Abstract
Purpose
While the possible ergogenic benefits of remote ischemic preconditioning (RIPC) make it an attractive training modality, the mechanisms of action remain unclear. Alterations in neural tone have been demonstrated in conjunction with circulatory occlusion, yet investigation of the autonomic nervous system following RIPC treatment has received little attention. We sought to characterize alterations in autonomic balance to both RIPC and augmented RIPC (RIPCaug) performed while cycling, using acute and sustained autonomic indices.
Methods
Thirteen participants (8M:5F) recorded baseline waking heart rate variability (HRV) for 5 days prior to treatment. Participants then completed control exercise (CON), RIPC, and RIPCaug interventions in a randomized cross-over design. Cardiovascular measurements were recorded immediately before and after each intervention at rest, and during an orthostatic challenge. Waking HRV was repeated the morning after each intervention.
Results
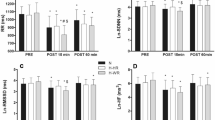
RIPC resulted in acutely reduced resting heart rates (HR) (∆ − 4 ± 6 bpm, P = 0.02) and suppressed HR 30 s following the orthostatic challenge compared to CON (64 ± 10 vs 74 ± 9 bpm, P = 0.003). RIPCaug yielded elevated HRs compared to CON and RIPC prior to (P = 0.003) and during the orthostatic challenge (P = 0.002). RIPCaug reduced LnSDNN (Baseline 4.39 ± 0.27; CON 4.44 ± 0.39; RIPC 4.41 ± 0.34; RIPCaug 4.22 ± 0.29, P = 0.02) and LnHfa power (Baseline 7.82 ± 0.54; CON 7.73 ± 1.11; RIPC 7.89 ± 0.78; RIPCaug 7.23 ± 0.87, P = 0.04) the morning after treatment compared to all other conditions.
Conclusions
Our data suggest that RIPC may influence HR acutely, possibly through a reduction in cardiac sympathetic activity, and that RIPCaug reduces HRV through cardiac vagal withdrawal or increased cardiac sympathetic modulation, with alterations persisting until the following morning. These findings imply a dose–response relationship with potential for optimization of performance.





Similar content being viewed by others
Data availability
Available upon request.
Abbreviations
- ANOVA:
-
Analysis of variance
- BP:
-
Blood pressure
- CON:
-
Control exercise
- DBP:
-
Diastolic blood pressure
- HFa:
-
High-frequency absolute power
- HR:
-
Heart rate
- HRR:
-
Heart rate recovery
- HRV:
-
Heart rate variability
- RIPC:
-
Remote ischemic preconditioning
- RIPCaug :
-
Augmented remote ischemic preconditioning
- LF/HF:
-
Low-frequency-to-high-frequency ratio
- LnHFA:
-
Natural log high-frequency absolute power
- LnRMSSD:
-
Natural log of root mean square of successive differences
- LOP:
-
Least occlusion pressure
- RM-ANOVA:
-
Repeated-measures analysis of variance
- RMSSD:
-
Root mean square of successive differences
- ROS:
-
Reactive oxidative species
- SBP:
-
Systolic blood pressure
- SDNN:
-
Standard deviation of normal-to-normal intervals
References
Adreani CM, Hill JM, Kaufman MP (1997) Responses of group III and IV muscle afferents to dynamic exercise. J Appl Physiol 82:1811–1817. https://doi.org/10.1152/jappl.1997.82.6.1811
Aebi MR, Willis SJ, Girard O et al (2019) Active preconditioning with blood flow restriction or/and systemic hypoxic exposure does not improve repeated sprint cycling performance. Front Physiol. https://doi.org/10.3389/fphys.2019.01393
Alessio HM, Hagerman AE, Fulkerson BK et al (2000) Generation of reactive oxygen species after exhaustive aerobic and isometric exercise. Med Sci Sports Exerc 32:1576–1581. https://doi.org/10.1097/00005768-200009000-00008
Archer SL, Huang J, Henry T et al (1993) A redox-based 02 sensor in rat pulmonary vasculature. Circ Res 73:1100–1112
Basalay M, Barsukevich V, Mastitskaya S et al (2012) Remote ischaemic pre- and delayed postconditioning—similar degree of cardioprotection but distinct mechanisms. Exp Physiol 97:908–917. https://doi.org/10.1113/expphysiol.2012.064923
Billman G, Huikuri H, Sacha J, Trimmel K (2015) An introduction to heart rate variability: Methodological considerations and clinical applications. Front Physiol 6:2013–2015. https://doi.org/10.3389/fphys.2015.00055
