Abstract
Introduction
Spinal epidural hematomas are uncommon in children. The diagnosis can be elusive as most cases present without a history of trauma, while symptoms can be atypical.
Case Report
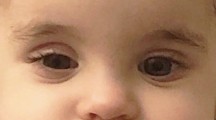
We encountered a 35-month-old male presenting with nonspecific symptoms and no history of trauma. He later developed unilateral miosis and ptosis; MRI discovered a subacute cervicothoracic epidural which was promptly evacuated. The patient made an excellent recovery.
Coclusions
We emphasize the frequent absence of identifiable trauma and the importance of thorough imaging when this entity is suspected. Miosis and ptosis, likely representing a partial Horner syndrome, is an extremely rare presentation, this being one of the only reported cases.



Similar content being viewed by others
References
Babayev R, Ekşi MŞ (2016) Spontaneous thoracic epidural hematoma: a case report and literature review. Childs Nerv Syst 32(1):181–187. https://doi.org/10.1007/s00381-015-2768-5
Cakir E, Karaarslan G, Usul H, Baykal S, Kuzeyli K, Mungan I, Yazar U, Peksoylu B, Aynaci M, Cakir F (2004) Clinical course of spontaneous spinal epidural hematoma mimicking Guillain-Barré syndrome in a child: a case report and literature review. Dev Med Child Neurol 46(12):838–842
Caldarelli M, Di Rocco C, La Marca F (1994) Spontaneous spinal epidural hematoma in toddlers: description of two cases and review of the literature. Surg Neurol 41:325–329
Chang FC, Lirng JF, Luo CB, Yen YS, Guo WY, Teng MM et al (2005) Evaluation of clinical and MR findings for the prognosis of spinal epidural hematomas. Clin Radiol 60(7):762–770. https://doi.org/10.1016/j.crad.2004.12.008
Cooper DW (1967) Spontaneous spinal epidural hematoma: case report. J Neurosurg 26(3):343–345. https://doi.org/10.3171/jns.1967.26.3.0343
Cuenca PJ, Tulley EB, Devita D, Stone A (2004) Delayed traumatic spinal epidural hematoma with spontaneous resolution of symptoms. J Emerg Med 27(1):37–41. https://doi.org/10.1016/j.jemermed.2004.02.008
Domenicucci M, Mancarella C, Santoro G, Dugoni DE, Ramieri A, Arezzo MF, Missori P (2017) Spinal epidural hematomas: personal experience and literature review of more than 1000 cases. J Neurosurgery Spine 27(2):1–11
Groen RJ (2010) Hemophilia A and spinal epidural hematoma in children. Neuropediatrics 41(3):154–154. https://doi.org/10.1055/s-0030-1265155
Holtas S, Heiling M, Lonntoft M (1996) Spontaneous spinal epidural hematoma: findings at MR imaging and clinical correlation. Radiology 199:409–413
Jumani DB, Littlewood R, Iyer A, Fellows G, Healey A, Abernethy L, Spinty S, Sarginson R, Pettorini B (2013) Spontaneous spinal epidural hematoma mimicking meningitis in a 2-year-old child: a case report and literature review. Childs Nerv Syst 29(10):1795–1798. https://doi.org/10.1007/s00381-013-2130-8
Kreppel D, Antoniadis G, Seeling W (2003) Spinal hematoma: a literature survey with meta-analysis of 613 patients. Neurosurg Rev 26(1):1–49
Lee JH, Lee HK, Lee DH, Choi CG, Kim SJ, Suh DC (2007) Neuroimaging strategies for three types of Horner syndrome with emphasis on anatomic location. AJR Am J Roentgenol 188(1):W74–W81. https://doi.org/10.2214/AJR.05.1588
Narawong D, Gibbons VP, McLaughlin JR, Bouhasin JD, Kotegal S (1988) Conservative management of spinal epidural hematoma in hemophilia. Pediatr Neurol 4(3):169–171. https://doi.org/10.1016/0887-8994(88)90006-9
Pollard ZF, Greenberg MF, Bordenca M (2010) Atypical acquired pediatric Horner syndrome. Arch Ophthalmol 128(7):937–940. https://doi.org/10.1001/archophthalmol.2010.119
Pomeranz J (2002) Isolated Horner syndrome and syrinx of the cervical spinal cord. Am J Ophthalmol 133(5):702–704. https://doi.org/10.1016/S0002-9394(02)01340-5
Raimondi AJ, Gutierrez FA, Di Rocco C (1976) Laminotomy and total reconstruction of the posterior spinal arch for spinal canal surgery in childhood. J Neurosurg 45(5):555–560. https://doi.org/10.3171/jns.1976.45.5.0555
Rechtine GR 2nd, Bolesta MJ, Chrin AM, Louis K (2001) Spontaneous resolution of symptomatic post-traumatic cervical epidural hematoma: a case report. J Bone Joint Surg Am 83(2):255–258. https://doi.org/10.2106/00004623-200102000-00014
Robertson WC, Lee YE, Edmonson MB (1979) Spontaneous spinal epidural hematoma in the young. Neurology 29(1):120–122. https://doi.org/10.1212/WNL.29.1.120
Schoonjans AS, De Dooy J, Kenis S, Menovsky T, Verhulst S, Hellinckx J, van Ingelghem I, Parizel PM, Jorens PG, Ceulemans B (2013) Spontaneous spinal epidural hematoma in infancy: review of the literature and the “seventh” case report. Eur J Paediatr Neurol 17(6):537–542. https://doi.org/10.1016/j.ejpn.2013.05.012
Sim HB, Weon YC, Park JB, Yang DS (2010) Chronic traumatic spinal epidural hematoma in a child. Am J Phys Med Rehabil 89(11):936–940. https://doi.org/10.1097/PHM.0b013e3181ec9689
Smeets N, van den Akker M, Peters B, Vanderhasselt T, Jansen A (2016) Spontaneous spinal epidural hematoma in two toddlers: diagnostic pitfalls. Pediatric Dimensions 1(6):3–3
Tailor J, Dunn IF, Smith E (2006) Conservative treatment of spontaneous spinal epidural hematoma associated with oral anticoagulant therapy in a child. Childs Nerv Syst 22(12):1643–1645. https://doi.org/10.1007/s00381-006-0220-6
Watanabe T (2006) Traumatic spinal epidural hematoma without bone disruption. Eur J Pediatr 165(4):278–279. https://doi.org/10.1007/s00431-005-0038-3
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Additional information
This work has not been previously presented or published in any form.
Rights and permissions
About this article
Cite this article
Root, B.K., Schartz, D.A., Calnan, D.R. et al. Cervicothoracic epidural hematoma in a toddler with miosis, ptosis, nonspecific symptoms, and no history of major trauma: case report. Childs Nerv Syst 34, 1259–1262 (2018). https://doi.org/10.1007/s00381-018-3736-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-018-3736-7