Abstract
Purpose
The endotracheal tube (ETT) constitutes a significant component of total airway resistance. However, a discrepancy between measured and theoretical values has been reported in airway resistance through ETTs. The causes of the discrepancy were estimated by physical and rheological simulations.
Methods
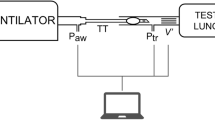
The pressure losses through total lengths of ETTs and slip joints under a volumetric flow rate of 30 L/min were measured, and the pressure losses through the tubular parts of ETTs with internal diameters (IDs) of 6.0-, 6.5-, 7.0-, 7.5-, and 8.0 mm were measured. The Reynolds number of each setting was calculated, and the pressure losses through the total length of the ETT, the tubular part, and the slip joint of each size of tube were estimated.
Results
The Reynolds numbers were >5000 in all sizes of ETTs. Measured pressure losses were larger in small sized ETTs than in large sized ETTs—520.9 Pascals (Pa) in 6.0-mm ID and 136.4 Pa in 8.0-mm ID tubes. The measured pressure losses through the tubular part were comparable to the predicted values. The measured pressure losses through the slip joints were larger than the predicted values, and they accounted for approximately 25–40% of total pressure losses of the ETTs.
Conclusion
Especially in small sized tubes, the pressure loss through the slip joint accounts for a large percentage of the total pressure loss through the ETT. The pressure loss through the slip joint may play a role in the discrepancy between measured and theoretical pressure losses through ETTs.





Similar content being viewed by others
References
Fabry B, Haberthür C, Zappe D, Guttmann J, Kuhlen R, Stocker R, Breathing pattern and additional work of breathing in spontaneously breathing patients with different ventilatory demands during inspiratory pressure support and automatic tube compensation. Intensive Care Med. 1997;23:545–52.
Messinger G, Banner MJ, Blanch PB, Layon AJ. Using tracheal pressure to trigger the ventilator and control airway pressure during continuous positive airway pressure decreases work of breathing. Chest. 1995;108:509–14.
Brochard L, Rua F, Lorino H, Lemaire F, Harf A. Inspiratory pressure support compensates for the additional work of breathing caused by the endotracheal tube. Anesthesiology. 1991;75:739–45.
Bersten AD, Rutten AJ, Vedig AE, Skowronski GA. Additional work of breathing imposed by endotracheal tubes, breathing circuits, and intensive care ventilators. Crit Care Med. 1989;17:671–7.
Flevari AG, Maniatis N, Kremiotis TE, Siempos I, Betrosian AP, Roussos C, Douzinas E, Armaganidis A. Rohrer’s constant, K2, as a factor of determining inspiratory resistance of common adult endotracheal tubes. Anaesth Intensive Care. 2011;39:410–7.
Shandro J. Resistance to gas flow in the “new” anaesthesia circuits: a comparative study. Can Anaesth Soc J. 1982;29:387–90.
Lofaso F, Louis B, Brochard L, Harf A, Isabey D. Use of the Blasius resistance formula to estimate the effective diameter of endotracheal tubes. Am Rev Respir Dis. 1992;146:974–9.
Katz IM, Martin AR, Feng CH, Majoral C, Caillibotte G, MarxT Bazin JE, Daviet C. Airway pressure distribution during xenon anesthesia: the insufflation phase at constant flow (volume controlled mode). Appl Cardiopulm Pathophysiol. 2012;16:5–16.
Schumann S, Krappitz M, Möller K, Hentschel R, Braun G, Guttmann J. Pressure loss caused by pediatric endotracheal tubes during high-frequency-oscillation-ventilation. Respir Physiol Neurobiol. 2008;162(2):132–7.
Zarei S, Mirtar A, Andresen B, Salamon P. Modeling the airflow in a lung with cystic fibrosis. J Non-Equilib Thermodyn. 2013;38:119–40.
McGovern J. Technical note: friction diagrams for pipe flow. Dublin Institute of Technology. 2011;1–15.
Swamee P, Jain A. Explicit equations for pipe-flow problems. J Hydraul Div (ASCE). 1976;102:657–64.
Schmidt M, Marx T, Papp-Jambor C, Reinelt H, Schirmer U. Airway pressures during xenon anaesthesia. Appl Cardiopulm Pathophysiol. 2009;13:208–11.
Çengel YA, Cimbala JM, Turner RH. Chapter 12 Bernoulli and energy equations. In: Çengel YA, Cimbala JM, Turner RH, editors. Fundamentals of thermal-fluid sciences. 4th ed. New York: McGraw-Hill Higher Education; 2012. p. 471–503.
Kamat SS, Muralidhar K. Chapter 28 volume controlled ventilation. In: Kamat SS, Muralidhar K, editors. Practical applications of mechanical ventilation. 2nd edn. New Delhi: Jaypee Brothers Medical Publishers; 2016. p. 372–385.
Acknowledgments
The authors thank Mr. Hajime Tamitsu (dental technician, Department of Oral and Maxillofacial Surgery, Kindai University Hospital) for his help in moulding the slip joints.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
YT, KF and TO declare that there is no conflict of interest regarding the publication of this paper. KK and SM have been employed by Product Development Research Center, Daiken Medical Co. Ltd., Osaka, Japan.
About this article
Cite this article
Takasugi, Y., Futagawa, K., Kazuhara, K. et al. Roles of endotracheal tubes and slip joints in respiratory pressure loss: a laboratory study. J Anesth 30, 789–795 (2016). https://doi.org/10.1007/s00540-016-2210-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00540-016-2210-5