Boulton D, Taylor CE, Green S, Macefield VG (2018) The metaboreflex does not contribute to the increase in muscle sympathetic nerve activity to contracting muscle during static exercise in humans. J Physiol 596:1091–1102. https://doi.org/10.1113/JP275526
Camm AJ, Malik M, Bigger JTJ et al (1996) Heart rate variability: standards of measurement, physiological interpretation, and clinical use. Eur Heart J 17:354–381. https://doi.org/10.1161/01.CIR.93.5.1043
Campese VM, Ye S, Zhong H et al (2004) Reactive oxygen species stimulate central and peripheral sympathetic nervous system activity. Am J Physiol Hear Circ Physiol 287:695–703. https://doi.org/10.1152/ajpheart.00619.2003
Cole CR, Blackstone EH, Pashkow FJ et al (1999) Heart-rate recovery immediately after exercise as a predictor of mortality. N Engl J Med 341:1351–1357. https://doi.org/10.1056/NEJM199910283411804
Crisafulli A, Tangianu F, Tocco F et al (2011) Ischemic preconditioning of the muscle improves maximal exercise performance but not maximal oxygen uptake in humans. J Appl Physiol 111:530–536. https://doi.org/10.1152/japplphysiol.00266.2011
Danieli A, Lusa L, Potočnik N et al (2014) Resting heart rate variability and heart rate recovery after submaximal exercise. Clin Auton Res 24:53–61. https://doi.org/10.1007/s10286-014-0225-2
De Groot PCE, Thijssen DHJ, Sanchez M et al (2010) Ischemic preconditioning improves maximal performance in humans. Eur J Appl Physiol. https://doi.org/10.1007/s00421-009-1195-2
De Vito G, Galloway SDR, Nimmo MA et al (2002) Effects of central sympathetic inhibition on heart rate variability during steady-state exercise in healthy humans. Clin Physiol Funct Imaging 22:32–38. https://doi.org/10.1046/j.1475-097x.2002.00395.x
Enko K, Nakamura K, Yunoki K et al (2011) Intermittent arm ischemia induces vasodilatation of the contralateral upper limb. J Physiol Sci 61:507–513. https://doi.org/10.1007/s12576-011-0172-9
Ferreira TN, Sabino-Carvalho JLC, Lopes TR et al (2016) Ischemic preconditioning and repeated sprint swimming: a placebo and nocebo study. Med Sci Sports Exerc 48:1967–1975. https://doi.org/10.1249/MSS.0000000000000977
Furlan R, Piazza S, Orto SD et al (1993) Early and late effects of exercise and athletic training on neural mechanisms controlling heart rate. Med Interna (Bucur) 16:482–488. https://doi.org/10.1093/cvr/27.3.482
Gibson N, White J, Neish M, Murray A (2013) Effect of ischemic preconditioning on land-based sprinting in team-sport athletes. Int J Sports Physiol Perform 8:671–676. https://doi.org/10.1123/ijspp.8.6.671
Giles D, Draper N, Neil W (2016) Validity of the Polar V800 heart rate monitor to measure RR intervals at rest. Eur J Appl Physiol 116:563–571. https://doi.org/10.1007/s00421-015-3303-9
Gourine A, Mastitskaya S, Ackland G (2010) “Remote preconditioning reflex”—a neural pathway of cardioprotection during myocardial ischaemia and reperfusion induced by remote ischaemic preconditioning. Eur Heart J 31:319–319
Halley SL, Marshall P, Siegler JC (2018) The effect of ischaemic preconditioning on central and peripheral fatiguing mechanisms in humans following sustained maximal isometric exercise. Exp Physiol. https://doi.org/10.1113/EP086981
Hara K, Floras JS (1992) Effects of naloxone on hemodynamics and sympathetic activity after exercise. J Appl Physiol 73:2028–2035. https://doi.org/10.1152/jappl.1992.73.5.2028
Holmes CJ, Fedewa M, Dobbs WC et al (2020) The effects of different body positions on the accuracy of ultra-short-term heart rate variability indexes. J High Technol Manag Res. https://doi.org/10.1016/j.hitech.2020.100375
Horiuchi M, Endo J, Thijssen DHJ (2015) Impact of ischemic preconditioning on functional sympatholysis during handgrip exercise in humans. Physiol Rep 3:1–9. https://doi.org/10.14814/phy2.12304
Hoshi RA, Pastre CM, Vanderlei LCM, Godoy MF (2013) Poincaré plot indexes of heart rate variability: relationships with other nonlinear variables. Auton Neurosci Basic Clin 177:271–274. https://doi.org/10.1016/j.autneu.2013.05.004
Incognito AV, Burr JF, Millar PJ (2016) The effects of ischemic preconditioning on human exercise performance. Sport Med
