Abstract
Background
The surgical management of papillary thyroid microcarcinoma (PTMC), especially regarding the necessity of central lymph node dissection (CLND), remains controversial. This meta-analysis was conducted to investigate the clinicopathologic factors predictive of central compartment lymph node metastasis (CLNM) in patients diagnosed with PTMC.
Methods
PubMed, EMBASE, Ovid, Web of Science, and the Cochrane Library were searched from their inception to September 2013. Published studies that explored the association between clinicopathologic factors and CLNM in PTMC patients were included. From the identified studies, we extracted the number of individuals with or without each risk factor to calculate the CLNM-positive proportions and used fixed/random-effects models for the meta-analyses of overall relative risk (RR). The pooling analysis on the association between CLNM or the different CLNDs and prognosis was also conducted.
Results
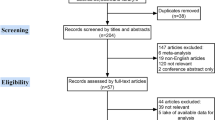
A total of 19 eligible studies that included 8345 patients were identified. Three studies did therapeutic CLND, while the other 16 studies performed prophylactic CLND in PTMC patients. Meta-analyses revealed that CLNM was associated with male gender (RR = 1.36; 95 % CI 1.22–1.52, p = 0.001), younger age (<45 years; RR = 1.15; 95 % CI 1.04–1.27, p = 0.006), larger tumor size (>5 mm; RR = 1.51 95 % CI 1.32–1.65, p = 0.001), multifocality (RR = 1.40; 95 % CI 1.27–1.54, p = 0.001), and extrathyroidal extension (RR = 1.81; 95 % CI 1.34–2.43, p = 0.001). Meta-regression analysis indicated that a disparity in the proportion of PTMC patients with CLNM in each study was the main factor resulting in heterogeneity among the 19 studies. In addition, the pooling analyses suggested that CLNM did not significantly predict neck recurrences [hazard ratio (HR) = 0.95, 95 % CI 0.67–1.22, p = 0.054], and the prophylactic CLND group did not improve local control significantly compared to the therapeutic group (RR = 0.96, 95 % CI 0.46–2.01, p = 0.544).
Conclusion
Prophylactic CLND may be performed in PTMC patients with clinically uninvolved central lymph nodes but with high risk factors; multicenter studies with long-term follow-up are recommended to better understand the risk factors and surgical management for central nodes in PTMC.








Similar content being viewed by others
Abbreviations
- DTC:
-
Differentiated thyroid cancer
- PTC:
-
Papillary thyroid cancer
- PTMC:
-
Papillary thyroid microcarcinoma
- ETE:
-
Extrathyroidal extension
- US:
-
Ultrasonography
- FNA:
-
Fine-needle aspiration
- CLNM:
-
Central lymph node metastasis
- CLND:
-
Central lymph node dissection
- ATA:
-
American Thyroid Association
- AJCC:
-
American Joint Committee on Cancer
- RR:
-
Relative risk
- CI:
-
Confidence interval
References
Hedinger C, Williams ED, Sobin LH (1989) The WHO histological classification of thyroid tumors: a commentary on the second edition. Cancer 63(908–91):1
Chen AY, Jemal A, Ward EM (2009) Increasing incidence of differentiated thyroid cancer in the United States, 1988-2005. Cancer 115:3801–3807
Grebe SK, Hay ID (1996) Thyroid cancer nodal metastases: biologic significance and therapeutic considerations. Surg Oncol Clin N Am 5:43–63
Ito Y, Uruno T, Nakano K et al (2003) An observation trial without surgical treatment in patients with papillary microcarcinoma of the thyroid. Thyroid 13:381–387
Cooper DS, Doherty GM, Haugen BR et al (2009) Revised American Thyroid Association management guidelines for patients with thyroid nodules and differentiated thyroid cancer. Thyroid 19:1167–1214
Haugen BR, Alexander EK, Bible KC et al (2014) American Thyroid Association Management Guidelines for Patients with Thyroid Nodules and Differentiated Thyroid Cancer ATA guidelines recommendations are taken from an ATA Satellite meeting in Chicago in June 2014, and may differ from the final published version
Roh JL, Park JY, Park CI (2009) Prevention of postoperative hypocalcemia with routine oral calcium and vitamin D supplements in patients with differentiated papillary thyroid carcinoma undergoing total thyroidectomy plus central neck dissection. Cancer 115:251–258
Leboulleux S, Girard E, Rose M et al (2007) Ultrasound criteria of malignancy for cervical lymph nodes in patients followed up for differentiated thyroid cancer. J Clin Endocrinol Metab 92:3590–3594
Stang A (2010) Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol 25:603–605
Zhou YL, Gao EL, Zhang W et al (2012) Factors predictive of papillary thyroid micro-carcinoma with bilateral involvement and central lymph node metastasis: a retrospective study. World J Surg Oncol 10:67
