Abstract
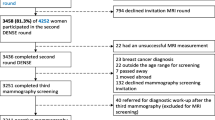
Pilot study to evaluate whether the use of a standardized questionnaire to document family history of cancer improves identification of women who warrant referral to cancer genetic services (CGS) for increased risk of hereditary cancer, compared to their identification in usual care. Prospective intervention study with historic control group. Gynecology outpatient clinic, Maastricht University Medical Centre, the Netherlands. The prospective intervention group consisted of new outpatients between June 1 and August 1, 2011. The historic control group consisted of new outpatients between May 1, 2009 and April 30, 2010. A standardized questionnaire based on established referral criteria for hereditary breast/ovarian cancer and Lynch syndrome was completed for the intervention group. The referral rate in routine consultation, based on non-standardized family history recording, was determined retrospectively for the control group. The difference in referral rate between intervention and control group, tested by Chi square test. In the control group, 8 of 3,036 women (0.26 %) were referred to CGS. In the intervention group, 209 (42 %) of 500 screening questionnaires were completed. Nineteen women (9, 1 %) met the referral guidelines, of which 5 were newly referred to CGS (2, 4 %). Referral rates differed significantly (p < 0.001) between the two groups. This pilot study shows that the routine use of a screening questionnaire may improve detection and referral rate to CGS of individuals at risk for hereditary cancer. Improving genetic literacy of physicians and use of web-site questionnaires deserve attention in future studies.

Similar content being viewed by others
Abbreviations
- CGS:
-
Cancer genetic services
References
Lu KH (2008) Hereditary gynecologic cancers: differential diagnosis, surveillance, management and surgical prophylaxis. Fam Cancer 7(1):53–58
Meyer LA, Broaddus RR, Lu KH (2009) Endometrial cancer and lynch syndrome: clinical and pathologic considerations. Cancer Control 16(1):14–22
Lancaster JM, Powell CB, Kauff ND, Cass I, Chen LM, Lu KH, Mutch DG, Berchuck A, Karlan BY, Herzog TJ (2007) Society of Gynecologic Oncologists Education Committee statement on risk assessment for inherited gynecologic cancer predispositions. Gynecol Oncol 107(2):159–162
Dinh TA, Rosner BI, Atwood JC, Boland CR, Syngal S, Vasen HF, Gruber SB, Burt RW (2011) Health benefits and cost-effectiveness of primary genetic screening for lynch syndrome in the general population. Cancer Prev Res (Phila) 4(1):9–22
Teng I, Spigelman A (2013) Attitudes and knowledge of medical practitioners to hereditary cancer clinics and cancer genetic testing. Fam Cancer. doi:10.1007/s10689-013-9695-y
Marquez-Rodas I, Lopez-Trabada D, Ruperez Blanco AB, Custodio Cabello S, Peligros Gomez MI, Orera Clemente M, Calvo FA, Martin M (2012) Family history record and hereditary cancer risk perception according to national cancer institute criteria in a Spanish medical oncology service: a retrospective study. Oncology 82(1):30–34
Lanceley A, Eagle Z, Ogden G, Gessler S, Razvi K, Ledermann JA, Side L (2012) Family history and women with ovarian cancer: is it asked and does it matter?: an observational study. Int J Gynecol Cancer 22(2):254–259
Grover S, Stoffel EM, Bussone L, Tschoegl E, Syngal S (2004) Physician assessment of family cancer history and referral for genetic evaluation in colorectal cancer patients. Clin Gastroenterol Hepatol 2(9):813–819
Murff HJ, Byrne D, Syngal S (2004) Cancer risk assessment: quality and impact of the family history interview. Am J Prev Med 27(3):239–245
Meyer LA, Anderson ME, Lacour RA, Suri A, Daniels MS, Urbauer DL, Nogueras-Gonzalez GM, Schmeler KM, Gershenson DM, Lu KH (2010) Evaluating women with ovarian cancer for BRCA1 and BRCA2 mutations: missed opportunities. Obstet Gynecol 115(5):945–952
