Abstract
Objectives
Biofilm formation reduces the efficacy of standard microbiological techniques in prosthetic joint infection. This study aimed to investigate the sensitivity, specificity and predictive values of tissue sample enrichment as a means to increase diagnostic yield.
Methods
Patients undergoing revision arthroplasty surgery between May 2004 and January 2013 had intraoperative tissue samples cultured in standard media as well as enriched in brain heart infusion broth. Patients were separated into infected or non-infected groups according to modified criteria from the Musculoskeletal Infection Society.
Results
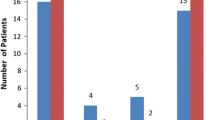
A total of 197 revision arthroplasties were included (non-infected, n = 165; proven infection, n = 32). The mean time until revision in non-infected and infected groups was 75.9 and 41.7 months, respectively. The commonest microorganisms cultured were coagulase-negative staphylococci (42.9 %) and Staphylococcus aureus (34.4 %). The sensitivity and specificity of standard tissue culture were 0.25 (CI 0.18–0.33) and 0.98 (CI 0.95–0.99), respectively. Including enrichment culture results increased the sensitivity to 0.45 (CI 0.37–0.54), but decreased specificity to 0.59 (CI 0.52–0.66).
Conclusion
Any potential increase in the sensitivity is far outweighed by the extremely high false-positive rate. Results of tissue samples cultured by enrichment should be used with caution and may lead to a worse outcome if incorrectly interpreted.
Similar content being viewed by others
References
Kurtz SM, Lau E, Schmier J, Ong KL, Zhao K, Parvizi J (2008) Infection burden for hip and knee arthroplasty in the United States. J Arthroplasty 23(7):984–991
Jamsen E, Varonen M, Huhtala H, Lehto MU, Lumio J, Konttinen YT, Moilanen T (2010) Incidence of prosthetic joint infections after primary knee arthroplasty. J Arthroplasty 25(1):87–92
Pulido L, Ghanem E, Joshi A, Purtill JJ, Parvizi J (2008) Periprosthetic joint infection: the incidence, timing, and predisposing factors. Clin Orthop 466(7):1710–1715
Phillips JE, Crane TP, Noy M, Elliott TS, Grimer RJ (2006) The incidence of deep prosthetic infections in a specialist orthopaedic hospital: a 15 year prospective survey. J Bone Joint Surg Br 88(7):943–948
Parvizi J, Zmistowksi B, Berbar EF, Bauer TW, Springer BD, Della Valle CJ, Garvin KL, Mont MA, Wongworawat MD, Zalavras CG (2011) New definition for periprosthetic joint infection: from the workgroup of the Musculoskeletal Infection Society. Clin Orthop Relat Res 469:2992–2994
Bauer TW, Parvizi J, Kobayashi N, Krebs V (2006) Current concepts review—diagnosis of periprosthetic infection. J Bone Joint Surg Am 88(4):869–881
Parvizi J, Adeli B, Zmistowski B, Restrepo C, Greenwald A (2012) Management of periprosthetic joint infection: the current knowledge. AAOS exhibit selection. J Bone Joint Surg Am 94(14):104
Atkins BL, Athanasou N, Deeks JJ, Crook DWM, Simpson H, Peto TEA, Mclardy-Smith P, Berendt AR (1998) Prospective evaluation of criteria for microbiological diagnosis of prosthetic-joint infection at revision arthroplasty. J Clin Microbiol 36:2932–2939
Parvizi J, Ghanem E, Sharkey P, Aggarwal A, Burnett SJ, Barrack RL (2008) Diagnosis of infected total knee: findings of a multicenter database. Clin Orthop Relat Res 466(11):2628–2633
Trampuz A, Piper KE, Jacobson MJ, Hanssen AD, Unni KK, Osmon DR, Mandrekar JN, Cockerill FR, Steckelberg JM, Greenleaf JF, Patel R (2007) Sonication of removed hip and knee prostheses for diagnosis of infection. N Engl J Med 357(7):654–663
Daur AV, Klimak F Jr, Cogo LL, Botão GD, Monteiro CL, Dalla Costa LM (2006) Enrichment methodology to increase the positivity of cultures from body fluids. Braz J Infect Dis 10(6):372–373
Hughes HC, Newnham R, Athanasou N, Atkins BL, Bejon P, Bowler IC (2011) Microbiological diagnosis of prosthetic joint infections: a prospective evaluation of four bacterial culture media in the routine laboratory. Clin Microbiol Infect 17(10):1528–1530
Velay A, Schramm F, Gaudias J, Jaulhac B, Riegel P (2010) Culture with BACTEC Peds Plus bottle compared with conventional media for the detection of bacteria in tissue samples from orthopedic surgery. Diagn Microbiol Infect Dis 68(1):83–85
Trampuz A, Steckelberg JM, Osmon DR, Cockerill FR, Hanssen AD, Patel R (2003) Advances in the laboratory diagnosis of prosthetic joint infection. Rev Clin Microbiol 14:1–14
http://www.oxoid.com/UK/blue/prod_detail/prod_detail.asp?pr=CM1135&c. Accessed 1 Sept 2014
Larsen LH, Lange J, Xu Y, Schonheyder HC (2012) Optimizing culture methods for diagnosis of prosthetic joint infections: a summary of modifications and improvements reported since 1995. J Med Microbiol 61(3):309–316
Sharma D, Douglas J, Coulter C, Weinrauch P, Crawford R (2008) Microbiology of infected arthroplasty: implications for empiric peri-operative antibiotics. J Orthop Surg 16(3):339–342
Nickinson RSJ, Board TN, Gambhir AK, Porter ML, Kay PR (2010) The microbiology of the infected knee arthroplasty. Int Orthop 34(4):505–510
Stefánsdóttir A, Johansson D, Knutson K, Lidgren L, Robertsson O (2009) Microbiology of the infected knee arthroplasty: report from the Swedish Knee Arthroplasty Register on 426 surgically revised cases. Scand J Infect Dis 41(11–12):831–840
Tsukayama DT, Estrada R, Gustilo RB (1996) Infection after total hip arthroplasty: a study of the treatment of one hundred and six infections. J Bone Joint Surg Am 78:512–523
Berbari EF, Marculescu C, Sia I, Lahr BD, Hanssen AD, Steckelberg JM, Gullerud R, Osmon DR (2007) Culture-negative prosthetic joint infection. Clin Infect Dis 45:1113–1119
Katz RP, Callaghan JJ, Sullivan PKM, Johnston RC (1997) Long-term results of revision total hip arthroplasty with improved cementing technique. J Bone Joint Surg Br 79(2):322–326
Kosashvili Y, Backstein D, Safir O, Lakstein D, Gross AE (2011) Dislocation and infection after revision total hip arthroplasty: comparison between the first and multiply revised total hip arthroplasty. J Arthroplasty 26(8):1170–1175
Mortazavi SM, Schwartzenberger J, Austin MS, Purtill JJ, Parvizi J (2010) Revision total knee arthroplasty infection: incidence and predictors. Clin Orthop Relat Res 468(8):2052–2059
Conflict of interest
All authors confirm that there are no conflict of interest to declare.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Jordan, R.W., Saithna, A., Smith, N. et al. Does intraoperative tissue sample enrichment help or hinder the identification of microorganisms in prosthetic joint infection?. Eur J Orthop Surg Traumatol 25, 731–736 (2015). https://doi.org/10.1007/s00590-014-1564-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-014-1564-3