Abstract
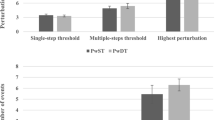
This study aimed to examine the effect of explicit cuing on reactive stepping with the paretic limb during slip-like perturbations in stroke survivors and to identify differences in postural stability and fall-risk while stepping with either limb. Eleven chronic hemiparetic stroke survivors received slip-like stance perturbations in no-cue (implicit, no instructions) and cued (explicit, instructions to step with paretic limb) conditions. Frequency of stepping with the paretic limb was recorded. Differences between non-paretic and paretic steps for falls, number of compensatory steps, relative center-of-mass position (X COM/BOS), and velocity \((\dot{X}_{\rm COM/BOS} )\), and vertical limb support (hip descent—Z hip) were analyzed. Stepping with the paretic limb increased from 6 % in no-cue condition to 42 % in cued condition with no significant difference in number of falls and steps regardless of stepping limb. At liftoff of the compensatory step, stability was greater (anterior X COM/BOS) with paretic than non-paretic limb stepping whereas, at touchdown (TD) of the step, stability with paretic limb reduced (posterior X COM/BOS and \(\dot{X}_{\rm COM/BOS}\)) due to a smaller compensatory step taken with the paretic versus non-paretic limb. There was no significant difference in peak Z hip regardless of stepping limb; however, the timing of peak Z hip differed (occuring prior to TD during non-paretic stepping and post-TD during paretic stepping). Thus, fall onset was earlier with non-paretic versus paretic stepping. The results support that explicit cueing can facilitate initiation of reactive step from the paretic limb as compared with the no-cue condition. Stepping with the paretic limb in the cued condition however altered time of fall onset. Regardless of the stepping side, individuals demonstrated a fall risk suggesting the need for interventions focusing on reactive step training with both the limbs.






Similar content being viewed by others
Abbreviations
- BOS:
-
Base of support
- COM:
-
Center of mass
- LO:
-
Liftoff
- TD:
-
Touchdown
- X COM/BOS :
-
Center-of-mass position relative to the base of support
- \(\dot{X}_{\rm COM/BOS}\) :
-
Center-of-mass velocity relative to heel velocity of the limb forming the posterior margin of base of support
References
Adkin AL, Quant S, Maki BE, McIlroy WE (2006) Cortical responses associated with predictable and unpredictable compensatory balance reactions. Exp Brain Res 172:85–93
Appelros P, Jonsson F, Asberg S, Asplund K, Glader EL, Asberg KH, Norrving B, Stegmayr B, Terent A, Riks-Stroke C (2014) Trends in stroke treatment and outcome between 1995 and 2010: observations from Riks-Stroke, the Swedish stroke register. Cerebrovasc Dis 37:22–29
Batchelor FA, Mackintosh SF, Said CM, Hill KD (2012) Falls after stroke. Int J Stroke 7:482–490
Begg RK, Tirosh O, Said CM, Sparrow WA, Steinberg N, Levinger P, Galea MP (2014) Gait training with real-time augmented toe-ground clearance information decreases tripping risk in older adults and a person with chronic stroke. Front Hum Neurosci 8:243
Bhatt T, Wening JD, Pai YC (2006) Adaptive control of gait stability in reducing slip-related backward loss of balance. Exp Brain Res 170:61–73
Bolton DA, Williams L, Staines WR, McIlroy WE (2012) Contribution of primary motor cortex to compensatory balance reactions. BMC Neurosci 13:102
Dault MC, de Haart M, Geurts AC, Arts IM, Nienhuis B (2003) Effects of visual center of pressure feedback on postural control in young and elderly healthy adults and in stroke patients. Hum Mov Sci 22:221–236
de Haart M, Geurts AC, Dault MC, Nienhuis B, Duysens J (2005) Restoration of weight-shifting capacity in patients with postacute stroke: a rehabilitation cohort study. Arch Phys Med Rehabil 86:755–762
Den Otter AR, Geurts AC, de Haart M, Mulder T, Duysens J (2005) Step characteristics during obstacle avoidance in hemiplegic stroke. Exp Brain Res 161:180–192