Moon HJ, Kim EK, Yoon JH et al (2012) Clinical implication of elastography as a prognostic factor of papillary thyroid microcarcinoma. Ann Surg Oncol 19:2279–2287
Kim TY, Hong SJ, Kim JM et al (2008) Prognostic parameters for recurrence of papillary thyroid microcarcinoma. BMC Cancer 8:296
Moon HJ, Kim EK, Chung WY et al (2011) Minimal extrathyroidal extension in patients with papillary thyroid microcarcinoma: is it a real prognostic factor? Ann Surg Oncol 18:1916–1923
So YK, Son YI, Hong SD et al (2010) Subclinical lymph node metastasis in papillary thyroid microcarcinoma: a study of 551 resections. Surgery 148:526–531
Zheng X, Wei S, Han Y et al (2013) Papillary microcarcinoma of the thyroid: clinical characteristics and BRAF(V600E) mutational status of 977 cases. Ann Surg Oncol 20:2266–2273
Zhao Q, Ming J, Liu C et al (2013) Multifocality and total tumor diameter predict central neck lymph node metastases in papillary thyroid microcarcinoma. Ann Surg Oncol 20:746–752
Lee J, Park JH, Lee CR et al (2013) Long-Term Outcomes of Total Thyroidectomy Versus Thyroid Lobectomy for Papillary Thyroid Microcarcinoma: Comparative Analysis After Propensity Score Matching Thyroid
Lee HS, Park HS, Kim SW et al (2013) Clinical characteristics of papillary thyroid microcarcinoma less than or equal to 5 mm on ultrasonography. Eur Arch Otorhinolaryngol 270:2969–2974
Kim KE, Kim EK, Yoon JH et al (2013) Preoperative prediction of central lymph node metastasis in thyroid papillary microcarcinoma using clinicopathologic and sonographic features. World J Surg 37:385–391. doi:10.1007/s00268-012-1826-3
Zhang L, Wei WJ, Ji QH et al (2012) Risk factors for neck nodal metastasis in papillary thyroid microcarcinoma: a study of 1066 patients. J Clin Endocrinol Metab 97:1250–1257
Kim BY, Jung CH, Kim JW et al (2012) Impact of clinicopathologic factors on subclinical central lymph node metastasis in papillary thyroid microcarcinoma. Yonsei Med J 53:924–930
Hyun SM, Song HY, Kim SY et al (2012) Impact of combined prophylactic unilateral central neck dissection and hemithyroidectomy in patients with papillary thyroid microcarcinoma. Ann Surg Oncol 19:591–596
Caliskan M, Park JH, Jeong JS et al (2012) Role of prophylactic ipsilateral central compartment lymph node dissection in papillary thyroid microcarcinoma. Endocr J 59:305–311
Lee KJ, Cho YJ, Kim SJ et al (2011) Analysis of the clinicopathologic features of papillary thyroid microcarcinoma based on 7-mm tumor size. World J Surg 35:318–323. doi:10.1007/s00268-010-0886-5
Ogilvie JB, Patel KN, Heller KS (2010) Impact of the 2009 American Thyroid Association guidelines on the choice of operation for well-differentiated thyroid microcarcinomas. Surgery 148:1222–1226 discussion 1226–1227
Lim YC, Choi EC, Yoon YH et al (2009) Central lymph node metastases in unilateral papillary thyroid microcarcinoma. Br J Surg 96:253–257
Lee SH, Lee SS, Jin SM et al (2008) Predictive factors for central compartment lymph node metastasis in thyroid papillary microcarcinoma. Laryngoscope 118:659–662
Wada N, Duh QY, Sugino K et al (2003) Lymph node metastasis from 259 papillary thyroid microcarcinomas: frequency, pattern of occurrence and recurrence, and optimal strategy for neck dissection. Ann Surg 237:399–407
Miccoli P, Minuto MN, Ugolini C et al (2007) Intrathyroidal differentiated thyroid carcinoma: tumor size-based surgical concepts. World J Surg 31:888–894
Lang BH, Lo CY, Chan WF et al (2007) Staging systems for papillary thyroid carcinoma: a review and comparison. Ann Surg 245:366–378
Lee J, Park JH, Lee CR et al (2013) Long-term outcomes of total thyroidectomy versus thyroid lobectomy for papillary thyroid microcarcinoma: comparative analysis after propensity score matching. Thyroid 23:1408–1415
Mercante G, Frasoldati A, Pedroni C et al (2009) Prognostic factors affecting neck lymph node recurrence and distant metastasis in papillary microcarcinoma of the thyroid: results of a study in 445 patients. Thyroid 19:707–716
Acknowledgments
This research was supported by Grants from the Key Project of Science and Technology Commission of Shanghai Municipality (11DJ1400200).
Conflict of interest
The authors have nothing to disclose.
Author information
Authors and Affiliations
Corresponding author
Additional information
Ning Qu and Ling Zhang contributed equally to this work.
Rights and permissions
About this article
Cite this article
Qu, N., Zhang, L., Ji, Qh. et al. Risk Factors for Central Compartment Lymph Node Metastasis in Papillary Thyroid Microcarcinoma: A Meta-Analysis. World J Surg 39, 2459–2470 (2015). https://doi.org/10.1007/s00268-015-3108-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-015-3108-3