Abstract
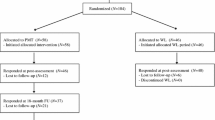
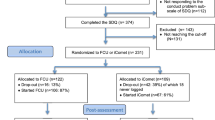
This study evaluated two Internet-based versions of Parent Management Training (PMT) and the effects of greatly reducing the contact required of a mental health professional on treatment of children referred for conduct problems. We were interested whether reduced contact with a therapist influenced treatment outcome, therapeutic alliance, parent adherence to treatment prescriptions, and parent reactions to and evaluations of the treatment procedures. Sixty children and their caregivers were assigned to receive either Full Contact PMT (with the amount of weekly contact similar to traditional PMT; approximately 50 min of direct therapist contact each week) or Reduced Contact PMT (with most information provided through recordings; approximately 10 min of direct therapist contact each week). Children in both groups showed significant and similar reductions in antisocial behaviors specifically, internalizing and externalizing symptoms more generally, and improvements in overall adaptive functioning. Therapeutic alliance also was similar across the two treatment groups. However, parents rated Full Contact treatment as more acceptable than the reduced version. Both treatments were similar in outcomes to in-person treatment as evaluated by a nonrandomized matched sample used as a benchmark in supplementary analyses. Overall, the findings indicate that therapist contact can be reduced while positive treatment outcomes are maintained but that interventions that reduce direct time with a therapist may be viewed less positively by clients.

Similar content being viewed by others
References
Abidin, R.R. (1990). Parenting Stress Index (PSI). Charlottesville, VA: Pediatric Psychology Press.
Achenbach, T. M. (1991). Child behavior checklist/4-18. Burlington: University of Vermont.
American Psychiatric Association. (2000). Diagnostic and statistical manual of mental Disorders (4th ed.). Washington: American Psychiatric association.
Andersson, G., Bergström, J., Carlbring, P., & Lindefors, N. (2005). The use of the Internet in the treatment of anxiety disorders. Current Opinion in Psychiatry, 18, 73–77.
Andrews, G., Cuijpers, P., Craske, M. G., McEvoy, P., & Titov, N. (2010). Computer therapy for the anxiety and depressive disorders is effective, acceptable and practical health care: A meta-analysis. PLoS One, 5(10), e13196.
Ankuta, G. Y., & Abeles, N. (1993). Client satisfaction, clinical significance, and meaningful change in psychotherapy. Professional Psychology: Research and Practice, 24, 70–74.
Beck, A. T., Steer, R. A., & Brown, G. K. (1996). Beck depression inventory-II. San Antonio: Psychological Corporation.
Bennett-Levy, J., Richards, D., Farrand, P., Christensen, H., & Griffiths, K. (Eds.). (2010). Oxford guide to low intensity CBT interventions. Oxford: Oxford University Press.
Bird, H. R., Canino, G., Rubio-Stipec, M., & Ribera, J. C. (1987). Further measures of the psychometric properties of the children’s global assessment scale. Archives of General Psychiatry, 44, 821–824.
Bird, H. R., Yager, T. J., Staghezza, B., Gould, M. S., Canino, G., & Rubio-Stipec, M. (1990). Impairment in the epidemiological measurement of childhood psychopathology in the community. Journal of the American Academy of Child and Adolescent Psychiatry, 29, 796–803.
Bouchard, S., Payeur, R., Rivard, V., Allard, M., Paquin, B., & Renaud, P. (2000). Cognitive behavior therapy for panic disorder with agoraphobia in videoconference: Preliminary results. CyberPsychology & Behavior, 3, 999–1007.
Carlbring, P., & Andersson, G. (2006). Internet and psychological treatment. How well can they be combined? Computers in Human Behavior, 22, 545–553.
Carroll, K. M., Kiluk, B. D., Nich, C., Gordon, M. A., Portnoy, G. A., Marino, D. R., et al. (2014). Computer-assisted delivery of cognitive-behavioral therapy: Efficacy and durability of CBT4CBT among cocaine-dependent individuals maintained on methadone. American Journal of Psychiatry, 171, 436–444.
