Abstract
Aims
There are concerns that biosimilar erythropoiesis-stimulating agents (ESAs) are less effective than the originator ESAs. The objective of our study was to investigate differences between originator and biosimilar ESA utilisation based on defined daily doses (DDD), doses upon switching, differences between short- and long-acting ESAs and prescribed daily doses (PDD) of either ESA in ambulatory patients with renal anaemia undergoing chronic maintenance haemodialysis [chronic kidney disease (CKD) stage 5].
Methods
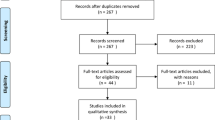
Patients with CKD stage 5 and specific pharmacotherapy with ESAs for at least six 3-month periods (accounting quarters) were selected from a population-based database of accounting information of Bavarian physicians and pharmacy claims data (January 2008 to December 2010). The DDD was used to determine mean ESA consumption. Descriptive statistics were used to describe the results.
Results
In our study, 6,177 CKD stage 5 patients received ESAs for ≥6 accounting quarters, of whom 64.4 % received originator ESAs, 21.1 % received biosimilars and 14.6 % received any sequence originator and biosimilar (total of 35.7 % any biosimilar). Patients receiving either originator short-acting ESAs, long-acting darbepoetin-alfa or M-PEG epoetin-beta had a median DDD consumption of 0.77, 0.81 and 0.90, respectively. Patients receiving a biosimilar short-acting ESA had a median DDD consumption of 0.82. Doses were not increased when the therapy was switched from the originator to the biosimilar ESA. These results were confirmed in 1,886 patients receiving a continuous prescription over 12 accounting quarters, with patients receiving short-acting originator ESAs, long-acting darbepoetin-alfa and biosimilar ESAs having a median daily DDD consumption of 0.80, 0.86 and 0.81, respectively.
Conclusions
We conclude that, based on a population based analysis, ESA consumption of patients on chronic haemodialysis is similar for biosimilar and originator ESAs.


Similar content being viewed by others
References
Jelkmann W (2007) Recombinant EPO production–points the nephrologist should know. Nephrol Dial Transplant 22(10):2749–2753
Macdougall IC (2008) Novel erythropoiesis-stimulating agents: a new era in anemia management. Clin J Am Soc Nephrol 3(1):200–207
Jelkmann W (2009) Efficacy of recombinant erythropoietins: is there unity of international units? Nephrol Dial Transplant 24(5):1366–1368
Brinks V, Hawe A, Basmeleh AH, Joachin-Rodriguez L, Haselberg R, Somsen GW, Jiskoot W, Schellekens H (2011) Quality of original and biosimilar epoetin products. Pharm Res 28(2):386–393
Eschbach JW, Abdulhadi MH, Browne JK, Delano BG, Downing MR, Egrie JC, Evans RW, Friedman EA, Graber SE, Haley NR et al (1989) Recombinant human erythropoietin in anemic patients with end-stage renal disease. Results of a phase III multicenter clinical trial. Ann Intern Med 111(12):992–1000
Goldsmith D, Gesualdo L (2012) Biosimilar epoetins in nephrology—where are we now? Eur Nephrol 6:21–24
Covic A, Cannata-Andia J, Cancarini G, Coppo R, Frazao JM, Goldsmith D, Ronco P, Spasovski GB, Stenvinkel P, Utas C, Wiecek A, Zoccali C, London G (2008) Biosimilars and biopharmaceuticals: what the nephrologists need to know—a position paper by the ERA-EDTA Council. Nephrol Dial Transplant 23(12):3731–3737
Schellekens H (2004) Biosimilar epoetins: how similar are they? Eur J Hosp Pharm 3:43–47
Schöffski O, Müller H-J, Kostev K, Claus D (2011) Consumption of eroythropoiesis-stimulating agents. Nieren- und Hochdruckkrankheiten 40(2):84–90
EMA (2010) Guideline on non-clinical and clinical development of similar biological medicinal products containing recombinant erythropoietins (Revision). Document: EMEA/CHMP/BMWP/301636/2008. Available at: ema.europa.eu. Accessed 15 Feb 2011
Teng L, Xin HW, Blix HS, Tsutani K (2012) Review of the use of defined daily dose concept in drug utilisation research in China. Pharmacoepidemiol Drug Saf. doi: 10.1002/pds.3240
Horl WH, Locatelli F, Haag-Weber M, Ode M, Roth K (2012) Prospective multicenter study of HX575 (biosimilar epoetin-I+/−) in patients with chronic kidney disease applying a target hemoglobin of 10–12 g/dl. Clin Nephrol 78(1):24–32
WIdO (2010) Anatomisch-therapeutisch chemische Klassifikation mit Tagesdosen—amtliche deutsche Fassung. Accessed: 15 Feb 2011
Sorgel F, Thyroff-Friesinger U, Vetter A, Vens-Cappell B, Kinzig M (2009) Bioequivalence of HX575 (recombinant human epoetin alfa) and a comparator epoetin alfa after multiple intravenous administrations: an open-label randomised controlled trial. BMC Clin Pharmacol 9:10
