Abstract
Background
The vascularization of an orbital implant is a key issue for reducing complications, such as exposure and infection.
Methods
Here, we developed a facile layer-by-layer assembly approach to modify porous hydroxyapatite (pHA) orbital implants with five collagen (COL)/heparin (HEP) multilayers.
Results
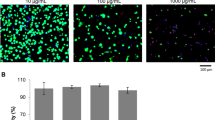
SEM characterization showed that the average pore size of the pHA/(COL/HEP)5 scaffold was 316.8 ± 77.1 μm. After being coated with five COL/HEP multilayers, the mechanical strength was improved compared with that of the pHA scaffolds. The in vitro assay displayed that the pHA scaffolds covered with COL/HEP multilayers resulted in a larger number of human umbilical vein endothelial cells after being cultured for 14 days. The macroscopic evaluation and semi-quantitative vascular density analysis of the chicken chorioallantoic membrane assay showed that the pHA/(COL/HEP)5 scaffolds resulted in more intense angiogenesis than the pHA scaffolds.
Conclusions
These studies demonstrate that the biomembrane-mimicking coating of COL/HEP multilayers is a simple and effective strategy to endow combined biological performances of pHA orbital implants and to potentially reduce implant-related complications.







Similar content being viewed by others
References
Thaller VT (1997) Enucleation volume measurement. Ophthal Plast Reconstr Surg 13(1):18–20
Mourits DL, Hartong DT, Bosscha MI, Kloos RJ, Moll AC (2015) Worldwide enucleation techniques and materials for treatment of retinoblastoma: an international survey. PLoS One 10(3), e0121292. doi:10.1371/journal.pone.0121292
Baino F, Perero S, Ferraris S, Miola M, Balagna C, Verne E, Vitale-Brovarone C, Coggiola A, Dolcino D, Ferraris M (2014) Biomaterials for orbital implants and ocular prostheses: overview and future prospects. Acta Biomater 10(3):1064–1087. doi:10.1016/j.actbio.2013.12.014
Sami D, Young S, Petersen R (2007) Perspective on orbital enucleation implants. Surv Ophthalmol 52(3):244–265. doi:10.1016/j.survophthal.2007.02.007
Perry AC (1990) Integrated orbital implants. Adv Ophthalmic Plast Reconstr Surg 8:75–81
Hornblass A, Biesman BS, Eviatar JA (1995) Current techniques of enucleation: a survey of 5,439 intraorbital implants and a review of the literature. Ophthal Plast Reconstr Surg 11(2):77–88
Custer PL, Trinkaus KM (2007) Porous implant exposure: incidence, management, and morbidity. Ophthal Plast Reconstr Surg 23(1):1–7. doi:10.1097/01.iop.0000249432.18688.ee
Remulla HD, Rubin PA, Shore JW, Sutula FC, Townsend DJ, Woog JJ, Jahrling KV (1995) Complications of porous spherical orbital implants. Ophthalmology 102(4):586–593
Lovett M, Lee K, Edwards A, Kaplan DL (2009) Vascularization strategies for tissue engineering. Tissue Eng Part B Rev 15(3):353–370. doi:10.1089/ten.TEB.2009.0085
Gong Y, Zhu Y, Liu Y, Ma Z, Gao C, Shen J (2007) Layer-by-layer assembly of chondroitin sulfate and collagen on aminolyzed poly(L-lactic acid) porous scaffolds to enhance their chondrogenesis. Acta Biomater 3(5):677–685. doi:10.1016/j.actbio.2007.04.007
Decher G (1997) Fuzzy nanoassemblies: toward layered polymeric multicomposites. Science 277(5330):1232–1237
Sato M, Ishihara M, Ishihara M, Kaneshiro N, Mitani G, Nagai T, Kutsuna T, Asazuma T, Kikuchi M, Mochida J (2007) Effects of growth factors on heparin-carrying polystyrene-coated atelocollagen scaffold for articular cartilage tissue engineering. J Biomed Mater Res B Appl Biomater 83(1):181–188. doi:10.1002/jbm.b.30782
Jayson GC, Gallagher JT (1997) Heparin oligosaccharides: inhibitors of the biological activity of bFGF on Caco-2 cells. Br J Cancer 75(1):9–16
Soker S, Goldstaub D, Svahn CM, Vlodavsky I, Levi BZ, Neufeld G (1994) Variations in the size and sulfation of heparin modulate the effect of heparin on the binding of VEGF165 to its receptors. Biochem Biophys Res Commun 203(2):1339–1347. doi:10.1006/bbrc.1994.2329
Lu S, Zhang P, Sun X, Gong F, Yang S, Shen L, Huang Z, Wang C (2013) Synthetic ePTFE grafts coated with an anti-CD133 antibody-functionalized heparin/collagen multilayer with rapid in vivo endothelialization properties. ACS Appl Mater Interfaces 5(15):7360–7369. doi:10.1021/am401706w
Liu X, Wang X, Horii A, Wang X, Qiao L, Zhang S, Cui FZ (2012) In vivo studies on angiogenic activity of two designer self-assembling peptide scaffold hydrogels in the chicken embryo chorioallantoic membrane. Nanoscale 4(8):2720–2727. doi:10.1039/c2nr00001f
