Abstract
Purpose
Sleep architecture can be affected by alteration in circulating lipopolysaccaride and cytokines. However, still unknown are the effects of lipopolysaccaride-binding protein (LBP) on sleep architecture. Therefore, potential relationship between alteration in serum LBP concentrations and sleep architecture was analyzed.
Methods
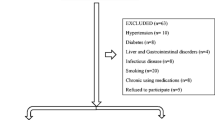
This is a cross-sectional study. Consecutive 54 hypertensive males, aged 30–65 years. and with no obstructive sleep apnea via polysomnography, were recruited. Subjects were divided into two groups via the LBP median as hypertensives with higher and lower serum LBP (n = 27 and n = 27, respectively). Sleep architecture was assessed by polysomnography. Serum LBP, IL-1β, IL-6, and TNF-α were measured by commercial laboratories using sandwich-type enzyme immunoassay kit.
Results
Hypertensive subjects with higher LBP showed significantly higher inflammatory status as assessed by IL-1β (18.85 ± 3.71 vs 16.15 ± 4.00 ng/L, P = 0.009), IL-6 (67.64 ± 11.22 vs 58.94 ± 11.32 ng/L, P = 0.004), and TNF-α (322.27 ± 59.17 vs 283.89 ± 61.87 pg/ml, P = 0.024) than did those with lower LBP. Hypertensives with higher serum LBP also exhibited prolonged N1 % (7.63 ± 3.55 vs 4.98 ± 2.90 %, P = 0.002), the transition from wakefulness to other sleep stages or follows arousal during sleep, than did those with lower LBP. A significant positive correlation was observed between serum LBP concentrations and N1 % (r = 0.378, P = 0.005) via Spearman’s correlation and remained significant even after adjusting for age, apnea-hypopnea index, and body mass index.
Conclusion
Elevation in serum concentrations of LBP might prolong N1 % in this middle-aged hypertensive males, which needs to be confirmed further.

Similar content being viewed by others
References
Brown RE, Basheer R, McKenna JT, Strecker RE, McCarley RW (2012) Control of sleep and wakefulness. Physiol Rev 92:1087–1187
Imeri L, Opp MR (2009) How (and why) the immune system makes us sleep. Nat Rev Neurosci 10:199–210
Schaefer CF, Brackett DJ, Wilson MF, Gunn CG (1978) Lifelong hyperarousal in the spontaneously hypertensive rat indicated by operant behavior. Pavlov J Biol Sci 13:217–225
Obál F Jr, Krueger JM (2005) Biochemical regulation of non-rapid eye movement sleep. Frontiers Biosci 8:520–550
Krueger JM, Obal FJ, Fang J, Kubota T, Taishi P (2001) The role of cytokines in physiological sleep regulation. Ann N Y Acad Sci 933:211–221
Gamaldo CE, Shaikh AK, McArthur JC (2012) The sleep-immunity relationship. Neurol Clin 30:1313–1343
Gozal D, Serpero LD, Kheirandish-Gozal L, Capdevila OS, Khalyfa A, Tauman R (2010) Sleep measures and morning plasma TNF-alpha levels in children with sleep-disordered breathing. Sleep 33:319–325
Redwine L, Hauger RL, Gillin JC, Irwin M (2000) Effects of sleep and sleep deprivation on interleukin-6, growth hormone, cortisol, and melatonin levels in humans. J Clin Endocrinol Metab 85:3597–3603
Reiberger T, Ferlitsch A, Payer BA, Mandorfer M, Heinisch BB, Hayden H, Lammert F, Trauner M, Peck-Radosavljevic M, Vogelsang H, Vienna Hepatic Hemodynamic Lab (2013) Non-selective beta blocker therapy decreases intestinal permeability and serum levels of LBP and IL-6 in patients with cirrhosis. J Hepatol 58:911–921
Oishi Y, Yoshida K, Scammell TE, Urade Y, Lazarus M, Saper CB (2015) The roles of prostaglandin E2 and D2 in lipopolysaccharide-mediated changes in sleep. Brain Behav Immun 47:172–177
Lee YK, Mazmanian SK (2010) Has the microbiota played a critical role in the evolution of the adaptive immune system? Science 330:1768–1773