Eng JJ, Chu KS (2002) Reliability and comparison of weight-bearing ability during standing tasks for individuals with chronic stroke. Arch Phys Med Rehabil 83:1138–1144
Espy DD, Yang F, Bhatt T, Pai YC (2010) Independent influence of gait speed and step length on stability and fall risk. Gait Posture 32:378–382
Garland SJ, Ivanova TD, Mochizuki G (2007) Recovery of standing balance and health-related quality of life after mild or moderately severe stroke. Arch Phys Med Rehabil 88:218–227
Hu X, Suresh AK, Li X, Rymer WZ, Suresh NL (2012) Impaired motor unit control in paretic muscle post stroke assessed using surface electromyography: a preliminary report. Conf Proc IEEE Eng Med Biol Soc 2012:4116–4119
Hyngstrom A, Onushko T, Chua M, Schmit BD (2010) Abnormal volitional hip torque phasing and hip impairments in gait post stroke. J Neurophysiol 103:1557–1568
Imamizu H, Sugimoto N, Osu R, Tsutsui K, Sugiyama K, Wada Y, Kawato M (2007) Explicit contextual information selectively contributes to predictive switching of internal models. Exp Brain Res 181:395–408
Inness EL, Mansfield A, Lakhani B, Bayley M, McIlroy WE (2014) Impaired reactive stepping among patients ready for discharge from inpatient stroke rehabilitation. Phys Ther 94:1755–1764
Jorgensen HS, Nakayama H, Raaschou HO, Vive-Larsen J, Stoier M, Olsen TS (1995) Outcome and time course of recovery in stroke. Part I: outcome. The Copenhagen Stroke Study. Arch Phys Med Rehabil 76:399–405
Kajrolkar T, Yang F, Pai YC, Bhatt T (2014) Dynamic stability and compensatory stepping responses during anterior gait–slip perturbations in people with chronic hemiparetic stroke. J Biomech 47:2751–2758
Knarr BA, Reisman DS, Binder-Macleod SA, Higginson JS (2013) Understanding compensatory strategies for muscle weakness during gait by simulating activation deficits seen post-stroke. Gait Posture 38:270–275
Lakhani B, Mansfield A, Inness EL, McIlroy WE (2011a) Compensatory stepping responses in individuals with stroke: a pilot study. Physiother Theory Pract 27:299–309
Lakhani B, Mansfield A, Inness EL, McIlroy WE (2011b) Characterizing the determinants of limb preference for compensatory stepping in healthy young adults. Gait Posture 33:200–204
Lewek MD, Feasel J, Wentz E, Brooks FP Jr, Whitton MC (2012) Use of visual and proprioceptive feedback to improve gait speed and spatiotemporal symmetry following chronic stroke: a case series. Phys Ther 92:748–756
Lewek MD, Bradley CE, Wutzke CJ, Zinder SM (2014) The relationship between spatiotemporal gait asymmetry and balance in individuals with chronic stroke. J Appl Biomech 30:31–36
Lin YH, Tang PF, Wang YH, Eng JJ, Lin KC, Lu L, Jeng JS, Chen SC (2014) Reactive postural control deficits in patients with posterior parietal cortex lesions after stroke and the influence of auditory cueing. Am J Phys Med Rehabil 93:849–859
Liu J, Lockhart TE (2009) Age-related joint moment characteristics during normal gait and successful reactive-recovery from unexpected slip perturbations. Gait Posture 30:276–281
Mackintosh SF, Goldie P, Hill K (2005) Falls incidence and factors associated with falling in older, community-dwelling, chronic stroke survivors (>1 year after stroke) and matched controls. Aging Clin Exp Res 17:74–81
Maki BE, McIlroy WE (1997) The role of limb movements in maintaining upright stance: the “change-in-support” strategy. Phys Ther 77:488–507
Mansfield A, Maki BE (2009) Are age-related impairments in change-in-support balance reactions dependent on the method of balance perturbation? J Biomech 42:1023–1031
Mansfield A, Inness EL, Komar J, Biasin L, Brunton K, Lakhani B, McIlroy WE (2011) Training rapid stepping responses in an individual with stroke. Phys Ther 91:958–969
Mansfield A, Inness EL, Lakhani B, McIlroy WE (2012) Determinants of limb preference for initiating compensatory stepping poststroke. Arch Phys Med Rehabil 93:1179–1184
