Abstract
Purpose
The present study aimed to analyze patients’ aesthetic concerns after breast reconstruction with abdominal free flap by reporting secondary cosmetic procedures performed based on the patients’ request, and analyzed the effect of adjuvant therapies and other variables on such outcomes.
Methods
All patients who underwent unilateral immediate reconstruction were enrolled prospectively. Free abdominal flaps were placed horizontally with little manipulation. Secondary procedures were actively recommended during the follow-up period to meet the patients’ aesthetic concerns. The numbers and types of the secondary procedures and the effects of various factors were analyzed.
Results
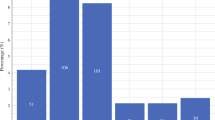
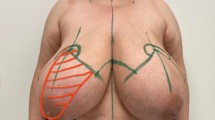
150 patients met the eligibility criteria. The average number of overall secondary surgeries per patient was 1.25. Patients with skin-sparing mastectomy required significantly higher number of secondary surgeries compared with those who underwent nipple-areolar skin-sparing mastectomy. When confined to the cosmetic procedures, 58 (38.7 %) patients underwent 75 operations. The most common procedures were flank dog ear revision, fat injection of the reconstructed breast, and breast liposuction. None of the radiated patients underwent liposuction of the flap. Most commonly liposuctioned regions were the central-lateral and lower-lateral, while fat was most commonly injected to the upper-medial and upper-central part of the breast.
Conclusion
The present study delineated the numbers and types of the secondary operations after horizontally placed abdominal free flap transfer with analysis of the influence of various factors. Addressing such issues during the primary reconstruction would help to reduce the need and extent of the secondary operations and to maximize aesthetic outcome.
Level of Evidence IV
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.





Similar content being viewed by others
References
Spear SL, Davison SP (2003) Aesthetic subunits of the breast. Plast Reconstr Surg 112:440–447
Chang DW (2012) Breast reconstruction with microvascular MS-TRAM and DIEP flaps. Arch Plast Surg 39:3–10
Blondeel PN, Hijjawi J, Depypere H, Roche N, Van Landuyt K (2009) Shaping the breast in aesthetic and reconstructive breast surgery: an easy three-step principle. Part II—breast reconstruction after total mastectomy. Plast Reconstr Surg 123:794–805
Dionyssiou D, Demiri E, Tsimponis A, Boorman J (2014) Predesigned breast shaping assisted by multidetector-row computed tomographic angiography in autologous breast reconstruction. Plast Reconstr Surg 133:100e–108e
Lee TJ, Yoon SY (2006) Simplified insetting strategy in pedicled TRAM flap breast reconstruction. J Korean Soc Plast Reconstr Surg 33:298–302
Enajat M, Smit JM, Rozen WM, Hartman EH, Liss A, Kildal M, Audolfsson T, Acosta R (2010) Aesthetic refinements and reoperative procedures following 370 consecutive DIEP and SIEA flap breast reconstructions: important considerations for patient consent. Aesthet Plast Surg 34:306–312
Losken A, Pinell XA, Sikoro K, Yezhelyev MV, Anderson E, Carlson GW (2011) Autologous fat grafting in secondary breast reconstruction. Ann Plast Surg 66:518–522
Kanchwala SK, Glatt BS, Conant EF, Bucky LP (2009) Autologous fat grafting to the reconstructed breast: the management of acquired contour deformities. Plast Reconstr Surg 124:409–418
Eom JS, Kobayashi MR, Paydar K, Wirth GA, Evans GRD (2014) The number of operations required for completing breast reconstruction. Plast Reconstr Surg Glob Open 2:e242
Damen TH, Mureau MA, Timman R, Rakhorst HA, Hofer SO (2009) The pleasing end result after DIEP flap breast reconstruction: a review of additional operations. J Plast Reconstr Aesthet Surg 62:71–76
Weichman KE, Broer PN, Tanna N, Wilson SC, Allan A, Levine JP et al (2013) The role of autologous fat grafting in secondary microsurgical breast reconstruction. Ann Plast Surg 71:24–30
Fischer JP, Nelson JA, Cleveland E, Sieber B, Rohrbach JI, Serletti JM, Kanchwala S (2013) Breast reconstruction modality outcome study: a comparison of expander/implants and free flaps in select patients. Plast Reconstr Surg 131:928–934
Nahabedian MY (2005) Symmetrical breast reconstruction: analysis of secondary procedures after reconstruction with implants and autologous tissue. Plast Reconstr Surg 115:257–260
Spear SL, Ducic I, Low M, Cuoco F (2005) The effect of radiation on pedicled TRAM flap breast reconstruction: outcomes and implications. Plast Reconstr Surg 115:84–95
Shah C, Kundu N, Arthur D, Vicini F (2013) Radiation therapy following postmastectomy reconstruction: a systematic review. Ann Surg Oncol 20:1313–1322
Schaverien MV, Macmillan RD, McCulley SJ (2013) Is immediate autologous breast reconstruction with postoperative radiotherapy good practice?: a systematic review of the literature. J Plast Reconstr Aesthet Surg 66:1637–1651
Bar-Meir ED, Lin SJ, Momoh AO, Tobias AM, Colakoglu S, Yueh JH, Slavin SA, Lee BT (2011) The lateral chest wall: a separate aesthetic unit in breast surgery. Plast Reconstr Surg 128:626e–634e
Berrino P, Santi P (1988) Preoperative TRAM flap planning for postmastectomy breast reconstruction. Ann Plast Surg 21:264–272
Cone JD, Tavana ML, Ching JA, Smith PD (2012) The Bikini inset: a reliable method for postradiation breast reconstruction with transverse rectus abdominis myocutaneous and free abdominal tissue transfer. Ann Plast Surg 68:420–424
Acknowledgments
The authors would like to thank Hyomin Choi at the University of Chicago for her assistance with data analysis.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Kim, E.K., Suh, Y.C., Maldonado, A.A. et al. Patients’ Aesthetic Concerns After Horizontally Placed Abdominal Free Flap Breast Reconstruction. Aesth Plast Surg 39, 686–693 (2015). https://doi.org/10.1007/s00266-015-0532-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-015-0532-6