Hooper LV, Littman DR, Macpherson AJ (2012) Interactions between the microbiota and the immune system. Science 336:1268–1273
Wen L, Ley RE, Volchkov PY, Stranges PB, Avanesyan L, Stonebraker AC, Hu C, Wong FS, Szot GL, Bluestone JA, Gordon JI, Chervonsky AV (2008) Innate immunity and intestinal microbiota in the development of type 1 diabetes. Nature 455:1109–1113
Turnbaugh PJ, Hamady M, Yatsunenko T, Cantarel BL, Duncan A, Ley RE, Sogin ML, Jones WJ, Roe BA, Affourtit JP, Egholm M, Henrissat B, Heath AC, Knight R, Gordon JI (2009) A core gut microbiome in obese and lean twins. Nature 457:480–484
Hanaoka Y, Soejima H, Yasuda O, Nakayama H, Nagata M, Matsuo K, Shinohara M, Izumi Y, Ogawa H (2013) Level of serum antibody against a periodontal pathogen is associated with atherosclerosis and hypertension. Hypertens Res 36:829–833
Gaetti-Jardim E Jr, Marcelino SL, Feitosa AC, Romito GA, Avila-Campos MJ (2009) Quantitative detection of periodontopathic bacteria in atherosclerotic plaques from coronary arteries. J Med Microbiol 58:1568–1575
Soto-Barreras U, Olvera-Rubio JO, Loyola-Rodriguez JP, Reyes-Macias JF, Martinez-Martinez RE, Patiño-Marin N, Martinez-Castañon GA, Aradillas-Garcia C, Little JW (2013) Peripheral arterial disease associated with caries and periodontal disease. J Periodontol 84:486–494
Cani PD, Amar J, Iglesias MA, Poggi M, Knauf C, Bastelica D, Neyrinck AM, Fava F, Tuohy KM, Chabo C, Waget A, Delmée E, Cousin B, Sulpice T, Chamontin B, Ferrières J, Tanti JF, Gibson GR, Casteilla L, Delzenne NM, Alessi MC, Burcelin R (2007) Metabolicendotoxemia initiates obesity and insulin resistance. Diabetes 56:1761–1772
Sen R, Baltimore D (1986) Multiple nuclear factors interact with the immunoglobulin enhancer sequence. Cell 46:705–716
van Eijk LT, Dorresteijn MJ, Smits P, van der Hoeven JG, Netea MG, Pickkers P (2007) Gender differences in the innate immune response and vascular reactivity following the administration of endotoxin to human volunteers. Crit Care Med 35:1464–1469
Saad MJ, Santos A, Prada PO (2016) Linking gut microbiota and inflammation to obesity and insulin resistance. Physiology (Bethesda) 31:283–293
Trakada G, Steiropoulos P, Zarogoulidis P, Nena E, Papanas N, Maltezos E, Bouros D (2014) A fatty meal aggravates apnea and increases in patients with obstructive sleep apnea. Sleep Breath 18:53–58
Erridge C, Attina T, Spickett CM, Webb DJ (2007) A high-fat meal induces low-grade endotoxemia: evidence of a novel mechanism of postprandial inflammation. Am J Clin Nutr 86:1286–1292
Acknowledgments
The authors thank all the participants for agreeing to provide all the clinical data and blood samples, and all the staffs of hypertension center for collaborating to accomplish this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
Xinjiang China provided financial support in the form of the Natural Science Foundation of Xinjiang (2015211C197). The sponsor had no role in the design or conduct of this research.
Conflict of interest
All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest, or non-financial interest in the subject matter or materials discussed in this manuscript.
Ethical approval
Ethics Committee of the People’s Hospital of Xinjiang Uygur Autonomous Region approved the study protocol. All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Heizhati, M., Li, N., Shao, L. et al. Elevated serum concentrations of lipopolysaccharide binding protein might prolong sleep stage one in middle-aged hypertensive males. Sleep Breath 21, 327–332 (2017). https://doi.org/10.1007/s11325-016-1415-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-016-1415-z