Abstract
Background
Previous studies addressing the changes in serum visfatin levels after bariatric surgery yielded conflicting results.
Methods
We measured serum visfatin levels in 41 morbidly obese women before bariatric surgery and after losing at least 15% of the initial weight, and analyzed the results taking into account the type of surgery, reproductive and diabetic status, among others. Body mass index, waist circumference, lipid profile, and insulin resistance determined by homeostasis model assessment (HOMA-IR) were also measured.
Results
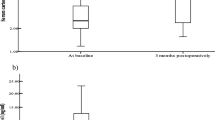
Patients lost 30.3 ± 6.1% of the initial body weight, and serum visfatin levels increased from 22.2 ± 20.9 to 32.2 ± 27.6 ng/ml (P = 0.031). A multiple regression model (R 2 = 0.314, F = 3.555, P = 0.017) including the percentage of weight loss, changes in waist circumference, HOMA-IR, high-density lipoprotein-cholesterol, and triglycerides (also expressed as percentage from baseline), the surgical procedure, time elapsed since surgery, and previous diabetic status as independent variables showed that weight loss (β = −0.670, P = 0.010), previous diabetic status (β = −0.330, P = 0.036), and change in waist circumference (β = 0.556, P = 0.031) were the main determinants of the percentual increase in serum visfatin levels observed after bariatric surgery.
Conclusion
Serum visfatin increased after bariatric surgery in relation to the amount of weight lost and to the changes in waist circumference, and this increase was higher in diabetic patients.

Similar content being viewed by others
References
Santry HP, Gillen DL, Lauderdale DS. Trends in bariatric surgical procedures. JAMA. 2005;294:1909–17.
Shah M, Simha V, Garg A. Review: long-term impact of bariatric surgery on body weight, comorbidities, and nutritional status. J Clin Endocrinol Metab. 2006;91:4223–31.
Fontaine KR, Redden DT, Wang C, Westfall AO, Allison DB. Years of life lost due to obesity. JAMA. 2003;289:187–93.
Sjostrom L, Lindroos AK, Peltonen M, et al. Lifestyle, diabetes, and cardiovascular risk factors 10 years after bariatric surgery. N Engl J Med. 2004;351:2683–93.
Sugerman HJ, Wolfe LG, Sica DA, Clore JN. Diabetes and hypertension in severe obesity and effects of gastric bypass-induced weight loss. Ann Surg. 2003;237:751–6; discussion 7–8.
Escobar-Morreale HF, Botella-Carretero JI, Alvarez-Blasco F, Sancho J, San Millan JL. The polycystic ovary syndrome associated with morbid obesity may resolve after weight loss induced by bariatric surgery. J Clin Endocrinol Metab. 2005;90:6364–9.
Fukuhara A, Matsuda M, Nishizawa M, et al. Visfatin: a protein secreted by visceral fat that mimics the effects of insulin. Science. 2005;307:426–30.
Stephens JM, Vidal-Puig AJ. An update on visfatin/pre-B cell colony-enhancing factor, an ubiquitously expressed, illusive cytokine that is regulated in obesity. Curr Opin Lipidol. 2006;17:128–31.
Pilz S, Mangge H, Obermayer-Pietsch B, Marz W. Visfatin/pre-B-cell colony-enhancing factor: a protein with various suggested functions. J Endocrinol Invest. 2007;30:138–44.
Krzyzanowska K, Mittermayer F, Krugluger W, Kopp HP, Schernthaner G. Increase in visfatin after weight loss induced by gastroplastic surgery. Obesity (Silver Spring). 2006;14:1886–9.
Manco M, Fernandez-Real JM, Equitani F, et al. Effect of massive weight loss on inflammatory adipocytokines and the innate immune system in morbidly obese women. J Clin Endocrinol Metab. 2007;92:483–90.
Haider DG, Schindler K, Schaller G, Prager G, Wolzt M, Ludvik B. Increased plasma visfatin concentrations in morbidly obese subjects are reduced after gastric banding. J Clin Endocrinol Metab. 2006;91:1578–81.
Li L, Yang G, Li Q, et al. Changes and relations of circulating visfatin, apelin, and resistin levels in normal, impaired glucose tolerance, and type 2 diabetic subjects. Exp Clin Endocrinol Diabetes. 2006;114:544–8.
Lopez-Bermejo A, Chico-Julia B, Fernandez-Balsells M, et al. Serum visfatin increases with progressive beta-cell deterioration. Diabetes. 2006;55:2871–5.
Tan BK, Chen J, Digby JE, Keay SD, Kennedy CR, Randeva HS. Increased visfatin messenger ribonucleic acid and protein levels in adipose tissue and adipocytes in women with polycystic ovary syndrome: parallel increase in plasma visfatin. J Clin Endocrinol Metab. 2006;91:5022–8.
Scopinaro N. Biliopancreatic diversion: mechanisms of action and long-term results. Obes Surg. 2006;16:683–9.
Rosenthal RJ, Szomstein S, Kennedy CI, Soto FC, Zundel N. Laparoscopic surgery for morbid obesity: 1,001 consecutive bariatric operations performed at The Bariatric Institute, Cleveland Clinic Florida. Obes Surg. 2006;16:119–24.
