Abstract
Aim
Managing periprosthetic joint infections remains a challenging task, and adequate treatment strategies seem to be mandatory to avoid irreversible damage of the affected joint and/or systemic complications. Two-stage revision arthroplasty includes removing all implants and subsequent implantation of an antibiotic-loaded cement spacer, followed by revision arthroplasty as the second stage. Although this procedure is well described in the literature, results remain unpredictable due to various clinical findings and the absence of prospective randomised trials. We analysed (1) mortality and (2) reinfection rates in a series of patients who underwent two-stage revision surgery for periprosthetic hip joint infections with antibiotic-augmented joint spacers. We maintained a special focus on the spacer retention period and its influence on outcome in order to determine the best time for second-stage surgery.
Patients and methods
A consecutive series of 76 patients with native and periprosthetic hip joint infections and who underwent two-stage revision surgery with antibiotic-loaded cement spacers were studied between 2005 and 2010. The second-stage operation was performed when it was assumed that infection was eradicated. The further operative procedure depended upon intra-operative findings (frozen section, local status).
Results
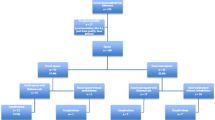
Mean implant-free period with the antibiotic-loaded spacer in situ was 12.6 weeks. Spacer re-implantation was necessary in 13 cases due to positive signs of acute infection in the frozen section and suspect intra-operative findings. Eight patients were not operated for a second time in the investigated time period due to poor general condition. In 40 patients, the spacer retention period was four to 11 weeks: <four weeks for five and >11 weeks for 23. We observed a significantly higher proportion of women free from reinfection in the four to 11-week group than in patients with the shorter or longer period.
Conclusion
According to our findings, the optimal timing for second-stage surgery as a second-stage procedure is between four and 11 weeks. A significantly optimal reinfection rate was seen in patients undergoing revision arthroplasty within that time frame, and 90 % of those patients remained infection free until final follow-up.


Similar content being viewed by others
References
Wolf CF, Gu NY, Doctor JN, Manner PA, Leopold SS (2011) Comparison of one and two-stage revision of total hip arthroplasty complicated by Infection-A Markov expected-utility decision analysis. J Bone Joint Surg Am 93:631–639
Zimmerli W, Trampuz A, Ochsner PE (2004) Prosthetic-joint infections. N Engl J Med 351:1645–1654
Romanò CL, Romanò D, Meani E, Logoluso N, Drago L (2011) Two-stage revision surgery with preformed spacers and cementless implants for septic hiparthritis: a prospective, non-randomized cohort study. BMC Infect Dis 11:129
Westrich GH, Salvati EA, Brause B (1999) Postoperative infection. In: Bono JV, McCarty JC, Thornhill TS, Bierbaum BE, Turner RH (eds) Revision total hip arthroplasty. Springer-Verlag, New York, pp 371–390
McPherson, Woodson C, Holtom P, Roidis N, Shufelt C, Patzakis M (2002) Periprosthetic total hip infection: outcomes using a staging system. Clin Orthop Relat Res (403):8–15
Parvizi J, Zmistowski B, Berbari EF, Bauer TW, Springer BD, Della Valle CJ, Garvin KL, Mont MA, Wongworawat MD, Zalavras CG (2011) New definition for periprosthetic joint infection-from the Workgroup of the Musculoskeletal Infection Society. Clin Orthop Relat Res 469:2992–2994
Berbari EF, Hanssen AD, Duffy MC et al (1998) Risk factors for prosthetic joint infection: case–control study. Clin Infect Dis 27:1247–1254
Meehan AM, Osmon DR, Duffy MC, Hanssen AD, Keating MR (2003) Outcome of penicillin-susceptible streptococcal prostheticjoint infection treated with debridement andretention of theprosthesis. Clin Infect Dis 36:845–849
Elgeidi A, Elganainy AE, Abou Elkhier N, Rakha S (2014) Interleukin-6 and other inflammatory markers in diagnosis of periprosthetic joint infection. Int Orthop 38(12):2591–2595. doi:10.1007/s00264-014-2475-y
