Abstract
Background
Open fractures are orthopaedic emergencies that carry a high risk for infection, non-union and soft tissue complications. Evidence-based treatment is impeded by the lack of high-quality evidence-based studies. The aim of this investigation was to elucidate the current practice of open fracture management in Germany and to determine major differences in treatment.
Methods
Surgeons were asked to complete an online questionnaire consisting of 45 items developed by an expert consensus. The first part covered questions on general principles of open fracture management. The second part included questions on soft tissue management, the preferred method of initial surgical stabilisation, microbiological testing, employment of pulsatile lavage and local antibiotics, antibiotic regimen, second-look operations, and blood testing.
Results
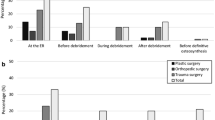
Of 653 respondents, 364 (65 %) completed the first part and 314 (48 %) completed the second part of the online survey. 55 % answered that a standard operating procedure for the diagnosis and treatment of patients with open fractures exists in their hospital. Only 25 % leave pre-hospitalisation applied dressings intact until arrival of the patient in the operating room, and 40 % make this decision depending on information provided by pre-hospitalisation emergency personnel. 84 % participants exclude the use of antibiotic-coated implants in the treatment of open fractures. The favoured stabilisation method in Gustilo type I fractures is definitive internal osteosynthesis and primary wound closure for 61 % of respondents. In Gustilo type II (74 %) and type III fractures (93 %), temporary external fixation is preferred. High-pressure pulsatile lavage is used by 22 % responding surgeons in Gustilo type I fractures, 53 % for type II fractures and 67 % for type III fractures.
Conclusions
Open fracture management differs considerably among surgeons in Germany. Further studies are needed to deliver high-quality evidence concerning primary fracture stabilisation, soft tissue management and second-look operations. Existing evidence-based recommendations for general treatment, antibiotic prophylaxis and soft tissue management should be followed more strictly in clinical practice.




Similar content being viewed by others
References
Khatod M, Botte MJ, Hoyt DB, Meyer RS, Smith JM, Akeson WH (2003) Outcomes in open tibia fractures: relationship between delay in treatment and infection. J Trauma 55(5):949–954. doi:10.1097/01.TA.0000092685.80435.63
Court-Brown CM, Bugler KE, Clement ND, Duckworth AD, McQueen MM (2012) The epidemiology of open fractures in adults. A 15-year review. Injury 43(6):891–897. doi:10.1016/j.injury.2011.12.007
Bosse MJ, MacKenzie EJ, Kellam JF, Burgess AR, Webb LX, Swiontkowski MF, Sanders RW, Jones AL, McAndrew MP, Patterson BM, McCarthy ML, Travison TG, Castillo RC (2002) An analysis of outcomes of reconstruction or amputation after leg-threatening injuries. N Engl J Med 347(24):1924–1931. doi:10.1056/NEJMoa012604
Hoff WS, Bonadies JA, Cachecho R, Dorlac WC (2011) East Practice Management Guidelines Work Group: update to practice management guidelines for prophylactic antibiotic use in open fractures. J Trauma 70(3):751–754. doi:10.1097/TA.0b013e31820930e5
Gustilo RB, Mendoza RM, Williams DN (1984) Problems in the management of type III (severe) open fractures: a new classification of type III open fractures. T J Trauma 24(8):742–746
Oestern HJ, Tscherne H (1984) Pathophysiology and classification of soft tissue injuries associated with fractures. In: Fractures with soft tissue injuries. Springer, Berlin Heidelberg, pp 1–9. doi:10.1007/978-3-642-69499-8_1
Bednar DA, Parikh J (1993) Effect of time delay from injury to primary management on the incidence of deep infection after open fractures of the lower extremities caused by blunt trauma in adults. J Orthop Trauma 7(6):532–535
Patzakis MJ, Wilkins J (1989) Factors influencing infection rate in open fracture wounds. Clin Orthop Relat Res 243:36–40