Carter, S. L. (2007). Review of recent treatment acceptability research. Education and Training in Developmental Disabilities, 42, 301–316.
Chen, L. Y., Crum, R. M., Martins, S. S., Kaufmann, C. N., Strain, E. C., & Mojtabai, R. (2013). Service use and barriers to mental health care among adults with major depression and comorbid substance dependence. Psychiatric Services, 64, 863–870.
Comer, J. S., Furr, J. M., Cooper-Vince, C., Madigan, R. J., Chow, C., Chan, P. T., et al. (2015). Rationale and considerations for the Internet-based delivery of parent-child interaction therapy. Cognitive and Behavioral Practice, 22, 302–316.
Cuijpers, P., Donker, T., van Straten, A., Li, J., & Andersson, G. (2010). Is guided self-help as effective as face-to-face psychotherapy for depression and anxiety disorders? A systematic review and meta-analysis of comparative outcome studies. Psychological Medicine, 40, 1943–1957.
Donker, T., Petrie, K., Proudfoot, J., Clarke, J., Birch, M. R., & Christensen, H. (2013). Smartphones for smarter delivery of mental health programs: A systematic review. Journal of Medical Internet Research, 15(11), e247.
Dozois, D., Dobson, K. S., & Ahnberg, J. L. (1998). A psychometric evaluation of the beck depression inventory–II. Psychological Assessment, 10, 83–89.
Enebrink, P., Högström, J., Forster, M., & Ghaderi, A. (2012). Internet-based parent management training: A randomized controlled study. Behaviour Research and Therapy, 50, 240–249.
Hersen, M. (Ed.). (2005). Encyclopedia of behavior modification and cognitive behavior therapy. Adult clinical applications (Vol. 1). Thousand Oaks: Sage Publications.
Hill, J., & Maughan, B. (2001). Conduct disorders in childhood and adolescence. Cambridge: Cambridge University Press.
Horvath, A. O., & Bedi, R. P. (2002). The alliance. In J. C. Norcross (Ed.), Psychotherapy relationships that work: Therapist contributions and responsiveness to patients (pp. 37–69). New York: Oxford University Press.
Horvath, A. O., & Greenberg, L. S. (1989). Development and validation of the working alliance inventory. Journal of Counseling Psychology, 36, 223–233.
Horvath, A. O., Del Re, A. C., Flückiger, C., & Symonds, D. (2011). Alliance in individual psychotherapy. Psychotherapy, 48, 9–16.
Kazdin, A. E. (2000). Perceived barriers to treatment participation and treatment acceptability among antisocial children and their families. Journal of Child and Family Studies, 9, 157–174.
Kazdin, A. E. (2001). Almost clinically significant (p < .10): Current measures may only approach clinical significance. Clinical Psychology: Science and Practice, 8, 455–462.
Kazdin, A. E. (2005). Parent management training: Treatment for oppositional, aggressive, and antisocial behavior in children and adolescents. New York: Oxford University Press.
Kazdin, A. E. (2010). Problem-solving skills training and parent management training for oppositional defiant disorder and conduct disorder. In J. R. Weisz & A. E. Kazdin (Eds.), Evidence-based psychotherapies for children and adolescents (2nd ed., pp. 211–226). New York: Guilford Press.
Kazdin, A. E. (2015a). Technology-based interventions and reducing the burdens of mental illness: Perspectives and comments on the special series. Cognitive and Behavioral Practice, 22, 359–366.
Kazdin, A. E. (2015b). Psychosocial treatments for conduct disorder in children and adolescents. In P. E. Nathan & J. M. Gorman (Eds.), A guide to treatments that work (4th ed., pp. 71–104). New York: Oxford University Press.
