Abstract
Objectives
To investigate the duration of remission and low disease activity (LDA) after cessation of tocilizumab (TCZ) treatment in rheumatoid arthritis patients who showed remission or LDA as assessed by DAS28 in response to preceding TCZ monotherapy, and to explore the factors contributing to prolonged efficacy duration.
Methods
Disease activity was monitored for 56 weeks. The rate of continued efficacy was estimated by Kaplan–Meier curves.
Results
A total of 187 patients were eligible. At baseline of this study, median disease duration was 7.8 years, preceding TCZ treatment period was 4.0 years and DAS28 was 1.5. The rate of continued LDA at 52 weeks was 13.4 % according to the Kaplan–Meier estimate. 19 patients (10 %) were completely drug-free and 17 patients (9.1 %) fulfilled DAS28 remission at 52 weeks. Multivariate Cox regression analysis identified low serum IL-6 and normalisation of MMP-3 levels at cessation of TCZ as independent predictive markers for longer duration of LDA. In patients with low serum IL-6 (<12.9 pg/mL) and normal MMP-3 levels, the rate of continued LDA reached 38.0 % at 52 weeks.
Conclusions
TCZ monotherapy may induce biologics-free remission or LDA without concomitant use of synthetic DMARDs. Serum levels of IL-6 and MMP-3 are useful markers for identifying patients who could discontinue TCZ without acute disease flare.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Newly licensed medications, especially biological agents, have enabled the attainment of unprecedented outcomes for patients with rheumatoid arthritis (RA) [1–4], and structured patient management aiming to achieve remission is an achievable goal in many patients in clinical trials and in actual clinical practice [5–8]. However, because biologics are more expensive than conventional synthetic DMARDs, continuous therapy with biologics strains medical finances; the next step in research on the treatment of RA should be to evaluate the possibility of sustaining remission without the use of biologics.
Tocilizumab (TCZ) is a humanised anti-human IL-6 receptor (IL-6R) monoclonal antibody that inhibits IL-6 binding to IL-6R [9]. TCZ as monotherapy and in combination with methotrexate (MTX) has been demonstrated to frequently induce remission according to the 28-joint disease activity score (DAS28)-erythrocyte sedimentation rate (ESR) and also to prevent joint damage [10–20].
In a previous study, we showed that the degree of abnormality of serum IL-6 levels in RA patients was positively correlated with RA disease activity, and that serum IL-6 levels were decreased in patients who sustained DAS28 remission by TCZ monotherapy [21, 22]. This evidence suggests that TCZ may be able to be discontinued without acute flare of disease activity in patients whose serum IL-6 has normalised. Based on this assumption, we planned an open-labelled, single-arm, multicentre clinical trial to investigate Drug-free REmission/low disease activity (LDA) after cessation of tocilizumab (Actemra as a product name) Monotherapy (DREAM study) in RA patients.
Method
Patients
Eligible patients were those who had participated in previous long-term clinical studies of TCZ monotherapy conducted in Japan, and the inclusion criteria and study design for each of these studies have already been reported [23]. Briefly, eligible patients were ≥20 years of age and fulfilled the 1987 American Rheumatism Association criteria for RA[24] with a disease history of 6 months or longer (with the exception of the SAMURAI study [14], in which the eligible disease duration was restricted to between 6 months and 5 years). All subjects failed to respond satisfactorily to treatment with at least one DMARD, including MTX or immunosuppressants. At enrolment in the initial trials, the patients had active RA, defined as the presence of six or more swollen joints and six or more tender joints. Patients receiving corticosteroids (≤10 mg/day as prednisolone equivalent) and/or non-steroidal anti-inflammatory drugs (NSAIDs) were eligible if the dose had not increased during the 1-month washout period. Sexually active premenopausal women were required to have a negative urine pregnancy test at entry and periodically thereafter and to use effective contraception during the study period.
