Abstract
Rationale
Studies have demonstrated that both pain and opioids have actions on the central nervous system that may interfere with cognitive function, but their effects have mainly been analysed separately and not as an integrated process.
Objective
The objective of this study is to test two hypotheses: (1) the analgesic effect of opioids improves cognitive function by decreasing pain, and (2) pain antagonizes cognitive effects of opioids.
Methods
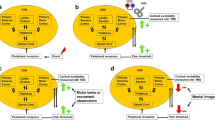
Randomized, placebo-controlled, crossover study. Three experiments were conducted with 22 healthy males. Sustained attention, memory and motor function/attention/mental flexibility were evaluated by continuous reaction time (CRT), verbal fluency test (VFT) and trail making test-B (TMT-B), respectively. In the 1st experiment, the cognitive effects of experimental tonic pain of mild and moderate intensities produced by a computer-controlled pneumatic tourniquet cuff were assessed; in the 2nd, the effects of saline solution and remifentanil were assessed in the absence of pain; and in the 3rd experiment, the cognitive effects of moderate pain intensity relieved by remifentanil infusion were assessed followed by increasing pain to moderate intensity during a constant remifentanil infusion.
Results
The first two experiments demonstrated that pain and remifentanil impaired CRT. In the 3rd experiment, remifentanil infusion relieving pain significantly impaired CRT and further deterioration was noted following increasing pain intensity.
Conclusion
Pain and remifentanil seemed to have additive deleterious cognitive effects. This study represents an initial step to enhance our basic understanding of some of the cognitive effects following a painful stimulus and an opioid infusion separately and combined in a sequence comparable to clinical settings.


Similar content being viewed by others
References
Abwender DA, Swan JG, Bowerman JT, Connolly SW (2001) Qualitative analysis of verbal fluency output: review and comparison of several scoring methods. Assessment 8:323–338
Benton AL (1969) Development of a multilingual aphasia battery: progress and problems. J Neurol Sci 9:39–48
Black ML, Hill JL, Zacny JP (1999) Behavioral and psysiological effects of remifentanil and alfentanil in healthy volunteers. Anesthesiology 90:718–726
Crombez G, Eccleston C, Baeyens F, Eelen P (1996) The disruptive nature of pain: an experimental investigation. Behav Res Ther 34:911–918
Dick BD, Rashiq S (2007) Disruption of attention and working memory traces in individuals with chronic pain. Anesth Analg 104:1223–1229
Eccleston C (1994) Chronic pain and attention: a cognitive approach. Br J Clin Psychol 33:535–547
Eccleston C (1995) Chronic pain and distraction: an experimental investigation into the role of sustained and shifting attention in the processing of chronic persistent pain. Behav Res Ther 33:391–405
Eccleston C, Crombez G (1999) Pain demands attention: a cognitive-affective model of the interruptive function of pain. Psychol Bull 125:356–366
Eccleston C, Crombez G, Aldrich S, Stannard C (1997) Attention and somatic awareness in chronic pain. Pain 72:209–215
Elsass P (1986) Continuous reaction times in cerebral dysfunction. Acta Neurol Scand 73:225–246
Ersek M, Cherrier MM, Overman SS, Irving GA (2004) The cognitive effects of opioids. Pain Manag Nurs 5:75–93
Folstein MF, Folstein SE, McHugh PR (1975) Mini-mental state: a practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 12:189–198
Hart RP, Wade JB, Martelli MF (2003) Cognitive impairment in patients with chronic pain: the significance of stress. Curr Pain Headache Rep 7:116–126
Haythornthwaite JA, Menefee LA, Quatrano-Piacentini AL, Pappagallo M (1998) Outcome of chronic opioid therapy for non-cancer pain. J Pain Symptom Manag 15:185–194
Højsted J, Kurita GP, Kendall S, Lundorff L, de Mattos Pimenta CA, Sjøgren P (2012) Non-analgesic effects of opioids: the cognitive effects of opioids in chronic pain of malignant and non-malignant origin. An update. Curr Pharm Des 18:6116–6122
