Abstract
Purpose. We compared 3-Tesla (3-T) and 1.5-Tesla (1.5-T) cardiac magnetic resonance imaging (MRI) for the assessment of myocardial viability in nearly identical experimental conditions
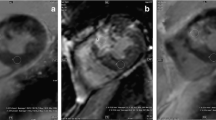
Materials and methods. Thirty-five patients (mean age 63±11; 94.2% men) submitted to primary coronary angioplasty underwent both 3-T and 1.5-T cardiac MRI, which was considered the gold standard. Comparison was performed on the basis of the same viability imaging protocol, which included resting cine-MR [balanced fastfield echo (b-FFE) sequence] followed by contrastenhanced MR to evaluate perfusion and delayed enhancement (DE). We then performed functional index measurements and visual estimation of kinesis, perfusion and DE referring to a 5-point scale. Image quality was assessed on the basis of signal to noise ratio (SNR) and contrast to noise ratio (CNR)
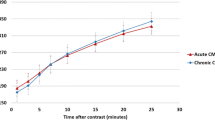
Results. We found nonsignificant differences between the two scanners (p=NS) in measuring the functional and viability parameters. Myocardial SNR was significantly higher with 3-T MRI compared with 1.5-T MRI (61.3% gain). Even though a loss of CNR was recorded in b-FFE and in first-pass perfusion sequences (12.4% and 23.7%, respectively), on DE images, we quantified the increase of SNR and CNR of infarction of 387.8% and 330%, respectively
Conclusions. We found that 3-T MRI showed high concordance with 1.5-T MRI in the evaluation of functional and viability parameters and provided better evidence of damaged myocardium
Riassunto
Obiettivo. Confrontare la risonanza magnetica (RM) cardiaca a 3 Tesla (3 T) con quella a 1,5 Tesla (1,5 T) per la valutazione della vitalità miocardica in condizioni sperimentali essenzialmente identiche
Materiali e metodi. Trentacinque pazienti (età media di 63±11; 94,2% maschi) dopo essere stati sottoposti ad angioplastica primaria sono stati esaminati sia con RM cardiaca a 3 T che RM cardiaca a 1,5 T, che è stata considerata il gold standard. Il confronto è stato effettuato basandosi sullo stesso protocollo di imaging di vitalità che includeva: cine-MR a riposo (sequenza b-FFE) seguito da somministrazione di contrasto per la valutazione della perfusione e dell’enhancement tardivo (DE). È stata poi eseguita la misura degli indici funzionali e l’analisi visuale della cinesi, perfusione e dell’enhancement tardivo basandosi su una scala a 5 punti. La qualità di immagine è stata valutata sulla base del rapporto segnale-rumore (SNR) e del rapporto contrasto-rumore (CNR)
Risultati. Abbiamo trovato una differenza statisticamente non significativa tra le due apparecchiature RM (p=NS) nella misurazione dei parametri funzionali e di vitalità. Il SNR miocardico è risultato significativamente più alto con lo scanner a 3 T MR rispetto a quello a 1,5 T (61,3% guadagno). Nonostante sia stata apprezzata una perdita di CNR nelle sequenze b-FFE e di perfusione al primo passaggio (12,4% e 23,7% rispettivamente), nelle immagini di enhancement tardivo abbiamo quantificato un aumento del SNR e CNR del tessuto infartuato del 387,8% e 330% rispettivamente
Conclusioni. La RM a 3 Tesla ha dimostrato una alta concordanza con quella a 1,5 Tesla riguardo alla valutazione dei parametri funzionali e di vitalità con una più cospicua evidenza del miocardio danneggiato
Similar content being viewed by others
References/Bibliografia
Pairoj Rerkpattanapipat P, Mazur W, Link KM, Hundley GW (2003) Assessment of cardiac function with MR imaging. Magn Reson Imaging Clin N Am 11:67–80
Kim RJ, Wu E, Rafael A et al (2000) The use of contrast-enhanced magnetic resonance imaging to identify myocardial dysfunction. N Engl J Med 343:1445–1453
Fassa AA, Urban P, Radovanovic D et al; AMIS Plus Investigators (2005) Trends in reperfusion therapy of ST segment elevation myocardial infarction in Switzerland: six year results from a nationwide registry. Heart 91:882–888
Klem I, Heitner JF, Shah DJ et al (2006) Improved detection of coronary artery disease by stress perfusion cardiovascular magnetic resonance with the use of delayed enhancement infarction imaging. J Am Coll Cardiol 47:1630–1638
Xu D, Henry RG, Mukherjee P et al (2004) Single-shot fast spin-echo diffusion tensor imaging of the brain and spine with head and phased array coils at 1.5 T and 3.0 T. Magn Reson Imaging 22:751–759
Al-Kwifi O, Emery DJ, Wilman AH (2002) Vessel contrast at three Tesla in time-of-flight magnetic resonance angiography of the intracranial and carotid arteries. Magn Reson Imaging 20:181–187
McGee KP, Debbins JP, Boskamp EB et al (2004) Cardiac magnetic resonance parallel imaging at 3.0 Tesla: technical feasibility and advantages. J Magn Reson Imaging 19:291–297
