Abstract
Background
The recurrence rates of atrial fibrillation (Af) after ablation are still high, and repeat procedures are required in these patients. The main reason for Af recurrence is the recovery of the conduction between the pulmonary veins and left atrium. The importance of catheter stability during the pulmonary vein isolation (PVI) is not well studied.
Purpose
The purpose of this study was to evaluate the contact force (CF), stable ablation time, and power during conduction blocking lesion formation for PVI.
Methods
Thirty-two consecutive drug-refractory Af patients who underwent an initial PVI using CARTO 3 and Visitag were included. The CF, ablation time, force time integral (FTI), and ablation power were recorded by Visitag. Residual conduction gap points requiring touch-up ablation after an encircling linear ablation (R point), spontaneous reconnection points (S point), and dormant conduction points (D point) were considered as non-conduction blocking lesion points. Each ablation parameter for the non-conduction blocking lesion points was compared with the other lesion points.
Results
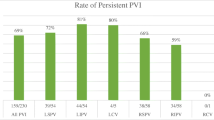
Twenty-one points in 16 patients were considered non-conduction blocking lesions. Ten were R, eight were S, and three were D points. The CF, ablation time, FTI, and power at the non-conduction blocking lesion points and other points were 12.0 g (7.0–21.5) and 12.0 g (9.0–16.0) (P = 0.9), 7.7 s (5.6–10.1) and 12.5 s (9.4–16.8) (P < 0.05), 103.0 g*s (62.0–174.5) and 149.0 g*s (104.0–213.0) (P < 0.05), and 30.0 W (22.5–30.0) and 30.0 W (30.0–30.0) (P = 0.06), respectively.
Conclusions
Shorter ablation time recorded in Visitag lead to non-conduction blocking lesion.





Similar content being viewed by others
Abbreviations
- PV:
-
Pulmonary vein
- Af:
-
Atrial fibrillation
- PVI:
-
Pulmonary vein isolation
- CF:
-
Contact force
- FTI:
-
Force time integral
References
Haissaguerre, M., Jais, P., Shah, D. C., Takahashi, A., Hocini, M., Quiniou, G., et al. (1998). Spontaneous initiation of atrial fibrillation by ectopic beats originating in the pulmonary veins. New England Journal of Medicine, 339(10), 659–666.
Camm, A. J., Lip, G. Y., De Caterina, R., Savelieva, I., Atar, D., Hohnloser, S. H., et al. (2012). 2012 focused update of the ESC Guidelines for the management of atrial fibrillation: an update of the 2010 ESC guidelines for the management of atrial fibrillation—developed with the special contribution of the European Heart Rhythm Association. Europace, 14(10), 1385–1413.
January, C. T., Wann, L. S., Alpert, J. S., Calkins, H., Cigarroa, J. E., Cleveland, J. C., Jr., et al. (2014). 2014 AHA/ACC/HRS guideline for the management of patients with atrial fibrillation: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and the Heart Rhythm Society. Journal of the American College of Cardiology, 64(21), e1–76.
Calkins, H., Kuck, K. H., Cappato, R., Brugada, J., Camm, A. J., Chen, S. A., et al. (2012). 2012 HRS/EHRA/ECAS expert consensus statement on catheter and surgical ablation of atrial fibrillation: recommendations for patient selection, procedural techniques, patient management and follow-up, definitions, endpoints, and research trial design. Journal of Interventional Cardiac Electrophysiology, 33(2), 171–257.
Ouyang, F., Tilz, R., Chun, J., Schmidt, B., Wissner, E., Zerm, T., et al. (2010). Long-term results of catheter ablation in paroxysmal atrial fibrillation: lessons from a 5-year follow-up. Circulation, 122(23), 2368–2377.
Takigawa, M., Takahashi, A., Kuwahara, T., Okubo, K., Takahashi, Y., Watari, Y., et al. (2014). Long-term follow-up after catheter ablation of paroxysmal atrial fibrillation: the incidence of recurrence and progression of atrial fibrillation. Circulation. Arrhythmia and Electrophysiology, 7(2), 267–273.
Cappato, R., Negroni, S., Pecora, D., Bentivegna, S., Lupo, P. P., Carolei, A., et al. (2003). Prospective assessment of late conduction recurrence across radiofrequency lesions producing electrical disconnection at the pulmonary vein ostium in patients with atrial fibrillation. Circulation, 108(13), 1599–1604.
Nanthakumar, K., Plumb, V. J., Epstein, A. E., Veenhuyzen, G. D., Link, D., & Kay, G. N. (2004). Resumption of electrical conduction in previously isolated pulmonary veins: rationale for a different strategy? Circulation, 109(10), 1226–1229.