All patients were registered in this study within 4 weeks of the last observation in each preceding long-term extension study of TCZ monotherapy. Patients were enrolled if their DAS28-ESR was <2.6 at two or three of three consecutive assessment points, including the last observation point in the preceding study. Patients with DAS28-ESR ≤3.2 at two or three of three consecutive assessment points were additionally enrolled to know if the disease activity at TCZ discontinuation might influence the duration of DAS28 remission or LDA. Patients were excluded if they had received DMARDs, immunosuppressants, oral corticosteroids in excess of the dose at the initial infusion of TCZ, intravenous or intramuscular injections of corticosteroids, or plasmapheresis before being enrolled in this study. The baseline for each enrolled patient was defined as the time of the last TCZ infusion in the preceding clinical trial.
Study protocol
The study protocol was approved by the Ministry of Health, Labour and Welfare of Japan, and by the local ethical committees. All patients gave their written informed consent. This study is registered with http://clinicaltrials.gov/ (NCT00661284).
The primary endpoint of this study was the rate of DAS28 remission (DAS28-ESR <2.6) or LDA (DAS28-ESR ≤3.2) at 52 weeks after cessation of TCZ monotherapy, which was estimated from Kaplan–Meier curves prepared with the duration of continued efficacy for each patient defined as the time from the last infusion of TCZ in the preceding clinical study until loss of efficacy.
Nineteen hospitals in Japan participated in this study. Disease activities were monitored every 4 weeks for 56 weeks after cessation of TCZ for RA disease activity. During the study period, concomitant uses of NSAIDs and oral corticosteroid were allowed if the doses were not increased. Intra-articular injections of corticosteroids and hyaluronate preparations were avoided as far as possible, but surgical treatments were not limited. Additional RA treatments, including DMARDs, increases in oral corticosteroid dose, intravenous or intramuscular injections of corticosteroids, or plasmapheresis, were not allowed throughout the discontinuation period. Criteria for loss of efficacy was defined as DAS28-ESR >3.2 at two consecutive observations, initiation of additional RA treatments including increase in oral corticosteroid dose, the patient’s request for retreatment, or the treating physician judging that retreatment was necessary. If patients met the criteria for loss of efficacy, observations in the study period were terminated.
Statistical analysis
Patients who had maintained a DAS28-ESR ≤3.2 at the last observation point in this study were handled as censored at that time. DAS28 remission and the 2011 American College of Rheumatology (ACR)/European League Against Rheumatism (EULAR) remission criteria (Boolean approach) were also considered [25].
The rate of continued efficacy at each time point was also estimated from Kaplan–Meier curves. The factors contributing to the duration of efficacy were estimated from univariate and multivariate Cox regression analyses using the following patient background data for this study: age, gender, disease duration, American College of Rheumatology functional class, RA stage determined by Steinbrocker’s criteria, corticosteroid dose, rheumatoid factor (RF), DAS28-ESR, modified health assessment questionnaire (MHAQ) score, serum IL-6 concentration, and serum matrix metalloproteinase (MMP)-3 concentration. The receiver operating characteristic (ROC) curve was used to determine the most sensitive and specific cut-off value for the serum IL-6 level. Ineligible patients were excluded from efficacy evaluations.
Results
Characteristics of patients
We enrolled 189 patients and 187 of them were eligible. The two patients who did not meet DAS28-ESR LDA at the last observation of preceding long-term extension studies were excluded from this study from 189 patients. At the baseline of this study, the median disease duration was 7.8 years and the median preceding TCZ treatment period was 4.0 years (min–max = 1.9–8.6 years). Of the patients, 126 (67.4 %) received TCZ with 8 mg/kg every 4 weeks before enrolling in this study, 45 (24.1 %) extended the treatment interval (39.7 ± 10.9 days, mean ± SD) and 3 reduced the TCZ dosage (2 for 4 mg/kg; 1 for 6 mg/kg every 4 week), mostly due to sufficient efficacy, while 13 patients (7.0 %) shortened the interval (10 for patient’s convenience; 3 for insufficient efficacy).
