Abstract
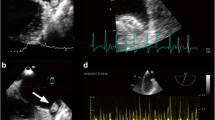
A 59-year-old white woman with previous history of arterial hypertension consulted because of palpitations. Atrial fibrillation of uncertain duration was diagnosed. She was not receiving anticoagulants. A trans-esophageal echocardiogram was performed, and a large left atrial appendage thrombus was detected. A strategy of rate control and anti-vitamin K treatment was started. On the subsequent days, we could not reach therapeutic INRs. Therefore, it was decided to stop warfarin and initiate dabigatran. We describe the evolution of the patient, the thrombus resolution, and a successful electrical cardioversion. In our comments, we summarize the natural history of left atrial thrombus, both with and without anticoagulant therapy. We also discuss the differences between warfarin and dabigatran.

Similar content being viewed by others
References
Prasad V, Kaplan RM, Passman RS (2012) New frontiers for stroke prevention in atrial fibrillation. Cerebrovasc Dis. 33:199–208
Freeman WD, Aguilar MI (2011) Prevention of cardioembolic stroke. Neurotherapeutics 8:488–502
Wolfram O, Hammwoehner M, Gramley F, Goette A (2011) Update on pharmacologic approaches to prevent thromboembolism in atrial fibrillation: are thrombin and factor Xa inhibitors the ultimate answer? Curr Vasc Pharmacol 9:350–357
Broukhim M, Halperin JL (2011) Stroke prevention in the high-risk atrial fibrillation patient: Medical management. Curr Cardiol Rep. 13:9–17
Medi C, Hankey GJ, Freedman SB (2010) Stroke risk and antithrombotic strategies in atrial fibrillation. Stroke 41:2705–2713
Santos-Gallego CG, Bayón J, Badimón JJ (2010) Thrombi of different pathologies: implications for diagnosis and treatment. Curr Treat Options Cardiovasc Med. 12:274–291
Savelieva I, Bajpai A, Camm AJ (2007) Stroke in atrial fibrillation: update on pathophysiology, new antithrombotic therapies, and evolution of procedures and devices. Ann Med 39:371–391
Thambidorai SK, Murray RD, Parakh K, Shah TK, Black IW, Jasper SE, Li J, Apperson-Hansen C, Asher CR, Grimm RA (2005) ACUTE investigators. utility of transesophageal echocardiography in identification of thrombogenic milieu in patients with atrial fibrillation (an ACUTE ancillary study). Am J Cardiol 96:935–941
Odum LE, Cochran KA, Aistrope DS, Snella KA (2012) The CHADS(2) versus the new CHA(2) DS(2) -VASc scoring systems for guiding Antithrombotic treatment of patients with Atrial Fibrillation: Review of the Literature and Recommendations for Use. Pharmacotherapy 32:285–296
Harenberg J, Leber G, Dempfle CE, Heene DL, Zimmermann R, Kübler W (1989) Long term anticoagulation with low molecular weight heparin in outpatients with side effects on oral anticoagulants. Nouv Rev Fr Hematol 31:363–369
Roijer A, Eskilsson J, Olsson B (2000) Transoesophageal echocardiography-guided cardioversion of atrial fibrillation or flutter. Selection of a low-risk group for immediate cardioversion. Eur Heart J 21:837–847
Sinnaeve PR, Huang Y, Bogaerts K, Vahanian A, Adgey J, Armstrong PW, Wallentin L, Van de Werf FJ (2006) age, outcomes, and treatment effects of fibrinolytic and antithrombotic combinations: findings from assessment of the Safety and Efficacy of a new Thrombolytic (ASSENT)-3 and ASSENT-3 PLUS. Am Heart J 152(684):e1–e9
Connolly SJ, Ezekowitz MD, Yusuf S, et al., and the RE-LY Steering Committee and Investigators(2009) Dabigatran versus Warfarin in Patients with Atrial Fibrillation. N Engl J Med361:1139-1151
Di Nisio M, Middeldorp S, Büller HR (2005) Direct thrombin inhibitors. N Engl J Med 353:1028–1040
Clouse LH, Comp PC (1986) The regulation of hemostasis: The protein C system. N Engl J Med 314:1298
Weinreich DJ, Burke JF, Pauletto FJ (1984) Left ventricular mural thrombi complicating acute myocardial infarction. Long-term follow-up with serial echocardiography. Ann Intern Med 100:789–794
Banner DW, Hadvary P (1993) Inhibitor binding to thrombin: X-ray crystallographic studies. Adv Exp Med Biol 340:27–33
Hauptmann J, Sturzebecher J (1999) Synthetic inhibitors of thrombin and factor Xa: from bench to bedside. Thromb Res 93:203–241
Xiao Z, Theroux P (1998) Platelet activation with unfractionated heparin at therapeutic concentrations and comparisons with a low-molecular-weight heparin and with a direct thrombin inhibitor. Circulation 97:251–256
Sarich TC, Wolzt M, Eriksson UG et al (2003) Effects of ximelagatran, an oral direct thrombin inhibitor, r-hirudin and enoxaparin on thrombin generation and platelet activation in healthy male subjects. J Am Coll Cardiol 41:557–564
Conflict of interest
The authors declare that they have no conflict interests.
Author information
Authors and Affiliations
Corresponding author
Additional information
Written informed consent was obtained from the patient for publication of this Case report and any accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of this journal.
Rights and permissions
About this article
Cite this article
Vidal, A., Vanerio, G. Dabigatran and left atrial appendage thrombus. J Thromb Thrombolysis 34, 545–547 (2012). https://doi.org/10.1007/s11239-012-0747-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11239-012-0747-1