Kazdin, A. E., & Blase, S. L. (2011). Rebooting psychotherapy research and practice to reduce the burden of mental illness. Perspectives on Psychological Science, 6, 21–37.
Kazdin, A. E., & Durbin, K. A. (2012). Predictors of child-therapist alliance in cognitive-behavioral treatment of children referred for oppositional and antisocial behavior. Psychotherapy, 49, 202–217.
Kazdin, A. E., & Esveldt-Dawson, K. (1986). The interview for antisocial behavior: Psychometric characteristics and concurrent validity with child psychiatric inpatients. Journal of Psychopathology and Behavioral Assessment, 8, 289–303.
Kazdin, A. E., & Rabbitt, S. M. (2013). Novel models for delivering mental health services and reducing the burdens of mental illness. Clinical Psychological Science, 1, 170–191.
Kazdin, A. E., & Whitley, M. K. (2003). Treatment of parental stress to enhance therapeutic change among children referred for aggressive and antisocial behavior. Journal of Consulting and Clinical Psychology, 71, 504–515.
Kazdin, A. E., & Whitley, M. K. (2006a). Comorbidity, case complexity, and effects of evidence-based treatment for children referred for disruptive behavior. Journal of Consulting and Clinical Psychology, 74, 455–467.
Kazdin, A. E., & Whitley, M. K. (2006b). Pretreatment social relations, therapeutic alliance, and improvements in parenting practices in parent management training. Journal of Consulting and Clinical Psychology, 74, 346–355.
Kazdin, A. E., French, N. H., & Sherick, R. B. (1981). Acceptability of alternative treatments for children: Evaluations by inpatient children, parents, and staff. Journal of Consulting and Clinical Psychology, 49, 900–907.
Kazdin, A. E., Siegel, T. C., & Bass, D. (1992). Cognitive problem-solving skills training and parent management training in the treatment of antisocial behavior in children. Journal of Consulting and Clinical Psychology, 60, 733–747.
Kazdin, A. E., Holland, L., & Crowley, M. (1997a). Family experience of barriers to treatment and premature termination from child therapy. Journal of Consulting and Clinical Psychology, 65, 453–463.
Kazdin, A. E., Holland, L., Crowley, M., & Breton, S. (1997b). Barriers to participation in treatment scale: Evaluation and validation in the context of child outpatient treatment. Journal of Child Psychology and Psychiatry, 38, 1051–1062.
Kazdin, A. E., Marciano, P. L., & Whitley, M. (2005). The therapeutic alliance in cognitive-behavioral treatment of children referred for oppositional, aggressive, and antisocial behavior. Journal of Consulting and Clinical Psychology, 73, 726–730.
Kazdin, A. E., Whitley, M., & Marciano, P. L. (2006). Child-therapist and parent-therapist alliance and therapeutic change in the treatment of children referred for oppositional, aggressive, and antisocial behavior. Journal of Child Psychology and Psychiatry, 47, 436–445.
Kessler, R. C., & Wang, P. S. (2008). The descriptive epidemiology of commonly occurring mental disorders in the United States. Annual Review of Public Health, 29, 115–129.
Kessler, R. C., Demler, O., Frank, R. G., Olfson, M., Pincus, H. A., Walters, E. E., et al. (2005). Prevalence and treatment of mental disorders, 1990 to 2003. New England Journal of Medicine, 352, 2515–2523.
Lambert, M. J., & Ogles, B. M. (2014). Common factors: Post hoc explanation or empirically based therapy approach? Psychotherapy, 51, 500–504.
Lambert, W., Salzer, M. S., & Bickman, L. (1998). Clinical outcome, consumer satisfaction, and ad hoc ratings of improvement in children’s mental health. Journal of Consulting and Clinical Psychology, 66, 270–279.
Ljotsson, B., Lundin, C., Mitsell, K., Carlbring, P., Ramklint, M., & Ghaderi, A. (2007). Remote treatment of bulimia nervosa and binge eating disorder: A randomized trial of Internet-assisted cognitive behavioural therapy. Behaviour Research and Therapy, 45, 649–661.