Chuang ML, Hibberd MG, Salton CJ et al (2000) Importance of imaging method over imaging modality in noninvasive determination of left ventricular volumes and ejection fraction: assessment by two-and threedimensional echocardiography and magnetic resonance imaging. J Am Coll Cardiol 35:477–484
Cerqueira MD, Weissman NJ, Dilsizian V et al (2002) Standardized myocardial segmentation and nomenclature for tomographic imaging of the heart: a statement for healthcare professionals from the Cardiac Imaging Committee of the Council on Clinical Cardiology of the American Heart Association. Circulation 105:539–542
Wu E, Judd RM, Vargas JD et al (2001) Visualisation of presence, location, and transmural extent of healed Q-wave and non-Q-wave myocardial infarction. Lancet 357:21–28
Gerber TC, Fasseas P, Lennon RJ et al (2003) Clinical safety of magnetic resonance imaging early after coronary artery stent placement. Am Coll Cardiol 42:1295–1298
Doherty NE 3rd, Seelos KC, Suzuki J et al (1992) Application of cine nuclear magnetic resonance imaging for sequential evaluation of response to angiotensin-converting enzyme inhibitor therapy in dilated cardiomyopathy. J Am Coll Cardiol 19:1294–1302
Lombardi M, Kvaerness J, Torheim G et al (2001) Relationship between function and perfusion early after acute myocardial infarction. Int J Cardiovasc Imaging 17:383–393
Penzkofer H, Wintersperger BJ, Knez A et al (1999) Assessment of myocardial perfusion using multisection first-pass MRI and color-coded parameter maps: a comparison to 99mTc sesta MIBI SPECT and systolic myocardial wall thickening analysis. Magn Reson Imaging 17:161–170
Kim RJ, Chen EL, Lima JAC, Judd RM (1996) Myocardial Gd-DTPA kinetics determine MRI contrast enhancement and reflect the extent and severity of myocardial injury after acute reperfused infarction. Circulation 94:3318–3326
Kaandorp TAM, Bax JJ, Schuijf JD et al (2004) Head-to-head comparison between contrast-enhanced magnetic resonance imaging and dobutamine magnetic resonance imaging in men with ischemic cardiomyopathy. Am J Cardiol 93:1461–1464
Schuijf JD, Kaandorp TAM, Lamb HJ et al (2004) Quantification of myocardial infarct size and transmurality by contrast-enhanced magnetic resonance imaging in men. Am J Cardiol 94:284–288
Kim RJ, Manning WJ (2004) Viability assessment by delayed enhancement cardiovascular magnetic resonance will low-dose dobutamine dull the shine? Circulation 109:2476–2479
Task Force of the European Society of Cardiology, in collaboration with the Association of European Paediatric Cardiologists (1998) The clinical role of magnetic resonance in cardiovascular disease. Eur Heart J 19:19–39
Barkhausen J, Ruehm SG, Goyen M (2001) MR evaluation of LV function: true fast imaging with steady-state precession versus fast low-angle shot cine MR imaging: feasibility study. Radiology 219:264–269
Thiele H, Paetsch I, Schnackenburg B et al (2002) Improved accuracy of quantitative assessment of left ventricular volume and ejection fraction by geometric models with steady-state free precession. J Cardiovasc Magn Reson 4:327–339
Michaely HJ, Nael K, Schoenberg SO et al (2006) Analysis of cardiac function-comparison between 1.5 Tesla and 3 Tesla cardiac cine magnetic resonance imaging: preliminary experience. Invest Radiol 41:133–140
Takahashi M, Hidemasa U, Hatabu H (2003) MR imaging at high magnetic fields. Eur J Radiol 46:45–52
Dougherty L, Connick TJ, Mizsei G (2001) Cardiac imaging at 4.0 Tesla. Magn Reson Med 45:176–178
Noeske R, Seifert F, Rhein KH, Rinneberg H (2000) Human cardiac imaging at 3 T using phased array coils. Magn Reson Med 44:978–982
Shellock FG, Crues JV (2004) MR procedures: biologic effects, safety, and patient care. Radiology 232:635–652
McGee KP, Debbins JP, Boskamp EB et al (2004) Cardiac magnetic resonance parallel imaging at 3.0 Tesla: technical feasibility and advantages. J Magn Reson Imaging 19:291–297
Araoz PA, Glockner JF, McGee KP et al (2005) 3 Tesla MR imaging provides improved contrast in first-pass myocardial perfusion imaging over a range of gadolinium doses. J Cardiovasc Magn Reson 7:559–564
Gutberlet M, Noeske R, Schwinge K et al (2006) Comprehensive cardiac magnetic resonance imaging at 3 Tesla: feasibility and implicationd for clinical applications. Invest Radiol 41:154–167
Nakajima T, Oriuchi N, Tsushima Y et al (2004) Noninvasive determination of regional myocardial perfusion with first-pass magnetic resonance (MR) imaging. Acad Radiol 11:802–808
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ligabue, G., Fiocchi, F., Ferraresi, S. et al. 3-Tesla MRI for the evaluation of myocardial viability: a comparative study with 1.5-Tesla MRI. Radiol med 113, 347–362 (2008). https://doi.org/10.1007/s11547-008-0256-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-008-0256-7