Oral corticosteroids were being taken by 64 patients (34.2 %), with a mean dose of 2.8 mg/day for those patients; 143 patients (76.5 %) had no swollen joints; 137 patients (73.3 %) had no tender joints; 115 patients (61.5 %) had no swollen and no tender joints. The medina serum IL-6 concentration and serum MMP-3 concentration were also decreased at enrolment in this study compared with the patient background before starting the TCZ treatment (Table 1). At enrolment in this study, 169 (90.4 %) met DAS28 remission, and 107 (57.2 %) met Boolean remission. The DAS28 remission and LDA were kept more than 24 weeks in 133 patients (71.1 %) and 159 patients (85.0 %), respectively, before enrolment into this study.
Continuation rate of DAS28 remission and LDA efficacy after cessation of TCZ treatment
The rate of continued efficacy LDA without concomitant use of synthetic DMARDs was 35.1 % [95 % confidence interval (CI) 28.2–42.0 %] at 24 weeks and 13.4 % (95 % CI 8.4–18.3 %) at 52 weeks according to the Kaplan–Meier estimate (Fig. 1). DAS28 remission and 2011 ACR/EULAR remission criteria (Boolean approach) were maintained in 17 patients (9.1 %) and 14 patients (7.5 %), respectively, at 52 weeks. Furthermore, efficacy continued throughout the study period without concomitant use of corticosteroids or NSAIDs during the study period in 19 patients (10.2 %). The mean DAS28-ESR of these 19 patients was 2.2 at week 52.
When we estimated the LDA continuation rates by the Kaplan–Meier method in the patients with DAS28 remission and new stringent Boolean-based remission at the cessation of TCZ, LDA continuation rates (95 % CI) at 52 weeks were 14.2 % (8.9–19.5 %) and 16.1 % (9.1–23.1 %), respectively. Further analysis for the factors contributing to the prolongation of efficacy duration is described later.
In total, 161 patients were withdrawn from this study. The major reason for the loss of efficacy was DAS28-ESR >3.2 at two consecutive visits in 44.7 % of patients (72/161 patients) and investigator’s judgment in 39.8 % of patients (64/161 patients). The major reason of investigator’s judgement was DAS28-ESR >3.2 at one visit in 84.4 % of patients (54/64 patients). However, there were no patients in whom disease activity flared up at the end of the observational period. Only 6.8 % (11/161 patients) were patients’ request.
In terms of disease activity at cessation of TCZ monotherapy, the patients who completed the 52 weeks of this study period were comparable to the patients who withdrew from the study and restarted anti-rheumatic therapy before 52 weeks (Table 2).The serum IL-6 levels at baseline in the patients who restarted anti-rheumatic therapy before 52 weeks were higher than those in the patients who completed the 52-week study period [19.3 (range 0.7–431.0) pg/mL vs 10.9 (range 0.9–32.6) pg/mL]. In addition, the percentage of patients whose MMP-3 levels were within normal range was lower in the group of patients who restarted anti-rheumatic therapy (56.7 %) than in the group who completed the 52-week study period (91.7 %).
Even though the median DAS28 was slightly increased from 1.0 at baseline of this study to 2.4 at the last observation point of this study (Table 2), tender joint count and swollen joint count at week 52 did not meaningfully worsen from the baseline of this study in the patients who completed the 52-week study period. MMP-3 concentration at week 52 was also almost stable during the study period in these patients.
In the patients who restarted anti-rheumatic therapy, disease activity and MMP-3 levels had worsened compared to the baseline of this study. Nevertheless, the values of those parameters were no worse than they had been before the initiation of TCZ treatment in previous studies (Table 2).
Factors contributing to the prolongation of duration of DAS28 remission and LDA
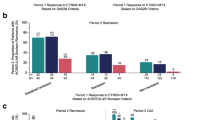
Univariate Cox regression analysis showed the following variables to be associated with the rate of continued efficacy: negative RF at baseline of the previous study and low serum IL-6 level (<35 pg/mL), under upper limit of the normal MMP-3 level, no concomitant corticosteroid use, DAS28-ESR <median, and an MHAQ score of zero at TCZ discontinuation.In contrast, disease duration, gender, functional class, and RA stage were not associated with continued efficacy (Fig. 2a). Multivariate Cox regression analysis showed that low serum IL-6 (<35 pg/mL) and normalisation of MMP-3 levels at TCZ cessation were independently associated with continued efficacy (Fig. 2b).