Gustilo RB, Anderson JT (1976) Prevention of infection in the treatment of one thousand and twenty-five open fractures of long bones: retrospective and prospective analyses. J Bone Joint Surg Am 58(4):453–458
American College of Surgeons (2012) ATLS® for Doctors Student Manual with DVD, 8th edn. ISBN 978-1880696316
Ryan SP, Pugliano V (2014) Controversies in initial management of open fractures. Scand J Surg 103(2):132–137. doi:10.1177/1457496913519773
Brumback RJ, Jones AL (1994) Interobserver agreement in the classification of open fractures of the tibia. The results of a survey of two hundred and forty-five orthopaedic surgeons. J Bone Joint Surg Am 76(8):1162–1166
Beck A, Strecker W (2002) Wunde—fraktur—luxation. Notfall Rettungsmedizin 5(5):613–624. doi:10.1007/s10049-002-0508-3
Cross WW 3rd, Swiontkowski MF (2008) Treatment principles in the management of open fractures. Indian J Orthop 42(4):377–386. doi:10.4103/0019-5413.43373
Giannoudis PV, Papakostidis C, Roberts C (2006) A review of the management of open fractures of the tibia and femur. J Bone Joint Surg Br 88(3):281–289. doi:10.1302/0301-620X.88B3.16465
Schmidmaier G, Lucke M, Wildemann B, Haas NP, Raschke M (2006) Prophylaxis and treatment of implant-related infections by antibiotic-coated implants: a review. Injury 37(Suppl 2):S105–S112. doi:10.1016/j.injury.2006.04.016
Fuchs T, Stange R, Schmidmaier G, Raschke MJ (2011) The use of gentamicin-coated nails in the tibia: preliminary results of a prospective study. Arch Orthop Trauma Surg 131(10):1419–1425. doi:10.1007/s00402-011-1321-6
Metsemakers WJ, Reul M, Nijs S (2015) The use of gentamicin-coated nails in complex open tibia fracture and revision cases: a retrospective analysis of a single centre case series and review of the literature. Injury 46(12):2433–2437. doi:10.1016/j.injury.2015.09.028
Romano CL, Scarponi S, Gallazzi E, Romano D, Drago L (2015) Antibacterial coating of implants in orthopaedics and trauma: a classification proposal in an evolving panorama. J Orthop Surg Res 10:157. doi:10.1186/s13018-015-0294-5
Foote CJ, Guyatt GH, Vignesh KN, Mundi R, Chaudhry H, Heels-Ansdell D, Thabane L, Tornetta P 3rd, Bhandari M (2015) Which surgical treatment for open tibial shaft fractures results in the fewest reoperations? A network meta-analysis. Clin Orthop Relat Res 473(7):2179–2192. doi:10.1007/s11999-015-4224-y
Anglen JO, Apostoles S, Christensen G, Gainor B (1994) The efficacy of various irrigation solutions in removing slime-producing Staphylococcus. J Orthop Trauma 8(5):390–396
Petrisor B, Jeray K, Schemitsch E, Hanson B, Sprague S, Sanders D, Bhandari M, Investigators F (2008) Fluid lavage in patients with open fracture wounds (FLOW): an international survey of 984 surgeons. BMC Musculoskelet Disord 9:7. doi:10.1186/1471-2474-9-7
Investigators Flow, Bhandari M, Jeray KJ, Petrisor BA, Devereaux PJ, Heels-Ansdell D, Schemitsch EH, Anglen J, Della Rocca GJ, Jones C, Kreder H, Liew S, McKay P, Papp S, Sancheti P, Sprague S, Stone TB, Sun X, Tanner SL, Tornetta P 3rd, Tufescu T, Walter S, Guyatt GH (2015) A trial of wound irrigation in the initial management of open fracture wounds. N Engl J Med 373(27):2629–2641. doi:10.1056/NEJMoa1508502
D’Alleyrand JC, Manson TT, Dancy L, Castillo RC, Bertumen JB, Meskey T, O’Toole RV (2014) Is time to flap coverage of open tibial fractures an independent predictor of flap-related complications? J Orthop Trauma 28(5):288–293. doi:10.1097/BOT.0000000000000001
Stannard JP, Singanamala N, Volgas DA (2010) Fix and flap in the era of vacuum suction devices: what do we know in terms of evidence based medicine? Injury 41(8):780–786. doi:10.1016/j.injury.2009.08.011
Stannard JP, Volgas DA, Stewart R, McGwin G Jr, Alonso JE (2009) Negative pressure wound therapy after severe open fractures: a prospective randomized study. J Orthop Trauma 23(8):552–557. doi:10.1097/BOT.0b013e3181a2e2b6
OCEBM Levels of Evidence Working Group (2011) The Oxford Levels of Evidence 2. Oxford Centre for Evidence-Based Medicine. http://www.cebm.net/index.aspx?o=5653
Arti H, Khorami M, Ebrahimi-Nejad V (2016) Comparison of negative pressure wound therapy (NPWT) and conventional wound dressings in the open fracture wounds. Pak J Med Sci 32(1):65–69. doi:10.12669/pjms.321.8568