Bellcross CA, Kolor K, Goddard KA, Coates RJ, Reyes M, Khoury MJ (2011) Awareness and utilization of BRCA1/2 testing among U.S. primary care physicians. Am J Prev Med 40(1):61–66
Reid GT, Walter FM, Brisbane JM, Emery JD (2009) Family history questionnaires designed for clinical use: a systematic review. Public Health Genomics 12(2):73–83
Family Medical History in Disease Prevention (2004) American Medical Association. http://www.ama-assn.org/resources/doc/genetics/family_history02.pdf
Scheuner MT, McNeel TS, Freedman AN (2010) Population prevalence of familial cancer and common hereditary cancer syndromes. The 2005 California health interview survey. Genet Med 12(11):726–735
Wallace E, Hinds A, Campbell H, Mackay J, Cetnarskyj R, Porteous ME (2004) A cross-sectional survey to estimate the prevalence of family history of colorectal, breast and ovarian cancer in a Scottish general practice population. Br J Cancer 91(8):1575–1579
Hughes KS, Roche C, Campbell CT, Siegel N, Salisbury L, Chekos A, Katz MS, Edell E (2003) Prevalence of family history of breast and ovarian cancer in a single primary care practice using a self-administered questionnaire. Breast J 9(1):19–25
Ziogas A, Horick NK, Kinney AY, Lowery JT, Domchek SM, Isaacs C, Griffin CA, Moorman PG, Edwards KL, Hill DA, Berg JS, Tomlinson GE, Anton-Culver H, Strong LC, Kasten CH, Finkelstein DM, Plon SE (2011) Clinically relevant changes in family history of cancer over time. JAMA 306(2):172–178
Suther S, Goodson P (2003) Barriers to the provision of genetic services by primary care physicians: a systematic review of the literature. Genet Med 5(2):70–76
Mehnert A, Bergelt C, Koch U (2003) Knowledge and attitudes of gynecologists regarding genetic counseling for hereditary breast and ovarian cancer. Patient Educ Couns 49(2):183–188
Acton RT, Burst NM, Casebeer L, Ferguson SM, Greene P, Laird BL, Leviton L (2000) Knowledge, attitudes, and behaviors of Alabama’s primary care physicians regarding cancer genetics. Acad Med 75(8):850–852
Schlich-Bakker KJ, ten Kroode HF, Ausems MG (2006) A literature review of the psychological impact of genetic testing on breast cancer patients. Patient Educ Couns 62(1):13–20
Vadaparampil ST, Miree CA, Wilson C, Jacobsen PB (2006) Psychosocial and behavioral impact of genetic counseling and testing. Breast Dis 27:97–108
Hopwood P (2005) Psychosocial aspects of risk communication and mutation testing in familial breast-ovarian cancer. Curr Opin Oncol 17(4):340–344
Ackermann S, Lux MP, Fasching PA, Strissl P, Renner SP, Poehls U, Bender HG, Beckmann MW (2006) Acceptance for preventive genetic testing and prophylactic surgery in women with a family history of breast and gynaecological cancers. Eur J Cancer Prev 15(6):474–479
Durfy SJ, Bowen DJ, McTiernan A, Sporleder J, Burke W (1999) Attitudes and interest in genetic testing for breast and ovarian cancer susceptibility in diverse groups of women in western Washington. Cancer Epidemiol Biomarkers Prev 8(4 Pt 2):369–375
Boulos MN, Wheeler S, Tavares C, Jones R (2011) How smartphones are changing the face of mobile and participatory healthcare: an overview, with example from eCAALYX. Biomed Eng Online 10:24
Acknowledgments
None.
Conflict of interest
None declares by all authors.
Ethical standard
As the recording of personal and family history is a fundamental part of the medical history, the study was exempt from Institutional Review Board approval.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Koeneman, M.M., Kruse, AJ., Sep, S.J.S. et al. A family history questionnaire improves detection of women at risk for hereditary gynecologic cancer: a pilot study. Familial Cancer 13, 469–475 (2014). https://doi.org/10.1007/s10689-014-9711-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10689-014-9711-x