Factors associated with continued LDA. a Univariate Cox regression analysis, b multivariate Cox regression analysis. HR hazard ratio, CI confidence interval, RF rheumatoid factor, DAS28 28-joint disease activity score, MHAQ modified health assessment questionnaire, IL-6 interleukin 6, MMP-3 matrix metalloproteinase 3
Based on this result, we examined the effects that IL-6 and MMP-3 levels at cessation of TCZ treatment had on the rate of continued efficacy. We found that the rate of continued efficacy in the patients with low serum IL-6 (<35 pg/mL) was 39.3 % (95 % CI 31.1–47.4) at 24 weeks and 15.9 % (95 % CI 9.7–22.0) at 52 weeks (Fig. 3a). In contrast, 69.7 % of the patients with serum IL-6 levels ≥35 pg/mL met the criteria for loss of efficacy within 12 weeks, and in none was efficacy maintained until 52 weeks. Analysis of the ROC curve identified the most sensitive and specific cut-off value for the serum IL-6 level to be 12.9 pg/mL. The rate of continued efficacy in patients whose serum IL-6 levels were less than 12.9 pg/mL was 63.2 % (95 % CI 48.8–77.5) at 24 weeks and 30.2 % (95 % CI 16.4–44.0) at 52 weeks (Fig. 3b).
Effects of serum IL-6 and MMP-3 levels on rate of continued LDA after cessation of tocilizumab treatment estimated by Kaplan–Meier method over 52 weeks. Contributing factors: a serum IL-6 level (cut-off level: 35 pg/mL), b serum IL-6 level (cut-off level: 12.9 pg/mL), c MMP-3 level (normal vs abnormal), d combinations of MMP-3 (normal vs abnormal) and serum IL-6 levels (cut-off level: 12.9 pg/mL). Space between curves represents the contribution of each factor to rate of continued efficacy
The rate of continued efficacy in those with normalised MMP-3 levels was 50.9 % (95 % CI 41.6–60.2) at 24 weeks and 20.3 % (95 % CI 12.8–27.8) at 52 weeks (Fig. 3c), compared with 11.8 % at 24 weeks and 3.0 % at 52 weeks in patients with abnormal MMP-3 levels.
In patients with both serum IL-6 <12.9 pg/mL and normalised MMP-3 level, the rate of continued efficacy reached 70.6 % (95 % CI 55.3–85.9) at 24 weeks and 38.0 % (95 % CI 21.6–54.4) at 52 weeks (Fig. 3d).
Discussion
This study indicated that, in about 13 % of patients who achieve LDA (70.8 % of them were DAS28 remission) during long-term TCZ monotherapy, efficacy can be sustained for 1 year after cessation of TCZ treatment without concomitant use of synthetic DMARDs or immune suppressants; and in 79 % of them (19 patients), efficacy was maintained without concomitant use of corticosteroids or NSAIDs. To the best of our knowledge, this is the first report to show evidence that anti-IL-6 therapy can induce drug-free remission/LDA for 1 year in RA patients. The treatment recommendations of the EULAR state that, in patients who achieve remission with biological products, it may be possible to taper off the biological product after tapering off the corticosteroid. However, at present, evidence in support of this conjecture is insufficient [26]. We believe that this report supports the possibility of discontinuing biological products as per the ACR/EULAR recommendations.
In a previous study (the BeST study), van der Kooij et al. [27] indicated that 18 % of patients could discontinue infliximab and synthetic DMARDs. Even though the characteristics of the patients in our study differed from those in BeSt study, the success rate of discontinuing TCZ without synthetic DMARDs in our study is comparable to that of the BeSt study. Moreover, with the use of synthetic DMARDs including MTX, a high rate of continued efficacy was shown after discontinuation of infliximab in the BeSt study [27]. A similar result was shown in the Japanese RRR study [28]. Therefore, it can be expected that introducing the use of synthetic DMARDs would similarly result in an increased rate of continued DAS28 remission or LDA after cessation of TCZ.
