Abstract
Purpose
Obstructive sleep apnea (OSA) is a highly prevalent disease. For diagnostic and therapeutic purposes, OSA has been divided into several subgroups. Positional OSA (POSA), the most frequent subgroup (56 %), is described as overall apnea hypopnea index (AHI) ≥5 and supine AHI at least twice as high when compared to non-supine AHI. We aimed to investigate the frequency of ulnar nerve entrapment neuropathy at the elbow (UNEE) in OSA patients without clinical signs and symptoms of ulnar neuropathy and intended to find if sleeping position in OSA had an impact on UNEE development.
Methods
Fifty POSA, 48 non-positional OSA (NPOSA) patients, and 45 healthy controls without diabetes mellitus, hypothyroidism, rheumatic diseases, and cervical radiculopathy underwent nerve conduction studies.
Results
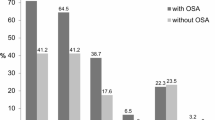
We found that UNEE was highly frequent in OSA patients (42.9 %) and significantly more frequent in moderate to severe POSA patients than mild POSA patients (65.4 vs. 33.3 %, p < 0.05). Furthermore, when compared to non-positional ones, UNEE was significantly more frequent in moderate to severe POSA patients (65.4 vs. 36.4 %, p < 0.05).
Conclusions
Our results showed that the severity of OSA in positional patients was correlated with increased frequency of UNEE. OSA patients should be informed about the predisposition of UNEE and questioned for the symptoms in periodical controls. POSA patients should be alerted about the additional effect of sleeping position on UNEE and the necessity of OSA treatment should be emphasized.

Similar content being viewed by others
References
Assmus H, Antoniadis G, Bischoff C (2015) Carpal and cubital tunnel and other, rarer nerve compression syndromes. Dtsch Arztebl Int 112:14–25
Assmus H, Antoniadis G, Bischoff C, Hoffmann R, Martini AK, Preissler P, Scheglmann K, Schwerdtfeger K, Wessels KD, Wüstner-Hofmann M (2011) Cubital tunnel syndrome—a review and management guidelines. Cent Eur Neurosurg 72:90–98
Macnicol MF (1982) Extraneural pressures affecting the ulnar nerve at the elbow. Hand 14:5–11
Sakurai M, Miyasaka Y (1986) Neural fibrosis and the effect of neurolysis. J Bone Joint Surg (Br) 68:483–488
Vinik A, Mehrabyan A, Colen L, Boulton A (2004) Focal entrapment neuropathies in diabetes. Diabetes Care 27:1783–1788
Landau ME, Barner KC, Campbell WW (2005) Effect of body mass index on ulnar nerve conduction velocity, ulnar neuropathy at the elbow, and carpal tunnel syndrome. Muscle Nerve 32:360–363
Stamboulis E, Vlachou N, Drossou-Servou M, Tsaftaridis P, Koutsis G, Katsaros N, Economou-Petersen E, Loutradi-Anagnostou A (2004) Axonal sensorimotor neuropathy in patients with beta-thalassaemia. J Neurol Neurosurg Psychiatry 75:1483–1486
Kryger MH (2000) Diagnosis and management of sleep apnea syndrome. Clin Cornerstone 2:39–47
Peppard PE, Young T, Barnet JH, Palta M, Hagen EW, Hla KM (2013) Increased prevalence of sleep-disordered breathing in adults. Am J Epidemiol 177:1006–1014
Gastaut H, Tassinari CA, Duron B (1966) Polygraphic study of the episodic diurnal and nocturnal (hypnic and respiratory) manifestations of the Pickwick syndrome. Brain Res 1:167–186
Ryan S, Taylor CT, McNicholas WT (2005) Selective activation of inflammatory pathways by intermittent hypoxia in obstructive sleep apnea syndrome. Circulation 112:2660–2667
Silber MH, Ancoli-Israel S, Bonnet MH, Chokroverty S, Grigg-Damberger MM, Hirshkowitz M, Kapen S, Keenan SA, Kryger MH, Penzel T, Pressman MR, Iber C (2007) The visual scoring of sleep in adults. J Clin Sleep Med 3:121–131
Cartwright R, Ristanovic R, Diaz F, Caldarelli D, Alder G (1991) A comparative study of treatments for positional sleep apnea. Sleep 14:546–552
Yaggi HK, Concato J, Kernan WN, Lichtman JH, Brass LM, Mohsenin V (2005) Obstructive sleep apnea as a risk factor for stroke and death. N Engl J Med 353:2034–2041
