Abstract
Objective
To retrospectively assess the frequency and indications for emergency pancreatoduodenctomies in a tertiary referral center.
Methods
Pancreatoduodenectomies between January 2005 and January 2014 were retrospectively assessed for emergency indications defined as surgery following unplanned hospital admission in less than 24 h. Data on indications and on the intraoperative as well as the post-operative course were collected.
Results
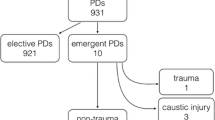
Out of 583 pancreatoduodenectomies during the interval, a total of 10 (1.7 %) were performed as an emergency surgery. Indications included uncontrollable bleeding, duodenal and proximal jejunal perforations, and endoscopic retrograde cholangiopancreatography-related complications. Three of the 10 (30.0 %) patients died during the hospital course. In one patient, an intraoperative mass transfusion was necessary. No intraoperative death occurred. All but one patient were American Society of Anesthesiologists class three or higher. In two cases, the pancreatic remnant was left without anastomosis for second-stage pancreatojejunostomy. Median operation time was 326.5 min (SD 100.3 min). Hospital stay of the surviving patients was prolonged (median 43.0 days; SD 24.0 days).
Conclusion
Emergency pancreatoduodenectomies are non-frequent, have a diverse range of indications and serve as an ultima ratio to cope with severe injuries and complications around the pancreatic head area.
Similar content being viewed by others
References
Mezhir JJ (2013) Management of complications following pancreatic resection: an evidence-based approach. J Surg Oncol 107:58–66
Asensio JA, Petrone P, Roldan G et al (2003) Pancreaticoduodenectomy: a rare procedure for the management of complex pancreaticoduodenal injuries. J Am Coll Surg 197:937–942
Lin BC, Chen RJ, Fang JF et al (2004) Management of blunt major pancreatic injury. J Trauma 56:774–778
Lin BC, Fang JF, Wong YC et al (2007) Blunt pancreatic trauma and pseudocyst: management of major pancreatic duct injury. Injury 38:588–593
Z’Graggen K, Strobel O, Schmied BM et al (2002) Emergency pancreatoduodenectomy in nontrauma patients. Pancreas 24:258–263
Standop J, Glowka T, Schmitz V et al (2010) Emergency Kausch-Whipple procedure: indications and experiences. Pancreas 39:156–159
Ragulin-Coyne E, Witkowski ER, Chau Z, et al (2013) National trends in pancreaticoduodenal trauma: interventions and outcomes. HPB
Velmahos GC, Tabbara M, Gross R et al (2009) Blunt pancreatoduodenal injury: a multicenter study of the Research Consortium of New England Centers for Trauma (ReCONECT). Arch Surg 144:413–419 (discussion 419–420)
Parray FQ, Lone IM, Chowdri NA et al (2011) Emergency pancreaticoduodenectomy in duodenal paraganglioma: case report. ISRN Surg 2011:268674
Stratigos P, Kouskos E, Kouroglou M et al (2007) Emergency pancreatoduodenectomy (whipple procedure) for massive upper gastrointestinal bleeding caused by a diffuse B-cell lymphoma of the duodenum: report of a case. Surg Today 37:680–684
Maeda H, Okabayashi T, Kobayashi M et al (2006) Emergency pancreatoduodenectomy for pancreatic metastasis from renal cell carcinoma in a patient with von Hippel-Lindau disease: a case report. Dig Dis Sci 51:1383–1387
Sakakima Y, Inoue S, Fujii T et al (2004) Emergency pylorus-preserving pancreatoduodenectomy followed by second-stage pancreatojejunostomy for a gastrointestinal stromal tumor of the duodenum with an intratumoral gas figure: report of a case. Surg Today 34:701–705
Zittel TT, Jehle EC, Becker HD (2000) Surgical management of peptic ulcer disease today–indication, technique and outcome. Langenbeck’s Arch Surg 385:84–96
Udd M, Leppaniemi AK, Bidel S et al (2007) Treatment of bleeding pseudoaneurysms in patients with chronic pancreatitis. World J Surg 31:504–510. doi:10.1007/s00268-006-0209-z
Sato N, Yamaguchi K, Shimizu S et al (1998) Coil embolization of bleeding visceral pseudoaneurysms following pancreatectomy: the importance of early angiography. Arch Surg 133:1099–1102
Blanc T, Cortes A, Goere D et al (2007) Hemorrhage after pancreaticoduodenectomy: when is surgery still indicated? Am J Surg 194:3–9
Choi SH, Moon HJ, Heo JS et al (2004) Delayed hemorrhage after pancreaticoduodenectomy. J Am Coll Surg 199:186–191
Druart ML, Van Hee R, Etienne J et al (1997) Laparoscopic repair of perforated duodenal ulcer. A prospective multicenter clinical trial. Surg Endosc 11:1017–1020
Lunevicius R, Morkevicius M (2005) Management strategies, early results, benefits, and risk factors of laparoscopic repair of perforated peptic ulcer. World J Surg 29:1299–1310. doi:10.1007/s00268-005-7705-4
Anderson MA, Fisher L et al (2012) Complications of ERCP. Gastrointestinal endoscopy 75:467–473
Salminen P, Laine S, Gullichsen R (2008) Severe and fatal complications after ERCP: analysis of 2555 procedures in a single experienced center. Surg Endosc 22:1965–1970
Lai CH, Lau WY (2008) Management of endoscopic retrograde cholangiopancreatography-related perforation. Surgeon 6:45–48
Enns R, Eloubeidi MA, Mergener K et al (2002) ERCP-related perforations: risk factors and management. Endoscopy 34:293–298
Miyagawa S, Makuuchi M, Kawasaki S et al (1994) Second-stage pancreatojejunostomy following pancreatoduodenectomy in high-risk patients. Am J Surg 168:66–68
Cho A, Arita S, Koike N et al (2005) Two-staged hepato-pancreatoduodenectomy and interventional pancreaticojejunostomy. Hepatogastroenterology 52:1886–1888
Gupta V, Wig JD, Garg H (2008) Trauma pancreaticoduodenectomy for complex pancreaticoduodenal injury. Delayed reconstruction. JOP: J Pancreas 9:618–623
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The author has no conflict of interest.
Rights and permissions
About this article
Cite this article
Nentwich, M.F., Reeh, M., Uzunoglu, F.G. et al. Non-trauma Emergency Pancreatoduodenectomies: A Single-Center Retrospective Analysis. World J Surg 40, 2261–2266 (2016). https://doi.org/10.1007/s00268-016-3525-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-016-3525-y