Langlais F (2003) Can we improve the resultsof revision arthroplasty for infected total hipreplacement? J Bone Joint Surg (Br) 85:637–640
Lausen B, Schumacher M (1992) Maximally selected rank statistics. Biometrics 48:73–85
Hothorn T maxstat: Maximally Selected Rank Statistics. R package version 0.7-18, 02 Sep 2013 (available from http://cran.r-project.org/web/packages/maxstat/)
Fisman DN, Reilly DT, Karchmer AW, Goldie SJ (2001) Clinical effectiveness and costeffectivenessof 2 management strategies forinfected total hip arthroplasty in the elderly. Clin Infect Dis 32:419–430
Windsor RE, Insall JN, Urs WK, Miller DV, Brause BD (1990) Two-stage reimplantationfor the salvage of total knee arthroplasty complicatedby infection: further follow-up and refinement of indications. J Bone Joint Surg Am 72:272–278
Colyer RA, Capello WN (1994) Surgical treatmentof the infected hip implant: two-stagereimplantation with a one-month interval. Clin Orthop 298:75–79
Wolf M, Clar H, Friesenbichler J, Schwantzer G, Bernhardt G, Gruber G, Glehr M, Leithner A, Sadoghi P (2014) Prosthetic joint infection following total hip replacement: results of one-stage versus two-stage exchange. Int Orthop 38(7):1363–1368. doi:10.1007/s00264-014-2309-y
Nelson CL, Jones RB, Wingert NC, Foltzer M, Bowen TR (2014) Sonication of antibiotic spacers predicts failure during two-stage revision for prosthetic knee and hip infections. Clin Orthop Relat Res 472:2208–2214
Hirakawa K, Stulberg BN, Wilde AH, Bauer TW, Secic M (1998) Results of 2-stage reimplantation for infected total kneearthroplasty. J Arthroplasty 13:22–28
Kendall RW, Duncan CP, Beauchamp CP (1995) Bacterial growth on antibiotic-loaded acrylic cement: a prospective in vivo retrieval study. J Arthroplasty 10:817–822
Mariconda M, Ascione T, Balato G et al (2013) Sonication of antibiotic-loaded cement spacers in a two-stage revision protocol for infected joint arthroplasty. BMC Musculoskelet Disord 14:193. doi:10.1186/1471-2474-14-193
Lass R, Giurea A, Kubista B, Hirschl AM, Graninger W, Presterl E, Windhager R, Holinka J (2014) Bacterial adherence to different components of total hip prosthesis in patients with prosthetic joint infection. Int Orthop 38(8):1597–1602
Maier GS, Horas K, Seeger JB, Roth KE, Kurth AA, Maus U (2014) Is there an association between periprosthetic joint infection and low vitamin D levels? Int Orthop 38(7):1499–1504. doi:10.1007/s00264-014-2338-6
Pignatti P, Nitta S, Dallari D, Sabbioni G, Stagni C, Giunti A (2010) Two stage revision in periprostetic infection: results of 41 cases. Open Orthop J 4:193–200
Senthi S, Munro JT, Pitto RP (2011) Infection in total hip replacement: meta-analysis. Int Orthop 35:253–260
Masri BA, Panagiotopoulos KP, Greidanus NV, Garbuz DS, Duncan CP (2007) Cementless two-stage exchange arthroplastyfor infection after total hip arthroplasty. J Arthroplasty 22:72–78
Kraay MJ, Goldberg VM, Fitzgerald SJ, Salata MJ (2005) Cementless two-staged total hip arthroplasty for deep periprostheticinfection. Clin Orthop Relat Res 441:243–249
Fink B, Grossmann A, Fuerst M, Schäfer P, Frommelt L (2009) Two-stage cementless revision of infected hip endoprostheses. Clin Orthop Relat Res 467:1848–1858
Huang R, Hu CC, Adeli B, Mortazavi J, Parvizi J (2012) Culture-negative periprosthetic joint infection does not preclude infection control. Clin Orthop Relat Res 470:2717–2723
Ekpo TE, Berend KR, Morris MJ, Adams JB, Lombardi AV (2014) Partial two-stage exchange for infected total hip arthroplasty: a preliminary report. Clin Orthop Relat Res 472:437–448
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Vielgut, I., Sadoghi, P., Wolf, M. et al. Two-stage revision of prosthetic hip joint infections using antibiotic-loaded cement spacers: When is the best time to perform the second stage?. International Orthopaedics (SICOT) 39, 1731–1736 (2015). https://doi.org/10.1007/s00264-015-2751-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-015-2751-5