Abstract
Background
Wound dehiscence is a known complication following abdominoperineal resection (APR) and can have a negative impact on recovery and outcome. The aim of this study was to determine the predictors of post-APR 30-day abdominal and/or perineal wound dehiscence, readmission, and reoperation, and to assess the impact of wound dehiscence on 30-day mortality.
Methods
All patients undergoing APR between 2005 and 2012 were analyzed using the American College of Surgeons National Surgical Quality Improvement Program.
Results
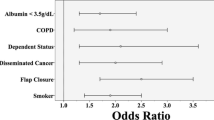
There were 5161 patients [male = 3076 (59.6 %)] with a mean age of 61.9 ± 14.3 years. Mean body mass index was 27.4 ± 6.6 kg/m2. The most common indication for surgery was rectal cancer (79.1 %), followed by inflammatory bowel disease (8.2 %). The overall rate of wound dehiscence was 2.7 % (n = 141). Older age (p = 0.013), baseline dyspnea (p = 0.043), smoking history (p = 0.009), and muscle flap creation (p ≤ 0.001) were independently associated with the risk of dehiscence. No association was observed between omental flap creation and dehiscence risk (p = 0.47). The 30-day readmission rate (15.6 vs. 5.6 %, p ≤ 0.001) and need for reoperation (39 vs. 6.6 %, p ≤ 0.001) were significantly higher in patients who experienced dehiscence. Dehiscence was an independent risk factor for 30-day mortality [OR = 2.69 (1.02–7.08), p = 0.045)].
Conclusions
Older age, baseline dyspnea, smoking, and the use of muscle flap were associated with higher risk of wound dehiscence following APR. Patients with wound dehiscence had a higher rate of readmission and need for reoperation, and an increased risk of 30-day mortality.

Similar content being viewed by others
References
Moore HG, Gittleman AE, Minsky BD et al (2004) Rate of pathologic complete response with increased interval between preoperative combined modality therapy and rectal cancer resection. Dis Colon Rectum 47:279–286
Hawkins AT, Berger DL, Shellito PC, Sylla P, Bordeianou L (2014) Wound dehiscence after abdominoperineal resection for low rectal cancer is associated with decreased survival. Dis Colon Rectum 57:143–150
Christian CK, Kwaan MR, Betensky RA, Breen EM, Zinner MJ, Bleday R (2005) Risk factors for perineal wound complications following abdominoperineal resection. Dis Colon Rectum 48:43–48
Butler CE, Gündeslioglu AÖ, Rodriguez-Bigas MA (2008) Outcomes of immediate vertical rectus abdominis myocutaneous flap reconstruction for irradiated abdominoperineal resection defects. J Am Coll Surg 206:694–703
Artioukh D, Smith R, Gokul K (2007) Risk factors for impaired healing of the perineal wound after abdominoperineal resection of rectum for carcinoma. Colorectal Dis 9:362–367
Khuri SF, Henderson WG, Daley J, Principal Investigators of the Patient Safety in Surgery Study et al (2008) Successful implementation of the department of veterans affairs’ National Surgical Quality Improvement Program in the private sector: the patient safety in surgery study. Ann Surg 248:329–336
Daley J, Forbes MG, Young GJ et al (1997) Validating risk-adjusted surgical outcomes: Site visit assessment of process and structure. J Am Coll Surg 185:341–351
Hinojosa MW, Parikh DA, Menon R, Wirth GA, Stamos MJ, Mills S (2009) Recent experience with abdominal perineal resection with vertical rectus abdominis myocutaneous flap reconstruction after preoperative pelvic radiation. Am Surg 75:995–999
Touny A, Othman H, Maamoon S, Ramzy S, Elmarakby H (2014) Perineal reconstruction using pedicled vertical rectus abdominis myocutaneous flap (VRAM). J Surg Oncol 110:752–757
Di Mauro D, D’Hoore A, Penninckx F, De Wever I, Vergote I, Hierner R (2009) V-Y bilateral gluteus maximus myocutaneous advancement flap in the reconstruction of large perineal defects after resection of pelvic malignancies. Colorectal Dis 11:508–512
Persichetti P, Cogliandro A, Marangi GF et al (2007) Pelvic and perineal reconstruction following abdominoperineal resection: the role of gracilis flap. Ann Plast Surg 59:168–172
Abbott DE, Halverson AL, Wayne JD, Kim JY, Talamonti MS, Dumanian GA (2008) The oblique rectus abdominal myocutaneous flap for complex pelvic wound reconstruction. Dis Colon Rectum 51:1237–1241
Miles WE (1908) A method of performing abdominoperineal excision for carcinoma of the rectum and the terminal portion of the pelvic colon. Lancet 2:1812–1813
Campos FG, Habr-Gama A, Nahas SC, Perez RO (2012) Abdominoperineal excision: evolution of a centenary operation. Dis Colon Rectum 55:844–853
Byrne BE, Mamidanna R, Vincent CA, Faiz O (2013) Population-based cohort study comparing 30- and 90-day institutional mortality rates after colorectal surgery. Br J Surg 13:1810–1817
Mamidanna R, Almoudaris AM, Faiz O (2012) Is 30-day mortality an appropriate measure of risk in elderly patients undergoing elective colorectal resection? Colorectal Dis 14:1175–1182
Damhuis RA, Wijnhoven BP, Plaisier PW, Kirkels WJ, Kranse R, van Lanschot JJ (2012) Comparison of 30-day, 90-day and in-hospital postoperative mortality for eight different cancer types. Br J Surg 99:1149–1154
Bullard KM, Trudel JL, Baxter NN, Rothenberger DA (2005) Primary perineal wound closure after preoperative radiotherapy and abdominoperineal resection has a high incidence of wound failure. Dis Colon Rectum 48:438–443
Choudry U, Harris D (2013) Perineal wound complications, risk factors, and outcome after abdominoperineal resections. Ann Plast Surg 71:209–213
De Broux E, Parc Y, Rondelli F, Dehni N, Tiret E, Parc R (2005) Sutured perineal omentoplasty after abdominoperineal resection for adenocarcinoma of the lower rectum. Dis Colon Rectum 48:476–482
Hay JM, Fingerhut A, Paquet JC, Flamant Y (1997) Management of the pelvic space with or without omentoplasty after abdominoperineal resection for carcinoma of the rectum: a prospective multicenter study. The french association for surgical research. Eur J Surg 163:199–206
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest or financial ties to disclose. American College of Surgeons National Surgical Quality Improvement Program and the hospitals participating in the ACS-NSQIP are the source of the data used herein; they have not verified and are not responsible for the statistical validity of the data analysis or the conclusions derived by the authors.
Ethical approval
Institutional review board approval related to study at the Cleveland Clinic was obtained. As this study contained de-identified nationwide data without any protected health information.
Informed consent
Informed consent is not required.
Rights and permissions
About this article
Cite this article
Rencuzogullari, A., Gorgun, E., Binboga, S. et al. Predictors of wound dehiscence and its impact on mortality after abdominoperineal resection: data from the National Surgical Quality Improvement Program. Tech Coloproctol 20, 475–482 (2016). https://doi.org/10.1007/s10151-016-1486-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10151-016-1486-7