Lloyd, B. H., & Abidin, R. R. (1985). Revision of the parenting stress index. Journal of Pediatric Psychology, 10, 169–177.
Miranda, J., Bernal, G., Lau, A. S., Kohn, L., Hwang, W. C., & LaFromboise, T. (2005). State of the science on psychosocial interventions for ethnic minorities. Annual Review of Clinical Psychology, 1, 113–142.
Mojtabai, R., Olfson, M., Sampson, N. A., Jin, R., Druss, B., Wang, P. S., et al. (2011). Barriers to mental health treatment: Results from the national comorbidity survey replication. Psychological Medicine, 41(08), 1751–1761.
Moos, R. H. (1990). Conceptual and empirical approaches to developing family-based assessment procedures: Resolving the case of the family environment scale. Family Process, 29, 199–208.
Moos, R. H., & Moos, B. S. (1981). Family environment scale manual. Palo Alto: Consulting Psychologists Press.
Nock, M. K., Kazdin, A. E., Hiripi, E., & Kessler, R. C. (2007). Lifetime prevalence, correlates, and persistence of oppositional defiant disorder: Results from the national comorbidity survey replication. Journal of Child Psychology and Psychiatry, 48, 703–713.
Norcross, J. C. (Ed.). (2011). Psychotherapy relationships that work: Evidence-based responsiveness (2nd ed.). New York: Oxford University Press.
Norcross, J. C., & Wampold, B. E. (2011). Evidence-based therapy relationships: Research conclusions and clinical practices. Psychotherapy, 48, 98–102.
Perepletchikova, F., & Kazdin, A. E. (2004). Assessment of parenting practices related to conduct problems: Development and validation of the management of children’s behavior scale. Journal of Child and Family Studies, 13, 385–403.
Rabbitt, S. M., Kazdin, A. E., & Scassellati, B. (2015). Integrating socially assistive robotics into mental healthcare interventions: applications and recommendations for expanded use. Clinical Psychology Review, 35, 35–46.
Reimers, T. M., Wacker, D. P., Cooper, L. J., & DeRaad, A. O. (1992). Clinical evaluation of the variables associated with treatment acceptability and their relation to compliance. Behavioral Disorders, 18, 67–76.
Sanders, M. R., Baker, S., & Turner, K. M. (2012). A randomized controlled trial evaluating the efficacy of Triple P online with parents of children with early-onset conduct problems. Behaviour Research and Therapy, 50, 675–684.
Sanford, M. N., Offord, D. R., Boyle, M. H., Peace, A., & Racine, Y. A. (1992). Ontario child health study: Social and school impairments in children aged 6 to 16 years. Journal of the American Academy of Child and Adolescent Psychiatry, 31, 60–67.
Shaffer, D., Gould, M. S., Brasic, J., Ambrosini, P., Fisher, P., Bird, H., et al. (1983). A children’s global assessment scale (CGAS). Archives of General Psychiatry, 40, 1228–1231.
Wampold, B. E., & Imel, Z. E. (2015). The great psychotherapy debate: The evidence for what makes psychotherapy work. New York: Routledge.
Weisz, J. R., & Kazdin, A. E. (Eds.). (2010). Evidence-based psychotherapies for children and adolescents (2nd ed.). New York: Guilford Press.
Acknowledgments
This study was funded by a grant from the National Institute of Mental Health (NIMH) to the last author (Grant Number: 1R34MH093326-01A1).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All study procedures involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Rabbitt, S.M., Carrubba, E., Lecza, B. et al. Reducing Therapist Contact in Parenting Programs: Evaluation of Internet-Based Treatments for Child Conduct Problems. J Child Fam Stud 25, 2001–2020 (2016). https://doi.org/10.1007/s10826-016-0363-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10826-016-0363-3