Mansfield A, Inness EL, Wong JS, Fraser JE, McIlroy WE (2013) Is impaired control of reactive stepping related to falls during inpatient stroke rehabilitation? Neurorehabil Neural Repair 27:526–533
Marigold DS, Eng JJ (2006a) The relationship of asymmetric weight-bearing with postural sway and visual reliance in stroke. Gait Posture 23:249–255
Marigold DS, Eng JJ (2006b) Altered timing of postural reflexes contributes to falling in persons with chronic stroke. Exp Brain Res 171:459–468
Martinez KM, Mille ML, Zhang Y, Rogers MW (2013) Stepping in persons poststroke: comparison of voluntary and perturbation-induced responses. Arch Phys Med Rehabil 94:2425–2432
Mazzoni P, Krakauer JW (2006) An implicit plan overrides an explicit strategy during visuomotor adaptation. J Neurosci 26:3642–3645
McIlroy WE, Maki BE (1996) Age-related changes in compensatory stepping in response to unpredictable perturbations. J Gerontol A Biol Sci Med Sci 51:M289–M296
McMahon TA (1984) Muscles, reflexes, and locomotion. Princeton University Press, Princeton
Page SJ, Gater DR, Bach YRP (2004) Reconsidering the motor recovery plateau in stroke rehabilitation. Arch Phys Med Rehabil 85:1377–1381
Pai YC (2003) Movement termination and stability in standing. Exerc Sport Sci Rev 31:19–25
Pai YC, Rogers MW, Patton J, Cain TD, Hanke TA (1998) Static versus dynamic predictions of protective stepping following waist–pull perturbations in young and older adults. J Biomech 31:1111–1118
Pai YC, Yang F, Wening JD, Pavol MJ (2006) Mechanisms of limb collapse following a slip among young and older adults. J Biomech 39:2194–2204
Pavol MJ, Pai YC (2007) Deficient limb support is a major contributor to age differences in falling. J Biomech 40:1318–1325
Pavol MJ, Runtz EF, Pai YC (2004) Diminished stepping responses lead to a fall following a novel slip induced during a sit-to-stand. Gait Posture 20:154–162
Sackley CM, Lincoln NB (1997) Single blind randomized controlled trial of visual feedback after stroke: effects on stance symmetry and function. Disabil Rehabil 19:536–546
Titianova EB, Tarkka IM (1995) Asymmetry in walking performance and postural sway in patients with chronic unilateral cerebral infarction. J Rehabil Res Dev 32:236–244
van Asseldonk EH, Buurke JH, Bloem BR, Renzenbrink GJ, Nene AV, van der Helm FC, van der Kooij H (2006) Disentangling the contribution of the paretic and non-paretic ankle to balance control in stroke patients. Exp Neurol 201:441–451
van Vliet PM, Wulf G (2006) Extrinsic feedback for motor learning after stroke: what is the evidence? Disabil Rehabil 28:831–840
Walker C, Brouwer BJ, Culham EG (2000) Use of visual feedback in retraining balance following acute stroke. Phys Ther 80:886–895
Weerdesteyn V, de Niet M, van Duijnhoven HJ, Geurts AC (2008) Falls in individuals with stroke. J Rehabil Res Dev 45:1195–1213
Yang F, Pai YC (2011) Automatic recognition of falls in gait-slip training: harness load cell based criteria. J Biomech 44:2243–2249
Yang F, Bhatt T, Pai YC (2009) Role of stability and limb support in recovery against a fall following a novel slip induced in different daily activities. J Biomech 42:1903–1908
Acknowledgments
This study was supported by the American Heart Association, National Affiliate for the Scientific Development Grant 12SDG12170022. Findings from this study were presented at the Society of Neuroscience Conference 2014, Washington, DC. We would like to thank Vandana Vaid, Abdul Karim, and Pooja Salot for assistance with data collection and processing.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Patel, P., Bhatt, T. Modulation of reactive response to slip-like perturbations: effect of explicit cues on paretic versus non-paretic side stepping and fall-risk. Exp Brain Res 233, 3047–3058 (2015). https://doi.org/10.1007/s00221-015-4367-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00221-015-4367-9