Sorgel F, Thyroff-Friesinger U, Vetter A, Vens-Cappell B, Kinzig M (2009) Bioequivalence of HX575 (recombinant human epoetin alfa) and a comparator epoetin alfa after multiple subcutaneous administrations. Pharmacology 83(2):122–130
Haag-Weber M, Vetter A, Thyroff-Friesinger U (2009) Therapeutic equivalence, long-term efficacy and safety of HX575 in the treatment of anemia in chronic renal failure patients receiving hemodialysis. Clin Nephrol 72(5):380–390
Krivoshiev S, Todorov VV, Manitius J, Czekalski S, Scigalla P, Koytchev R (2008) Comparison of the therapeutic effects of epoetin zeta and epoetin alpha in the correction of renal anaemia. Curr Med Res Opin 24(5):1407–1415
Krivoshiev S, Wizemann V, Czekalski S, Schiller A, Pljesa S, Wolf-Pflugmann M, Siebert-Weigel M, Koytchev R, Bronn A (2010) Therapeutic equivalence of epoetin zeta and alfa, administered subcutaneously, for maintenance treatment of renal anemia. Adv Ther 27(2):105–117
Wizemann V, Rutkowski B, Baldamus C, Scigalla P, Koytchev R (2008) Comparison of the therapeutic effects of epoetin zeta to epoetin alfa in the maintenance phase of renal anaemia treatment. Curr Med Res Opin 24(3):625–637
Wiecek A, Ahmed I, Scigalla P, Koytchev R (2010) Switching epoetin alfa and epoetin zeta in patients with renal anemia on dialysis: Posthoc analysis. Adv Ther 27(12):941–952
Abu-Alfa AK, Sloan L, Charytan C, Sekkarie M, Scarlata D, Globe D, Audhya P (2008) The association of darbepoetin alfa with hemoglobin and health-related quality of life in patients with chronic kidney disease not receiving dialysis. Curr Med Res Opin 24(4):1091–1100
Agarwal A, Silver MR, Walczyk M, Liu W, Audhya P (2007) Once-monthly darbepoetin alfa for maintaining hemoglobin levels in older patients with chronic kidney disease. J Am Med Dir Assoc 8(2):83–90
Biggar P, Ketteler M, Hennemann H, Domling R (2008) Switch of ESA therapy from darbepoetin-alpha to epoetin-beta in hemodialysis patients: a single-center experience. Clin Nephrol 69(3):185–192
Bock HA, Hirt-Minkowski P, Brunisholz M, Keusch G, Rey S, von Albertini B (2008) Darbepoetin alpha in lower-than-equimolar doses maintains haemoglobin levels in stable haemodialysis patients converting from epoetin alpha/beta. Nephrol Dial Transplant 23(1):301–308
Brunkhorst R, Bommer J, Braun J, Haag-Weber M, Gill C, Wagner J, Wagener T (2004) Darbepoetin alfa effectively maintains haemoglobin concentrations at extended dose intervals relative to intravenous or subcutaneous recombinant human erythropoietin in dialysis patients. Nephrol Dial Transplant 19(5):1224–1230
Locatelli F, Canaud B, Giacardy F, Martin-Malo A, Baker N, Wilson J (2003) Treatment of anaemia in dialysis patients with unit dosing of darbepoetin alfa at a reduced dose frequency relative to recombinant human erythropoietin (rHuEpo). Nephrol Dial Transplant 18(2):362–369
Acknowledgements
This data analysis has been a part of the PHARAO (objective drug utilisation analysis/Objektive Arzneimittelanalysen) project of the Bavarian statutory health insurance physician’s association. We would like to acknowledge the pharmaceutical contribution of Larissa Gampert and the valuable help of Nadine Stryewski with the project management.
Conflict of interest/Disclosure
The efforts for this study, which go beyond the core tasks of the Bavarian statutory health insurance physician’s association, were financially covered by Hexal (Epoetin alfa Hexal®), Medice (Abseamed®) and Sandoz (Binocrit®). All authors have completed the Unified Competing Interest form at www.icmje.org/coi_disclosure.pdf (available on request from the corresponding author) and declare that Peter Bramlage, Joerg Hasford and Reinhard Brunkhorst had support from the KV Bayern for the submitted work. There were no financial relationships with any organisations that might have an interest in the submitted work in the previous 3 years and no other relationships or activities that could appear to have influenced the submitted work.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hörbrand, F., Bramlage, P., Fischaleck, J. et al. A population-based study comparing biosimilar versus originator erythropoiesis-stimulating agent consumption in 6,117 patients with renal anaemia. Eur J Clin Pharmacol 69, 929–936 (2013). https://doi.org/10.1007/s00228-012-1412-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00228-012-1412-5