Because multivariate Cox regression analysis identified low serum IL-6 and normalised MMP-3 levels at the start of cessation of TCZ to be factors associated with continued efficacy, it can be considered that these factors may predict continued efficacy of a preceding TCZ treatment. With long-term TCZ treatment, reduced serum IL-6 levels are observed in some patients although TCZ does not directly inhibit IL-6 production but blocks IL-6R. We previously reported that, during blockade of IL-6R by TCZ, the serum IL-6 level represents the true IL-6 production in vivo and correlates well with true disease activity in RA patients [21, 22]. Therefore, TCZ treatment may improve not only inflammation-related symptoms but also the underlying cause of RA in patients whose serum IL-6 levels decrease. This implies that TCZ could be discontinued without acute disease flare in patients with normalised serum IL-6 levels. IL-6, as such a biomarker, is available only for anti-IL-6R antibody therapy but for anti-IL-6 neutralizing antibody therapies.
MMP-3 is deeply involved in cartilage destruction in RA and is also correlated with disease activity [29]. Since normalisation of the MMP-3 level is thought to reflect inhibition of excessive cartilage and bone destruction in the joints, normalisation of the MMP-3 level may indicate an improvement in the underlying cause of RA as well as synovial inflammation. In this study, we did not examine the progression of joint damage by imaging after cessation of TCZ. However, since the MMP-3 level during the TCZ-free period did not increase in the majority of the patients showing continued efficacy, it can be inferred that there was no sudden progression of joint destruction during the cessation of TCZ treatment. Further study will be necessary to evaluate this question.
In conclusion, these results showed that TCZ monotherapy can induce biologics-free remission/LDA without concomitant use of conventional DMARDs. Serum levels of IL-6 and MMP-3 are useful markers for identifying patients who could possibly discontinue TCZ without acute disease flare. This evidence has also encouraged us to taper and adjust the interval of TCZ treatment in patients who show good response and normalisation of serum IL-6 and MMP-3 levels.
References
Smolen JS, Aletaha D, Koeller M, et al. New therapies for treatment of rheumatoid arthritis. Lancet. 2007;370:1861–74.
Verstappen SM, Jacobs JW, van der Veen MJ, et al. Intensive treatment with methotrexate in early rheumatoid arthritis: aiming for remission. Computer assisted management in early rheumatoid arthritis (CAMERA, an open-label strategy trial). Ann Rheum Dis. 2007;66:1443–9.
Grigor C, Capell H, Stirling A, et al. Effect of a treatment strategy of tight control for rheumatoid arthritis (the TICORA study): a single-blind randomised controlled trial. Lancet. 2004;364:263–9.
Goekoop-Ruiterman YP, de Vries-Bouwstra JK, Allaart CF, et al. Comparison of treatment strategies in early rheumatoid arthritis: a randomized trial. Ann Intern Med. 2007;146:406–15.
Mierau M, Schoels M, Gonda G, et al. Assessing remission in clinical practice. Rheumatology (Oxford). 2007;46:975–9.
Emery P, Breedveld FC, Hall S, et al. Comparison of methotrexate monotherapy with a combination of methotrexate and etanercept in active, early, moderate to severe rheumatoid arthritis (COMET): a randomised, double-blind, parallel treatment trial. Lancet. 2008;372:375–82.
Emery P, Salmon M. Early rheumatoid arthritis: time to aim for remission? Ann Rheum Dis. 1995;54:944–7.
Sokka T, Hetland ML, Mäkinen H, et al. Remission and rheumatoid arthritis: data on patients receiving usual care in twenty four countries. Arthritis Rheum. 2008;58:2642–51.
Sato K, Tsuchiya M, Saldanha J, et al. Reshaping a human antibody to inhibit the interleukin 6-dependent tumor cell growth. Cancer Res. 1993;53:851–6.
Choy EH, Isenberg DA, Garrood T, et al. Therapeutic benefit of blocking interleukin-6 activity with an anti-interleukin 6 receptor monoclonal antibody in rheumatoid arthritis: a randomized, double-blind, placebo-controlled, dose-escalation trial. Arthritis Rheum. 2002;46:3143–50.