Incognito AV, Doherty CJ, Lee JB et al (2017) Ischemic preconditioning does not alter muscle sympathetic responses to static handgrip and metaboreflex activation in young healthy men. Physiol Rep 5:1–10. https://doi.org/10.14814/phy2.13342
Jean-St-Michel E, Manlhiot C, Li J et al (2011) Remote preconditioning improves maximal performance in highly trained athletes. Med Sci Sports Exerc. https://doi.org/10.1249/MSS.0b013e318206845d
Kenney MJ, Seals DR (1993) Brief review postexercise hypotension. Hypertension 22:653–664
Killilea DW, Hester R, Balczon R, et al (2000) Free radical production in hypoxic pulmonary artery smooth muscle cells. 279:408–412
Koch S, Della-Morte D, Dave KR, et al (2014) Biomarkers for ischemic preconditioning: finding the responders. J Cereb Blood Flow Metab
Korthuis RJ, Granger DN, Townsley MI, Taylor AE (1985) The role of oxygen-derived free radicals in ischemia-induced increases in canine skeletal muscle vascular permeability. Circ Res 57:599–609. https://doi.org/10.1161/01.RES.57.4.599
Lakens D (2013) Calculating and reporting effect sizes to facilitate cumulative science: a practical primer for t-tests and ANOVAs. Front Psychol 4:1–12. https://doi.org/10.3389/fpsyg.2013.00863
Li J, Sinoway LI (2002) ATP stimulates chemically sensitive and sensitizes mechanically sensitive afferents. Am J Physiol Hear Circ Physiol 283:2636–2643. https://doi.org/10.1152/ajpheart.00395.2002
Lim SY, Yellon DM, Hausenloy DJ (2010) The neural and humoral pathways in remote limb ischemic preconditioning. Basic Res Cardiol 105:651–655. https://doi.org/10.1007/s00395-010-0099-y
Liu JQ, Sham JSK, Shimoda LA et al (2003) Hypoxic constriction and reactive oxygen species in porcine distal pulmonary arteries. Am J Physiol Lung Cell Mol Physiol 285:322–333. https://doi.org/10.1152/ajplung.00337.2002
Lopes TR, Sabino-Carvalho JL, Ferreira THN et al (2018) Effect of ischemic preconditioning on the recovery of cardiac autonomic control from repeated sprint exercise. Front Physiol 9:1–11. https://doi.org/10.3389/fphys.2018.01465
Manzi V, Castagna C, Padua E et al (2009) Dose-response relationship of autonomic nervous system responses to individualized training impulse in marathon runners. Am J Physiol Hear Circ Physiol 296:1733–1740. https://doi.org/10.1152/ajpheart.00054.2009
Masri BA, Day B, Younger ASE, Jeyasurya J (2016) Technique for measuring limb occlusion pressure that facilitates personalized tourniquet systems: a randomized trial. J Med Biol Eng 36:644–650. https://doi.org/10.1007/s40846-016-0173-5
Mastitskaya S, Marina N, Gourine A et al (2012) Cardioprotection evoked by remote ischaemic preconditioning is critically dependent on the activity of vagal pre-ganglionic neurones. Cardiovasc Res 95:487–494. https://doi.org/10.1093/cvr/cvs212
McEwen JA, Masri BA, Day B, Younger AS (2015) Development of personalized tourniquet systems using a new technique for measuring limb occlusion pressure. IFMBE Proc. https://doi.org/10.1007/978-3-319-19387-8
Michelakis ED, Hampl V, Nsair A et al (2002) Diversity in mitochondrial function explains differences in vascular oxygen sensing. Circ Res 90:1307–1315. https://doi.org/10.1161/01.RES.0000024689.07590.C2
Murry CE, Jennings RB, Reimer KA (1986) Preconditioning with ischemia: a delay of lethal cell injury in ischemic myocardium. Circulation 74:1124–1136. https://doi.org/10.1161/01.CIR.74.5.1124
Murry CE, Richard VJ, Reimer KA, Jennings RB (1990) Ischemic preconditioning slows energy metabolism and delays ultrastructural damage during a sustained ischemic episode. Circ Res. https://doi.org/10.1161/01.RES.66.4.913
Patterson SD, Hughes L, Warmington S et al (2019) Blood flow restriction exercise position stand: considerations of methodology, application, and safety. Front Physiol. https://doi.org/10.3389/fphys.2019.00533
Petrick HL, Pignanelli C, Barbeau PA et al (2019) Blood flow restricted resistance exercise and reductions in oxygen tension attenuate mitochondrial H2O2 emission rates in human skeletal muscle. J Physiol 597:3985–3997. https://doi.org/10.1113/JP277765
Pichot V, Roche F, Gaspoz JM et al (2000) Relation between heart rate variability and training load in middle-distance runners. Med Sci Sports Exerc 32:1729–1736. https://doi.org/10.1097/00005768-200010000-00011