Inui N, Walsh LD, Taylor JL, Gandevia SC (2011) Dynamic changes in the perceived posture of the hand during ischaemic anaesthesia of the arm. J Physiol 589:5775–5784
Jamison RN, Schein JR, Vallow S, Ascher S, Vorsanger GJ, Katz NP (2003) Neuropsychological effects of long-term opioid use in chronic pain patients. J Pain Symptom Manag 26:913–921
Kendall SE, Sjøgren P, Pimenta CA, Højsted J, Kurita GP (2010) The cognitive effects of opioids in chronic non-cancer pain. Pain 150:225–230
Keogh E, Moore DJ, Duggan GB, Payne SJ, Eccleston C (2013) The disruptive effects of pain on complex cognitive performance and executive control. PLoS ONE 8:e83272
Kurita GP, Lundorff L, Pimenta CAM, Sjøgren P (2009) The cognitive effects of opioids in cancer: a systematic review. Supp Care Cancer 17:11–21
Lezak M, Howieson DB, Loring DW (2004) Neuropsychological assessment. Oxford University Press, New York
Lorenz J, Beck H, Bromm B (1997) Cognitive performance, mood and experimental pain before and during morphine-induced analgesia in patients with chronic non-malignant pain. Pain 73:369–375
McGuire BE (2013) Chronic pain and cognitive function. Pain 154:964–965
Moore DJ, Keogh E, Eccleston C (2012) The interruptive effect of pain on attention. Q J Exp Psychol (Hove) 65:565–586
Moore DJ, Keogh E, Eccleston C (2013) Headache impairs attentional performance. Pain 154:1840–1845
Moriarty O, McGuire BE, Finn DP (2011) The effect of pain on cognitive function: a review of clinical and preclinical research. Prog Neurobiol 93:385–404
Petersen-Felix S, Curatolo M (2002) Neuroplasticity: an important factor in acute and chronic pain. Swiss Med Wkly 132:273–278
Polianskis R, Graven-Nielsen T, Arendt-Nielsen L (2001) Computer-controlled pneumatic pressure algometry: a new technique for quantitative sensory testing. Eur J Pain 5:267–277
Polianskis R, Graven-Nielsen T, Arendt-Nielsen L (2002) Spatial and temporal aspects of deep tissue pain assessed by cuff algometry. Pain 100:19–26
Reitan RM (1958) Validity of the trail making test as an indicator of organic brain damage. Percept Mot Skills 8:271–276
Sjogren P, Thomsen AB, Olsen AK (2000) Impaired neuropsychological performance in chronic nonmalignant pain patients receiving long-term oral opioid therapy. J Pain Symptom Manag 19:100–108
Sjøgren P, Banning A, Christensen CB, Pedersen O (1994) Continuous reaction time after single dose, long-term oral and epidural opioid administration. Eur J Anaesthesiol 11:95–100
Tassain V, Attal N, Fletcher D et al (2003) Long term effects of oral sustained release morphine on neuropsychological performance in patients with chronic non-cancer pain. Pain 104:389–400
Wade JB, Hart RP (2002) Attention and the stages of pain processing. Pain Med 3:30–38
Walsh DM, Liggett C, Baxter D, Allen JM (1995) A double-blind investigation of the hypoalgesic effects of transcutaneous electrical nerve stimulation upon experimentally induced ischaemic pain. Pain 61:39–45
Woolf CJ, Salter MW (2000) Neuronal plasticity: increasing the gain in pain. Science 288:1765–1769
Zacny JP (1995) A review of the effects of opioids on psychomotor and cognitive functioning in humans. Exp Clin Psychopharmacol 3:432–466
Zacny JP, Beckman NJ (2004) The effects of a cold-water stimulus on butorphanol effects in males and females. Pharmacol Biochem Behav 78:653–659
Acknowledgments
The study was supported by The Danish Cancer Society and The Danish Council for Strategic Research. The authors worked independently at all stages of the study, including the design, data collection, analysis, data interpretation, preparation and revision of the manuscript. In addition, the authors have full control of all primary data and agree to allow the journal to review their data if requested.
Conflict of interest
The authors declare no conflicts of interest related to this study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kurita, G.P., Malver, L.P., Andresen, T. et al. Does mutual compensation of the cognitive effects induced by pain and opioids exist? An experimental study. Psychopharmacology 232, 1373–1381 (2015). https://doi.org/10.1007/s00213-014-3768-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00213-014-3768-y