Yaffe K, Laffan AM, Harrison SL, Redline S, Spira AP, Ensrud KE, Ancoli-Israel S, Stone KL (2011) Sleep-disordered breathing, hypoxia, and risk of mild cognitive impairment and dementia in older women. JAMA 306:613–619
Lüdemann P, Dziewas R, Sörös P, Happe S, Frese A (2001) Axonal polyneuropathy in obstructive sleep apnoea. J Neurol Neurosurg Psychiatry 70:685–687
Dziewas R, Schilling M, Engel P, Boentert M, Hor H, Okegwo A, Lüdemann P, Ringelstein EB, Young P (2007) Treatment for obstructive sleep apnoea: effect on peripheral nerve function. J Neurol Neurosurg Psychiatry 78:295–297
Pevernagie DA, Shepard JW Jr (1992) Relations between sleep stage, posture and effective nasal CPAP levels in OSA. Sleep 15:162–167
Joosten SA, Edwards BA, Wellman A, Turton A, Skuza EM, Berger PJ, Hamilton GS (2015) The effect of body position on physiological factors that contribute to obstructive sleep apnea. Sleep 38:1469–1478
Mador MJ, Kufel TJ, Magalang UJ, Rajesh SK, Watwe V, Grant BJ (2005) Prevalence of positional sleep apnea in patients undergoing polysomnography. Chest 128:2130–2137
Filippou G, Mondelli M, Greco G, Bertoldi I, Frediani B, Galeazzi M, Giannini F (2010) Ulnar neuropathy at the elbow: how frequent is the idiopathic form? An ultrasonographic study in a cohort of patients. Clin Exp Rheumatol 28:63–67
Berry RB, Budhiraja R, Gottlieb DJ, Gozal D, Iber C, Kapur VK, Marcus CL, Mehra R, Parthasarathy S, Quan SF, Redline S, Strohl KP, Davidson Ward SL, Tangredi MM, American Academy of Sleep Medicine (2012) Rules for scoring respiratory events in sleep: update of the 2007 AASM manual for the scoring of sleep and associated events. Deliberations of the sleep apnea definitions task force of the american academy of sleep medicine. J Clin Sleep Med 8:597–619
Thibault MW, Robinson LR, Franklin G, Fulton-Kehoe D (2005) Use of the AAEM guidelines in electrodiagnosis of ulnar neuropathy at the elbow. Am J Phys Med Rehabil 84:267–273
American Association of Electrodiagnostic Medicine, Campbell WW (1999) Guidelines in electrodiagnostic medicine. Practice parameter for electrodiagnostic studies in ulnar neuropathy at the elbow. Muscle Nerve Suppl 8:S171–S205
Franklin KA, Lindberg E (2015) Obstructive sleep apnea is a common disorder in the population—a review on the epidemiology of sleep apnea. J Thorac Dis 7:1311–1322
Bixler EO, Vgontzas AN, Ten Have T, Tyson K, Kales A (1998) Effects of age on sleep apnea in men: I. Prevalence and severity. Am J Respir Crit Care Med 157:144–148
Chung JW, Enciso R, Levendowski DJ, Westbrook PR, Clark GT (2010) Patients with positional versus nonpositional obstructive sleep apnea: a retrospective study of risk factors associated with apnea-hypopnea severity. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 110:605–610
Mayer P, Dematteis M, Pépin JL, Wuyam B, Veale D, Vila A, Lévy P (1999) Peripheral neuropathy in sleep apnea. A tissue marker of the severity of nocturnal desaturation. Am J Respir Crit Care Med 159:213–219
Enright PL, Newman AB, Wahl PW, Manolio TA, Haponik EF, Boyle PJ (1996) Prevalence and correlates of snoring and observed apneas in 5,201 older adults. Sleep 19:531–538
Oksenberg A, Gadoth N (2014) Are we missing a simple treatment for most adult sleep apnea patients? The avoidance of the supine sleep position. J Sleep Res 23:204–210
Acknowledgments
The authors thank Dr. Hande Alibaş for her tolerant support on statistical analysis; Mrs. Sercan Davulcu for her ambitious technical assistance in Clinical Neurophysiology Laboratory; and Mrs. Birsen Tarım, Mrs. Olga Bahar Güler, and Mr. Ercan Yavuz for their kind support in the Sleep Laboratory.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No funding was received for this research.
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Bilgin Topçuoğlu, Ö., Oruç, Ö., Afşar, G.Ç. et al. Ulnar nerve entrapment at elbow in obstructive sleep apnea patients: a randomized controlled trial. Sleep Breath 21, 45–51 (2017). https://doi.org/10.1007/s11325-016-1360-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-016-1360-x