Abstract
Purpose
Dry mouth (xerostomia) is one of the commonest symptoms in cancer patients and can adversely affect quality of life. The aim of this review was to determine the effectiveness of pharmacological and non-pharmacological interventions in treating xerostomia in adult advanced cancer patients.
Methods
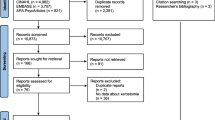
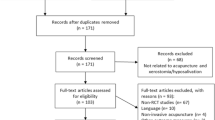
The literature search was performed in February 2014 using databases including EMBASE, MEDLINE, CINAHL, BNI and Cochrane library. The search was carried out using standard MeSH terms and was limited to adult population and English language. Studies investigating xerostomia secondary to head and neck cancer treatment and autoimmune disease were excluded. Titles and abstracts were screened and reviewed for eligibility. Only studies involving primary research were included in the analysis.
Results
Six studies met the eligibility criteria for review: three randomized controlled trials and three prospective studies. The quality assessment and reporting was performed using PRISMA, Jadad and STROBE. These studies compared acupuncture, pilocarpine, Saliva Orthana and chewing gum with each other or with placebo. All interventions were considered effective in treating xerostomia. However, effectiveness versus placebo could not be demonstrated for Saliva Orthana. Meta-analysis could not be performed due to heterogeneity of the study type and intervention.
Conclusion
Limited published data exists reporting the effectiveness of measures in the treatment of xerostomia in cancer patients. Based on primary research of low quality, firm conclusions cannot be drawn. However, pilocarpine, artificial saliva, chewing gum and acupuncture can be tried based on the available data. This highlights the explicit need to improve our evidence base. Properly constructed randomized controlled trials demonstrating effectiveness of pharmacological and non-pharmacological interventions for dry mouth are required.

Similar content being viewed by others
References
von Bultzingslowen I, Sollecito TP, Fox PC, Daniels T, Jonsson R, Lockhart PB, Wray D, Brennan MT, Carrozzo M, Gandera B, Fujibayashi T, Navazesh M, Rhodus NL, Schiodt M (2007) Salivary dysfunction associated with systemic diseases: systematic review and clinical management recommendations. Oral Surg, Oral Med, Oral Pathol, Oral Radiology Endod 103(S57):e51–15. doi:10.1016/j.tripleo.2006.11.010
Atkinson JC, Grisius M, Massey W (2005) Salivary hypofunction and xerostomia: diagnosis and treatment. Dent Clin N Am 49(2):309–326. doi:10.1016/j.cden.2004.10.002
Porter SR, Scully C, Hegarty AM (2004) An update of the etiology and management of xerostomia. Oral Surg, Oral Med, Oral Pathol, Oral Radiol Endod 97(1):28–46. doi:10.1016/S1079210403005572
Jobbins J, Bagg J, Finlay IG, Addy M, Newcombe RG (1992) Oral and dental disease in terminally ill cancer patients. BMJ 304(6842):1612
Shragge JE, Wismer WV, Olson KL, Baracos VE (2006) The management of anorexia by patients with advanced cancer: a critical review of the literature. Palliat Med 20(6):623–629. doi:10.1177/0269216306070322
Twycross R, Wilcock A, Toller C (2009) Alimentary symptoms. In: Twycross R, Wilcock A, Toller C (eds) Symptom management in advanced cancer, 4th edition. 4th edn. Palliativedrugs.com Ltd, Oxford, pp 62–65
Rydholm M, Strang P (2002) Physical and psychosocial impact of xerostomia in palliative cancer care: a qualitative interview study. Int J Palliat Nurs 8(7):318–323
Davies A, Bagg J, Laverty D, Sweeney P, Filbet M, Newbold K, De Andres J, Mercadante S (2010) Salivary gland dysfunction (‘dry mouth’) in patients with cancer: a consensus statement. Eur J Cancer Care 19(2):172–177. doi:10.1111/j.1365-2354.2009.01081.x
Twycross R, Wilcock A (2012) Ear nose and oropharynx. In: Twycross R, Wilcock A (eds) PCF4- palliative care formulary. Radcliffe Press, Oxford, pp 569–573
Davies AN, Broadley K, Beighton D (2002) Salivary gland hypofunction in patients with advanced cancer. Oral Oncol 38(7):680–685
Simcock R, Shields P (2011) Management of radiation induced xerostomia in the UK. Clin Oncol 23(1):S53
Adkinson L, Hussain J, Daniel S, Oxberry S (2014) Oral health is an important issue in end-of-life care, December 2012. Support Care Cancer: Off J Multinatl Assoc Support Care Cancer 22(2):293–294. doi:10.1007/s00520-013-1992-3
Wilberg P, Hjermstad MJ, Ottesen S, Herlofson BB (2012) Oral health is an important issue in end-of-life cancer care. Support Care Cancer: Off J Multinatl Assoc Support Care Cancer 20(12):3115–3122. doi:10.1007/s00520-012-1441-8
