Abstract
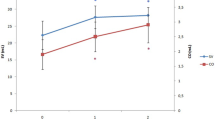
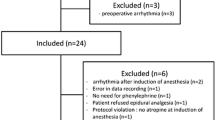
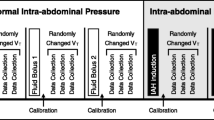
Pulse pressure variation (PPV) and stroke volume variation (SVV) during mechanical ventilation have been shown to be effective parameters to predict preload responsiveness. Although induced hypertension decreases PPV and SVV, the influences of different vasopressors on PPV and SVV are unknown. 94 patients undergoing elective otologic surgery were randomly divided into three groups: Group P (patients were given phenylephrine), Group D (patients were given dopamine), Group E (patients were given ephedrine). When surgery was ongoing and the circulation state was stable, patients were given the vasopressor to increase the systolic arterial pressure (SAP) to the pre-calculated levels: low level, 10 % < ΔSAP ≤ 20 %; medium level, 20 % < ΔSAP ≤ 30 %; high level, 30 % < ΔSAP ≤ 40 %. When invasive arterial pressure reached the target value, PPV, SVV and other parameters were recorded. Dopamine decreased the PPV and SVV more significantly than ephedrine, but less significantly than phenylephrine. The influences of phenylephrine, dopamine and ephedrine on SVV and PPV are different due to their different pharmacological mechanisms.
Similar content being viewed by others
References
Michard F. Changes in arterial pressure during mechanical ventilation. Anesthesiology. 2005;103:419–28.
Dunki-Jacobs EM, Philips P, Scoqqins CR, McMasters KM, Martin RC 2nd. Stroke volume variation in hepatic resection: a replacement for standard central venous pressure monitoring. Ann Surg Oncol. 2014;21:473–8.
Kramer A, Zygun D, Hawes H, Easton P, Ferland A. Pulse pressure variation predicts fluid responsiveness following coronary artery bypass surgery. Chest. 2004;126:1563–8.
Renner J, Cavus E, Meybohm P, Tonner P, Steinfath M, Scholz J, Lutter G, Bein B. Stroke volume variation during hemorrhage and after fluid loading: impact of different tidal volumes. Acta Anaesthesiol Scand. 2007;51(5):538–44.
Kim HK, Pinsky MR. Effect of tidal volume, sampling duration, and cardiac contractility on pulse pressure and stroke volume variation during positive-pressure ventilation. Crit Care Med. 2008;36(10):2858–62.
Suehiro K, Okutani R. Influence of tidal volume for stroke volume variation to predict fluid responsiveness in patients undergoing one-lung ventilation. Jpn Soc Anesthesiol. 2011;25(5):777–80.
Biais M, Nouette-Gaulain K, Cottenceau V, Revel P, Sztark F. Uncalibrated pulse contour-derived stroke volume variation predicts fluid responsiveness in mechanically ventilated patients undergoing liver transplantation. Br J Anaesth. 2008;101:761–8.
Jacques D, Bendjelid K, Duperret S, Colling J, Piriou V, Viale JP. Pulse pressure variation and stroke volume variation during increased intra-abdominal pressure: an experimental study. Crit Care. 2011;15:R33.
Chin JH, Lee EH, Hwang GS, Choi WJ. Prediction of fluid responsiveness using dynamic preload indices in patients undergoing robot-assisted surgery with pneumoperitoneum in the Trendelenburg position. Anaesth Intensive Care. 2013;41(5):515–22.
Darlong V, Kunhabdulla NP, Pandey R, Chandralekha Puni J, Garq R, Kumar R. Hemodynamic changes during robotic radical prostatectomy. Saudi J Anaesth. 2012;6(3):213–8.
Hadian M, Severyn DA, Pinsky MR. The effects of vasoactive drugs on pulse pressure and stroke volume variation in postoperative ventilated patients. J Crit Care. 2011;26(3):328.e1–8.
Wajima Z, Shiga T, Imanaga K, Inoue T. Do induced hypertension and hypotension affect stroke volume variation in man. J Clin Anesth. 2012;24(3):207–11.
Pinsky MR. Instantaneous venous return curves in an intact canine preparation. J Appl Physiol. 1984;56:765–71.
Michard F, Chemla D, Richard C, et al. Clinical use of respiratory changes in arterial pulse pressure to monitor the hemodynamic effects of PEEP. Am J Respir Crit Care Med. 1999;159:935–9.
Reuter DA, Bayerlein J, Goepfert MSG, et al. Influence of tidal volume on left ventricular stroke volume variation measured by pulse contour analysis in mechanically ventilated patients. Intensive Care Med. 2003;29:476–80.
Thiele RH, Nemergut EC, Lynch C 3rd. The physiologic implications of isolated alpha(1) adrenergic stimulation. Anesth Analg. 2011;113:284–96.
Thiele RH, Nemergut EC, Lynch C 3rd. The clinical implications of isolated alpha(1) adrenergic stimulation. Anesth Analg. 2011;113:297–304.
Butterworth J. Do alpha agonist increase venous return? Anesthesiology 2004; 101:1038. Author reply 1039.
Simon AC, Levenson JA, Levy BY, Bouthier JE, Peronneau PP, Safar ME. Effect of nitroglycerin on peripheral large arteries in hypertension. Br J Clin Pharmacol. 1982;14:241–6.
Toraman F, Karabulut H, Goksel O, Evrenkaya S, Tarcan S, Alhan C. Comparison of antihypertensives after coronary artery surgery. Asian Cardiovasc Thorac Ann. 2005;13:302–6.
Pinsky MR. The dynamic interface between hemodynamic variables and autonomic tone. Crit Care Med. 2005;33:2437–8.
Acknowledgments
First of all, I would like to extend my sincere gratitude to my supervisor, Wei-dong Mi, for his instructive advice and useful suggestions on my thesis. I am deeply grateful of his help in the completion of this thesis. High tribute shall be paid to Ms. Bin Zhao, whose profound knowledge of English triggers my love for this beautiful language and whose earnest attitude tells me how to learn English. I am also deeply indebted to all the other tutors and teachers in Department of Anesthesiology of People’s Liberation Army General Hospital for their direct and indirect help to me.
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kong, R., Liu, Y., Mi, W. et al. Influences of different vasopressors on stroke volume variation and pulse pressure variation. J Clin Monit Comput 30, 81–86 (2016). https://doi.org/10.1007/s10877-015-9687-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10877-015-9687-6