Zawadzki JK, Dunaif A. Diagnostic criteria for polycystic ovary syndrome: toward a rational approach. In: Dunaif A, Givens JR, Haseltine FP, Merriam GR, editors. Polycystic ovary syndrome. Boston: Blackwell Scientific Publications; 1992. pp. 377–84.
Botella-Carretero J, Alvarez-Blasco F, Martinez-Garcia MA, Luque-Ramirez M, San Millan JL, Escobar-Morreale HF. The decrease in serum IL-18 levels after bariatric surgery in morbidly obese women is a time-dependent event. Obes Surg. 2007;17:1199–208.
Vermeulen A, Verdonck L, Kaufman JM. A critical evaluation of simple methods for the estimation of free testosterone in serum. J Clin Endocrinol Metab. 1999;84:3666–72.
Matthews DR, Hosker JP, Rudenski AS, Naylor BA, Treacher DF, Turner RC. Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia. 1985;28:412–9.
Zahorska-Markiewicz B, Olszanecka-Glinianowicz M, Janowska J, et al. Serum concentration of visfatin in obese women. Metabolism. 2007;56:1131–4.
Jian WX, Luo TH, Gu YY, et al. The visfatin gene is associated with glucose and lipid metabolism in a Chinese population. Diabet Med. 2006;23:967–73.
Pagano C, Pilon C, Olivieri M, et al. Reduced plasma visfatin/pre-B cell colony-enhancing factor in obesity is not related to insulin resistance in humans. J Clin Endocrinol Metab. 2006;91:3165–70.
Garcia-Fuentes E, Garcia-Almeida JM, Garcia-Arnes J, et al. Plasma visfatin concentrations in severely obese subjects are increased after intestinal bypass. Obesity (Silver Spring). 2007;15:2391–5.
Fernandez-Real JM, Moreno JM, Chico B, Lopez-Bermejo A, Ricart W. Circulating visfatin is associated with parameters of iron metabolism in subjects with altered glucose tolerance. Diabetes Care. 2007;30:616–21.
Takebayashi K, Suetsugu M, Wakabayashi S, Aso Y, Inukai T. Association between plasma visfatin and vascular endothelial function in patients with type 2 diabetes mellitus. Metabolism. 2007;56:451–8.
Bottcher Y, Teupser D, Enigk B, et al. Genetic variation in the visfatin gene (PBEF1) and its relation to glucose metabolism and fat-depot-specific messenger ribonucleic acid expression in humans. J Clin Endocrinol Metab. 2006;91:2725–31.
Chan TF, Chen YL, Lee CH, et al. Decreased plasma visfatin concentrations in women with gestational diabetes mellitus. J Soc Gynecol Investig. 2006;13:364–7.
Haider DG, Handisurya A, Storka A, et al. Visfatin response to glucose is reduced in women with gestational diabetes mellitus. Diabetes Care. 2007;30:1889–91.
Haider DG, Mittermayer F, Schaller G, et al. Free fatty acids normalize a rosiglitazone-induced visfatin release. Am J Physiol Endocrinol Metab. 2006;291:E885–90.
Dogru T, Sonmez A, Tasci I, et al. Plasma visfatin levels in patients with newly diagnosed and untreated type 2 diabetes mellitus and impaired glucose tolerance. Diabetes Res Clin Pract. 2007;76:24–9.
Chen MP, Chung FM, Chang DM, et al. Elevated plasma level of visfatin/pre-B cell colony-enhancing factor in patients with type 2 diabetes mellitus. J Clin Endocrinol Metab. 2006;91:295–9.
Krzyzanowska K, Krugluger W, Mittermayer F, et al. Increased visfatin concentrations in women with gestational diabetes mellitus. Clin Sci (Lond). 2006;110:605–9.
Hsieh CH, He CT, Lee CH, Wu LY, Hung YJ. Both slow-release and regular-form metformin improve glycemic control without altering plasma visfatin level in patients with type 2 diabetes mellitus. Metabolism. 2007;56:1087–92.
Hammarstedt A, Pihlajamaki J, Rotter Sopasakis V, et al. Visfatin is an adipokine, but it is not regulated by thiazolidinediones. J Clin Endocrinol Metab. 2006;91:1181–4.
Arner P. Visfatin-a true or false trail to type 2 diabetes mellitus. J Clin Endocrinol Metab. 2006;91:28–30.
Prins JB, O’Rahilly S. Regulation of adipose cell number in man. Clin Sci (Lond). 1997;92:3–11.
Loftus TM, Kuhajda FP, Lane MD. Insulin depletion leads to adipose-specific cell death in obese but not lean mice. Proc Natl Acad Sci U S A. 1998;95:14168–72.
Acknowledgments
We thank Ms. Genoveva Gonzalez, Endocrinology Laboratory, Hospital Universitario Ramón y Cajal for excellent technical help. This study was supported by the Spanish Ministry of Health and Consumer Affairs, Instituto de Investigación Carlos III, grants FIS PI050341 and REDIMET RD06/0015/0007.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Botella-Carretero, J.I., Luque-Ramírez, M., Álvarez-Blasco, F. et al. The Increase in Serum Visfatin After Bariatric Surgery in Morbidly Obese Women is Modulated by Weight Loss, Waist Circumference, and Presence or Absence of Diabetes Before Surgery. OBES SURG 18, 1000–1006 (2008). https://doi.org/10.1007/s11695-007-9369-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-007-9369-7