Ouyang, F., Antz, M., Ernst, S., Hachiya, H., Mavrakis, H., Deger, F. T., et al. (2005). Recovered pulmonary vein conduction as a dominant factor for recurrent atrial tachyarrhythmias after complete circular isolation of the pulmonary veins: lessons from double Lasso technique. Circulation, 111(2), 127–135.
Verma, A., Kilicaslan, F., Pisano, E., Marrouche, N. F., Fanelli, R., Brachmann, J., et al. (2005). Response of atrial fibrillation to pulmonary vein antrum isolation is directly related to resumption and delay of pulmonary vein conduction. Circulation, 112(5), 627–635.
Kowalski, M., Grimes, M. M., Perez, F. J., Kenigsberg, D. N., Koneru, J., Kasirajan, V., et al. (2012). Histopathologic characterization of chronic radiofrequency ablation lesions for pulmonary vein isolation. Journal of the American College of Cardiology, 59(10), 930–938.
Yokoyama, K., Nakagawa, H., Shah, D. C., Lambert, H., Leo, G., Aeby, N., et al. (2008). Novel contact force sensor incorporated in irrigated radiofrequency ablation catheter predicts lesion size and incidence of steam pop and thrombus. Circulation. Arrhythmia and Electrophysiology, 1(5), 354–362.
Reddy, V. Y., Shah, D., Kautzner, J., Schmidt, B., Saoudi, N., Herrera, C., et al. (2012). The relationship between contact force and clinical outcome during radiofrequency catheter ablation of atrial fibrillation in the TOCCATA study. Heart Rhythm, 9(11), 1789–1795.
Neuzil, P., Reddy, V. Y., Kautzner, J., Petru, J., Wichterle, D., Shah, D., et al. (2013). Electrical reconnection after pulmonary vein isolation is contingent on contact force during initial treatment: results from the EFFICAS I study. Circulation. Arrhythmia and Electrophysiology, 6(2), 327–333.
Kimura, M., Sasaki, S., Owada, S., Horiuchi, D., Sasaki, K., Itoh, T., et al. (2014). Comparison of lesion formation between contact force-guided and non-guided circumferential pulmonary vein isolation: a prospective, randomized study. Heart Rhythm, 11(6), 984–991.
Natale, A., Reddy, V. Y., Monir, G., Wilber, D. J., Lindsay, B. D., McElderry, H. T., et al. (2014). Paroxysmal AF catheter ablation with a contact force sensing catheter: results of the prospective, multicenter SMART-AF trial. Journal of the American College of Cardiology, 64(7), 647–656.
Wutzler, A., Huemer, M., Parwani, A. S., Blaschke, F., Haverkamp, W., & Boldt, L. H. (2014). Contact force mapping during catheter ablation for atrial fibrillation: procedural data and one-year follow-up. Archives Medical Science, 10(2), 266–272.
le Polain de Waroux, J. B., Weerasooriya, R., Anvardeen, K., Barbraud, C., Marchandise, S., De Meester, C., et al. (2015). Low contact force and force-time integral predict early recovery and dormant conduction revealed by adenosine after pulmonary vein isolation. Europace.
Park, C. I., Lehrmann, H., Keyl, C., Weber, R., Schiebeling, J., Allgeier, J., et al. (2014). Mechanisms of pulmonary vein reconnection after radiofrequency ablation of atrial fibrillation: the deterministic role of contact force and interlesion distance. Journal of Cardiovascular Electrophysiology, 25(7), 701–708.
Makimoto, H., Tilz, R. R., Lin, T., Rillig, A., Mathew, S., Deiss, S., et al. (2014). Incidence and anatomical locations of catheter instability during circumferential pulmonary vein isolation using contact force. International Heart Journal, 55(3), 249–255.
Takigawa, M., Yamada, T., Yoshida, Y., Ishikawa, K., Aoyama, Y., Yamamoto, T., et al. (2014). Patterns of pulmonary vein potential disappearance during encircling ipsilateral pulmonary vein isolation can predict recurrence of atrial fibrillation. Circulation Journal, 78(3), 601–609.
Takigawa, M., Kuwahara, T., Takahashi, A., Okubo, K., Takahashi, Y., Nakashima, E., et al. (2015). Simultaneous isolation of superior and inferior pulmonary veins on both the left and right sides could yield better outcomes in patients with paroxysmal atrial fibrillation. Europace, 17(5), 732–740.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Fujiwara, R., Imamura, K., Kijima, Y. et al. The importance of catheter stability evaluated by VisitagTM during pulmonary vein isolation. J Interv Card Electrophysiol 46, 161–166 (2016). https://doi.org/10.1007/s10840-016-0103-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-016-0103-z