Zhang K, Li JA, Deng K, Liu T, Chen JY, Huang N (2013) The endothelialization and hemocompatibility of the functional multilayer on titanium surface constructed with type IV collagen and heparin. Colloids Surf B: Biointerfaces 108:295–304. doi:10.1016/j.colsurfb.2012.12.053
Guda T, Walker JA, Singleton B, Hernandez J, Oh DS, Appleford MR, Ong JL, Wenke JC (2014) Hydroxyapatite scaffold pore architecture effects in large bone defects in vivo. J Biomater Appl 28(7):1016–1027. doi:10.1177/0885328213491790
Kalwerisky K, Mihora L, Czyz CN, Foster JA, Holck DE (2013) Rate of vascularization and exposure of silicone-capped porous polyethylene spherical implants: an animal model. Ophthal Plast Reconstr Surg 29(5):350–356. doi:10.1097/IOP.0b013e318295f9c1
Kim HW, Knowles JC, Kim HE (2005) Hydroxyapatite porous scaffold engineered with biological polymer hybrid coating for antibiotic Vancomycin release. J Mater Sci Mater Med 16(3):189–195. doi:10.1007/s10856-005-6679-y
Macarak EJ, Howard PS (1983) Adhesion of endothelial cells to extracellular matrix proteins. J Cell Physiol 116(1):76–86. doi:10.1002/jcp.1041160112
Nanda HS, Chen S, Zhang Q, Kawazoe N, Chen G (2014) Collagen scaffolds with controlled insulin release and controlled pore structure for cartilage tissue engineering. Biomed Res Int 2014:623805. doi:10.1155/2014/623805
Hanjaya-Putra D, Wong KT, Hirotsu K, Khetan S, Burdick JA, Gerecht S (2012) Spatial control of cell-mediated degradation to regulate vasculogenesis and angiogenesis in hyaluronan hydrogels. Biomaterials 33(26):6123–6131. doi:10.1016/j.biomaterials.2012.05.027
Auerbach R, Lewis R, Shinners B, Kubai L, Akhtar N (2003) Angiogenesis assays: a critical overview. Clin Chem 49(1):32–40
Martinez-Madrid B, Donnez J, Van Eyck AS, Veiga-Lopez A, Dolmans MM, Van Langendonckt A (2009) Chick embryo chorioallantoic membrane (CAM) model: a useful tool to study short-term transplantation of cryopreserved human ovarian tissue. Fertil Steril 91(1):285–292. doi:10.1016/j.fertnstert.2007.11.026
Singh S, Wu BM, Dunn JC (2012) Delivery of VEGF using collagen-coated polycaprolactone scaffolds stimulates angiogenesis. J Biomed Mater Res A 100(3):720–727. doi:10.1002/jbm.a.34010
Iruela-Arispe ML, Diglio CA, Sage EH (1991) Modulation of extracellular matrix proteins by endothelial cells undergoing angiogenesis in vitro. Arterioscler Thromb 11(4):805–815
Mao Z, Ma L, Zhou J, Gao C, Shen J (2005) Bioactive thin film of acidic fibroblast growth factor fabricated by layer-by-layer assembly. Bioconjug Chem 16(5):1316–1322. doi:10.1021/bc049755b
Yan Y, Bjonmalm M, Caruso F (2014) Assembly of Layer-by-Layer particles and their interactions with biological systems. Chem Mater 26(1):452–460. doi:10.1021/cm402126n
Shen H, Hu X, Yang F, Bei J, Wang S (2011) Cell affinity for bFGF immobilized heparin-containing poly(lactide-co-glycolide) scaffolds. Biomaterials 32(13):3404–3412. doi:10.1016/j.biomaterials.2011.01.037
Melchiorri AJ, Hibino N, Yi T, Lee YU, Sugiura T, Tara S, Shinoka T, Breuer C, Fisher JP (2015) Contrasting biofunctionalization strategies for the enhanced endothelialization of biodegradable vascular grafts. Biomacromolecules 16(2):437–446. doi:10.1021/bm501853s
Acknowledgments
This work was financially supported by the National “Twelfth Five-Year” Plan for Science & Technology Support of China (2012BAI08B01), Zhejiang Provincial Program for Cultivation of High-Level Innovative Health Talents, The Specialized Key Science & Technology Foundation of Zhejiang Provincial S & T Department (No.2012C13023-2), Zhejiang Key Laboratory fund of China (2011E10006) and Zhejiang Key Innovation Team Project of China (No.2009R50039). We thank Dr. Shaoze Wang (Institute of Translational Medicine, Zhejiang University) for assisting in digital segmentation.
Conflict of Interest
All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest (such as honoraria, educational grants, participation in speakers’ bureaus, membership, employment, consultancies, stock ownership, or other equity interest, expert testimony, or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge, or beliefs) in the subject matter or materials discussed in this manuscript.
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Jin, K., Ye, X., Li, S. et al. A biomimetic collagen/heparin multi-layered porous hydroxyapatite orbital implant for in vivo vascularization studies on the chicken chorioallantoic membrane. Graefes Arch Clin Exp Ophthalmol 254, 83–89 (2016). https://doi.org/10.1007/s00417-015-3144-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-015-3144-6