Nishimoto N, Yoshizaki K, Maeda K, et al. Toxicity, pharmacokinetics, and dose-finding study of repetitive treatment with the humanized anti-interleukin 6 receptor antibody MRA in rheumatoid arthritis. Phase I/II clinical study. J Rheumatol. 2003;30:1426–35.
Nishimoto N, Yoshizaki K, Miyasaka N, et al. Treatment of rheumatoid arthritis with humanized anti-interleukin-6 receptor antibody: a multicenter, double-blind, placebo-controlled trial. Arthritis Rheum. 2004;50:1761–9.
Maini RN, Taylor PC, Szechinski J, et al. Double-blind randomized controlled clinical trial of the interleukin-6 receptor antagonist, tocilizumab, in European patients with rheumatoid arthritis who had an incomplete response to methotrexate. Arthritis Rheum. 2006;54:2817–29.
Nishimoto N, Hashimoto J, Miyasaka N, et al. Study of active controlled monotherapy used for rheumatoid arthritis, an IL-6 inhibitor (SAMURAI): evidence of clinical and radiographic benefit from an x ray reader-blinded randomised controlled trial of tocilizumab. Ann Rheum Dis. 2007;66:1162–7.
Smolen JS, Beaulieu A, Rubbert-Roth A, et al. Effect of interleukin-6 receptor inhibition with tocilizumab in patients with rheumatoid arthritis (OPTION study): a double-blind, placebo-controlled, randomised trial. Lancet. 2008;371:987–97.
Genovese MC, McKay JD, Nasonov EL, et al. Interleukin-6 receptor inhibition with tocilizumab reduces disease activity in rheumatoid arthritis with inadequate response to disease-modifying antirheumatic drugs: the tocilizumab in combination with traditional disease-modifying antirheumatic drug therapy study. Arthritis Rheum. 2008;58:2968–80.
Emery P, Keystone E, Tony HP, et al. IL-6 receptor inhibition with tocilizumab improves treatment outcomes in patients with rheumatoid arthritis refractory to anti-tumour necrosis factor biologicals: results from a 24-week multicentre randomised placebo-controlled trial. Ann Rheum Dis. 2008;67:1516–23.
Nishimoto N, Miyasaka N, Yamamoto K, et al. Study of active controlled tocilizumab monotherapy for rheumatoid arthritis patients with an inadequate response to methotrexate (SATORI): significant reduction in disease activity and serum vascular endothelial growth factor by IL-6 receptor inhibition therapy. Mod Rheumatol. 2009;19:12–9.
Jones G, Sebba A, Gu J, et al. Comparison of tocilizumab monotherapy versus methotrexate monotherapy in patients with moderate to severe rheumatoid arthritis: the AMBITION study. Ann Rheum Dis. 2010;69:88–96.
Kremer JM, Blanco R, Brzosko M, et al. Tocilizumab inhibits structural joint damage in rheumatoid arthritis patients with inadequate responses to methotrexate: results from the double-blind treatment phase of a randomized placebo-controlled trial of tocilizumab safety and prevention of structural joint damage at one year. Arthritis Rheum. 2011;63:609–21.
Nishimoto N, Miyasaka N, Yamamoto K, et al. Relationship between serum IL-6 levels after tocilizumab treatment and clinical remission in active rheumatoid arthritis (RA) patients (abstract). Ann Rheum Dis. 2008;67(Suppl 2):90.
Nishimoto N, Terao K, Mima T, et al. Mechanisms and pathologic significances in increase in serum interleukin-6 (IL-6) and soluble IL-6 receptor after administration of an anti-IL-6 receptor antibody, tocilizumab, in patients with rheumatoid arthritis and Castleman disease. Blood. 2008;112:3959–64.
Nishimoto N, Ito K, Takagi N. Safety and efficacy profiles of tocilizumab monotherapy in Japanese patients with rheumatoid arthritis: meta-analysis of six initial trials and five long-term extensions. Mod Rheumatol. 2010;20:222–32.
