Abstract
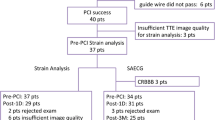
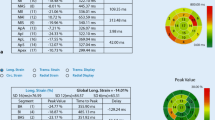
Percutaneous coronary interventions (PCIs) are increasingly being used to treat unprotected left main coronary artery (ULMCA) lesions. However, research is sparse on the acute changes of left ventricular (LV) hemodynamics and function during PCI in patients with ULMCA stenosis. We aimed to assess the acute changes of LV function using speckle-tracking imaging during PCI in these patients. Fifteen consecutive patients who underwent elective PCI for ULMCA stenosis were enrolled. Echocardiographic studies and pressure measurement were performed at baseline, during PCI and after PCI. LMCA occlusion with a first balloon inflation induced a marked reduction in the peak positive derivative of LV pressure (dP/dt max), LV global longitudinal strain (GLS), and systolic and diastolic strain rates, and a marked increase in LV end-diastolic pressure (EDP) (all P < 0.01). During the second inflation, the degrees of LV hemodynamic and functional changes were similar to those of the first inflation, even with a higher inflation pressure. During the third inflation, the values of GLS and dP/dt max were higher than those of the second inflation (P = 0.03 and P = 0.05, respectively). After optimal PCI, dP/dt max, LVEDP, and strain parameters were improved to baseline values. LV hemodynamics and function were considerably impaired with the first ballooning during PCI for ULMCA stenosis. However, the degrees of LV hemodynamic and functional changes decreased with each successive balloon inflation, which can be explained by ischemic preconditioning. After all procedures were safely completed, LV systolic function was improved without LV diastolic stunning.



Similar content being viewed by others
References
Yusuf S, Zucker D, Peduzzi P, Fisher LD, Takaro T, Kennedy JW, Davis K, Killip T, Passamani E, Norris R (1994) Effect of coronary artery bypass graft surgery on survival: overview of 10-year results from randomised trials by the Coronary Artery Bypass Graft Surgery Trialists Collaboration. Lancet 344:563–570
Agostoni P, Valgimigli M, Van Mieghem CA, Rodriguez-Granillo GA, Aoki J, Ong AT, Tsuchida K, McFadden EP, Ligthart JM, Smits PC, de Jaegere P, Sianos G, Van der Giessen WJ, De Feyter P, Serruys PW (2005) Comparison of early outcome of percutaneous coronary intervention for unprotected left main coronary artery disease in the drug-eluting stent era with versus without intravascular ultrasonic guidance. Am J Cardiol 95:644–647
Chieffo A, Stankovic G, Bonizzoni E, Tsagalou E, Iakovou I, Montorfano M, Airoldi F, Michev I, Sangiorgi MG, Carlino M, Vitrella G, Colombo A (2005) Early and mid-term results of drug-eluting stent implantation in unprotected left main. Circulation 111:791–795
Pepe M, Napodano M, Tarantini G, Fraccaro C, Cutolo A, Peluso D, Isabella G, Ramondo A, Iliceto S (2011) Percutaneous coronary intervention for unprotected left main disease in very high risk patients: safety of drug-eluting stents. Heart Vessels 26:17–24
Theroux P, Franklin D, Ross J Jr, Kemper WS (1974) Regional myocardial function during acute coronary artery occlusion and its modification by pharmacologic agents in the dog. Circ Res 35:896–908
Villarreal FJ, Lew WY, Waldman LK, Covell JW (1991) Transmural myocardial deformation in the ischemic canine left ventricle. Circ Res 68:368–381
Kukulski T, Jamal F, Herbots L, D’Hooge J, Bijnens B, Hatle L, De Scheerder I, Sutherland GR (2003) Identification of acutely ischemic myocardium using ultrasonic strain measurements: a clinical study in patients undergoing coronary angioplasty. J Am Coll Cardiol 41:810–819
Kukulski T, Jamal F, D’Hooge J, Bijnens B, De Scheerder I, Sutherland GR (2002) Acute changes in systolic and diastolic events during clinical coronary angioplasty: a comparison of regional velocity, strain rate, and strain measurement. J Am Soc Echocardiogr 15:1–12
Pirat B, Khoury DS, Hartley CJ, Tiller L, Rao L, Schulz DG, Nagueh SF, Zoghbi WA (2008) A novel feature-tracking echocardiographic method for the quantitation of regional myocardial function: validation in an animal model of ischemia-reperfusion. J Am Coll Cardiol 51:651–659
Urheim S, Edvardsen T, Torp H, Angelsen B, Smiseth OA (2000) Myocardial strain by Doppler echocardiography: validation of a new method to quantify regional myocardial function. Circulation 102:1158–1164
Hoshi H, Takagi A, Uematsu S, Ashihara K, Hagiwara N (2013) Risk stratification of patients with non-ST-elevation acute coronary syndromes by assessing global longitudinal strain. Heart Vessels. doi:10.1007/s00380-013-0361-y
Steendijk P, Tulner SA, Bax JJ, Oemrawsingh PV, Bleeker GB, van Erven L, Putter H, Verwey HF, van der Wall EE, Schalij MJ (2006) Hemodynamic effects of long-term cardiac resynchronization therapy: analysis by pressure–volume loops. Circulation 113:1295–1304
Kelly RP, Ting CT, Yang TM, Liu CP, Maughan WL, Chang MS, Kass DA (1992) Effective arterial elastance as index of arterial vascular load in humans. Circulation 86:513–521
Sunagawa K, Maughan WL, Burkhoff D, Sagawa K (1983) Left ventricular interaction with arterial load studied in isolated canine ventricle. Am J Physiol 245:H773–H780