Okike K, Bhattacharyya T (2006) Trends in the management of open fractures. A critical analysis. J Bone Joint Surg Am 88(12):2739–2748. doi:10.2106/JBJS.F.00146
Gosselin RA, Roberts I, Gillespie WJ (2004) Antibiotics for preventing infection in open limb fractures. Cochrane Database Syst Rev 1:CD003764. doi:10.1002/14651858.CD003764.pub2
Hauser CJ, Adams CA, Eachempati SR Jr, Council of the Surgical Infection S (2006) Surgical Infection Society guideline: prophylactic antibiotic use in open fractures: an evidence-based guideline. Surg Infect (Larchmt) 7(4):379–405. doi:10.1089/sur.2006.7.379
Patzakis MJ, Harvey JP Jr, Ivler D (1974) The role of antibiotics in the management of open fractures. J Bone Joint Surg Am 56(3):532–541
Al-Arabi YB, Nader M, Hamidian-Jahromi AR, Woods DA (2007) The effect of the timing of antibiotics and surgical treatment on infection rates in open long-bone fractures: a 9-year prospective study from a district general hospital. Injury 38(8):900–905. doi:10.1016/j.injury.2007.02.043
Lee C, Porter KM (2005) Prehospital management of lower limb fractures. Emerg Med J 22(9):660–663. doi:10.1136/emj.2005.024489
Grosse A, Christie J, Taglang G, Court-Brown C, McQueen M (1993) Open adult femoral shaft fracture treated by early intramedullary nailing. J Bone Joint Surg Br 75(4):562–565
Bhandari M, Schemitsch EH, Adili A, Lachowski RJ, Shaughnessy SG (1999) High and low pressure pulsatile lavage of contaminated tibial fractures: an in vitro study of bacterial adherence and bone damage. J Orthop Trauma 13(8):526–533
Adili A, Bhandari M, Schemitsch EH (2002) The biomechanical effect of high-pressure irrigation on diaphyseal fracture healing in vivo. J Orthop Trauma 16(6):413–417
Bhandari M, Adili A, Lachowski RJ (1998) High pressure pulsatile lavage of contaminated human tibiae: an in vitro study. J Orthop Trauma 12(7):479–484
Krug E, Berg L, Lee C, Hudson D, Birke-Sorensen H, Depoorter M, Dunn R, Jeffery S, Duteille F, Bruhin A, Caravaggi C, Chariker M, Dowsett C, Ferreira F, Martinez JM, Grudzien G, Ichioka S, Ingemansson R, Malmsjo M, Rome P, Vig S, Runkel N, Martin R, Smith J, International Expert Panel on Negative Pressure Wound T (2011) Evidence-based recommendations for the use of Negative Pressure Wound Therapy in traumatic wounds and reconstructive surgery: steps towards an international consensus. Injury 42(Suppl 1):S1–12. doi:10.1016/S0020-1383(11)00041-6
Vasenius J, Tulikoura I, Vainionpaa S, Rokkanen P (1998) Clindamycin versus cloxacillin in the treatment of 240 open fractures. A randomized prospective study. Ann Chir Gynaecol 87(3):224–228
Huddleston PM, Steckelberg JM, Hanssen AD, Rouse MS, Bolander ME, Patel R (2000) Ciprofloxacin inhibition of experimental fracture healing. J Bone Joint Surg Am 82(2):161–173
Holtom PD, Pavkovic SA, Bravos PD, Patzakis MJ, Shepherd LE, Frenkel B (2000) Inhibitory effects of the quinolone antibiotics trovafloxacin, ciprofloxacin, and levofloxacin on osteoblastic cells in vitro. J Orthop Res 18(5):721–727. doi:10.1002/jor.1100180507
Gopal S, Majumder S, Batchelor AG, Knight SL, De Boer P, Smith RM (2000) Fix and flap: the radical orthopaedic and plastic treatment of severe open fractures of the tibia. J Bone Joint Surg Br 82(7):959–966
Acknowledgments
The authors would like to acknowledge all members of the Sektion NIS of the German Trauma Society (DGU) who gave their thoughtful comments during survey initiation and internal presentations.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors deny any conflict of interest.
Financial disclosure
All authors disclose any funding received for this work by the following organisations: National Institute of Health (NIH); Wellcome Trust; and the Howard Hughes Medical Institute (HHMI).
Rights and permissions
About this article
Cite this article
Gümbel, D., Matthes, G., Napp, M. et al. Current management of open fractures: results from an online survey. Arch Orthop Trauma Surg 136, 1663–1672 (2016). https://doi.org/10.1007/s00402-016-2566-x
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-016-2566-x