Abstract
Purpose
Although many studies have concluded that prophylactic drain insertion during elective liver resection offers few advantages, we reassessed the clinical value and appropriate management of drain insertion.
Methods
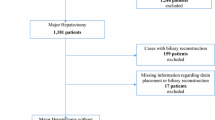
We retrospectively studied the clinical value of abdominal drainage in 167 consecutive patients who underwent hepatectomy, focusing on drainage volumes, bilirubin concentrations, drainage fluid bacterial culture results and short-term postoperative outcomes. The results were then validated prospectively in the next 50 consecutive patients to undergo hepatectomy.
Results
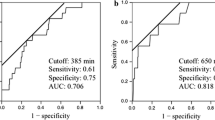
Most of the patients with morbidities such as biliary fistulas, ascites, fluid collection or duodenal perforation (20/24 or 83 %) were treated using operative drainage tubes, avoiding the use of percutaneous drainage procedures. The values obtained with the formula (drainage fluid bilirubin concentration/serum bilirubin concentration) × drainage fluid volume, were greater on both postoperative days (POD) 2 and 3 (P = 0.03 and P < 0.01) in patients with biliary leakage compared with those observed in the patients without leakage. The bacteriologic cultures of drainage fluid were positive less frequently on POD 4 or earlier (7/203) than on POD 5 or later (24/74, P < 0.01). In the validation cohort, new drain removal criteria based on the retrospective results led to successful drain management without additional treatment in 96 % of patients.
Conclusions
Abdominal drainage is effective for both postoperative monitoring and morbidity treatment.


Similar content being viewed by others
Abbreviations
- CT:
-
Computed tomography
- HCC:
-
Hepatocellular carcinoma
- Hx:
-
Hepatectomy
- LDLT:
-
Living donor liver transplant
- MRSE:
-
Methicillin-resistant Staphylococcus epidermidis
- POD:
-
Postoperative day(s)
- PS:
-
Prediction score
- SE:
-
Standard error
- SIRS:
-
Systemic inflammatory response syndrome
References
Duthie HL. Drainage of the abdomen. N Engl J Med. 1972;287:1081–3.
Cerise EJ, Pierce WA, Diamond DL. Abdominal drains: their role as a source of infection following splenectomy. Ann Surg. 1970;171:764–9.
Smith SRG, Gilmore OJA. Surgical drainage. Br J Hosp Med. 1985;33:308–15.
Benjamin PJ. Faeculent peritonitis: a complication of vacuum drainage. Br J Surg. 1980;67:453–4.
Elboim CM, Goldman L, Hann L, Palestrant AM, Silen W. Significance of post-cholecystectomy subhepatic fluid collections. Ann Surg. 1983;198:137–41.
Monson JR, MacFie J, Irving H, Keane FB, Brennan TG, Tanner WA. Influence of intraperitoneal drains on subhepatic collections following cholecystectomy: a prospective clinical trial. Br J Surg. 1986;73:993–4.
Koffi E, Moutardier V, Sauvanet A, Noun R, Fléjou JF, Belghiti J. Wound recurrence after resection of hepatocellular carcinoma. Liver Transpl Surg. 1996;2:301–3.
Trowbridge PE. A randomized study of cholecystectomy with and without drainage. Surg Gynecol Obstet. 1982;155:171–6.
Hoffmann J, Lorentzen M. Drainage after cholecystectomy. Br J Surg. 1985;72:423–7.
Belghiti J, Kabbej M, Sauvanet A, Vilgrain V, Panis Y, Fekete F. Drainage after elective hepatic resection. A randomized trial. Ann Surg. 1993;218:748–53.
Fong Y, Brennan MF, Brown K, Heffernan N, Blumgart LH. Drainage is unnecessary after elective liver resection. Am J Surg. 1996;171:158–62.
Liu CL, Fan ST, Lo CM, Wong Y, Ng IO, Lam CM, et al. Abdominal drainage after hepatic resection is contraindicated in patients with chronic liver diseases. Ann Surg. 2004;239:194–201.
Sun HC, Qin LX, Lu L, Wang L, Ye QH, Ren N, et al. Randomized clinical trial of the effects of abdominal drainage after elective hepatectomy using the crushing clamp method. Br J Surg. 2006;93:422–6.
Yamanaka N, Okamoto E, Oriyama T, Fujimoto J, Furukawa K, Kawamura E, et al. A prediction scoring system to select the surgical treatment of liver cancer. Further refinement based on 10 years of use. Ann Surg. 1994;219:342–6.
Pringle JH. Notes on the arrest of hepatic hemorrhage due to trauma. Ann Surg. 1908;48:541–9.
Makuuchi M, Mori T, Gunvén P, Yamazaki S, Hasegawa H. Safety of hemihepatic vascular occlusion during resection of the liver. Surg Gynecol Obstet. 1987;164:155–8.
Takasaki K, Kobayashi S, Tanaka S, Muto H, Watayo T. Highly selected hepatic resection by Glissonean sheath-binding method. Dig Surg. 1986;3:121.
Santiago Delpin EA, Figueroa I, Lopez R, Vazquez J. Protective effect of steroids on liver ischemia. Am Surg 1975;41:683–5.
The Brisbane 2000 Terminology of Liver Anatomy and Resection. Terminology Committee of the International Hepato-Pancreato-Biliary Association. HPB 2000;2:333–9.
Dindo D, Demartines N, Clavien PA. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg. 2004;240:205–13.
Pachter HL, Hofstetter SR, Spencer FC. Evolving concepts in splenic surgery: splenorrhaphy versus splenectomy and postsplenectomy drainage: experience in 105 patients. Ann Surg. 1981;194:262–9.
Fuster J, Llovet JM, Garcia-Valdecasas JC, Grande L, Fondevila C, Vilana R, et al. Abdominal drainage after liver resection for hepatocellular carcinoma in cirrhotic patients: a randomized controlled study. Hepatogastroenterology. 2004;51:536–40.
Rosemurgy AS, Statman RC, Murphy CG, Albrink MH, McAllister EW. Postoperative ascitic leaks: the ongoing challenge. Surgery. 1992;111:623–5.
Ronaghan JE, Miller SF, Finley RK Jr, Jones LM, Elliott DW. A statistical analysis of drainage versus nondrainage of elective cholecystectomy. Surg Gynecol Obstet. 1986;162:253–5.
Bona S, Gavelli A, Huguet C. The role of abdominal drainage after major hepatic resection. Am J Surg. 1994;167:593–5.
Torzilli G, Olivari N, Del Fabbro D, Gambetti A, Leoni P, Gendarini A, et al. Bilirubin level fluctuation in drain discharge after hepatectomies justifies long-term drain maintenance. Hepatogastroenterology. 2005;52:1206–10.
Williams CB, Halpin DS, Knox AJ. Drainage following cholecystectomy. Br J Surg. 1972;59:293–6.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tanaka, K., Kumamoto, T., Nojiri, K. et al. The effectiveness and appropriate management of abdominal drains in patients undergoing elective liver resection: a retrospective analysis and prospective case series. Surg Today 43, 372–380 (2013). https://doi.org/10.1007/s00595-012-0254-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-012-0254-1