Lang RM, Bierig M, Devereux RB, Flachskampf FA, Foster E, Pellikka PA, Picard MH, Roman MJ, Seward J, Shanewise JS, Solomon SD, Spencer KT, Sutton MS, Stewart WJ (2005) Recommendations for chamber quantification: a report from the American Society of Echocardiography’s Guidelines and Standards Committee and the Chamber Quantification Writing Group, developed in conjunction with the European Association of Echocardiography, a branch of the European Society of Cardiology. J Am Soc Echocardiogr 18:1440–1463
Murry CE, Jennings RB, Reimer KA (1986) Preconditioning with ischemia: a delay of lethal cell injury in ischemic myocardium. Circulation 74:1124–1136
Cohen MV, Baines CP, Downey JM (2000) Ischemic preconditioning: from adenosine receptor to KATP channel. Annu Rev Physiol 62:79–109
Downey JM, Yellon DM (1997) The biology of preconditioning. In: Heyndrickx GR, Vatner SF, Wijns W (eds) Stunning, hibernation, and preconditioning: clinical pathophysiology of myocardial ischemia. Lippincott-Raven, Philadelphia, pp 105–119
Fryer RM, Hsu AK, Gross GJ (2001) Mitochondrial K(ATP) channel opening is important during index ischemia and following myocardial reperfusion in ischemic preconditioned rat hearts. J Mol Cell Cardiol 33:831–834
Cabiati M, Martino A, Mattii L, Caselli C, Prescimone T, Lionetti V, Morales MA, Del Ry S (2013) Adenosine receptor expression in an experimental animal model of myocardial infarction with preserved left ventricular ejection fraction. Heart Vessels. doi:10.1007/s00380-013-0380-8
Deutsch E, Berger M, Kussmaul WG, Hirshfeld JW Jr, Herrmann HC, Laskey WK (1990) Adaptation to ischemia during percutaneous transluminal coronary angioplasty: clinical, hemodynamic, and metabolic features. Circulation 82:2044–2051
Tomai F, Crea F, Gaspardone A, Versaci F, Esposito C, Chiariello L, Gioffrè PA (1993) Mechanisms of cardiac pain during coronary angioplasty. J Am Coll Cardiol 22:1892–1896
Argaud L, Rioufol G, Lièvre M, Bontemps L, Legalery P, Stumpf M, Finet G, Itti R, André-Fouët X, Ovize M (2004) Preconditioning during coronary angioplasty: no influence of collateral perfusion or the size of the area at risk. Eur Heart J 25:2019–2025
Kloner RA, Yellon D (1994) Does ischemic preconditioning occur in patients? J Am Coll Cardiol 24:1133–1142
Kloner RA, Jennings RB (2001) Consequences of brief ischemia: stunning, preconditioning, and their clinical implications: part 2. Circulation 104:3158–3167
Dupouy P, Geschwind H, Pelle G, Aptecar E, Hittinger L, El Ghalid A, Dubois-Randé JL (1996) Repeated coronary artery occlusions during routine balloon angioplasty do not induce myocardial preconditioning in humans. J Am Coll Cardiol 27:1374–1380
Liang HY, Cauduro S, Pellikka P, Wang J, Urheim S, Yang EH, Rihal C, Belohlavek M, Khandheria B, Miller FA, Abraham TP (2006) Usefulness of two-dimensional speckle strain for evaluation of left ventricular diastolic deformation in patients with coronary artery disease. Am J Cardiol 98:1581–1586
Bonow RO, Vitale DF, Bacharach SL, Frederick TM, Kent KM, Green MV (1985) Asynchronous left ventricular regional function and impaired global diastolic filling in patients with coronary artery disease: reversal after coronary angioplasty. Circulation 71:297–307
Wijns W, Serruys PW, Slager CJ, Grimm J, Krayenbuehl HP, Hugenholtz PG, Hess OM (1986) Effect of coronary occlusion during percutaneous transluminal angioplasty in humans on left ventricular chamber stiffness and regional diastolic pressure–radius relations. J Am Coll Cardiol 7:455–463
Miyamoto MI, Rose GA, Weissman NJ, Guerrero JL, Semigran MJ, Picard MH (1999) Abnormal global left ventricular relaxation occurs early during the development of pharmacologically induced ischemia. J Am Soc Echocardiogr 12:113–120
Azevedo CF, Amado LC, Kraitchman DL, Gerber BL, Osman NF, Rochitte CE, Edvardsen T, Lima JA (2004) Persistent diastolic dysfunction despite complete systolic functional recovery after reperfused acute myocardial infarction demonstrated by tagged magnetic resonance imaging. Eur Heart J 25:1419–1427
Ishii K, Imai M, Suyama T, Maenaka M, Nagai T, Kawanami M, Seino Y (2009) Exercise-induced post-ischemic left ventricular delayed relaxation or diastolic stunning: is it a reliable marker in detecting coronary artery disease? J Am Coll Cardiol 53:698–705
Ishii K, Suyama T, Imai M, Maenaka M, Yamanaka A, Makino Y, Seino Y, Shimada K, Yoshikawa J (2009) Abnormal regional left ventricular systolic and diastolic function in patients with coronary artery disease undergoing percutaneous coronary intervention: clinical significance of post-ischemic diastolic stunning. J Am Coll Cardiol 54:1589–1597
Acknowledgments
The authors thank Jun-Won Kang, Yo-Won Lee, and Ra-Seung Lim at the cardiac catheterization laboratory for their skilled assistance.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Park, SM., Ahn, CM., Hong, SJ. et al. Acute changes of left ventricular hemodynamics and function during percutaneous coronary intervention in patients with unprotected left main coronary artery disease. Heart Vessels 30, 432–440 (2015). https://doi.org/10.1007/s00380-014-0495-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00380-014-0495-6