De Conno F, Ripamonti C, Sbanotto A, Ventafridda V (1989) Oral complications in patients with advanced cancer. J Palliat Care 5(1):7–15
Jadad AR, Moore RA, Carroll D, Jenkinson C, Reynolds DJ, Gavaghan DJ, McQuay HJ (1996) Assessing the quality of reports of randomized clinical trials: is blinding necessary? Control Clin Trials 17(1):1–12
STROBE Statement: http://www.strobe-statement.org/index.php?id=available-checklists. http://www.strobe-statement.org/index.php?id=available-checklists. Accessed 8th Aug 2014
Davies AN (2000) A comparison of artificial saliva and chewing gum in the management of xerostomia in patients with advanced cancer. Palliat Med 14(3):197–203
Davies AN, Daniels C, Pugh R, Sharma K (1998) A comparison of artificial saliva and pilocarpine in the management of xerostomia in patients with advanced cancer. Palliat Med 12(2):105–111
Mercadante S, Calderone L, Villari P, Serretta R, Sapio M, Casuccio A, Fulfaro F (2000) The use of pilocarpine in opioid-induced xerostomia. Palliat Med 14(6):529–531
Rydholm M, Strang P (1999) Acupuncture for patients in hospital-based home care suffering from xerostomia. J Palliat Care 15(4):20–23
Meidell L, Holritz Rasmussen B (2009) Acupuncture as an optional treatment for hospice patients with xerostomia: an intervention study. Int J Palliat Nurs 15(1):12–20
Sweeney MP, Bagg J, Baxter WP, Aitchison TC (1997) Clinical trial of a mucin-containing oral spray for treatment of xerostomia in hospice patients. Palliat Med 11(3):225–232
Braga MA, Tarzia O, Bergamaschi CC, Santos FA, Andrade ED, Groppo FC (2009) Comparison of the effects of pilocarpine and cevimeline on salivary flow. Int J Dent Hyg 7(2):126–130. doi:10.1111/j.1601-5037.2008.00326.x
Loostrom H, Akerman S, Ericson D, Tobin G, Gotrick B (2011) Tramadol-induced oral dryness and pilocarpine treatment: effects on total protein and IgA. Arch Oral Biol 56(4):395–400. doi:10.1016/j.archoralbio.2010.10.019
Towler P, Molassiotis A, Brearley SG (2013) What is the evidence for the use of acupuncture as an intervention for symptom management in cancer supportive and palliative care: an integrative overview of reviews. Support Care Cancer: Off J Multinatl Assoc Support Care Cancer 21(10):2913–2923. doi:10.1007/s00520-013-1882-8
Kim JO, Kim NC (2014) Effects of 4% hypertonic saline solution mouthwash on oral health of elders in long term care facilities. J Korean Acad Nurs 44(1):13–20. doi:10.4040/jkan.2014.44.1.13
Senn HJ (1997) Orphan topics in supportive care: how about xerostomia? Support Care Cancer: Off J Multinatl Assoc Support Care Cancer 5(4):261–262
Jensen SB, Pedersen AM, Vissink A, Andersen E, Brown CG, Davies AN, Dutilh J, Fulton JS, Jankovic L, Lopes NN, Mello AL, Muniz LV, Murdoch-Kinch CA, Nair RG, Napenas JJ, Nogueira-Rodrigues A, Saunders D, Stirling B, von Bultzingslowen I, Weikel DS, Elting LS, Spijkervet FK, Brennan MT, Salivary Gland Hypofunction/Xerostomia S, Oral Care Study G, Multinational Association of Supportive Care in Cancer /International Society of Oral O (2010) A systematic review of salivary gland hypofunction and xerostomia induced by cancer therapies: management strategies and economic impact. Support Care Cancer: Off J Multinatl Assoc Support Care Cancer 18(8):1061–1079. doi:10.1007/s00520-010-0837-6
Furness S, Worthington HV, Bryan G, Birchenough S, McMillan R (2011) Interventions for the management of dry mouth: topical therapies. The Cochrane database of systematic reviews (12):CD008934. doi:10.1002/14651858.CD008934.pub2
Sullivan CA, Haddad RI, Tishler RB, Mahadevan A, Krane JF (2005) Chemoradiation-induced cell loss in human submandibular glands. Laryngoscope 115(6):958–964. doi:10.1097/01.MLG.0000163340.90211.87
Chambers MS, Artopoulou L, Garden AS (2007) Xerosomia. In: Myers EN, Ferris RL (eds) Salivary gland disorders. Springer, Berlin, pp 185–199
Chambers MS, Garden AS, Kies MS, Martin JW (2004) Radiation-induced xerostomia in patients with head and neck cancer: pathogenesis, impact on quality of life, and management. Head Neck 26(9):796–807. doi:10.1002/hed.20045
Acknowledgments
The authors would like thank Jenny Makeham, corporate support librarian at Leeds General Infirmary, for performing the database literature search and Dr. Amy Gadoud for reviewing the manuscript.
Conflict of interest
We declare that we do not have any conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Appendix
Appendix
Rights and permissions
About this article
Cite this article
Hanchanale, S., Adkinson, L., Daniel, S. et al. Systematic literature review: xerostomia in advanced cancer patients. Support Care Cancer 23, 881–888 (2015). https://doi.org/10.1007/s00520-014-2477-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-014-2477-8