, Arvidsson D, et al. International sleeve gastrectomy expert panel consensus statement: best practice guidelines based on experience of >12,000 cases. Surgery for obesity and related diseases: official journal of the American Society for Bariatric Surgery. 2012;8(1):8–19. doi:10.1016/j.soard.2011.10.019.
Gagner M, Deitel M, Erickson AL, et al. Survey on laparoscopic sleeve gastrectomy (LSG) at the fourth international consensus summit on sleeve gastrectomy. Obes Surg. 2013;23(12):2013–7. doi:10.1007/s11695-013-1040-x.
Birkmeyer JD, Finks JF, O'Reilly A, et al. Surgical skill and complication rates after bariatric surgery. N Engl J Med. 2013;369(15):1434–42. doi:10.1056/NEJMsa1300625.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical Approval
For this type of study, formal consent is not required.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Conflict of Interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Lin, S., Guan, W., Hans, P. et al. Status of Laparoscopic Sleeve Gastrectomy in China: A National Survey. OBES SURG 27, 2968–2973 (2017). https://doi.org/10.1007/s11695-017-2727-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-017-2727-1