Arnett FC, Edworthy SM, Bloch DA, et al. The American Rheumatism Association 1987 revised criteria for the classification of rheumatoid arthritis. Arthritis Rheum. 1988;31:315–24.
Felson DT, Smolen JS, Wells G, et al. America college of rheumatology/European league against rheumatism provisional definition of remission in rheumatoid arthritis for clinical trials. Ann Rheum Dis. 2011;70:404–13.
Smolen JS, Landewé R, Breedveld FC, et al. EULAR recommendations for the management of rheumatoid arthritis with synthetic and biological disease-modifying antirheumatic drugs. Ann Rheum Dis. 2010;69:964–75.
van der Kooij SM, Goekoop-Ruiterman YP, de Vries-Bouwstra JK, et al. Drug-free remission, functioning and radiographic damage after 4 years of response-driven treatment in patients with recent-onset rheumatoid arthritis. Ann Rheum Dis. 2009;68:914–21.
Tanaka Y, Takeuchi T, Mimori T, et al. Discontinuation of infliximab after attaining low disease activity in patients with rheumatoid arthritis: RRR (remission induction by Remicade in RA) study. Ann Rheum Dis. 2010;69:1286–91.
Ribbens C, Andre B, Jaspar JM, et al. Matrix metalloproteinase-3 serum levels are correlated with disease activity and predict clinical response in rheumatoid arthritis. J Rheumatol. 2000;27:888–93.
Acknowledgments
The authors wish to thank all members of the MRA study group for RA for treating the patients. This study was funded by Chugai Pharmaceutical Co., Ltd.
Conflict of interest
N. Nishimoto has served as a consultant to and received honoraria from Chugai Pharmaceutical Co., Ltd. N.N. also works as a scientific advisor to F. Hoffmann–La Roche, which is developing TCZ in collaboration with Chugai Pharmaceutical Co., Ltd. N.N. also has received research grants from Chugai Pharmaceutical Co. Ltd., Bristol–Myers Japan, and Pfizer Japan Inc. K. Amano has received research grants from Chugai Pharmaceutical Co. Ltd., Astellas Pharm Inc., and Mitsubishi Tanabe Pharma. Y. Hirabayashi has received speakers’ bureau honoraria from Chugai Pharmaceutical Co. Ltd. M. Iwamoto has received a Royalty from Chugai Pharmaceutical Co. Ltd. H. Kohsaka has received research grants, consultant fees, and/or speakers’ bureau honoraria from, Bristol-Myers Japan, Pfizer Japan Inc., and Takeda Pharmaceutical Co. Ltd. T. Mimura received research grants from Abbott Japan, Chugai Pharmaceutical Co. Ltd., Mitsubishi Tanabe Pharma, and Takeda Pharmaceutical Co. Ltd. T. Takeuchi has received research grants, consultant fees, and/or speakers’ bureau honoraria from Abbott Japan, Bristol-Myers Squibb, Chugai Pharmaceutical Co. Ltd., Eisai Co. Ltd., Janssen Pharmaceutical KK, Mitsubishi Tanabe Pharma, Novartis, Pfizer Japan Inc., and Takeda Pharmaceutical Co. Ltd. S. Tohma has received a research grant from Pfizer Japan Inc. and has received subsidies or donations from Health and Labour Sciences Research Grants for Research on Allergic Disease and Immunology, and Chugai Pharmaceutical Co. Ltd. N. Takagi is a full-time employee of Chugai Pharmaceutical Co., Ltd. All other authors have declared no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
For the MRA Study Group for RA.
Rights and permissions
This article is published under an open access license. Please check the 'Copyright Information' section either on this page or in the PDF for details of this license and what re-use is permitted. If your intended use exceeds what is permitted by the license or if you are unable to locate the licence and re-use information, please contact the Rights and Permissions team.
About this article
Cite this article
Nishimoto, N., Amano, K., Hirabayashi, Y. et al. Drug free REmission/low disease activity after cessation of tocilizumab (Actemra) Monotherapy (DREAM) study. Mod Rheumatol (2013). https://doi.org/10.1007/s10165-013-0894-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10165-013-0894-z