Plews DJ, Laursen PB, Stanley J et al (2013) Training adaptation and heart rate variability in elite endurance athletes: opening the door to effective monitoring. Sport Med 43:773–781
Plews DJ, Laursen PB, Le Meur Y et al (2014) Monitoring training with heart-rate variability: how much compliance is needed for valid assessment? Int J Sports Physiol Perform 9:783–790. https://doi.org/10.1123/IJSPP.2013-0455
Powers SK, Jackson MJ (2008) Exercise-induced oxidative stress: cellular mechanisms and impact on muscle force production. Physiol Rev 88:1243–1276. https://doi.org/10.1152/physrev.00031.2007
Sabino-Carvalho JL, Obeid-Freitas T, Paula-Ribeiro M et al (2019) Ischemic preconditioning boosts post-exercise but not resting cardiac vagal control in endurance runners. Eur J Appl Physiol 119:621–632. https://doi.org/10.1007/s00421-018-4052-3
Salvador AF, De Aguiar RA, Lisbôa FD et al (2016) Ischemic preconditioning and exercise performance: a systematic review and meta-analysis. Int J Sports Physiol Perform. https://doi.org/10.1123/ijspp.2015-0204
Shi M, Wang X, Yamanaka T et al (2007) Effects of anaerobic exercise and aerobic exercise on biomarkers of oxidative stress. Environ Health Prev Med 12:202–208. https://doi.org/10.1265/ehpm.12.202
Sivaraman V, Pickard JMJ, Hausenloy DJ (2015) Remote ischaemic conditioning: cardiac protection from afar. Anaesthesia 70:732–748. https://doi.org/10.1111/anae.12973
Slysz JT, Burr JF (2018) Enhanced metabolic stress augments ischemic preconditioning for exercise performance. Front Physiol. https://doi.org/10.3389/fphys.2018.01621
Slysz JT, Burr JF (2019) Impact of 8 weeks of repeated ischemic preconditioning on running performance. Eur J Appl Physiol 119:1431–1437. https://doi.org/10.1007/s00421-019-04133-6
Slysz JT, Petrick HL, Marrow JP, Burr JF (2019) An examination of individual responses to ischemic preconditioning and the effect of repeated ischemic preconditioning on cycling performance. Eur J Sport Sci. https://doi.org/10.1080/17461391.2019.1651401
Tsutsumi YM, Yokoyama T, Horikawa Y et al (2007) Reactive oxygen species trigger ischemic and pharmacological postconditioning: in vivo and in vitro characterization. Life Sci 81:1223–1227. https://doi.org/10.1038/jid.2014.371
Waypa GB, Schumacker PT (2005) Hypoxic pulmonary vasoconstriction: redox events in oxygen sensing. J Appl Physiol 98:404–414. https://doi.org/10.1152/japplphysiol.00722.2004
Waypa GB, Chandel NS, Schumacker PT (2001) Model for hypoxic pulmonary vasoconstriction involving mitochondrial oxygen sensing. Circ Res 88:1259–1266. https://doi.org/10.1161/hh1201.091960
Yellon DM, Baxter GF (1995) A “second window of protection” or delayed preconditioning phenomenon: future horizons for myocardial protection? J Mol Cell Cardiol 27:1023–1034. https://doi.org/10.1016/0022-2828(95)90071-3
Funding
This work was supported by a Discovery Grant from the Natural Sciences and Engineering Research Council of Canada (Grant #03974 to JFB), and the Canada Foundation for Innovation (Grant #460597 to JFB).
Author information
Authors and Affiliations
Contributions
All authors contributed to research conception, design, data interpretation, and editing. WNM and AMC conducted experiments, analyzed data, and drafted the manuscript. All authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
None.
Ethical approval
This study was carried out in accordance with the University research ethics board (REB #19-03-011), and all subjects provided written informed consent in accordance with the Declaration of Helsinki.
Consent to participate
All participants provided written, informed consent.
Consent to publication
All authors and participants provided written, informed consent for publication.
Additional information
Communicated by Ellen Adele Dawson.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Morley, W.N., Coates, A.M. & Burr, J.F. Cardiac autonomic recovery following traditional and augmented remote ischemic preconditioning. Eur J Appl Physiol 121, 265–277 (2021). https://doi.org/10.1007/s00421-020-04526-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-020-04526-y